Attached files
| file | filename |
|---|---|
| EX-32.1 - EX-32.1 - SUNLINK HEALTH SYSTEMS INC | d229875dex321.htm |
| EX-31.1 - EX-31.1 - SUNLINK HEALTH SYSTEMS INC | d229875dex311.htm |
| EX-31.2 - EX-31.2 - SUNLINK HEALTH SYSTEMS INC | d229875dex312.htm |
| EX-32.2 - EX-32.2 - SUNLINK HEALTH SYSTEMS INC | d229875dex322.htm |
| EX-21.1 - EX-21.1 - SUNLINK HEALTH SYSTEMS INC | d229875dex211.htm |
| EX-23.1 - EX-23.1 - SUNLINK HEALTH SYSTEMS INC | d229875dex231.htm |
| EX-10.18 - EX-10.18 - SUNLINK HEALTH SYSTEMS INC | d229875dex1018.htm |
| EX-10.19 - EX-10.19 - SUNLINK HEALTH SYSTEMS INC | d229875dex1019.htm |
| EX-10.17 - EX-10.17 - SUNLINK HEALTH SYSTEMS INC | d229875dex1017.htm |
Index to Financial Statements
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
WASHINGTON, D.C. 20549
Form 10-K
| x | ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the Fiscal Year Ended June 30, 2011
OR
| ¨ | TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the transition period from to
Commission File No. 1-12607
SunLink Health Systems, Inc.
(Exact name of registrant as specified in its charter)
| Ohio | 31-0621189 | |
| (State or other jurisdiction of incorporation or organization) |
(I.R.S. Employer Identification No.) |
900 Circle 75 Parkway, Suite 1120, Atlanta, Georgia 30339
(Address of principal executive offices)
Registrant’s telephone number, including area code: (770) 933-7000
Securities Registered Pursuant to Section 12(b) of the Act:
| Title of each Class |
Name of each Exchange on which registered | |
| Common Shares without par value | NYSE Amex Equities |
Indicate by check mark whether if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes ¨ No x
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes ¨ No x
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes x No ¨
Indicate by check mark whether the registrant has submitted electronically and posted on its corporate Web site, if any, every Interactive Data File required to be submitted and posted pursuant to Rule 405 of Regulation S-T (§ 232.405 of this chapter) during the preceding 12 months (or for such shorter period that the registrant was required to submit and post such files). Yes ¨ No ¨
Indicate by check mark if disclosure of delinquent filers pursuant to Item 405 of Regulation S-K (§ 229.405 of this chapter) is not contained herein, and will not be contained, to the best of the registrant’s knowledge, in definitive proxy or information statements incorporated by reference in Part III of this Form 10-K or any amendment to this Form 10-K Yes ¨ No x
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, or a non-accelerated filer, or a smaller reporting company. See definition of “large accelerated filer”, “accelerated filer” and “smaller reporting company” in Rule 12b-2 of the Exchange Act.
| Large accelerated filer ¨ | Accelerated filer ¨ | |
| Non-accelerated filer ¨ |
Smaller reporting company x | |
| (Do not check if a smaller reporting company) |
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Act). Yes ¨ No x
At the close of business on September 23, 2011, there were 9,456,869 shares of the registrant’s common shares without par value outstanding. The aggregate market value of the voting and non-voting common equity held by non-affiliates computed by reference to the closing price on December 31, 2010 of the registrant’s common shares as reported by NYSE Amex Equities stock exchange amounted to $7,323,000.
Index to Financial Statements
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the registrant’s definitive Proxy Statement to be filed under Regulation 14A in connection with the Annual Meeting of Shareholders of SunLink Health Systems, Inc., scheduled to be held on November 7, 2011, have been incorporated by reference into Part III of this Report. The Proxy Statement or an amendment to this Annual Report will be filed with the Securities and Exchange Commission within 120 days after June 30, 2011.
2
Index to Financial Statements
Certain Cautionary Statements
FORWARD-LOOKING STATEMENTS
This Annual Report and the documents that are incorporated by reference in this Annual Report contain certain forward-looking statements within the meaning of the safe harbor for forward-looking statements contained in the Private Securities Litigation Reform Act of 1995. Forward-looking statements include all statements that do not relate solely to historical or current facts and may be identified by the use of words such as “may,” “believe,” “will,” “expect,” “project,” “estimate,” “anticipate,” “plan” or “continue.” These forward-looking statements are based on current plans and expectations and are subject to a number of risks, uncertainties and other factors which could significantly affect current plans and expectations and our future financial condition and results. These factors, which could cause actual results, performance and achievements to differ materially from those anticipated, include, but are not limited to:
General Business Conditions
| • | general economic and business conditions in the U.S., both nationwide and in the states in which we operate; |
| • | the competitive nature of the U.S. community hospital, homecare, and specialty pharmacy businesses; |
| • | demographic changes in areas where we operate; |
| • | the availability of new long-term financing to replace our current credit agreement lender; |
| • | the availability of cash or borrowings to fund working capital, renovations, replacement, expansion and capital improvements at existing healthcare and specialty pharmacy facilities and for acquisitions and replacement of such facilities; |
| • | changes in accounting principles generally accepted in the U.S.; and, |
| • | fluctuations in the market value of equity securities including SunLink common shares; |
Operational Factors
| • | inability to operate profitably in one or more segments of the healthcare business; |
| • | the availability of, and our ability to attract and retain, sufficient qualified staff physicians, management, nurses, pharmacists and staff personnel for our operations; |
| • | timeliness and amount of reimbursement payments received under government programs; |
| • | increases in interest rates under debt agreements; |
| • | the inability to refinance existing indebtedness and potential defaults under existing indebtedness; |
| • | restrictions imposed by debt agreements; |
| • | the cost and availability of insurance coverage including professional liability (e.g., medical malpractice) and general liability insurance; |
| • | the efforts of insurers, healthcare providers, and others to contain healthcare costs; |
| • | the impact on hospital services of the treatment of patients in lower acuity healthcare settings, whether with drug therapy or via alternative healthcare services, such as surgery centers or urgent care centers; |
| • | changes in medical and other technology; |
| • | risks of changes in estimates of self insurance claims and reserves; |
| • | increases in prices of materials and services utilized in our Healthcare Facilities and Specialty Pharmacy Segments; |
3
Index to Financial Statements
| • | increases in wages as a result of inflation or competition for management, physician, nursing, pharmacy and staff positions; |
| • | increases in the amount and risk of collectability of accounts receivable, including deductibles and co-pay amounts; and, |
| • | the functionality or costs with respect to our management information system for our Healthcare Facilities and Specialty Pharmacy Segments, including both software and hardware; |
| • | the availability and competition from alternative drugs or treatments provided by our Specialty Pharmacy Segment; |
Liabilities, Claims, Obligations and Other Matters
| • | claims under leases, guarantees and other obligations relating to discontinued operations, including sold facilities, retained or acquired subsidiaries and former subsidiaries; |
| • | potential adverse consequences of known and unknown government investigations; |
| • | claims for product and environmental liabilities from continuing and discontinued operations; |
| • | professional, general and other claims which may be asserted against us; and |
| • | natural disasters and weather-related events such as earthquakes, flooding, snow, ice and wind damage and population evacuations affecting areas in which we operate. |
Regulation and Governmental Activity
| • | existing and proposed governmental budgetary constraints; |
| • | the regulatory environment for our businesses, including state certificate of need laws and pharmacy licensing laws and regulations, rules and judicial cases relating thereto; |
| • | anticipated adverse changes in the levels and terms of government (including Medicare, Medicaid and other programs) and private reimbursement for SunLink’s healthcare facilities and specialty pharmacy services including the payment arrangements and terms of managed care agreements; |
| • | changes in or failure to comply with Federal, state or local laws and regulations affecting our Healthcare Facilities and Specialty Pharmacy Segments; and, |
| • | the possible enactment of Federal healthcare reform laws or reform laws in states where we operate hospital and pharmacy facilities (including Medicaid waivers, competitive bidding and other reforms). |
Acquisition and Merger Related Matters
| • | the availability and terms of capital to fund acquisitions, improvements, renovations or replacement facilities; |
| • | impairment or uncollectibility of certain acquired assets; |
| • | assumed liabilities discovered subsequent to an acquisition; |
| • | our ability to integrate acquired healthcare businesses and implement our business strategy; and |
| • | competition in the market for acquisitions of hospitals and healthcare businesses. |
The foregoing are significant factors we think could cause our actual results to differ materially from expected results. However, there could be additional factors besides those listed herein that also could affect SunLink in an adverse manner.
4
Index to Financial Statements
You should read this Annual Report completely and with the understanding that actual future results may be materially different from what we expect. You are cautioned not to unduly rely on forward-looking statements when evaluating the information presented in this Annual Report or our other disclosures because current plans, anticipated actions, and future financial conditions and results may differ from those expressed in any forward-looking statements made by or on behalf of SunLink.
We have not undertaken any obligation to publicly update or revise any forward-looking statements. All of our forward-looking statements speak only as of the date of the document in which they are made or, if a date is specified, as of such date. We disclaim any obligation or undertaking to provide any updates or revisions to any forward-looking statement to reflect any change in our expectations or any changes in events, conditions, circumstances or information on which the forward-looking statement is based. All subsequent written and oral forward-looking statements attributable to us or persons acting on our behalf are expressly qualified in their entirety by the foregoing factors and the other risk factors set forth elsewhere in this report.
5
Index to Financial Statements
PART I
| Item 1. | Business (all dollar amounts in thousands except share, per share and revenue per equivalent admission amounts) |
Overview
We are SunLink Health Systems, Inc. Unless the context indicates otherwise, all references to “SunLink,” “we,” “our,” “ours,” “us” and the “Company” refer to SunLink Health Systems, Inc. and our consolidated subsidiaries. We are a provider of healthcare services in certain markets in the United States. References to our specific operations refers to operations conducted through our subsidiaries and references to “we,” “our,” “ours,” and “us” in such context refers to the operations of our subsidiaries. Our business is composed of two business segments, the Healthcare Facilities Segment and the Specialty Pharmacy Segment. Through our subsidiaries, we operate a total of six community hospitals in three states. Five of the community hospitals are owned and one is leased. Our community hospitals are acute care hospitals and have a total of 342 licensed beds. As part of our community hospital operations, we currently also operate (a) three nursing homes in two states, each of which is located adjacent to, or in close proximity with, one of our community hospitals, and (b) one home healthcare agency operated from one of our community hospitals. Our nursing homes have a total of 261 licensed beds. We also own a hospital building with a total of 60 licensed beds that we lease to a third party, which owns the hospital license for the facility, with an option to purchase. Through a subsidiary acquired in April 2008, we also operate a specialty pharmacy business with four service lines. Our healthcare operations are conducted through our direct and indirect subsidiaries, including SunLink Healthcare LLC (“SHL”), HealthMont LLC (“HealthMont”) and SunLink ScriptsRx, LLC (“ScriptsRx”).
Our executive offices are located at 900 Circle 75 Parkway, Suite 1120, Atlanta, Georgia 30339, and our telephone number is (770) 933-7000. Our website address is “www.sunlinkhealth.com.” Information contained on our website does not constitute part of this report. Any materials we file with the Securities and Exchange Commission (“SEC”) may be read at the SEC’s Public Reference Room at 100 F Street, NE, Room 1580 Washington, DC 20549. Information on the operation of the Public Reference Room may be obtained by calling the SEC at 1-800-SEC-0330. Certain materials we file with the SEC may also be read and copied at or through our website or at the Internet website maintained by the SEC at www.sec.gov.
History
We are an Ohio corporation and were incorporated in June 1959. In fiscal 2001 we redirected our business strategy toward healthcare services in the United States. On February 1, 2001, we purchased five community hospitals, leasehold rights for a sixth hospital and the related businesses of all six hospitals. On October 3, 2003, we acquired two additional hospitals through our acquisition of HealthMont, Inc. In June 2004, we sold our Mountainside Medical Center (“Mountainside”) facility, a 35-bed hospital located in Jasper, GA. In April 2008, our SunLink ScriptsRx, LLC subsidiary acquired Carmichael’s Cashway Pharmacy, Inc. (“Carmichael”). Carmichael provides services to patients in rural communities in southwest Louisiana and eastern Texas. In September 2009, we sold three of our home health businesses. In March 2011, we sold our Clanton Hospital (“Clanton”) operations but retained ownership of the hospital building. The hospital building is leased to the buyer of Clanton.
Business Strategy: Strategic Alternatives, Operations, Acquisitions and Dispositions
SunLink’s business strategy is to focus its efforts on internal operations of its existing healthcare facilities and its pharmacy business, supplemented by growth from potential healthcare acquisitions, including but not limited to hospitals, physician clinics, ambulatory surgery centers, nursing homes and pharmacy businesses. However, as was the case in 2004 with our Mountainside Medical Center hospital, in September 2009 with the sale of three home health agencies and in March 2011 with the sale of our Clanton Hospital operations, we
6
Index to Financial Statements
consider dispositions of one or more of our facilities or operations based on a variety of factors including asset values, return on investments, competition from existing and potential facilities, capital improvement needs, corporate strategy and other corporate objectives.
On April 8, 2011, SunLink Health Systems, Inc. announced that it has reached a preliminary agreement and executed a letter of intent with Foundation HealthCare Affiliates, LLC (“Foundation”) and New Age Fuel, Inc. (“New Age”), and Foundation Investment Affiliates I, LLC (“FIA”) for the non-cash merger of certain Foundation and New Age, FIA, subsidiaries and affiliates with and into newly formed acquisition subsidiaries of SunLink. The contemplated transaction is subject to a number of conditions, including completion of due diligence by each of the parties, negotiation and execution of a definitive merger agreement and consent of lenders. The subsidiaries and affiliates of Foundation contemplated to be merged into the SunLink acquisition subsidiaries per the letter of intent own minority equity interests in and manage 14 ambulatory surgery centers in seven states (Louisiana, Maryland, New Jersey, Ohio, Oklahoma, Pennsylvania and Texas), own a majority interest in and manage one general acute care hospital and manage a second acute care hospital, both of which are located in Texas. Three medical real properties, which are occupied by Foundation entities as well as other tenants in Oklahoma, are majority owned by New Age and FIA and would also be merged into the SunLink acquisition subsidiaries.
Under the Letter of Intent, the merger consideration to be issued by SunLink to the owners and affiliates of Foundation and New Age was contemplated to consist of approximately 1,560,000 SunLink common shares, approximately 133,000 shares of SunLink’s non-voting cumulative 5% Series A Preferred Stock, liquidation value $100.00 per share; approximately 277,000 shares of SunLink’s non-voting non-cumulative 4% Series B Preferred Stock, liquidation value $100.00 per share; and 3,000,000 Series A Warrants each of which would entitle the holder for three years to buy one SunLink common share at an exercise price of $6.00. In connection with the mergers, as was contemplated under the Letter of intent, SunLink would declare a stock dividend, issuing to its existing holders of common shares (as of a record date to be established), approximately 133,600 shares of its Series A Preferred Stock, approximately 79,900 shares of its Series B Preferred Stock, and 3,000,000 Series B Warrants each of which will entitle the holder for three years to buy one SunLink common share at an exercise price of $6.50.
Subsequent to execution of the letter of intent, SunLink effected a private placement of 1.3 million plus common shares at an average of approximately $1.90 per share with certain of its officers and directors and/or their affiliates. The proceeds of the private placement of approximately $2,500 were used, together with other available operating funds, to make an $8,000 pre-payment on the term loan outstanding under SunLink’s 2008 Credit Facility in order to, among other things, obtain the extension of the maturity of that facility and adjust certain financial covenants to bring SunLink into compliance thereunder. Given the inadequate number of authorized but unissued SunLink common shares presently remaining after the private placement, it is currently anticipated that, among other things, the merger consideration consisting of SunLink preferred shares will be correspondingly increased and the composition of the Foundation, New Age and FIA, subsidiaries and affiliates to be merged will be modified in certain particulars to be agreed.
No approval by the shareholders of SunLink is required for the proposed mergers. However, the Series B Preferred Stock will be automatically converted into common shares of SunLink at a to be agreed conversion price , such conversion to be effected upon receipt of approval of the common shareholders of SunLink. Similarly, the Series A and Series B Warrants would not be exercisable unless and until the exercise of such warrants for SunLink common shares is approved by the common shareholders of SunLink. Promptly following closing of the mergers, SunLink intends to seek such approval by its common shareholders of conversion of the Series B Preferred Stock into SunLink common shares and of the right of the holders to the exercise of the Series A and Series B Warrants after the mergers.
Upon completion of the mergers, the combined company would expect to change its name to Foundation SunLink Healthcare Affiliates, Inc. In addition, it is anticipated that two persons designated by Foundation/New
7
Index to Financial Statements
Age will join the board of directors of SunLink. Foundation SunLink is intended to be a premier healthcare facilities company positioned to respond to the changing marketplace developing under healthcare reform. Foundation SunLink’s mission will be to more closely align the interests of physicians, hospitals and related healthcare facilities to improve the quality of care and control healthcare costs in communities it serves. It is anticipated that Foundation SunLink will focus on growth through physician-centric hospitals, surgery centers and related ancillary service providers, including its existing hospitals and surgery centers, plus the aggressive acquisition and development of additional physician-centric hospitals, surgery centers and ancillary service providers nationwide.
No definitive agreement has been executed in relation to the contemplated mergers and there can be no assurance that the proposed transactions will in fact be consummated or, if consummated, that the terms and conditions referenced herein will not be changed.
Operations Strategy
Our operational strategy is focused on efforts to improve operations and generate internal growth. Our primary operational strategy for our community hospitals is to improve the operations and profitability of such hospitals by reducing out-migration of patients, recruiting physicians, expanding services and implementing and maintaining effective cost controls. Our operational strategy for our nursing homes and home health agency is similar to that for our community hospitals and is focused on expanding services and implementing and maintaining effective cost controls. Our operational strategy for our Specialty Pharmacy segment is focused on increasing market share, expanding services, and implementing and maintaining effective cost controls.
Acquisition and Disposition Strategy
Although the Company’s situation could change, based on its current financial position as well as uncertainties in the healthcare industry, the Company is not actively seeking acquisitions for its Healthcare Facilities or Specialty Pharmacy Segments. However, during the last fiscal year, we evaluated certain rural and exurban hospitals and healthcare businesses, which were for sale and monitored other selected healthcare acquisition targets which we believed might become available for sale.
When we seek to acquire pharmacy businesses, our acquisition strategy is to acquire such businesses in rural or exurban markets where the acquisition is complementary to our existing pharmacy services and in new markets where the scale of the acquisition is sufficient to provide a foundation to grow Specialty Pharmacy in that area.
Although we have no current plans to do so, from time to time we may consider the acquisition of other complementary based healthcare businesses, outside of our existing business segments, which are or may become available for acquisition.
We continue to engage in similar evaluation and monitoring activities with respect to hospitals, nursing homes, home health businesses, pharmacy and other rural or exurban healthcare businesses, which are or may become available for acquisition.
Historically, we targeted the rural or exurban community hospital market because we believed it provided an attractive sector for investment in healthcare facilities. We continue to believe hospitals and other healthcare businesses in our markets generally experience (1) less direct competition, (2) lower managed care penetration, (3) more manageable inflationary pressure with respect to certain costs, (4) higher staff, employee and community loyalty, and (5), in certain cases, opportunity for future growth. The focus of acquisition activities will depend on our evaluation of relative opportunities for growth and profitability within the business segments and services lines of our existing operations, the capital needs of our existing and potential operations within such existing and potential segments and services lines, current and potential changes in government regulation and reimbursement rules, competition for potential acquisitions and valuations of existing or potential new healthcare related facilities and operations and other factors.
8
Index to Financial Statements
Extensive competition may exist for healthcare facility acquisitions, primarily from for-profit management companies and not-for-profit entities which may have greater financial and other resources than SunLink. Competition for the acquisition of non-urban acute-care hospitals and other healthcare facilities could have an adverse impact on our ability to acquire such hospitals and other healthcare facilities on favorable terms or at all.
We believe there may be opportunities for acquisitions or dispositions of individual hospitals in the future due to, among other things, continued negative trends in certain government reimbursement programs and other factors. We also believe there may be opportunities for the acquisition or disposition of individual or groups of hospitals in the future as other for-profit hospital operators seeking to re-align the focus of their portfolios.
Opportunities to acquire not-for-profit hospitals remain uncertain. Even if such opportunities improve, in recent years, the legislatures and attorneys general of several states (including Georgia and other states which we believe might have suitable acquisition targets) have shown a heightened level of interest in reviewing transactions involving the sale of not-for-profit hospitals. The legal authority for such review is generally known as Conversion Legislation. Although the level of authority for, and interest in, such reviews varies from state to state, the trend is toward increased governmental authority for review and review of such transactions including, in some cases, the imposition of requirements on the seller, the buyer or both as a condition to the approval of a not-for-profit corporation selling a healthcare facility. Accordingly, even if the opportunity or desirability of acquiring not-for-profit hospitals improves, governmental review may make it more difficult or expensive to complete any such acquisitions.
Our acquisition strategy for nursing homes operations is to acquire businesses in areas which are complementary to either our existing hospitals or our pharmacy business or which are located in markets which we perceive as desirable.
As noted above, from time to time we may consider the disposition of one or more of our healthcare facilities, service lines or business segments, particularly if we determine that the operating results or potential growth of such facility, service line or segment no longer meet our business objectives.
Healthcare Facilities Operations
SunLink’s Healthcare Facilities Segment is composed of three operational areas:
| • | Our six community hospitals; |
| • | Our three nursing homes, each of which is located adjacent to, or in close proximity with a corresponding SunLink community hospital; and |
| • | One hospital related home health agency, which operates for a corresponding SunLink community hospital; |
In addition, we own one hospital facility which is leased to a third party, which owns the hospital license for the facility, with an option to purchase.
Through our subsidiaries, we operate a total of six community hospitals in three states. Five of the community hospitals are owned and one is leased. SunLink’s community hospitals are acute care hospitals and have a total of 342 licensed beds. We also own one 60 licensed bed hospital building that is leased to a third party with an option to purchase at the end of the lease. In connection with our community hospital operations in certain communities, we also operate (a) three nursing homes located in two states: each of our current nursing homes is located adjacent to our community hospitals, and (b) one home healthcare agency operated from one of our community hospitals. Our nursing homes have a total of 261 licensed beds.
Owned and Leased Hospitals
All of our hospitals which we operate are owned except Missouri Southern Healthcare, which is a leased hospital. The following sets forth certain information with respect to each of our six community hospitals which we operate:
| • | Chestatee Regional Hospital (“Chestatee”), located in Dahlonega, Lumpkin County, Georgia, is a 49-licensed-bed, acute-care hospital accredited by the Joint Commission on Accreditation of Healthcare |
9
Index to Financial Statements
| Organizations (the “JCAHO”). It includes a 12-bed obstetric department, a four-bed intensive care unit (“ICU”) and a 33-bed medical/surgical/pediatrics unit. Chestatee is the only hospital in its primary service area of Lumpkin and Dawson Counties. |
| • | North Georgia Medical Center (“North Georgia”), located in Ellijay, Gilmer County, Georgia, consists of a JCAHO accredited 50-licensed-bed, acute-care hospital and Gilmer Nursing Home, a 100-bed skilled nursing facility. North Georgia is the only hospital in Gilmer County. The Company has a 24-bed Certificate of Need (“CON”) to replace the existing hospital and a 10-bed inpatient geriatric psychiatric program. |
| • | Trace Regional Hospital (“Trace”), located in Houston, Chickasaw County, Mississippi, consists of a JCAHO accredited 84-licensed-bed, acute-care hospital and Floy Dyer Manor Nursing Home, a 66-bed nursing home. Trace is the only hospital in Chickasaw County. |
| • | Missouri Southern Healthcare (“Missouri Southern”), located in Dexter, Stoddard County, Missouri, is a 50-licensed-bed, acute-care hospital. It includes a four-bed ICU. It is the only hospital in Dexter, Missouri. The lease expires in 2019. It operates a home-health agency. |
| • | Callaway Community Hospital (“Callaway”), located in Fulton, Callaway County, Missouri, is a 49-licensed-bed, JCAHO accredited, acute-care hospital. Callaway is the only hospital in Callaway County. |
| • | Memorial Hospital of Adel (“Adel”), located in Adel, Cook County, Georgia, consists of a JCAHO accredited 60-licensed-bed, acute-care hospital and Memorial Convalescent Center, a 95-bed skilled nursing facility. Adel is the only hospital in Cook County. |
We also own the Chilton Medical Center (“Chilton”) hospital building located in Clanton, Chilton County, Alabama which we lease to a third party. Chilton is a 60-licensed-bed, JCAHO accredited, acute-care hospital. The third party has the option to purchase the facility. Chilton is the only hospital in Chilton County.
Hospital Operations
Utilization of Local Hospital Management Teams
We believe that the long-term potential of our hospitals is dependent on their ability to offer appropriate healthcare services and effectively recruit and retain physicians. Each SunLink hospital has developed and continuously seeks to implement an operating plan designed to improve efficiency and increase revenue including, but not limited to, the expansion of services offered by the hospital and the recruitment of physicians to the community.
Each hospital management team is comprised of a chief executive officer, chief financial officer and chief nursing officer. The quality of the on-site hospital management team is critical to the success of our hospitals. The on-site management team is responsible for implementing the operating plan under the guidance of SunLink’s senior management team. Each hospital management team participates in a performance-based compensation program based upon the achievement of operational, clinical and financial goals set forth in the operating plan.
Each hospital management team is responsible for the day-to-day operations of its hospital. Our corporate staff provides support services, assistance, and advice to each hospital in certain areas, including strategic planning, physician recruiting and relationship management, corporate compliance, reimbursement, information systems, human resources, accounting, cash management, capital financing, tax and insurance. Financial controls are maintained through the utilization of standardized policies and procedures and monitoring by corporate staff. Our hospitals have contracted with the HealthTrust Group Purchasing Organization, a purchasing group used by a large number of community hospitals, for certain supplies and equipment. We promote communication among our hospitals and management teams so that local expertise and improvements can be shared among all of our facilities.
10
Index to Financial Statements
Expansion of Services and Facilities
We seek to add services at our hospitals on an as-needed basis in order to improve access to quality healthcare services in the communities we serve, with the ultimate goal of reducing the out-migration of patients to other hospitals or alternate service providers. Additional and expanded services and programs, which may include specialty inpatient and outpatient services, are often dependent on recruiting physicians; therefore, physician recruiting goals are important to our ability to expand services. Capital investments in technology and facilities are often necessary to increase the quality and scope of services provided to the communities. Additional and expanded services and improvements add to each hospital’s quality of care and reputation in the community, reducing out-migration and increasing patient referrals and revenue. SunLink provides emergency room services in each of our hospitals. We seek to maintain a quality, patient-friendly emergency room because we view the emergency room as each facility’s “window to the community” and a critical component of its local service offering.
Medical Staff
The number and quality of physicians affiliated with a hospital directly affects the quality and availability of patient care and the reputation of the hospital. Physicians generally may terminate their affiliation with a hospital at any time. We seek to retain primary care physicians of varied physician specialties on the medical staffs of our hospitals and to attract other qualified physicians. SunLink believes physicians refer patients to a hospital primarily on the basis of the quality of services the hospital renders to patients and physicians; the quality of other physicians on the medical staff; the location of the hospital; and the quality of the hospital’s facilities, equipment and employees. Accordingly, SunLink strives to provide quality facilities, equipment, employees and services for physicians and their patients.
Physician Recruiting
Each SunLink hospital management team is responsible for assessing the need for additional physicians, including the number and specialty of additional physicians needed by the hospital’s community. Each of our local hospital management teams, with the assistance of outside recruiting firms and corporate staff, identifies and seeks to attract specific physicians to its hospital’s medical staff. While our hospitals historically have not employed physicians, we have moved forward to better align with physicians through employment relationships. The new business model for many hospitals and hospital systems is to gain closer alignment with physicians both clinically and financially. The hospital generally guarantees a newly recruited physician a minimum level of gross receipts during an initial period, generally one year, and assists the physician’s transition into the community. The physician is required to repay some or all of the amounts paid under such guarantee if the physician leaves the community within a specified period. Currently, 28 physicians are employed by the hospitals and 2 are under physician guarantee contracts. We continually evaluate each doctor and may terminate employment based on doctor performance and the needs of each facility. The Company believes physician recruiting is becoming more challenging and will continue to do so due to healthcare reform and market forces. The Company believes the costs of recruiting and retaining physicians will increase as more physicians are employed and salaries and support costs increase.
Quality Assurance
Each SunLink hospital implements quality assurance procedures to monitor the level and quality of care provided to its patients. Each hospital has a medical director who supervises and is responsible for the quality of medical care provided and a medical advisory committee comprised of physicians who review the professional credentials of physicians applying for medical staff privileges at the hospital. The medical advisory committee also reviews and monitors surgical outcomes along with procedures performed and the quality of the logistical, medical and technological support provided to the physicians. Each hospital periodically conducts surveys of its patients, either during their stay at the hospital or subsequently by mail, to identify potential areas of improvement. Each SunLink hospital, except the leased hospital in Dexter, Missouri, is accredited by the Joint Commission of Accreditation of Healthcare Organizations, also known as JCAHO.
11
Index to Financial Statements
Operating Statistics
The following table sets forth certain operating statistics for SunLink’s healthcare facilities included in continuing operations as of June 30, 2011 for the periods indicated.
| Fiscal Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Hospitals owned or leased at end of period |
6 | 6 | 6 | |||||||||
| Licensed hospital bed (at end of period) |
342 | 342 | 342 | |||||||||
| Hospital beds in service (at end of period) |
283 | 292 | 292 | |||||||||
| Nursing home beds in service (at end of period) |
261 | 261 | 261 | |||||||||
| Admissions |
6,197 | 6,818 | 7,683 | |||||||||
| Equivalent Admissions(1) |
18,702 | 20,062 | 20,343 | |||||||||
| Average Length of Stay(2) |
3.5 | 3.5 | 3.5 | |||||||||
| Patient days |
21,388 | 24,149 | 26,736 | |||||||||
| Adjusted patient days(3) |
63,821 | 70,084 | 70,013 | |||||||||
| Occupancy rate (% of licensed beds)(4) |
17.13 | % | 19.35 | % | 21.42 | % | ||||||
| Occupancy rate (% of beds in service)(5) |
20.71 | % | 22.66 | % | 25.09 | % | ||||||
| Net patient service revenues (in thousands) |
$ | 141,241 | $ | 140,556 | $ | 135,431 | ||||||
| Net outpatient service revenues (in thousands) |
$ | 59,299 | $ | 67,225 | $ | 63,689 | ||||||
| Net revenue per equivalent admissions |
$ | 7,552 | $ | 7,006 | $ | 6,657 | ||||||
| Net outpatient service revenues (as a % of net patient service revenues) |
41.98 | % | 47.83 | % | 47.03 | % | ||||||
| (1) | Equivalent admissions are a statistic used by management (and certain investors) as a general approximation of combined inpatient and outpatient volume. Equivalent admissions are computed by multiplying admissions (inpatient volume) by the sum of gross inpatient revenues and gross outpatient revenues and dividing the result by gross inpatient revenues. The equivalent admissions computation is intended to relate outpatient revenues to the volume measure (admissions) used to measure inpatient volume resulting in a general approximation of combined inpatient and outpatient volume. |
| (2) | Average length of stay is calculated based on the number of patient days divided by the number of admissions. |
| (3) | Adjusted patient days have been calculated based on a revenue-based formula of multiplying actual patient days by the sum of gross inpatient revenues and gross outpatient revenues and dividing the result by gross inpatient revenues for each hospital. Adjusted patient days is a statistic (which is used generally in the industry) designed to communicate an approximate volume of service provided to inpatients and outpatients by converting total patient revenues to a number representing adjusted patient days. |
| (4) | Percentages are calculated by dividing average daily census by the average number of licensed beds. |
| (5) | Percentages are calculated by dividing average daily census by the average number of beds in service. |
Sources of Revenue
Each SunLink hospital receives payments for patient care from Federal Medicare programs, State Medicaid programs, private insurance carriers, health maintenance organizations, preferred provider organizations, TriCare, and from employers and patients directly. Medicare is a Federal program that provides certain hospital and medical insurance benefits to persons age 65 and over, some disabled persons and persons with end-stage renal disease. Medicaid is a Federal-state program, administered by the states, that provides hospital and nursing home benefits to qualifying individuals who are unable to afford care. All of SunLink’s hospitals are certified as healthcare services providers for persons covered by Medicare and Medicaid programs. TriCare is a Federal program for the healthcare of certain U.S. military personnel and their dependants. See “Item 7 Management’s Discussion and Analysis of Financial Condition and Results of Operations”.
12
Index to Financial Statements
The following table sets forth the percentage of patient days from various payors in SunLink’s healthcare facilities for the periods indicated.
| Fiscal Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Source |
||||||||||||
| Medicare |
70.8 | % | 71.4 | % | 71.4 | % | ||||||
| Medicaid |
11.5 | % | 10.6 | % | 9.6 | % | ||||||
| Private and Other Sources |
17.7 | % | 18.0 | % | 19.0 | % | ||||||
|
|
|
|
|
|
|
|||||||
| 100.0 | % | 100.0 | % | 100.0 | % | |||||||
|
|
|
|
|
|
|
|||||||
The following table sets forth the percentage of the net patient revenues from major payors in SunLink’s hospitals.
| Fiscal Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Source |
||||||||||||
| Medicare |
43.2 | % | 39.1 | % | 40.2 | % | ||||||
| Medicaid |
14.3 | % | 12.9 | % | 14.9 | % | ||||||
| Private and Other Sources |
42.5 | % | 48.0 | % | 44.9 | % | ||||||
|
|
|
|
|
|
|
|||||||
| 100.0 | % | 100.0 | % | 100.0 | % | |||||||
|
|
|
|
|
|
|
|||||||
Hospital revenues depend upon inpatient occupancy levels, the extent to which ancillary services and therapy programs are ordered by physicians and provided to patients, and the volume of outpatient procedures. Reimbursement rates for routine inpatient services vary significantly depending on the type of service (e.g., acute care, intensive care or psychiatric care) and the geographic location of the hospital. The percentage of patient revenues attributable to outpatient services has increased in recent years, primarily as a result of medical technology advances that allow more services to be provided on an outpatient basis and from increased pressures from Medicare, Medicaid and private insurers to reduce hospital stays and provide services, where possible, on a less expensive outpatient basis.
Patients generally are not responsible for any difference between established hospital charges and amounts reimbursed for such services under Medicare, Medicaid and some private insurer plans, health maintenance organization (“HMO”) plans and preferred provider organizations(“PPO”) plans, but are responsible to the extent of any exclusions, deductibles or co-insurance features of their coverage. The amount of such exclusions, deductibles and co-insurance has been increasing in recent years. Collection of amounts due from individuals typically is more difficult than from governmental or third-party payors. Further, amounts received under the Medicare and Medicaid programs generally are significantly less than the established charges of most hospitals, including our own, for the services provided. Likewise, HMOs and PPOs generally seek and obtain discounts from the established charges of most hospitals. See “Item 1. Business—Government Reimbursement Programs—Medicare/Medicaid Reimbursement”.
Competition
Among the factors which we believe influence patient selection among hospitals in our markets are:
| • | The appearance and functionality of the healthcare facilities; |
| • | The quality and demeanor of professional staff and physicians; and |
| • | The participation of the hospital in plans which pay a portion of the patient’s bill. |
13
Index to Financial Statements
Such factors are influenced heavily by the quality and scope of medical services, strength of referral networks, hospital location and the price of hospital services. Our hospitals may face less competition in their immediate patient service areas than would be expected in larger communities because they are the primary provider of healthcare services in their respective communities. However, our hospitals usually face competition from larger tertiary care centers and, in some cases, other rural, exurban, suburban or, in limited circumstances, urban hospitals, some of which offer more specialized services. The competing hospitals may be owned by governmental agencies or not-for-profit entities supported by endowments and charitable contributions and may be able to finance capital expenditures on a tax-exempt basis. Such governmental-owned and not-for-profit hospitals, as well as various for-profit hospitals operating in the broader service area of our hospitals, likely have greater access to financial resources than do our hospitals.
Managed Care
Each SunLink hospital is affected by its ability to negotiate service contracts with purchasers of group healthcare services. HMOs and PPOs attempt to direct and control the use of hospital services through managed care programs. In addition, employers and traditional health insurers increasingly are seeking to contain costs through negotiations with hospitals for managed care programs and discounts from established charges. Generally, hospitals compete for service contracts with group healthcare service purchasers on the basis of market reputation, geographic location, quality and range of services, quality of medical staff, convenience and price.
The importance of obtaining contracts with managed care organizations varies from market to market, depending on the market strength of such organizations. Management believes that, on an industry basis, managed care contracts generally are less important in our markets than in urban and suburban markets where there is typically a higher level of managed care penetration. Nevertheless, a significant portion of hospital patients in our communities are covered by managed care or other reimbursement programs, all of which generally pay less than established charges for hospital services.
The healthcare industry as a whole faces the challenge of continuing to provide quality patient care while managing rising costs, facing strong competition for patients, and adjusting to a continued general reduction of reimbursement rates by both private and government payors. Both private and government payors continually seek to reduce the nature and scope of services which may be reimbursed. Healthcare reform at both the Federal and state level generally has created pressure to reduce reimbursement rates. Changes in medical technology, existing and future legislation, regulations and interpretations, and competitive contracting for provider services by private and government payors, may require changes in our facilities, equipment, personnel, rates and/or services in the future.
Efforts to Control Healthcare Costs
The hospital industry, including all of SunLink’s hospitals, continues to have significant unused capacity. Inpatient utilization, average lengths of stay and average inpatient occupancy rates continue to be affected negatively by payor-required pre-admission authorization, utilization review, and payment mechanisms designed to maximize outpatient and alternative healthcare delivery services for less acutely ill patients and to limit the cost of treating inpatients. Admissions constraints, payor pressures, and increased competition are likely to continue. Historically we have responded to such trends by adding and expanding outpatient services, upgrading facilities and equipment, offering new programs and adding or expanding certain inpatient and ancillary services. Currently we expect to continue to respond to such trends in a similar manner subject to the availability of capital resources and our evaluation of the continued utility of such historical responses.
14
Index to Financial Statements
Health Care Reform
The Patient Protection and Affordable Care Act and the Health Care Education Reconciliation Act of 2010 (collectively, the “Affordable Care Act” or “ACA”) were signed into law by President Obama on March 23, 2010, and March 30, 2010, respectively. The ACA dramatically alters the United States health care system and is intended to decrease the number of uninsured Americans and reduce overall health care costs. The ACA attempts to achieve these goals by, among other things, requiring most Americans to obtain health insurance, expanding Medicare and Medicaid eligibility, reducing Medicare and Medicaid payments, including disproportionate share payments, expanding the Medicare program’s use of value-based purchasing programs, tying hospital payments to the satisfaction of certain quality criteria, and bundling payments to hospitals and other providers. The ACA also contains a number of measures that are intended to reduce fraud and abuse in the Medicare and Medicaid programs, such as requiring the use of recovery audit contractors in the Medicaid program and generally prohibiting physician-owned hospitals from adding new physician owners or increasing the number of beds and operating rooms for which they are licensed. Because a majority of the measures contained in the ACA do not take effect until 2013 and 2014 and most of the rules and regulations that implement the provisions of the ACA have not been adopted or proposed, it is difficult to predict the impact the ACA will have on our facilities. However, it is possible that the implementation or interpretation of such rules and regulations or the provisions of the ACA could have an adverse effect on our financial condition and results of operations.
Government Reimbursement Programs
A significant portion of SunLink’s healthcare facilities net revenues are dependent upon reimbursement from Medicare and Medicaid. The Centers for Medicare and Medicaid Services or “CMS” is the federal agency which administers Medicare, Medicaid and the Children’s Health Insurance Program (“CHIP”). Although the Federal government generally reviews payment rates under its various programs annually, changes in reimbursement rates under such programs, including Medicare and Medicaid, generally occur based on the fiscal year of the Federal government which currently begins on October 1 and ends on September 30 of each year.
Medicare Inpatient Reimbursement
The Medicare program pays hospitals under the provisions of a prospective payment system for inpatient services. Under the inpatient prospective payment system, a hospital receives a fixed amount for inpatient hospital services based on the established fixed payment amount per discharge for categories of hospital treatment, known as diagnosis related groups (“DRGs”). Each patient admitted for care is assigned to a DRG based upon his or her primary admitting diagnosis. Every DRG is assigned a payment rate by the government based upon the estimated intensity of hospital resources necessary to treat the average patient with that particular diagnosis. DRG payments do not consider a specific hospital’s costs, but are national rates adjusted for area wage differentials and case-mix indices.
DRG rates are usually adjusted by an update factor each Federal fiscal year. The percentage increases to DRG payment rates for the last several years have been lower than the percentage increases in the related cost of goods and services provided by general hospitals. The index used to adjust the DRG payment rates is based on a price statistic, known as the CMS Market Basket Index, reduced by congressionally mandated reduction factors.
DRG rate increases were 2.1% and 2.35% for Federal fiscal years (“FFY”) 2010 and 2011, respectively, and currently is 1.1% for FFY 2012. The Balanced Budget Act of 1997 originally set the increase in DRG payment rates for future Federal fiscal years at rates that would be based on the market basket index, which in certain years have been, and in the future may be, subject to reduction factors. In FFY 2012 the market basket rate currently is affected by two such reduction factors. First as required by the Affordable Care Act, the market basket rate is reduced by 0.25%. Second, CMS is applying a “documentation and coding” adjustment to recoup a portion of excess aggregate payments in FFY 2008 and FY 2009 that did not reflect actual increases in patients’ severity of illness. Under legislation passed in 2007, CMS is required to recoup the entire amount of FFY 2008
15
Index to Financial Statements
and 2009 excess spending resulting from changes in hospital coding practices no later than FFY 2012. If the update factor does not adequately reflect increases in SunLink’s cost of providing inpatient services, our financial condition or results of operations could be negatively affected.
The ACA made a number of changes to Medicare which include but are not limited to:
| • | Reduction of market basket updates in Medicare payment rates for providers and incorporate adjustment for expected productivity gains. The market basket was reduced by 0.25% for both FFY 2010 and 2011, and will be reduced by 0.10% in FFYs 2012 and 2013, by 0.30% in FFY 2014, by 0.20% in 2015 and 2016, and by 0.75% in FFYs 2017-2019. |
| • | Reduction of Medicare payments that would otherwise be made to hospitals by specified percentages to account for preventable hospital readmissions, effective October 1, 2012. |
| • | Extension of the Medicare Dependent Hospital Program until September 30, 2012. |
| • | Expansion, on a temporary basis, of the low volume hospital inpatient payment adjustment to include hospitals that are more than 15 miles from other healthcare facilities and have less than 1,600 discharges per year. The new temporary criteria are effective for FFYs 2011 and 2012. |
Each of SunLink’s hospitals is an eligible hospital under one or more provisions of ACA.
Medicare Outpatient Reimbursement
Most outpatient services provided by general hospitals are reimbursed by Medicare under the outpatient prospective payment system. This outpatient prospective payment system is based on a system of Ambulatory Payment Classifications (“APC”). Each APC is designed to represent a “bundle” of outpatient services, and each APC is assigned a fully prospective reimbursement rate. Medicare pays a set price or rate for each APC group, regardless of the actual cost incurred in providing care. Each APC rate generally is subject to adjustment each year by an “update factor” based on a market basket of services index. For calendar years 2008, 2009, 2010 and 2011 the update factors were 3.3%, 3.6%, 2.1% and 2.6% respectively. If the update factor does not adequately reflect increases in SunLink’s cost of providing outpatient services, our financial condition or results of operations could be negatively affected.
Medicare Bad Debt Reimbursement
Under Medicare, the costs attributable to the deductible and coinsurance amounts that remain unpaid by Medicare beneficiaries can be added to the Medicare share of allowable costs as cost reports are filed. Hospitals generally receive interim pass-through payments during the cost report year which were determined by a fiscal intermediary from the prior cost report filing.
Bad debts must meet the following criteria to be allowable:
| • | the debt must be related to covered services and derived from deductible and coinsurance amounts; the provider must be able to establish that reasonable collection efforts were made; |
| • | the debt was actually uncollectible when claimed as worthless; and |
| • | sound business judgment established that there was no likelihood of recovery at any time in the future. |
Amounts uncollectible from specific beneficiaries are charged off as bad debts in the accounting period in which the accounts are deemed to be worthless. In some cases, an amount previously written off as a bad debt and allocated to the program may be recovered in a subsequent accounting period. In these cases, the recoveries must be used to reduce the cost of beneficiary services for the period in which the collection is made. In determining reasonable costs for hospitals, the amount of bad debts otherwise treated as allowable costs is reduced by 30%. Under this program, our hospitals received an aggregate of approximately $1,442, $1,823 and $988 for 2010, 2009 and 2008, respectively.
16
Index to Financial Statements
Medicare Disproportionate Share Payments
In addition to the standard DRG payment, the Social Security Act requires that additional Medicare payments be made to hospitals with a disproportionate share of low income patients. Beneficiary Improvement and Protection Act (“BIPA”) provisions, effective for services provided on and after April 1, 2001, stipulate that rural facilities with fewer than 100 beds with a disproportionate share percentage greater than 15% will be classified as a disproportionate share hospital entitled to receive a supplemental disproportionate share payment based on gross DRG payments. Since April 1, 2004, the effective rate has been 12.0% of DRG payments. All of our hospitals were classified as disproportionate share hospitals at June 30, 2011. Furthermore, the Affordable Care Act provides for material reductions in Medicare DSH funding. However, we estimate that Medicare disproportionate share payments represented only approximately 1% of our net patient service revenues for the years ended June 30, 2011, 2010 and 2009.
Medicaid Inpatient and Outpatient Reimbursement
Each state operates a Medicaid program funded jointly by the state and the Federal government. Federal law governs the general management of the Medicaid program, but there is wide latitude for states to customize Medicaid programs to fit local needs and resources. As a result, each state Medicaid plan has its own payment formula and recipient eligibility criteria.
In the recent past, the various states in which SunLink operates hospitals have initiated increased efforts to reduce Medicaid assistance payments. These efforts and reductions often are triggered by one or more of the following factors: an increased effort by CMS to decrease the federal share of payments for Medicaid beneficiaries and significant increases in program utilization resulting from increased enrollment or budgetary pressures on the applicable states. The Federal government’s percentage share of each state’s medical assistance expenditures under Medicaid is determined by a formula specified in Medicaid law referred to as the Federal Medical Assistance Percentage (“FMAP”).
On February 17, 2009, President Obama signed into law the “American Recovery and Reinvestment Act of 2009” (“ARRA”) This law provides a temporary increase in the state FMAPs during a 9-calendar quarter recession adjustment period retroactively beginning October 1, 2008 and ending December 31, 2010.
Traditionally under the Medicaid law, each state’s FMAP is determined by a formula based on the relationship of each state’s per capita income to the national per capita income; the lower a state’s per capita income, the higher its FMAP. The FMAP is determined for each fiscal year and applies for states’ expenditures during that fiscal year. As a result of the temporary ARRA increase in the FMAP, reductions in Medicaid programs which were scheduled to take effect on July 1, 2009 in various states where SunLink operates were postponed until January 1, 2011.
The State of Georgia, where SunLink operates three hospitals, has begun initiatives to decrease the Medicaid funds paid to providers. Georgia Medicaid pays providers for inpatient services in a manner similar to the Medicare prospective payment system in that hospitals receive a fixed fee for inpatient hospital services based on the established fixed payment amount per discharge for categories of hospital treatment, also known as DRGs. These Medicaid DRG payments do not consider a specific hospital’s costs, but are statewide rates adjusted for each hospital’s capital cost allotment.
Medicaid outpatient services are reimbursed with interim rates based on a facility specific cost to charge ratio. These interim payments are then adjusted subsequent to the end of the cost reporting period to an amount equal to 85.6% of the costs associated with providing care to the Medicaid outpatient population.
In 2006, Georgia implemented a Medicaid HMO program and awarded contracts to private companies for the management and processing of certain Medicaid claims. The intent of the Medicaid HMO program is to curtail utilization and reduce rates paid by the State of Georgia. All of SunLink’s facilities that operate in the
17
Index to Financial Statements
state of Georgia have secured contracts with all the HMO companies contracted by the state in their respective regions. Since the implementation of the Medicaid HMO program, all SunLink hospitals receive reimbursement from three different contractors instead of a single source. While the amounts of the inpatient payments have not changed since the contractors utilize the same payment rates, the timing of the receipt of the payments has changed due to the multiple payors. For outpatient services, our hospitals have contracts with the three HMO vendors and services are reimbursed at 102% of the current interim rate as determined by the Georgia Department of Community Health.
Adoption of Electronic Health Records
The Health Information Technology for Economic and Clinical Health Act (the “HITECH Act”) was enacted into law on February 17, 2009 as part of the ARRA. The HITECH Act includes provisions designed to increase the use of electronic health records (“EHR”) by both physicians and hospitals. Beginning with FFY 2011 and extending through FFY 2016, eligible hospitals and critical access hospitals (“CAHs”) participating in the Medicare and Medicaid programs are eligible for reimbursement incentives based on successfully demonstrating meaningful use of its certified EHR technology. Conversely, those hospitals that do not successfully demonstrate meaningful use of EHR technology are subject to reductions in reimbursements beginning in FFY 2015. On July 13, 2010, the Department of Health and Human Services (“DHHS”) released final meaningful use regulations for EHR. Meaningful use criteria are divided into three distinct stages; I, II and III. The final rules specify the initial criteria for: physicians, eligible hospitals, and CAHs necessary to qualify for incentive payments; calculation of the incentive payment amounts; payment adjustments under Medicare for covered professional services and inpatient hospital services, eligible hospitals and CAHs which fail to demonstrate meaningful use of certified EHR technology; and other program participation requirements.
Attestation of Medicare meaningful use requirements for the first year (October 1, 2010 – September 30, 2011) began on April 18, 2011. Each of SunLink’s six hospitals and its formerly owned Chilton Medical Center registered for the program with CMS and on April 18, 2011 all successfully attested compliance with Part I of the Medicare EHR incentive program for such first year. As of June 30, 2011, SunLink has accrued Medicare EHR incentive reimbursement of $6,952 for the six hospitals as of June 30, 2011 and $731 for its formerly owned Chilton Medical Center. The Company has received $7,731 in EHR Medicare incentive reimbursements for the six hospitals and $790 for its formerly owned Chilton Medical Center for the fiscal year then ended.
The Company has also successfully attested to the meaningful use requirements for Medicaid programs for its two Missouri Hospitals and its formerly owned Chilton Medical Center in Alabama, The Company accrued Medicaid EHR reimbursement for Mississippi and Missouri in the amount of $1,102 collectively and $141 for its formerly owned Chilton Medical Center. No amount has been accrued for Georgia Medicaid EHR incentive payments since the reimbursement program has not yet been established by the state. The amounts accrued are the estimates of the incentive payments for the periods earned through June 30, 2011.
We intend to continue to comply with the EHR meaningful use requirements of the HITECH Act in time to qualify for all available incentive payments. We believe our compliance will result in significant costs including professional services focused on successfully designing and implementing our EHR solutions along with costs associated with the hardware and software components of the project. As a result of our prior expenditures on information technology systems, our previously existing information technology systems already possessed certain components required for meaningful use of EHR technology. We continue to refine our budgeted costs and the expected reimbursement associated with our use of EHR technology. We currently estimate that, at a minimum, the incremental total costs and capital expenditures incurred to comply with the EHR regulations will be recovered through improved reimbursement amounts over the projected lifecycle of our EHR technology initiative, although such incremental costs and capital expenditures, have to a great degree, predated the reimbursements.
18
Index to Financial Statements
Government Reimbursement Program Administration and Adjustments
The Medicare, Medicaid and TriCare programs are subject to statutory and regulatory changes, administrative rulings, interpretations and determinations, requirements for utilization review and changing governmental funding restrictions, all of which may materially increase or decrease program payments as well as affect the cost of providing services and the timing of payments under such programs.
All hospitals participating in the Medicare and Medicaid programs, whether paid on a reasonable cost basis or under a prospective payment system, are required to meet certain financial reporting requirements. Federal and, where applicable, state regulations require the submission of annual cost reports covering the revenues, costs and expenses associated with the services provided by each hospital to Medicare beneficiaries and Medicaid recipients.
Annual cost reports required under the Medicare and Medicaid programs are subject to routine audits which may result in adjustments to the amounts ultimately determined to be due under these reimbursement programs. These audits often require several years to reach the final determination of amounts due. Providers have rights of appeal and it is common to contest issues raised in audits of prior years’ cost reports. Although the final outcome of these audits and the nature and amounts of any adjustments are difficult to predict, we believe that we have made adequate provisions in our financial statements for adjustments that may result from these audits and that final resolution of any contested issues should not have a material adverse effect upon our financial condition or results of operations. Until final adjustment, however, significant issues may remain unresolved and previously determined allowances could become either inadequate or greater than ultimately required.
In 2005, CMS began using recovery audit contractors (“RACs”) to detect Medicare overpayments not identified through existing claims review mechanisms. The RAC program relies on private companies to examine Medicare claims filed by healthcare providers. The RAC program was made permanent by the Tax Relief and Health Care Act of 2006 will gradually roll-out in additional states. The Affordable Care Act expands the RAC program’s scope to include managed Medicare and to include Medicaid claims beginning June 1, 2010, and by requiring all states to establish programs to contract with RACs in 2011. Currently all states where SunLink operates have RAC programs, and all SunLink facilities have had requests from the various RACs to review claims. To date since the commencement of the RAC program SunLink has experienced losses in the aggregate from audit adjustments of less than $10.
RACs perform post-discharge audits of medical records to identify Medicare overpayments resulting from incorrect payment amounts, non-covered services, incorrectly coded services, and duplicate services. CMS has given RACs the authority to look back at claims up to three years old, provided that the claim was paid on or after October 1, 2007. Claims review strategies used by RACs generally include a review of high dollar claims, including inpatient hospital claims. As a result, a large majority of the total amounts recovered by RACs has come from hospitals. Claims identified as overpayments will be subject to the Medicare appeals process.
RACs are paid a contingency fee based on the overpayments they identify and collect. We expect that the RACs will continue to look closely at claims submitted by our facilities in an attempt to identify possible overpayments. Although we believe the claims for reimbursement submitted to the Medicare program are accurate, we cannot predict the results of any future RAC audits.
In addition, CMS employs Medicaid Integrity Contractors (“MICs”) to perform post-payment audits of Medicaid claims and identify overpayments. The Affordable Care Act increases federal funding for the MIC program for federal fiscal year 2011 and later years. In addition to RACs and MICs, the state Medicaid agencies and other contractors have also increased their review activities.
If SunLink or any of our facilities were found to be in violation of Federal or state laws relating to Medicare, Medicaid or similar programs, the facility and SunLink could be subject to substantial monetary fines, civil penalties and exclusion from future participation in the Medicare and Medicaid programs. Any such sanctions could have a material adverse effect on our financial condition or results of operations.
19
Index to Financial Statements
SPECIALTY PHARMACY OPERATIONS
Our Specialty Pharmacy Segment is operated through our SunLink ScriptsRx, LLC subsidiary and is a pharmacy operations segment composed of four material service lines:
| 1. | Specialty Pharmacy Services which ordinarily include one or more of the following elements: |
| • | The provision of products relating to infusion therapy, enteral feeding services, oncology and chemotherapy drug administration, cardiac, diabetes, pain management, wound care, and psychiatric services; |
| • | Pharmaceutical or biological products administered via non-oral means, which are frequently through injectable or infusion therapies; |
| • | Products delivered to patients via express package or hand delivery and requiring special handling such as constant refrigeration or having an extremely limited shelf life; |
| • | Products that generally are administered in a non-hospital setting, including physicians’ offices, specialty clinics or patient homes; |
| • | The provision of pharmaceuticals or biological products not managed under traditional outpatient prescription drug benefits; and |
| • | Therapies that require complex care, patient education and continuous monitoring. |
The major conditions these drugs treat include, but are not limited to: respiratory system weakness, cancer, HIV/AIDS, hemophilia, hepatitis C, multiple sclerosis, infertility, Crohn’s disease, rheumatoid arthritis, and growth hormone deficiency.
| 2. | Institutional Pharmacy Services, consisting of the provision of specialty and non-specialty pharmaceuticals and biological products to institutional clients or to patients in institutional settings such as nursing homes, hospices, and correctional facilities; |
| 3. | Durable Medical Equipment Services, consisting primarily of products for patient-administered home care such as oxygen concentrators services, continuous positive airway pressure or CPAP machines, nebulizers, diabetes management products and prosthetics; |
| 4. | Retail Pharmacy Products and Services, consisting primarily of walk-in sales at our three distribution facilities in Louisiana of complementary products including uniforms, non-specialty pharmaceuticals, vitamins, supplements and nutritionals. We view our retail pharmacy operations as a source of incremental revenue to us while providing value added service to our patients in the form of full service pharmacy offerings. |
Certain of the service lines in our Specialty Pharmacy Segment may overlap with our healthcare operations. Likewise, institutional pharmacy services may overlap with pharmacies in our healthcare facilities.
Government Reimbursement Programs
Our Specialty Pharmacy Business is subject to certain rules implemented by the Medicare Modernization Act (“MMA”) and, in the future may be subject to other rules previously implemented by MMA with respect to urban providers. Regulations implementing the cost containment mandates under the MMA reduced the reimbursement for healthcare providers in urban areas for a number of products and services which are also provided by our pharmacy operations and established a competitive bidding program for certain durable medical equipment provided under Medicare Part B in urban areas. Competitive bidding is intended to further reduce reimbursement for certain products and will likely decrease the number of companies permitted to serve Medicare beneficiaries in the competitive bidding areas (“CBAs”). CMS had planned to implement the competitive bidding program for Medicare durable medical equipment, prosthetics, orthotics, and supplies (“DMEPOS”) products and services with the goal of offering beneficiaries access to quality with lower
20
Index to Financial Statements
out-of-pocket costs. We were exempted under the Deficit Reduction Act of 2005 from the proposed competitive acquisition program for DMEPOS, but we cannot be sure such exemption will continue to be available in the future or that the program, if expanded in the future, would be expanded in its original form. If the program is expanded in the future, loss of the exemption could have an adverse effect on our financial condition or results of operation. The program has, however, been deferred indefinitely, and whether or not the program will be implemented in the future is unknown.
The MMA also created a Medicare prescription drug benefit (which began in 2006) and a prescription drug card program. Final rules implementing the portions of the MMA relating to the new prescription drug benefit were adopted in 2005.
Under MMA Medicare Part B covered drugs and biological products generally are paid based on the average sales price (“ASP”) methodology. The ASP methodology uses quarterly drug pricing data submitted to the CMS by drug manufacturers. CMS will supply contractors with the ASP drug pricing files for Medicare Part B drugs on a quarterly basis. Principal products paid under the ASP methodology include certain oncology and renal dialysis drugs. Although, there are exceptions to this general rule which are listed in the latest ASP quarterly change request (“CR”) document and which exceptions generally are paid on a cost basis, such exceptions have not been and are not expected to be material to our operations.
Beginning in January 2008, CMS’s outpatient prospective payment system began paying for most separately payable Medicare Part B drugs administered in a hospital outpatient setting at a reimbursement level of ASP plus 5% and ASP plus 6% in other settings. Such outpatient price represented a decrease from ASP + 6%.
Section 303(d) of the MMA also requires the implementation of a competitive acquisition program (the “Part B CAP”) for Medicare Part B drugs and biologicals not paid on a cost or prospective payment system basis. The Part B CAP is an alternative to the ASP methodology for acquiring certain Part B drugs which are administered incident to a physician’s services. Currently, the Part B CAP is a voluntary program that offers physicians the option to acquire many injectable and infused drugs they use in their practice from an approved Part B CAP vendor, thus reducing the time and cost of buying and billing for drugs. Currently, the CAP for Part B Drugs and Biologicals is only for injectable and infused drugs currently billed under Part B that are administered in a physician’s office, “incident to” a physician’s service.
In late 2005, CMS conducted the first round of bidding for approved Part B CAP vendors. The Part B CAP was implemented on July 1, 2006. The 2009-2011 CAP vendor bidding period concluded on February 15, 2008. CMS received several qualified bids; however, contractual issues with the successful bidders resulted in the 2009 program being postponed by CMS in September 2008. As a result, CAP drugs were not available from an approved CAP vendor for dates of service after December 31, 2008.
At least one Medicaid program has adopted, and other Medicaid programs, some states and some private payors may be expected to adopt, those aspects of the MMA that either result in or appear to result in price reductions for drugs covered by such programs. Adoption of ASP as the measure for determining reimbursement by Medicare and Medicaid programs for additional drugs sold by our specialty pharmacy operations could reduce revenue and gross margins and could materially affect our current average wholesale price (“AWP”) based reimbursement structure with private payors.
We cannot assure you that the ASP reimbursement methodology will not be extended to the provision of all specialty pharmaceuticals or to the specialty pharmaceuticals most often sold by our specialty pharmacy operations or that we will be able to operate our specialty pharmacy operations profitably at either existing or at lower reimbursement rates. Likewise, we cannot assure you that the Part B CAP program will not be extended to rural or exurban areas in general or to the areas in which we operate, or may seek to operate, in particular or that we would be able to meet the qualifications to become a Part B CAP vendor either now or at any time in the future.
21
Index to Financial Statements
Competition
There are many companies which provide one or more of the healthcare operations which comprise or may compete with our pharmacy operations. For example, home healthcare business companies, which may compete with our specialty pharmacy services, our durable medical equipment services operations or both, range in size from small entrepreneurial companies to rapidly expanding companies with strategies for national operations such as Amedisys, Inc., Apria Healthcare Group, Inc., Gentiva Health Services, Inc., and Walgreen Co. Specialty pharmacy companies range from local or regional pharmacies to large public companies such as Option Care, Inc., a subsidiary of Walgreen Co., CVS Caremark Corporation, Priority Healthcare Corporation and BioScrip, Inc. Institutional pharmacy companies likewise range from local or regional pharmacies to large public companies including PharMerica Corporation and Omnicare, Inc.
Healthcare Regulation
Overview
The healthcare industry is one of the largest industries in the United States and continues to attract much legislative interest and public attention. There are many factors that are highly significant to the healthcare industry including Medicare, Medicaid, and other public and private hospital cost-containment programs, proposals to limit healthcare spending and proposals to limit prices and increase industry competition. The healthcare industry is governed by an extremely complex framework of Federal, state and local laws, rules and regulations.
There continue to be Federal and state proposals that would, and actions that do, impose limitations on government and private payments to providers, including community hospitals. In addition, there regularly are proposals to increase co-payments and deductibles from program and private patients. Hospital facilities also are affected by controls imposed by government and private payors designed to reduce admissions and lengths of stay. Such controls include what is commonly referred to as “utilization review”. Utilization review entails the review of a patient’s admission and course of treatment by a third party. Historically, utilization review has resulted in a decrease in certain treatments and procedures being performed. Utilization review is required in connection with the provision of care which is to be funded by Medicare and Medicaid and is also required under many managed care arrangements.
Many states have enacted, or are considering enacting, additional measures that are designed to reduce their Medicaid expenditures and to make changes to private healthcare insurance. Various states have applied, or are considering applying, for a waiver from current Medicaid regulations in order to allow them to serve some of their Medicaid participants through managed care providers. These proposals also may attempt to include coverage for some people who presently are uninsured, and generally could have the effect of reducing payments to hospitals, physicians and other providers for the same level of service provided under Medicaid.
Healthcare Facility Regulation
Certificate of Need Requirements
A number of states require approval for the purchase, construction and expansion of various healthcare facilities, including findings of need for additional or expanded healthcare facilities or services. Certificates of Need (“CONs”), which are issued by governmental agencies with jurisdiction over applicable healthcare facilities, are at times required for capital expenditures exceeding a prescribed amount, changes in bed capacity or the addition of services and certain other matters. All three states in which SunLink currently operates hospitals (Georgia, Mississippi and Missouri) have CON laws that apply to such facilities. The two states (Georgia and Mississippi) in which SunLink currently operates nursing homes/skilled nursing facilities also have CON laws that apply to nursing homes and other skilled nursing facilities. States periodically review, modify and revise their CON laws and related regulations.
22
Index to Financial Statements
In addition, future healthcare facility acquisitions also may occur in states that require CONs. SunLink is unable to predict whether its healthcare facilities will be able to obtain any CONs that may be necessary to accomplish their business objectives in any jurisdiction where such certificates of need are required. Violation of these state laws may result in the imposition of civil sanctions or the revocation of licenses for such facilities.
Future healthcare facility acquisitions also may occur in states that do not require CONs or which have less stringent CON requirements than the states in which SunLink currently operates healthcare facilities. Any healthcare facility operated by SunLink in such states may face increased competition from new or expanding facilities operated by competitors, including physicians.
Utilization Review Compliance and Hospital Governance
SunLink’s healthcare facilities are subject to, and comply with, various forms of utilization review. In addition, under the Medicare prospective payment system, each state must have a peer review organization to carry out a federally mandated system of review of Medicare patient admissions, treatments and discharges in hospitals. Medical and surgical services and physician practices are supervised by committees of staff doctors at each healthcare facility; are overseen by each healthcare facility’s local governing board, the primary voting members of which are physicians and community members; and are reviewed by SunLink’s quality assurance personnel. The local governing boards also help maintain standards for quality care, develop long-range plans, establish, review and enforce practices and procedures and approve the credentials and disciplining of medical staff members.
Emergency Medical Treatment and Active Labor Act
All of our facilities are subject to the Emergency Medical Treatment and Active Labor Act (“EMTALA”). This federal law requires any hospital that participates in the Medicare program to conduct an appropriate medical screening examination of every person who presents himself to the hospital’s emergency department for treatment and, if the patient is suffering from an emergency medical condition, to either stabilize that condition or make an appropriate transfer of the patient to a facility that can handle the condition. The obligation to screen and stabilize emergency medical conditions exists regardless of a patient’s ability to pay for treatment. There are severe penalties under EMTALA if a hospital fails to screen or appropriately stabilize or transfer a patient or if the hospital delays appropriate treatment in order to first inquire about the patient’s ability to pay. Penalties for violations of EMTALA include civil monetary penalties and exclusion from participation in the Medicare program, the Medicaid program or both. In addition, an injured patient, the patient’s family or a medical facility that suffers a financial loss as a direct result of another hospital’s violation of the law can bring a civil suit against that other hospital. Although we believe that our hospitals comply with EMTALA, we cannot predict whether CMS will implement new requirements in the future and whether we will be able to comply with any new requirements.
Conversion Legislation
Many states, including some where we have hospitals and others where we may in the future acquire hospitals, have adopted legislation regarding the sale or other disposition of hospitals operated by not-for-profit entities. In other states that do not have specific legislation, state attorneys generally have demonstrated an interest in these transactions under their general obligations to protect charitable assets from waste. These legislative and administrative efforts primarily focus on the appropriate valuation of the assets divested and the use of the proceeds of the sale by the not-for-profit seller. These reviews and, in some instances, approval processes, can add additional time to the closing of a hospital acquisition. There can be no assurance that future actions on the state level will not seriously delay or even prevent our ability to acquire hospitals. If these activities are widespread, they could limit our ability to acquire additional hospitals or increase our acquisition costs.
23
Index to Financial Statements
Specialty Pharmacy Segment Regulation
Overview
Much like our healthcare facility operations, the operations of our Specialty Pharmacy Segment are subject to various Federal and state statutes and regulations governing their operations including laws and regulations with respect to operation of pharmacies, repackaging of drug products, wholesale distribution, dispensing of controlled substances, cross jurisdictional sale and distribution of pharmacy products, medical waste disposal, clinical trials and non-discriminatory access. Federal statutes and regulations govern the labeling, packaging, advertising and adulteration of prescription drugs as well as the dispensing of controlled substances. Federal controlled substance laws require us to register our pharmacies and repackaging facilities with the United States Drug Enforcement Administration (“DEA”) and to comply with security, recordkeeping, inventory control and labeling standards in order to dispense controlled substances. Although we believe that the operations of our Specialty Pharmacy Segment have obtained the permits and/or licenses required to conduct our specialty pharmacy business as currently conducted, a failure to have the necessary permits and licenses could have a material adverse effect on our specialty pharmacy business, and our financial condition or results of operations.
Mail Order Activities
Currently the activities of our hospital pharmacies are ancillary to the operations of the facilities they serve. In contrast, the operations of our specialty pharmacy services operations are stand-alone operations that, in addition to walk-in customers, distribute pharmaceuticals through a variety of delivery methods, including by mail and express delivery services. Many states in which we deliver or may seek to deliver pharmaceuticals have laws and regulations that require out-of-state mail service pharmacies to register with, or be licensed by, the boards of pharmacy or similar regulatory bodies in those states. These states generally permit the dispensing pharmacy to follow the laws of the state within which the dispensing pharmacy is located.
However, various state Medicaid programs have enacted laws and/or adopted rules or regulations directed at restricting or prohibiting the operation of out-of-state pharmacies by, among other things, requiring compliance with all laws of the states into which the out-of-state pharmacy dispenses medications, whether or not those laws conflict with the laws of the state in which the pharmacy is located, or requiring the pharmacist-in-charge to be licensed in that state. To the extent that such laws or regulations are found to be applicable to our operations, we believe our specialty pharmacy operations comply with them in all material respects. To the extent that any of the foregoing laws or regulations prohibit or restrict the operation of mail service pharmacies and are found to be applicable to our specialty pharmacy operations, they could have an adverse effect on our ability to expand our pharmacy operations, which currently are concentrated in Louisiana. A number of state Medicaid programs prohibit the participation in such state’s Medicare program by either out-of-state retail pharmacies or mail order pharmacies, whether located in-state or out-of-state.
Advertising and Marketing Regulations
There are also other statutes and regulations which may affect advertising, marketing and distribution of pharmacy products by our specialty pharmacy services. The Federal Trade Commission requires mail order sellers of goods generally to engage in truthful advertising, to stock a reasonable supply of the products to be sold, to fill mail orders within 30 days, and to provide clients with refunds when appropriate.
Healthcare Regulations of General Application
Licensing Requirements
SunLink’s healthcare operations are subject to extensive Federal, state and local licensing requirements. In order to maintain their operating licenses, our healthcare facility operations must comply with strict standards concerning medical care, equipment and hygiene. Various licenses and permits also are required in order to
24
Index to Financial Statements
handle radioactive materials and operate certain equipment. All licenses, provider numbers, and other permits or approvals required to perform our business operations are held by individual subsidiaries of SunLink. Each of our hospital operating subsidiaries operates only a single hospital. All of SunLink’s hospitals, except the leased hospital in Dexter, Missouri, are fully accredited by the JCAHO.
Drugs and Controlled Substances
Various licenses and permits are required by our healthcare facilities and specialty pharmacy business in order to dispense narcotics and operate pharmacies. We are required to register our pharmacy operations for permits and/or licenses with, and comply with certain operating and security standards of, the United States DEA, the Food and Drug Administration, or FDA, State Boards of Pharmacy, state health departments and other state agencies in states where we operate or may seek to operate.
State controlled substance laws require registration and compliance with state pharmacy licensure, registration or permit standards promulgated by the state’s pharmacy licensing authority. Such standards often address the qualification of an applicant’s personnel, the adequacy of its prescription fulfillment and inventory control practices and the adequacy of its facilities. In general, pharmacy licenses are renewed annually. Pharmacists and pharmacy technicians employed at each of our dispensing locations must also satisfy applicable state licensing requirements.
Fraud and Abuse, Anti-Kickback and Self-Referral Regulations
Participation in the Medicare and/or Medicaid programs is heavily regulated by federal statutes and regulations. If a hospital fails to comply substantially with the numerous federal laws governing a facility’s activities, the hospital’s participation in the Medicare and/or Medicaid programs may be terminated and/or civil or criminal penalties may be imposed. For example, a hospital may lose its ability to participate in the Medicare and/or Medicaid programs if it:
| • | makes claims to Medicare and/or Medicaid for services not provided or misrepresents actual services provided in order to obtain higher payments; |
| • | pays money to induce the referral of patients or the purchase of items or services where such items or services are reimbursable under a Federal or state health program; |
| • | fails to report or repay; or |
| • | fails to provide appropriate emergency medical screening services to any individual who comes to a hospital’s campus or otherwise fails to properly treat and transfer emergency patients. |
Hospitals continue to be one of the primary focus areas of the OIG and other governmental fraud and abuse programs. In January 2005, the OIG issued Supplemental Compliance Program Guidance for Hospitals that focuses on hospital compliance risk areas. Some of the risk areas highlighted by the OIG include correct outpatient procedure coding, revising admission and discharge policies to reflect current CMS rules, submitting appropriate claims for supplemental payments such as pass-through costs and outlier payments and a general discussion of the fraud and abuse risks related to financial relationships with referral sources. Each federal fiscal year, the OIG also publishes a General Work Plan that provides a brief description of the activities that the OIG plans to initiate or continue with respect to the programs and operations of the Department of Health and Human Services (“HHS”) and details the areas that the OIG believes are prone to fraud and abuse.
Sections of the Anti-Fraud and Abuse Amendments to the Social Security Act, commonly known as the “anti-kickback” statute, prohibit certain business practices and relationships that might influence the provision and cost of healthcare services reimbursable under Medicare, Medicaid, TriCare or other healthcare programs, including the payment or receipt of remuneration for the referral of patients whose care will be funded by Medicare or other government programs. Sanctions for violating the anti-kickback statute include criminal penalties and civil sanctions, including fines and possible exclusion from future participation in government
25
Index to Financial Statements
programs, such as Medicare and Medicaid. Pursuant to the Medicare and Medicaid Patient and Program Protection Act of 1987, the U.S. Department of Health and Human Services (“DHHS”) issued regulations that create safe harbors under the anti-kickback statute. A given business arrangement that does not fall within an enumerated safe harbor is not per se illegal; however, business arrangements that fail to satisfy the applicable safe harbor criteria are subject to increased scrutiny by enforcement authorities.
The Health Insurance Portability and Accountability Act of 1996 (“HIPAA”) broadened the scope of the fraud and abuse laws by adding several criminal statutes that are not related to receipt of payments from a federal healthcare program. HIPAA created civil penalties for proscribed conduct, including upcoding and billing for medically unnecessary goods or services. These laws cover all health insurance programs, private as well as governmental. In addition, HIPAA broadened the scope of certain fraud and abuse laws, such as the anti-kickback statute, to include not just Medicare and Medicaid services, but all healthcare services reimbursed under a Federal or state healthcare program. Finally, HIPAA established enforcement mechanisms to combat fraud and abuse. These mechanisms include a bounty system where a portion of the payment recovered is returned to the government agencies, as well as a whistleblower program, where a portion of the payment received is paid to the whistleblower. HIPAA also expanded the categories of persons that may be excluded from participation in Federal and state healthcare programs.
There is increasing scrutiny by law enforcement authorities, the Office of Inspector General of the DHHS, the courts and the U.S. Congress of arrangements between healthcare providers and potential referral sources to ensure that the arrangements are not designed as mechanisms to exchange remuneration for patient-care referrals and opportunities. Investigators also have demonstrated a willingness to look behind the formalities of a business transaction to determine the underlying purpose of payments between healthcare providers and potential referral sources. Enforcement actions have increased, as is evidenced by highly publicized enforcement investigations of certain hospital activities.
In addition, provisions of the Social Security Act, known as the Stark Act, also prohibit physicians from referring Medicare and Medicaid patients to providers of a broad range of designated health services with which the physicians or their immediate family members have ownership or certain other financial arrangements. Certain exceptions are available for employment agreements, leases, physician recruitment and certain other physician arrangements. A person making a referral, or seeking payment for services referred, in violation of the Stark Act is subject to civil monetary penalties of up to $15 for each service; restitution of any amounts received for illegally billed claims; and/or exclusion from future participation in the Medicare program, which can subject the person or entity to exclusion from future participation in state healthcare programs.
Further, if any physician or entity enters into an arrangement or scheme that the physician or entity knows or should have known has the principal purpose of assuring referrals by the physician to a particular entity, and the physician directly makes referrals to such entity, then such physician or entity could be subject to a civil monetary penalty of up to $100. In addition, the monitoring of compliance with and the enforcing of penalties for violations of these laws and regulations is changing and increasing. For example, in 2010, CMS issued a “self-referral disclosure protocol” for hospitals and other providers that wish to self-disclose potential violations of the Stark Act and attempt to resolve those potential violations and any related overpayment liabilities at levels below the maximum penalties and amounts set forth in the statute. In light of the provisions of the Affordable Care Act that created potential liabilities under the federal False Claims Act (discussed below) for failing to report and repay known overpayments and return an overpayment within sixty (60) days of the identification of the overpayment or the date by which a corresponding cost report is due, whichever is later, hospitals and other healthcare providers are encouraged to disclose potential violations of the Stark Act to CMS. It is likely that self-disclosure of Stark violations will continue in the future. Finally, many states have adopted or are considering similar legislative proposals, some of which extend beyond the Medicaid program, to prohibit the payment or receipt of remuneration for the referral of patients and physician self-referrals regardless of the source of the payment for the care.
26
Index to Financial Statements
The Federal False Claims Act and Similar State Laws
The federal False Claims Act prohibits providers from, among other things, knowingly submitting false or fraudulent claims for payment to the federal government. The federal False Claims Act defines the term “knowingly” broadly, and while simple negligence generally will not give rise to liability, submitting a claim with reckless disregard to its truth or falsity can constitute the “knowing” submission of a false or fraudulent claim for the purposes of the False Claims Act. The “qui tam” or “whistleblower” provisions of the False Claims Act allow private individuals to bring actions under the False Claims Act on behalf of the government. These private parties are entitled to share in any amounts recovered by the government, and, as a result, the number of “whistleblower” lawsuits that have been filed against providers has increased significantly in recent years. When a private party brings a qui tam action under the federal False Claims Act, the defendant will generally not be aware of the lawsuit until the government makes a determination whether it will intervene and take a lead in the litigation. If a provider is found to be liable under the federal False Claims Act, the provider may be required to pay up to three times the actual damages sustained by the government plus mandatory civil monetary penalties of between $5 to $11 for each separate false claim. The government has used the federal False Claims Act to prosecute Medicare and other government healthcare program fraud such as coding errors, billing for services not provided, submitting false cost reports, and providing care that is not medically necessary or that is substandard in quality.
HIPAA Transaction, Privacy and Security Requirements
HIPAA and federal regulations issued pursuant to HIPAA contain, among other measures, provisions that have required us to implement modified or new computer systems, employee training programs and business procedures. The federal regulations are intended to encourage electronic commerce in the healthcare industry, provide for the confidentiality and privacy of patient healthcare information and ensure the security of healthcare information.
A violation of the HIPAA regulations could result in civil money penalties of $1 per incident, up to a maximum of $25 per person, per year, per standard violated. HIPAA also provides for criminal penalties of up to $50 and one year in prison for knowingly and improperly obtaining or disclosing protected health information, up to $100 and five years in prison for obtaining protected health information under false pretenses and up to $250 and ten years in prison for obtaining or disclosing protected health information with the intent to sell, transfer or use such information for commercial advantage, personal gain or malicious harm. Since there is no significant history of enforcement efforts by the Federal government at this time, it is not possible to ascertain the likelihood of enforcement efforts in connection with the HIPAA regulations or the potential for fines and penalties, which may result from any violation of the regulations.
HIPAA Privacy Regulations
HIPAA privacy regulations protect the privacy of individually identifiable health information. The regulations provide increased patient control over medical records, mandate substantial financial penalties for violation of a patient’s right to privacy and, with a few exceptions, require that an individual’s individually identifiable health information only be used for healthcare-related purposes. These privacy standards apply to all health plans, all healthcare clearinghouses and healthcare providers, such as our facilities, that transmit health information in an electronic form in connection with standard transactions, and apply to individually identifiable information held or disclosed by a covered entity in any form. These standards impose extensive administrative requirements on our facilities and require compliance with rules governing the use and disclosure of such health information, and they require our facilities to impose these rules, by contract, on any business associate to whom we disclose such information in order to perform functions on behalf of our facilities. In addition, our facilities are subject to any state laws that are more restrictive than the privacy regulations issued under HIPAA. These laws vary by state and could impose stricter standards and additional penalties.
27
Index to Financial Statements
The HIPAA privacy regulations also require healthcare providers to implement and enforce privacy policies to ensure compliance with the regulations and standards. Under the direction of SunLink’s Vice President, Technical and Compliance Services, and in conjunction with a private HIPAA consultant and HIPAA coordinators at each facility, individually tailored policies and procedures were developed and implemented and HIPAA privacy educational programs were presented to all employees and physicians at each facility prior to the compliance deadline. We believe we are in compliance with current HIPAA privacy regulations.
HIPAA Electronic Data Standards
The Administrative Simplification Provisions of HIPAA require the use of uniform electronic data transmission standards for all healthcare related electronic data interchange. These provisions are intended to streamline and encourage electronic commerce in the healthcare industry. Among other things, these provisions require healthcare facilities to use standard data formats and code sets established by the DHHS when electronically transmitting information in connection with certain transactions, including health claims and equivalent encounter information, healthcare payment and remittance advice and health claim status.
The DHHS regulations establish electronic data transmission standards that all healthcare providers and payors must use when submitting and receiving certain electronic healthcare transactions. The uniform data transmission standards are designed to enable healthcare providers to exchange billing and payment information directly with the many payors thereby eliminating data clearinghouses and simplifying the interface programs necessary to perform this function. We believe that the management information systems at our facilities and at our corporate headquarters comply with HIPAA’s electronic data regulations and standards.
HIPAA Security Standards
The Administrative Simplification Provisions of HIPAA require the use of a series of security standards for the protection of electronic health information. The HIPAA security standards rule specifies a series of administrative, technical and physical security procedures for covered entities to use to assure the confidentiality of electronic protected health information. The standards are delineated into either required or addressable implementation specifications.
Under the direction of SunLink’s Vice President, Technical and Compliance Services, and in conjunction with a consortium of rural hospitals, private HIPAA security consultants and HIPAA security officers at each facility, we have performed security assessments, and implemented individually tailored plans to apply required or addressable solutions and implemented a set of security policies and procedures. In addition, we developed and adopted an individually tailored comprehensive disaster contingency plan for each facility and presented a HIPAA security training program to all applicable personnel. SunLink believes it is in full compliance with all aspects of the HIPAA security regulations.
HIPAA National Provider Identifier
HIPAA also required DHHS to issue regulations establishing standard unique health identifiers for individuals, employers, health plans and healthcare providers to be used in connection with standard electronic transactions. All healthcare providers, including our facilities, were required to obtain a new National Provider Identifier (“NPI”) to be used in standard transactions instead of other numerical identifiers by May 23, 2007. Our facilities have fully implemented use of a standard unique healthcare identifier by utilizing their employer identification number. DHHS has not yet issued proposed rules that establish the standard for unique health identifiers for health plans or individuals. Once these regulations are issued in final form, we expect to have approximately one to two years to become fully compliant, but cannot predict the impact of such changes at this time. We cannot predict whether our facilities may experience payment delays during the transition to the new identifiers. DHHS is currently working on the standards for identifiers for health plans; however, there are currently no proposed timelines for issuance of proposed or final rules. The issuance of proposed rules for individuals is on hold indefinitely.
28
Index to Financial Statements
Medical Waste Regulations
Our operations, especially our healthcare facility operations, generate medical waste that must be disposed of in compliance with federal, state and local environmental laws, rules and regulations. Our operations are also generally subject to various other environmental laws, rules and regulations. Such compliance costs are not significant and we do not anticipate that such compliance costs will be significant in the future.
SUNLINK OPERATIONS
Regulatory Compliance Program
SunLink maintains a company-wide compliance program under the direction of the Director of Reimbursement and Compliance. SunLink’s compliance program is directed at all areas of regulatory compliance, including physician recruitment, reimbursement and cost reporting practices, as well as pharmacy and home healthcare operations. Each hospital designates a compliance officer and develops plans to correct problems should they arise. In addition, all employees are provided with a copy of and given an introduction to SunLink’s Code of Conduct, which includes ethical and compliance guidelines and instructions about the proper resources to utilize in order to address any concerns that may arise. Each hospital conducts annual training to re-emphasize SunLink’s Code of Conduct. We monitor our corporate compliance program to respond to developments in healthcare regulations and the industry. SunLink also maintains a toll-free hotline to permit employees to report compliance concerns on an anonymous basis.
Professional Liability
As part of our business, we are subject to claims of liability for events occurring in the ordinary course of operations. To cover a portion of these claims, we maintain professional malpractice liability insurance and general liability insurance in amounts, which are commercially available, that we believe are sufficient for our operations, although some claims may exceed the scope or amount of the coverage in effect.
In connection with the acquisition of our initial six community hospitals, SunLink assumed responsibility for general and professional liability claims reported after February 1, 2001 (our acquisition date of such hospitals), and the previous owner retained responsibility for all known and filed claims. We have purchased claims-made commercial insurance (with a substantial self-insured retention) for coverage prior to and after the acquisition date. The recorded liability for general and professional liability risks includes an estimate of the liability for claims incurred prior to February 1, 2001, but reported after February 1, 2001 and for claims incurred after February 1, 2001. In connection with the acquisition of HealthMont and its two hospitals, SunLink assumed responsibility for all professional liability claims. HealthMont had purchased claims-made commercial insurance for claims made prior to the acquisition. The recorded liability for professional liability risks includes an estimate of liability for claims assumed at the acquisition and for claims incurred after the acquisition. These estimates are based on actuarially determined amounts.
Environmental Regulation
We believe we are in substantial compliance with applicable federal, state and local environmental regulations. To date, compliance with federal, state and local laws regulating the discharge of material into the environment or otherwise relating to the protection of the environment have not had a material effect upon our consolidated results of operations, consolidated financial condition or competitive position. Similarly, we have not had to make material capital expenditures to comply with such regulations.
29
Index to Financial Statements
EXECUTIVE OFFICERS OF THE REGISTRANT
Our executive officers, as of September 15, 2011, their positions with the Company or its subsidiaries and their ages are as follows:
| Name |
Offices |
Age | ||||
| Robert M. Thornton, Jr. |
Director, Chairman of the Board of Directors, President and Chief Executive Officer | 62 | ||||
| Mark J. Stockslager |
Chief Financial Officer and Principal Accounting Officer | 52 | ||||
| A. Ronald Turner |
Chief Operating Officer | 65 | ||||
| Byron D. Finn |
President – SunLink ScriptsRx, LLC | 61 | ||||
| Jack M. Spurr, Jr |
Vice President, Hospital Financial Operations | 66 | ||||
All of our executive officers hold office for an indefinite term, subject to the discretion of the Board of Directors.
Robert M. Thornton, Jr. has been Chairman and Chief Executive Officer of SunLink Health Systems, Inc. since September 10, 1998, President since July 16, 1996 and was Chief Financial Officer from July 18, 1997 to August 31, 2002. From March 1995 to the present, Mr. Thornton has been a private investor in and Chairman and Chief Executive Officer of CareVest Capital, LLC, a private investment and management services firm. Mr. Thornton was President, Chief Operating Officer, Chief Financial Officer and a director of Hallmark Healthcare Corporation (“Hallmark”) from November 1993 until Hallmark’s merger with Community Health Systems, Inc. in October 1994. From October 1987 until November 1993, Mr. Thornton was Executive Vice President, Chief Financial Officer, Secretary, Treasurer and a director of Hallmark.
Mark J. Stockslager has been Chief Financial Officer of SunLink Health Systems, Inc. since July 1, 2007. He was interim Chief Financial Office from November 6, 2006 until June 30, 2007. He has been the Principal Accounting Officer since March 11, 1998 and was Corporate Controller from November 6, 1996 to June 4, 2007. He has been associated continuously with our accounting and finance operations since June 1988 and has held various positions, including Manager of U.S. Accounting, from June 1993 until November 1996. From June 1982 through May 1988, Mr. Stockslager was employed by Price Waterhouse & Co.
A. Ronald Turner was named Chief Operating Officer of SunLink on November 30, 2010. Mr. Turner is an entrepreneur, experienced hospital management company executive and CPA who worked as an independent management consultant for sixteen months prior to joining SunLink. Mr. Turner co-founded Associated Healthcare Systems, Inc. and served as its President and CEO from April 1999 to December 2009. From July 1985 to April 1999, Mr. Turner was a private investor and management consultant who, among other things, led the merger, acquisition and financing activities for a number of hospital and other healthcare industry transactions. Mr. Turner served as the President and Chief Operating Officer of Health Group Inc. from August 1982 to July 1985. Mr. Turner co-founded Southern Health Services, Inc. and served as its President, Chief Operating Officer and a director from December 1978 to August 1982. Prior to December 1978, Mr. Turner practiced as a CPA in Arthur Young & Company’s National Healthcare Group and with Ernst & Whinney.
Byron D. Finn was named President of SunLink ScriptsRx, LLC on October 1, 2010. Mr. Finn was most recently president of Byron D. Finn, CPA, PC, which provided accounting, financial consulting and litigation support services to its clients, including numerous healthcare clients. His experience also includes various positions with The Coca-Cola Company, where he served in a number of financial-related positions and in connection with special projects, and he was previously employed by Ernst & Young. Mr. Finn is a licensed CPA and received his BA in Business Administration and Master in Accountancy degrees from the University of Georgia.
Jack M. Spurr, Jr. has been Vice President, Hospital Financial Operations for the Company since October 1, 2002. From February 1, 2001 until September 30, 2002, Mr. Spurr performed several interim financial roles for
30
Index to Financial Statements
the Company. From 1978 to 2000, Mr. Spurr held financial positions with Hospital Corporation of America, Columbia Healthcare, Inc., Quorum Health Group, Inc., HealthTrust, Inc., and National Healthcare Inc.
| Item 1A. | Risk Factors |
In addition to other information contained in this Annual Report, including certain cautionary and forward-looking statements, you should carefully consider the following factors in evaluating an investment in SunLink:
Consolidated Operations Risks
We may not be able to obtain a replacement for our existing Credit Facility. SunLink’s primary credit agreement has been modified three times in the past year, with the latest modification dated July 28, 2011 (“July 2011 Modification”). The termination date of the Credit Facility was changed from September 30, 2011 to January 1, 2013. Although SunLink was not in compliance with certain of the financial covenants contained in the Credit Facility at June 30, 2011, the Credit Facility was subsequently amended by the July 2011 Modification to change the affected covenants so as to bring us into compliance.
We are seeking to refinance the Credit Facility with a new lender and reduced borrowing under the Term Loan of the Credit Facility by approximately $10,000. Although, we believe the Company will be able to refinance existing borrowings under one or more replacement loan facilities either on a company wide or individual facility basis, there can be no assurance that we will be able to obtain new financing in the amount needed, on improved or comparable terms, or at all. We believe that the Company should be able to continue in compliance with the financial covenants in our Credit Facility as amended, but there is also no assurance that we will be able to do so. Our ability to make the required debt service and increased interest payments under the Credit Facility depends on, among other things, our ability to generate sufficient cash flows from operating activities. If we are unable to generate sufficient cash flow from operations to meet our debt service commitments or are unable to refinance or restructure our indebtedness prior to maturity at January 1, 2013, such failure could have material adverse effects on the Company.
If our operating results continue to decline, we may not be able to generate sufficient cash flows to meet our liquidity needs.
We rely upon cash on hand, cash from operations and a revolving loan facility to fund our cash requirements for working capital, capital expenditures, commitments and payments of principal and interest on borrowings. Our ability to generate cash from operations has been negatively impacted by uncollectible self-pay net revenues of our Healthcare Facilities Segment, increased salaries expenses for employed physicians and decreased patient volume at our facilities as a result of economic conditions in the locations we serve as well as decreased sales volume and earning experienced by our Specialty Pharmacy Segment. We expect that these factors will continue to have a negative impact on our business for the foreseeable future. Further deterioration would negatively impact our results of operations and cash flows.
We may not be able to maintain compliance with or borrow under out existing Credit Facility.
We currently have borrowing capacity under the revolving portion of the Credit Facility but there can be no assurance that we will be in compliance with the financial covenants. If non-compliance occurs, we may have no ability to borrow funds under the revolving portion of the Credit Facility. If we are unable to borrow under our existing Credit Facility or obtain alternative financing such failure could have a material adverse effect on the Company.
31
Index to Financial Statements
Additional debt or equity capital for significant capital investments may be required to achieve SunLink’s operational and growth plans, the inability to access capital may affect SunLink’s competitive position, reduce earnings, and negatively affect the value of your SunLink common stock.
SunLink’s operational and growth plans require significant capital investments. Significant capital investments are required for on-going and planned capital improvements at existing hospitals and may be required in connection with future capital projects either in connection with existing properties or future acquired properties. SunLink’s ability to make capital investments depends on numerous factors such as the availability of funds from operations and its credit facility and access to additional debt and equity financing. No assurance can be given that the necessary funds will be available. Moreover, incurrence of additional debt financing, if available, may involve additional restrictive covenants that could negatively affect SunLink’s ability to operate its business in the desired manner, and raising additional equity may be dilutive to shareholders. The failure to obtain funds necessary for the realization of SunLink’s plans could prevent SunLink from realizing its strategies and, in particular, could force SunLink to forego opportunities that may arise in the future. This could, in turn, have a negative impact on SunLink’s competitive position.
SunLink’s revenues are heavily concentrated in Georgia which makes SunLink particularly sensitive to economic and other changes in the state of Georgia.
For the fiscal year ended June 30, 2011, our three Georgia hospitals generated approximately 57% of consolidated gross revenues for the year. Accordingly, any adverse change in the current demographic, economic, competitive or regulatory conditions in the state of Georgia could have a material adverse effect on the business, financial condition, results of operations or prospects of SunLink.
SunLink depends heavily on its management personnel and the loss of the services of one or more of SunLink’s key senior management personnel could weaken SunLink’s management team.
SunLink has been, and will continue to be, dependent upon the services and management experience of its executive officers. If any of SunLink’s executive officers were to resign their positions or otherwise be unable to serve, SunLink’s management could be weakened and operating results could be adversely affected; however, to our knowledge, no key executive personnel intend to retire or terminate their employment with SunLink in the near future.
SunLink conducts business in a heavily regulated industry; changes in regulations or violations of regulations may result in increased costs or sanctions that could reduce revenue and profitability.
The healthcare industry is subject to extensive Federal, state and local laws and regulations relating to:
| • | licensure; |
| • | conduct of operations including patient referrals, physician recruiting practices, cost reporting and billing practices; |
| • | ownership of facilities; |
| • | addition of facilities and services; |
| • | confidentiality, maintenance, and security issues associated with medical records; |
| • | billing for services; and |
| • | prices for services. |
These laws and regulations are extremely complex and, in many instances, the industry does not have the benefit of significant regulatory or judicial interpretation of these laws and regulations, including in particular, Medicare and Medicaid anti-fraud and abuse amendments, codified in Section 1128B(b) of the Social Security
32
Index to Financial Statements
Act and known as the “anti-kickback statute.” This law prohibits providers and others from soliciting, receiving, offering or paying, directly or indirectly, any remuneration with the intent to generate referrals of orders for services or items reimbursable under Medicare, Medicaid, and other Federal healthcare programs.
DHHS regulations describe some of the conduct and business relationships immune from prosecution under the anti-kickback statute. The fact that a given business arrangement does not fall within one of these “safe harbor” provisions does not render the arrangement illegal. However, business arrangements of healthcare service providers that fail to satisfy the applicable safe harbor criteria risk increased scrutiny by enforcement authorities.
We have a variety of financial relationships with physicians who refer patients to our hospitals. We have contracts with physicians providing services under a variety of financial arrangements such as employment contracts and professional service agreements. We also provide financial incentives, including loans and minimum revenue guarantees, to recruit physicians into the communities served by our hospitals.
HIPAA broadened the scope of the fraud and abuse laws to include all healthcare services, whether or not they are reimbursed under a Federal program. In addition, provisions of the Social Security Act, known as the Stark Act, also prohibit physicians from referring Medicare and Medicaid patients to providers of a broad range of designated health services in which the physicians or their immediate family members have an ownership interest or certain other financial arrangements.
In addition, SunLink’s facilities will continue to remain subject to any state laws that are more restrictive than the regulations issued under HIPAA, which vary by state and could impose additional penalties. In recent years, both Federal and state government agencies have announced plans for or implemented heightened and coordinated civil and criminal enforcement efforts.
Government officials charged with responsibility for enforcing healthcare laws could assert that SunLink or any of the transactions in which the Company or its subsidiaries or their predecessors is or was involved, are in violation of these laws. It is also possible that these laws ultimately could be interpreted by the courts in a manner that is different from the interpretations made by the Company or others. A determination that either SunLink or its subsidiaries or their predecessors is or was involved in a transaction that violated these laws, or the public announcement that SunLink or its subsidiaries or their predecessors is being investigated for possible violations of these laws, could have a material adverse effect on SunLink’s business, financial condition, results of operations or prospects and SunLink’s business reputation could suffer significantly.
The laws, rules, and regulations described above are complex and subject to interpretation. In the event of a determination that we are in violation of any of these laws, rules or regulations, or if further changes in the regulatory framework occur, our results of operations could be significantly harmed.
SunLink is and in the future could be subject to claims related to discontinued operations, hospitals sold by our HealthMont subsidiary prior to its acquisition, and claims related to the disposition of our former Mountainside Medical Center.
Over the past 22 years, SunLink has discontinued operations carried on by its former industrial and life sciences and engineering segments, and U.K. child safety segments, leisure marine, and housewares segments and its former Mountainside Medical Center (by virtue of the sale of such facility whose original facility was one of our original hospitals). Prior to our acquisition of our HealthMont subsidiaries, HealthMont had sold two hospitals and it also disposed of one additional hospital as a condition to our acquisition of HealthMont. Contingent obligations related to discontinued operations include guarantees of certain obligations of former subsidiaries. SunLink currently does not purchase insurance policies to reduce product liability or other discontinued operations exposures and does not anticipate it will purchase such insurance in the future. Based upon an evaluation of information currently available and consultation with legal counsel, management has not reserved any amounts for contingencies related to the discontinued operations.
33
Index to Financial Statements
The industry trend towards value-based purchasing may negatively impact our revenues.
There is a trend in the healthcare industry toward “value-based” purchasing of healthcare services. These value-based purchasing programs include both public reporting of quality data and preventable adverse events tied to the quality and efficiency of care provided by facilities. Governmental programs including Medicare and Medicaid currently require hospitals to report certain quality data to receive full reimbursement updates. In addition, Medicare does not reimburse for care related to certain preventable adverse events. Many large commercial payors currently require hospitals to report quality data, and several commercial payors do not reimburse hospitals for certain preventable adverse events.
The Affordable Care Act contains a number of provisions intended to promote value-based purchasing. Effective July 1, 2011, the Affordable Care Act will prohibit the use of federal funds under the Medicaid program to reimburse providers for medical assistance provided to treat hospital acquired conditions (“HACs”). An HAC is a condition that is acquired by a patient while admitted as an inpatient at a hospital, such as a surgical site infection. Beginning in federal fiscal year 2015, hospitals that fall into the top 25% of national risk-adjusted HAC rates for all hospitals in the previous year will receive a 1% reduction in their total Medicare payments. Hospitals with excessive readmissions for conditions designated by HHS will receive reduced payments for all inpatient discharges, not just discharges relating to the conditions subject to the excessive readmission standard.
The Affordable Care Act also requires DHHS to implement a value-based purchasing program for inpatient hospital services. The Affordable Care Act requires DHHS to reduce inpatient hospital payments for all discharges by a percentage beginning at 1% in federal fiscal year 2013 and increasing by 0.25% each fiscal year up to 2% in federal fiscal year 2017 and subsequent years. DHHS will pool the amount collected from these reductions to fund payments to reward hospitals that meet or exceed certain quality performance standards established by DHHS. DHHS will determine the amount each hospital that meets or exceeds the quality performance standards will receive from the pool of dollars created by these payment reductions.
We expect value-based purchasing programs, including programs that condition reimbursement on patient outcome measures, to become more common and to involve a higher percentage of reimbursement amounts. We are unable at this time to predict how this trend will affect our results of operations, but it could negatively impact our financial condition or results of operations.
The lingering effects of the economic recession could materially adversely affect our cash flows, financial position, or results of operations.
The United States economy recently experienced a major economic recession, the economy remains weak, unemployment levels remain high, and there is a substantial risk that the economy will lapse back into recession. While certain healthcare spending is considered non-discretionary and may not be significantly impacted by economic downturns, other types of healthcare spending may be adversely impacted by such conditions. When patients are experiencing personal financial difficulties or have concerns about general economic conditions, they may choose:
| • | to defer or forego elective surgeries and other non-emergent procedures, which are generally more profitable lines of business for hospitals; or |
| • | a high-deductible insurance plan or no insurance at all, which increases a hospital’s dependence on self-pay revenue. Moreover, a greater number of uninsured patients may seek care in our emergency rooms. |
We believe the economic recession has had an adverse effect on our business. Furthermore, although we are unable to predict the specific impact of continued adverse economic conditions on our business, we believe that the lingering effects of the economic recession could have an adverse impact on our operations and could impact not only the healthcare decisions of our patients, but also the solvency of managed care providers and other counterparties to transactions with us.
34
Index to Financial Statements
SunLink is subject to potential claims for professional liability, including claims based on the acts or omissions of third parties, which claims may not be covered by insurance.
SunLink is subject to potential claims for professional liability (medical malpractice), both in connection with our current operations, as well as acquired operations. To cover these claims, we maintain professional malpractice liability insurance and general liability insurance in amounts that we believe are sufficient for our operations, although some claims may exceed the scope or amount of the coverage in effect. The assertion of a significant number of claims, either within our self-insured retention (deductible) or individually or in the aggregate in excess of available insurance, could have a material adverse effect on our results of operations or financial condition. Premiums for professional liability insurance have historically been volatile and we cannot assure you that professional liability insurance will continue to be available on terms acceptable to us, if at all. The operations of our hospitals also depend on the professional services of physicians and other trained healthcare providers and technicians in the conduct of their respective operations, including independent laboratories and physicians rendering diagnostic and medical services. There can be no assurance that any legal action stemming from the act or omission of a third party provider of healthcare services, would not be brought against one of our hospitals or SunLink, resulting in significant legal expenses in order to defend against such legal action or to obtain a financial contribution from the third-party whose acts or omissions occasioned the legal action.
Risks Related to Our Healthcare Facility Operations
SunLink’s success depends on its ability to maintain good relationships with the physicians at its hospitals and, if SunLink is unable to successfully maintain good relationships with physicians, admissions and outpatient revenues at SunLink hospitals may decrease and SunLink’s operating performance could decline.
Because physicians generally direct the majority of hospital admissions and outpatient services, SunLink’s success is, in part, dependent upon the number and quality of physicians on the medical staffs of its hospitals, the admissions and referrals practices of the physicians at our hospitals, and our ability to maintain good relations with our physicians. Many physicians at SunLink hospitals are not employees of the hospitals at which they practice and, in many of the markets that SunLink serves, most physicians have admitting privileges at other hospitals in addition to SunLink’s hospitals. If SunLink is unable to successfully maintain good relationships with physicians, admissions at SunLink hospitals may decrease and SunLink’s operating performance could decline.
SunLink depends heavily on its healthcare facility management personnel and the loss of the services of one or more of SunLink’s key local management personnel could weaken SunLink’s management team and its ability to deliver healthcare services.
SunLink’s success depends on its ability to attract and retain managers at its hospitals and related health care facilities, on the ability of hospital-based officers and key employees to manage growth successfully, and on their ability to attract and retain skilled employees. SunLink has not had any material difficulties in attracting healthcare facility management; however, if SunLink is unable to attract and retain affective local management, the operating performance of our facilities could decline.
SunLink’s success depends on its ability to attract and retain qualified healthcare professionals and a shortage of qualified healthcare professionals in certain markets could weaken our ability to deliver healthcare services.
In addition to the physicians and management personnel whom SunLink employs, SunLink’s operations are dependent on the efforts, ability, and experience of other healthcare professionals, such as nurses, pharmacists and lab technicians. Nurses, pharmacists, lab technicians and other healthcare professionals are generally employees of each individual SunLink hospital. SunLink’s success has been, and will continue to be, influenced
35
Index to Financial Statements
by its ability to attract and retain these skilled employees. A shortage of healthcare professionals in certain markets, the loss of some or all of its key employees or the inability to attract or retain sufficient numbers of qualified healthcare professionals could cause SunLink’s operating performance to decline.
A significant portion of SunLink’s revenue is dependent on Medicare and Medicaid payments, and possible reductions in Medicare or Medicaid payments or the implementation of other measures to reduce reimbursements may reduce our revenues.
A significant portion of SunLink’s revenues are derived from the Medicare and Medicaid programs, which are highly regulated and subject to frequent and substantial changes. SunLink derived approximately 82% of its patient days and 57% of its net patient revenues from the Medicare and Medicaid programs for the year ended June 30, 2011. Previous legislative changes have resulted in, and future legislative changes may result in, limitations on and reduced levels of payment and reimbursement for a substantial portion of hospital procedures and costs.
Future healthcare legislation or other changes in the administration or interpretation of governmental healthcare programs may have a material adverse effect on SunLink’s business, financial condition, results of operations or prospects.
Revenue and profitability of our healthcare facility operations, especially our community hospital operations, may be constrained by future cost containment initiatives undertaken by purchasers of healthcare services if SunLink is unable to contain costs.
Our community hospital operations derived approximately 43% of their net patient revenues for the fiscal year ended June 30, 2011 from private payors and other non-governmental sources who contributed approximately 18% of SunLink’s patient days. Our hospitals have been affected by the increasing number of initiatives undertaken during the past several years by all major purchasers of healthcare, including (in addition to Federal and state governments) insurance companies and employers, to revise payment methodologies and monitor healthcare expenditures in order to contain healthcare costs. Initiatives such as managed care organizations offering prepaid and discounted medical services packages have adversely affected hospital revenue growth throughout the country and such packages represent an increasing portion of SunLink’s admissions and outpatient revenues and have resulted in reduced revenue growth at our hospitals. In addition, private payers increasingly are attempting to control healthcare costs through direct contracting with hospitals to provide services on a discounted basis, increased utilization review and greater enrollment in managed care programs such as health maintenance organizations and preferred provider organizations, referred to as PPOs. If we are unable to contain costs, especially in our hospital operations, through increased operational efficiencies and the trend toward declining reimbursements and payments continues, the results of healthcare facility segment operations and cash flow will be adversely affected and the results of our consolidated operations and our consolidated cash flow similarly likely would be adversely affected.
Our healthcare facilities, especially our community hospitals, face intense competition from other hospitals and healthcare providers which directly affect our segment and consolidated revenues and profitability.
Although each of our hospitals operates in communities where they are currently the only general, acute care hospital, they do face competition from other hospitals, including larger tertiary care centers. Although these competing hospitals may be as far as 30 to 50 miles away, patients in these markets may migrate to these competing facilities as a result of local physician referrals, managed care plan incentives or personal choice.
The healthcare business is highly competitive and competition among hospitals and other healthcare providers for patients has intensified in recent years. Each of our hospitals operates in geographic areas where they compete with at least one other hospital that provides services comparable to those offered by our hospitals. Some of these competing facilities offer services, including extensive medical research and medical education
36
Index to Financial Statements
programs, which are not offered by SunLink’s facilities. Some of the competing hospitals are owned or operated by tax-supported governmental bodies or by private not-for-profit entities supported by endowments and charitable contributions which can finance capital expenditures on a tax-exempt basis and are exempt from sales, property, and income taxes. In some of these markets, SunLink’s hospitals also face competition from other for-profit hospital companies, some of which have substantially greater resources, as well as other providers such as outpatient surgery and diagnostic centers.
The intense competition from other hospitals and other healthcare providers directly affects the market share of our community hospitals, as well as their and our revenues and profitability.
Changes in market demographics may increase competition for certain of our community hospitals.
Some of our hospitals are located in exurban areas which are becoming more suburban or metropolitan. Such markets are likely to attract additional competitors, including satellite operations of tertiary hospitals. We cannot assure you that we will have the financial resources to fund capital improvements to our existing facilities, which may face additional competition or that even if financial resources are available to us, projected operating results will justify such expenditures. An inability to fund or the infeasibility of funding capital improvements could directly or indirectly have an adverse impact on hospital revenues through lower patient utilization, increased difficulty in physician recruitment and otherwise as a result of increased competition.
SunLink’s hospitals are and our other healthcare facilities may be subject to, and depend on, certificate of need laws which could affect their ability to operate profitably.
All states in which SunLink currently operates hospitals and nursing homes have laws affecting acute care hospital facilities, nursing homes, ambulatory surgery centers and the provision of various services; such laws are known as “certificate of need” laws. Under such laws, prior state approval is required for the acquisition of major medical equipment or the purchase, lease, construction, expansion, sale or closure of covered healthcare facilities, based on a determination of need for additional or expanded facilities or services. The required approval is known generally as a certificate of need or CON. A CON may be required for capital expenditures exceeding a prescribed amount, changes in hospital and nursing home bed capacity or services, and certain other matters. The failure to obtain any required CON may impair SunLink’s ability to operate profitably.
In addition, the elimination or modification of CON laws in states in which SunLink operates or in the future may own hospitals and other covered healthcare facilities could subject our hospitals to greater competition making it more difficult to operate profitably.
Risk Relating to our Specialty Pharmacy Business
The operations of our Specialty Pharmacy Segment may be adversely affected by changes in government reimbursement regulations and payment levels.
For the year ended June 30, 2011, the operations of our Specialty Pharmacy Segment derived approximately 64% of its net revenues from government payors, principally Medicare and Medicaid. The Deficit Reduction Act of 2005 exempted rural providers of home care related services from the competitive acquisition program to which urban providers are subject.
We cannot assure you that the ASP reimbursement methodology will not be extended to the provision of all specialty pharmaceuticals or to the specialty pharmaceuticals most often sold by the operations of our Specialty Pharmacy Segment or that we will continue to be able to operate our Specialty Pharmacy Segment profitably at either existing or at lower reimbursement rates. Likewise, we cannot assure you that the Part B CAP program will not be extended to rural or exurban areas in general or to the areas in which we operate, or may seek to operate, in particular or that we would be able to meet the qualifications to become a Part B CAP vendor either now or at any time in the future.
37
Index to Financial Statements
The operations of our Specialty Pharmacy Segment could be harmed by further changes in government purchasing methodologies and reimbursement rates for Medicare or Medicaid.
In addition to the impact of MMA implemented or inspired changes, in order to deal with budget shortfalls, some states are attempting to create state administered prescription drug discount plans, to limit the number of prescriptions per person that are covered, and to raise Medicaid co-pays and deductibles, and are proposing more restrictive formularies and reductions in pharmacy reimbursement rates. Any reductions in amounts reimbursable by other government programs for our services or changes in regulations governing such reimbursements could materially and adversely affect our business, financial condition and results of operations.
Our durable medical equipment service line may be adversely affected by changes in government reimbursement regulations and payment levels, especially if our durable medical equipment service line becomes subject to competitive bidding procedures.
Although we are currently exempted under the Deficit Reduction Act of 2005 from the competitive acquisition program for DMEPOS, we cannot be sure such exemption will continue to be available in the future. Loss of such exemption could have an adverse effect on our results of operation.
The operations of our Specialty Pharmacy Segment depend on a continuous supply of key products. Any shortages of key products could adversely affect our business.
Many of the biopharmaceutical products distributed by the operations of our Specialty Pharmacy Segment are manufactured with ingredients that are susceptible to supply shortages. In addition, the manufacturers of these products may not have adequate manufacturing capability to meet rising demand. If any products we distribute are in short supply for long periods of time, this could result in a material adverse effect on our business and results of operations.
The operations of our Specialty Pharmacy Segment are highly dependent on relationships with key suppliers and the loss of any of such key suppliers could adversely affect our business.
Any termination of, or adverse change in, our relationships with our key suppliers, or the loss of supply of one of our key products for any other reason, could have a material adverse effect on our business and results of operations. The largest supplier for our specialty pharmacy operations accounted for approximately 56% of Carmichael’s total net sales in the fiscal year ended June 30, 2011. Our specialty pharmacy operations have a single source of supply for many of our key products, including one product which accounted for approximately 23% of Carmichael’s total net sales in the fiscal year ended June 30, 2011. In addition, we have few long-term contracts with our suppliers. Our arrangements with most of our suppliers may be canceled by either party, without cause, on minimal notice. Many of these arrangements are not governed by written agreements.
The loss of one or more of our larger institutional pharmacy customers could hurt our business by reducing the revenues and profitability of the operations of our Specialty Pharmacy Segment.
As is customary in the institutional pharmacy industry, our Specialty Pharmacy Segment generally does not have long-term contracts with our institutional pharmacy customers. Significant declines in the level of purchases by one or more of our larger institutional pharmacy customers could have a material adverse effect on our business and results of operations.
Our failure to maintain eligibility as a Medicare and Medicaid supplier could materially adversely affect our competitive position. Likewise, our failure to maintain and expand relationships with private payors, who can effectively determine the pharmacy source for their members, could materially adversely affect our competitive position.
38
Index to Financial Statements
Changes in average wholesale prices could reduce our pricing and margins.
Many government payors, including Medicare and Medicaid, have paid, or continue to pay, the operations of our Specialty Pharmacy Segment directly or indirectly at a rate based upon a drug’s AWP less a percentage factor. We also have contracted with some private payors to sell drugs at AWP or at AWP less a percentage factor. For most drugs, AWP is compiled and published by several private companies, including First DataBank, Inc. Several states have filed lawsuits against pharmaceutical manufacturers for allegedly inflating reported AWP for prescription drugs. In addition, class action lawsuits have been brought by consumers against pharmaceutical manufacturers alleging overstatement of AWP. We are not responsible for such calculations, reports or payments; however, there can be no assurance that the ability of our Specialty Pharmacy Segment to negotiate discounts from drug manufacturers will not be materially adversely affected by such investigations or lawsuits.
The Federal government also has entered into settlement agreements with several drug manufacturers relating to the calculation and reporting of AWP pursuant to which the drug manufacturers, among other things, have agreed to report new pricing information, the “average sales price”, to government healthcare programs. The average sales price is calculated differently than AWP.
We face numerous competitors and potential competitors in the market in which our Specialty Pharmacy Segment operates, many of whom are significantly larger and who have significantly greater financial resources.
Although we believe market penetration by large national companies into our existing market in which our Specialty Pharmacy Segment operates has not been substantial, we cannot assure you that one or more of such companies or other healthcare companies will not seek to compete or intensify their level of competition in the areas in which we conduct or may seek to conduct one or more of the components of the operations of our Specialty Pharmacy Segment.
The operations of our Specialty Pharmacy Segment may be adversely affected by industry trends in managed care contracting and consolidation.
A growing number of health plans are contracting with a single provider of specialty pharmacy services. Likewise, manufacturers may not be eager to contract with regional providers of specialty pharmacy services. If we are unable to obtain managed care contracts in the areas in which we provide specialty pharmacy services or are unable to obtain specialty pharmacy products at reasonable costs or at all, the business operations of our Specialty Pharmacy Segment could be adversely affected.
The specialty pharmacy market may grow slower than expected, which could adversely affect our revenues.
We cannot predict the rate of actual future growth in product availability and spending, the extent to which patient demand or spending for specialty drug services in rural or exurban areas will match national averages or whether government payors will provide reimbursement for new products under Medicare or Medicare on a timely basis, or at all, or at what rates. Adverse developments in any of these areas could have an adverse impact on the business operations of our Specialty Pharmacy Segment.
Other Risks
SunLink may issue additional equity in the future which could dilute the value of shares of existing shareholders.
SunLink’s working capital is limited to cash generated from operations and borrowings available under the revolving loan facility in our current credit facility (a $9,000 revolving loan with $5,300 of the revolver outstanding and approximately $2,560 available to borrow at June 30, 2011) and our additional debt capacity is limited. On July 28, 2011, SunLink announced the private placement of approximately 1,338,000 common shares at $1.90 per share with certain of its officers and directors and/or their affiliates. The net proceeds of the private placement of approximately $2,500 were used, together with the Company’s operating funds, to make an $8,000
39
Index to Financial Statements
pre-payment on the Credit Facility Term Loan. A special committee of the Company’s Board of Directors comprised of disinterested directors evaluated the private placement transaction and obtained an opinion of an outside advisor selected by the special committee that the price and terms of the private placement were fair from a financial point of view to the Company. The Company’s Board of Directors authorized the private placement before August 31, 2011 of a total of up to 3,800,000 of the Company’s common shares at a price equal to the average closing price for the prior ten trading days (on which the Company’s shares traded) with a minimum placement of $2,500. Although the Board of Directors has not decided to effect any additional equity transactions at this time, it may authorize the Company to do so in the future in connection with mergers and acquisitions, capital transactions or for other purposes. Any additional equity transactions could result in dilution in the value of existing shares.
Forward-looking statements in this annual report may prove inaccurate.
This document contains forward-looking statements about SunLink that are not historical facts but, rather, are statements about future expectations. Forward-looking statements in this document are based on management’s current views and assumptions and may be influenced by factors that could cause actual results, performance or events to be materially different from those projected. These forward-looking statements are subject to numerous risks and uncertainties. Important factors, some of which are beyond the control of SunLink, could cause actual results, performance or events to differ materially from those in the forward-looking statements. These factors include those described above under “Risk Factors” and elsewhere in this report under “Forward-Looking Statements.”
| Item 1B. | Unresolved Staff Comments |
None.
| Item 2. | Properties |
Our principal properties as of the date of filing of this report are listed below:
| Name or Function |
Location City and State |
Licensed Beds |
Date
of Acquisition/Lease Inception |
Ownership Type |
||||||||
| Healthcare Facilities |
||||||||||||
| Chestatee Regional Hospital |
Dahlonega, GA | 49 | February 1, 2001 | Owned | ||||||||
| North Georgia Medical Center & Gilmer Nursing Home |
Ellijay, GA | 50 | February 1, 2001 | Owned | ||||||||
| Trace Regional Hospital & Floy Dyer Manor Nursing Home |
Houston, MS | 84 | February 1, 2001 | Owned | ||||||||
| Callaway Community Hospital |
Fulton, MO | 49 | October 3, 2003 | Owned | ||||||||
| Memorial Hospital of Adel & Memorial Convalescent Center |
Adel, GA | 60 | October 3, 2003 | Owned | ||||||||
| Missouri Southern Healthcare(1) |
Dexter, MO | 50 | February 1, 2001 | Leased | ||||||||
| Specialty Pharmacy Operations |
||||||||||||
| Carmichael Cashway Pharmacy(2) |
Crowley, LA | N/A | April 22, 2008 | Leased | ||||||||
| Carmichael Cashway Pharmacy(3) |
Lafayette, LA | N/A | April 22, 2008 | Leased | ||||||||
| Carmichael Cashway Pharmacy(4) |
Lake Charles, LA | N/A | April 22, 2008 | Leased | ||||||||
| Other |
||||||||||||
| Chilton Medical Center(5) |
Clanton, AL | N/A | February 1, 2001 | Owned | ||||||||
| Corporate Offices(6) |
Atlanta, GA | N/A | June 1, 1998 | Leased | ||||||||
| (1) | The lease expires in March, 2019. |
| (2) | Lease of approximately 25,000 square feet of store location, warehouse and office space. The lease expires in April 2013 and provides for a renewal of the lease for two five year terms. |
40
Index to Financial Statements
| (3) | Lease of approximately 5,900 square feet of store location and warehouse space. The lease expires in October 2011. |
| (4) | Lease of approximately 4,000 square feet of store location and warehouse space. The lease expires in December 2011. |
| (5) | Operations were sold February 28, 2011. The buyer owns the hospital license and leases the facility from SunLink with an option to purchase. |
| (6) | Lease of approximately 4,800 square feet of office space for corporate staff. The lease was scheduled to expire in September 2009 but has been renewed through March 2015. |
| Item 3. | Legal Proceedings |
On December 7, 2007, Southern Health Corporation of Ellijay, Inc. (“SHC-Ellijay”), a SunLink subsidiary, filed a Complaint against James P. Garrett and Roberta Mundy, both individually and as Fiduciary of the Estate of Randy Mundy (collectively, “Defendants”), seeking specific performance of an Option Agreement (the “Option Agreement”) dated April 17, 2007, between SHC-Ellijay, Mr. Garrett, and Ms. Mundy as Executrix of the Estate of Randy Mundy for the sale of approximately 24.74 acres of real property located in Gilmer County, Georgia, and recovery of SHC-Ellijay’s damages suffered as a result of Defendants’ failure to close the transaction in accordance with the Option Agreement. SHC-Ellijay also stated alternative claims for breach of the Option Agreement and fraud, along with claims to recover attorney’s fees and punitive damages.
In January 2008, Ms. Mundy and Mr. Garrett filed motions to strike, motions to dismiss, answers, affirmative defenses, and counterclaims against SHC-Ellijay. On March 3, 2009, SHC-Ellijay filed a First Amended and Restated Complaint for Damages, which effectively dropped the cause of action for specific performance of the Option Agreement. On May 7, 2009, Mr. Garrett and Ms. Mundy served a motion for summary judgment on all counts and causes of action stated in the First Amended Complaint, contending that Mr. Garrett and Ms. Mundy did not intentionally breach the Option Agreement. SHC-Ellijay filed opposition papers in June 2009 and requested a continuance. The court postponed consideration of the defendants’ motion for summary judgment and SHC-Ellijay’s response thereto until after a discovery dispute between the parties was resolved and SHC-Ellijay had an opportunity to move for summary judgment. That discovery dispute was resolved and, after another discovery dispute was resolved, the parties completed discovery. In May 2011, SHC-Ellijay filed a motion for partial summary judgment on Count I of the Amended Complaint, seeking a judgment holding that Defendants willfully and intentionally breached the Option Agreement in eight ways, which would entitle SHC-Ellijay to recover damages from Defendants.
In July 2011, SHC-Ellijay filed a reply brief in further support of its motion for partial summary judgment on the complaint and full summary judgment on the Defendants’ counterclaims and brief in opposition to Defendants’ cross motion for summary judgment. The summary judgment motions remain pending.
SunLink denies that it has any liability to Mr. Garrett and Ms. Mundy and intends to vigorously defend the claims asserted against SunLink by Mr. Garrett’s and Ms. Mundy’s counterclaims and to vigorously pursue its claims against Mr. Garrett and Ms. Mundy. While the ultimate outcome and materiality of the litigation cannot be determined, in management’s opinion the litigation will not have a material adverse effect on SunLink’s financial condition or results of operations.
SunLink is a party to claims and litigation incidental to its business, for which it is not currently possible to determine the ultimate liability, if any. Based on an evaluation of information currently available and consultation with legal counsel, management believes that resolution of such claims and litigation is not likely to have a material effect on the financial position, cash flows, or results of operations of the Company. The Company expenses legal costs as they are incurred.
| Item 4. | Reserved |
41
Index to Financial Statements
PART II
| Item 5. | Market for Registrant’s Common Equity and Related Stockholder Matters |
SunLink common shares are listed on the NYSE Amex Equities exchange. SunLink’s ticker symbol is “SSY”. The following table shows, for the calendar quarters indicated, based on published financial sources, the high and low sale prices of SunLink common shares as reported on the NYSE Amex Equities exchange.
| Sales Price of SunLink Common Shares |
||||||||
| High | Low | |||||||
| Fiscal 2011 (July 1, 2010—June 30, 2011) |
||||||||
| Fourth Quarter |
$ | 2.65 | $ | 1.50 | ||||
| Third Quarter |
2.00 | 1.48 | ||||||
| Second Quarter |
2.40 | 1.40 | ||||||
| First Quarter |
2.40 | 1.75 | ||||||
| Fiscal 2010 (July 1, 2009—June 30, 2010) |
||||||||
| Fourth Quarter |
$ | 3.63 | $ | 2.17 | ||||
| Third Quarter |
4.19 | 1.44 | ||||||
| Second Quarter |
2.79 | 1.64 | ||||||
| First Quarter |
2.50 | 1.83 | ||||||
American Stock Transfer & Trust Company is the Transfer Agent and Registrar for our common shares. For all shareholder inquiries, call American Stock Transfer & Trust’s Shareholder Services Department at 1-888-937-5449.
Dividends
SunLink does not currently pay cash dividends. SunLink intends to retain its earnings for use in the operation and expansion of its business and, therefore, does not anticipate declaring or paying regular cash dividends in the foreseeable future. Any future determination to declare or pay cash dividends will be determined by SunLink’s board of directors and will depend on SunLink’s financial condition, results of operations, business, prospects, capital requirements, credit agreements and such other matters as the board of directors may consider relevant. SunLink is currently precluded from paying any cash dividends under its current Credit Facility.
Holders
As of June 30, 2011 there were approximately 526 registered holders of SunLink common shares.
42
Index to Financial Statements
Securities Authorized for Issuance under Equity Compensation Plans
The following provides tabular disclosure of the number of securities at June 30, 2011 to be issued upon the exercise of outstanding options, the weighted average exercise price of outstanding options and the number of securities remaining available for future issuance under equity compensation plans, reported by two categories- plans that have been approved by shareholders and plans that have not been so approved:
| (a) | (b) | (c) | ||||||||||
| Plan Category |
Number of securities to be issued upon exercise of outstanding options |
Weighted average exercise price of outstanding options |
Number of securities remaining available for future issuance under equity compensation plans (excluding securities reflected in column (a)) |
|||||||||
| Equity compensation plans approved by security holders: |
||||||||||||
| 2001 Outside Directors’ Stock Ownership and Stock Option Plan |
45,000 | $ | 4.37 | 0 | ||||||||
| 2001 Long-Term Stock Option Plan |
13,250 | $ | 3.96 | 0 | ||||||||
| 2005 Equity Incentive Plan |
115,999 | $ | 9.88 | 614,676 | ||||||||
|
|
|
|
|
|
|
|||||||
| 174,249 | $ | 5.91 | 614,676 | |||||||||
|
|
|
|
|
|
|
|||||||
| Equity compensation plans not approved by security holders: |
||||||||||||
| None |
0 | 0 | 0 | |||||||||
|
|
|
|
|
|
|
|||||||
| Total |
174,249 | $ | 5.91 | 614,676 | ||||||||
|
|
|
|
|
|
|
|||||||
43
Index to Financial Statements
Performance Graph
The following graph presents a comparison of five years cumulative total return for SunLink, the NYSE Amex Equities exchange Composite Index and a self constructed peer group. The peer group consists of Amsurg Corp., Community Health Systems Inc., Dynacq Healthcare Inc., Health Management Association Inc., Lifepoint Hospitals Inc., Magellan Health Services Inc., Medcath Corp., Paincare Holdings Inc., Tenet Healthcare Corp., and Universal Health Services Inc. There is no assurance the Hospital Index peer group or NYSE Amex Equities Composite is comparable to SunLink, because, among other reasons, both consist of larger companies than SunLink.
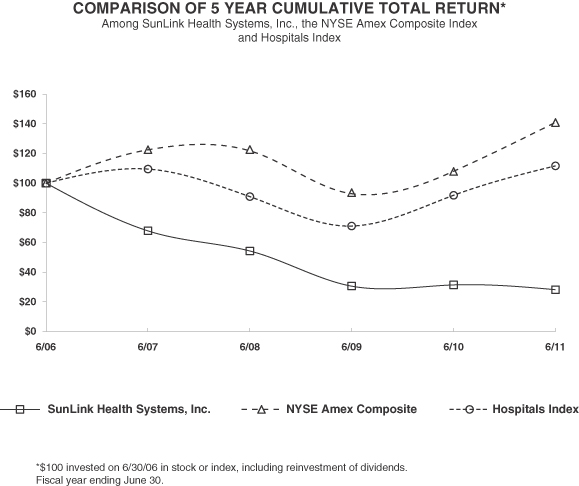
| 6/06 | 6/07 | 6/08 | 6/09 | 6/10 | 6/11 | |||||||||||||||||||
| SunLink Health Systems, Inc. |
100.00 | 63.84 | 48.59 | 21.92 | 22.78 | 19.19 | ||||||||||||||||||
| NYSE Amex Equities Composite |
100.00 | 125.36 | 124.63 | 92.01 | 108.97 | 146.13 | ||||||||||||||||||
| Hospitals Index |
100.00 | 110.71 | 89.82 | 67.47 | 90.83 | 113.16 | ||||||||||||||||||
44
Index to Financial Statements
| Item 6. | Selected Financial Data |
Selected historical financial data presented below as of and for the fiscal years ended June 30, 2011, 2010, 2009, 2008 and 2007 have been derived from the audited consolidated financial statements of SunLink. The following financial information reflects the acquisition of our two HealthMont hospitals and Carmichael and the disposition of Mountainside Medical Center, Chilton Medical Center and three home health agencies. This data should be read in conjunction with “Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations,” and the Consolidated Financial Statements of SunLink and the notes thereto included in Item 8 of this Annual Report.
SunLink Selected Historical Financial Data
(All amounts in thousands, except per share amounts)
| 2011 | 2010 | 2009 | 2008 | 2007 | ||||||||||||||||
| Net Revenues |
$ | 181,161 | $ | 183,166 | $ | 181,561 | $ | 142,885 | $ | 130,495 | ||||||||||
| Earnings (loss) from continuing operations |
(10,552 | ) | (858 | ) | 805 | 2,113 | 2,586 | |||||||||||||
| Net earnings (loss) |
(10,715 | ) | 102 | 912 | 1,720 | 2,405 | ||||||||||||||
| Earnings (loss) per share from continuing operations |
||||||||||||||||||||
| Basic |
(1.30 | ) | (0.11 | ) | 0.10 | 0.28 | 0.35 | |||||||||||||
| Diluted |
(1.30 | ) | (0.11 | ) | 0.10 | 0.27 | 0.33 | |||||||||||||
| Net earnings per share: |
||||||||||||||||||||
| Basic |
(1.32 | ) | 0.01 | 0.11 | 0.23 | 0.33 | ||||||||||||||
| Diluted |
(1.32 | ) | 0.01 | 0.11 | 0.22 | 0.31 | ||||||||||||||
| Total Assets |
89,536 | 98,490 | 107,383 | 111,624 | 77,843 | |||||||||||||||
| Long-term debt, including current maturities |
31,752 | 33,437 | 35,545 | 37,963 | 8,563 | |||||||||||||||
| Shareholders’ equity |
$ | 31,456 | $ | 42,692 | $ | 42,392 | $ | 40,244 | $ | 36,024 | ||||||||||
| Item 7. | Management’s Discussion and Analysis of Financial Condition and Results of Operations (all dollar amounts in thousands, except per share and revenue per equivalent admissions amounts) |
This Annual Report and the documents that are incorporated by reference in this Annual Report contain certain forward-looking statements within the meaning of the safe harbor for forward-looking statements contained in the Private Securities Litigation Reform Act of 1995. Forward-looking statements include all statements that do not relate solely to historical or current facts and may be identified by the use of words such as “may,” “believe,” “will,” “seeks to”, “expect,” “project,” “estimate,” “anticipate,” “plan” or “continue.” These forward-looking statements are based on the current plans and expectations and are subject to a number of risks, uncertainties and other factors which could significantly affect current plans and expectations and our future financial condition and results. For a listing and a discussion of such factors, which could cause actual results, performance and achievements to differ materially from those anticipated, see Certain Cautionary Statements—Forward Looking Information and Item 1A included elsewhere in this Annual Report on Form 10-K.
Critical Accounting Estimates
The preparation of financial statements in accordance with U.S. generally accepted accounting principles requires us to make estimates and assumptions that affect reported amounts and related disclosures. We consider an accounting estimate to be critical if:
| • | it requires assumptions to be made that were uncertain at the time the estimate was made; and |
| • | changes in the estimate or different estimates that could have been made could have a material impact on our consolidated statement of earnings or financial condition. |
The table of critical accounting estimates that follows is not intended to be a comprehensive list of all of our accounting policies that require estimates. We believe that of our significant accounting policies, as discussed in Note 2 of our Notes to Consolidated Financial Statements included in this Annual Report on Form 10-K for the
45
Index to Financial Statements
fiscal year ended June 30, 2011, the estimates discussed below involve a higher degree of judgment and complexity. We believe the current assumptions and other considerations used to estimate amounts reflected in our consolidated financial statements are appropriate. However, if actual experience differs from the assumptions and other considerations used in estimating amounts reflected in our consolidated financial statements, the resulting changes could have a material adverse effect on our consolidated results of operations and financial condition.
The table that follows presents information about our critical accounting estimates, as well as the effects of hypothetical changes in the material assumptions used to develop each estimate:
| Balance Sheet or Income Statement Caption/Nature of Critical Estimate Item (dollar amounts in thousands, except per |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per | ||
| Receivables-net and Provision for Bad Debts | ||||
| Receivables-net for our Healthcare Facilities Segment primarily consists of amounts due from third-party payors and patients from providing healthcare services to hospital facility patients. Receivables-net for our Specialty Pharmacy Segment primarily consists of amounts due from third-party payors; institutions such as nursing homes, home health, hospice, hospitals; pharmacy stores; Medicaid Part D program; and customers from the sale of pharmacy services and merchandise. Our ability to collect outstanding receivables is critical to our results of operations and cash flows. To provide for accounts receivable that could become uncollectible in the future, we establish an allowance for doubtful accounts to reduce the carrying value of such receivables to their estimated net realizable value. The primary uncertainty lies with accounts for which patients are responsible, which we refer to as patient responsibility accounts. These accounts include both amounts payable by uninsured patients and co-payments and deductibles payable by insured patients. Our allowance for doubtful accounts, included in our balance sheets as of June 30 was as follows:
2011—$12,317; and 2010—$14,725. |
The largest component of bad debts in our patient accounts receivable for our healthcare facilities and Specialty Pharmacy Segments relates to accounts for which patients are responsible, which we refer to as patient responsibility accounts. These accounts include both amounts payable by uninsured patients and co-payments and deductibles payable by insured patients. In general, we attempt to collect deductibles, co-payments and self-pay accounts prior to the time of service for non-emergency care. If we do not collect these patient responsibility accounts prior to the delivery of care, the accounts are handled through our billing and collections processes.
We attempt to verify each patient’s insurance coverage as early as possible before a scheduled non-emergency admission or procedure, including with respect to eligibility, benefits and authorization/pre-certification requirements, in order to notify patients of the estimated amounts for which they will be responsible. We attempt to verify insurance coverage within a reasonable amount of time for all emergency room visits and non-emergency urgent admissions in compliance with the Emergency Medical Treatment and Active Labor Act. |
A significant increase in our provision for doubtful accounts (as a percentage of revenues) would lower our earnings. This would adversely affect our results of operations, financial condition, liquidity and potentially our future access to capital.
If net revenues during fiscal year 2011 were changed by 1%, our 2011 after-tax income from continuing operations would change by approximately $1,196 or diluted earnings per share of $0.15.
This is only one example of reasonably possible sensitivity scenarios. The process of determining the allowance requires us to estimate uncollectible patient accounts that are highly uncertain and requires a high degree of judgment. It is impacted by, among other things, changes in regional economic conditions, business office operations, payor mix and trends in private and federal or state governmental healthcare coverage. | ||
46
Index to Financial Statements
| Balance Sheet or Income Statement Caption/Nature of Critical Estimate Item (dollar amounts in thousands, except per |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per | ||
| Receivables-net and Provision for Bad Debts (continued) | ||||
| Our provision for bad debts, included in our results of operations, was as follows:
2011—$19,690; 2010—$22,592; and 2009—$19,735. |
In general, we utilize the following steps in collecting accounts receivable: if possible, cash collection of all or a portion of deductibles, co-payments and self-pay accounts prior to or at the time service is provided; billing and follow-up with third party payors; collection calls; utilization of collection agencies; sue to collect if the patient has the means to pay and chooses not to pay; and if collection efforts are unsuccessful, write off the accounts. |
|||
| Our policy is to write off accounts after all collection efforts have failed, which is typically no longer than 120 days after the date of discharge of the patient or service to the patient or customer. Patient responsibility accounts represent the majority of our write-offs. All of our hospitals retain third-party collection agencies for billing and collection of delinquent accounts. At most of our hospitals, more than one collection agency is used to promote competition and improved performance. The selection of collection agencies and the timing of the referral of an account to a collection agency vary among hospitals. Generally, we do not write off accounts prior to utilizing the services of a collection agency. Once collection efforts have proven unsuccessful, an account is written off from our patient accounting system against the allowance for doubtful accounts. |
||||
47
Index to Financial Statements
| Balance Sheet or Income Statement Caption/Nature of Critical Estimate Item (dollar amounts in thousands, except per |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per | ||
| Receivables-net and Provision for Bad Debts (continued) | ||||
| We determine the adequacy of the allowance for doubtful accounts utilizing a number of analytical tools and benchmarks. No single statistic or measurement alone determines the adequacy of the allowance. |
||||
| We monitor our revenue trends by payor classification on a quarter-by-quarter basis along with the composition of our accounts receivable agings. This review is focused primarily on trends in self-pay revenues, accounts receivable, co-payment receivables and historic payment patterns. |
||||
| In addition, we analyze other factors such as day’s revenue in accounts receivable and we review admissions and charges by physicians, primarily focusing on recently recruited physicians. |
||||
| Days Outstanding1 | ||||||||||||||||||||||||||||||||
| Payor Class |
0-30 | 31-60 | 61-90 | 91-120 | 121-150 | 151-180 | >180 | Total | ||||||||||||||||||||||||
| Medicare |
$ | 3,315 | $ | 343 | $ | 241 | $ | 172 | $ | 68 | $ | 49 | $ | 257 | $ | 4,445 | ||||||||||||||||
| Commercial |
2,361 | 592 | 315 | 178 | 118 | 76 | 383 | 4,023 | ||||||||||||||||||||||||
| Medicaid |
1,777 | 375 | 281 | 182 | 112 | 107 | 460 | 3,294 | ||||||||||||||||||||||||
| Self Pay |
187 | 168 | 145 | 94 | 62 | 40 | 213 | 909 | ||||||||||||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||||||
| $ | 7,640 | $ | 1,478 | $ | 982 | $ | 626 | $ | 360 | $ | 272 | $ | 1,313 | $ | 12,671 | |||||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||||||
| 1 | The above table shows, as of June 30, 2011, net hospital patient accounts receivable aged from patient date of service and are grouped by classification of verified insurance coverage. The receivables are net of contractual allowances and allowance for doubtful accounts. Contractual allowances and the allowance for doubtful accounts are calculated by payor class and are not calculated by the aging of the patient billing date; therefore, these allowances have been allocated within the aging of the various payor classes based upon gross patient receivable amounts. |
48
Index to Financial Statements
| Balance Sheet or Income Statement |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per share) | ||
| Revenue recognition / Net Patient Service Revenues |
||||
| For our Healthcare Facilities Segment, we recognize revenues in the period in which services are provided. For our Specialty Pharmacy Segment, we recognize revenues in the period in which services are provided and at the time the customer takes possession of merchandise. Patient receivables primarily consist of amounts due from third-party payors and patients. Amounts we receive for treatment of patients covered by governmental programs, such as Medicare and Medicaid, and other third-party payors, such as HMOs, PPOs and other private insurers, are determined pursuant to contracts or established government rates and are generally less than our established billing rates. Accordingly, our gross revenues and patient receivables are reduced to net amounts receivable pursuant to such contracts or government payment rates through an allowance for contractual discounts. Approximately 85.0%, 82.8% and 86.4% of our revenues during the years ended June 30, 2011, 2010 and 2009, respectively, relate to discounted charges. The sources of these revenues were as follows (as a percentage of total revenues):
Medicare—43.2%; Medicaid—14.3%; and Commercial insurance—27.5%. |
Revenues are recorded at estimated amounts due from patients, third-party payors, institutions, pharmacies, and others for healthcare and pharmacy services and goods provided net of contractual discounts pursuant to contract or government payment rates. Estimates for contractual allowances are calculated using computerized and manual processes depending on the type of payor involved. In certain hospitals, the contractual allowances are calculated by a computerized system based on payment terms for each payor. In other hospitals, the contractual allowances are estimated manually using historical collections for each type of payor. For all hospitals, certain manual estimates are used in calculating contractual allowances based on historical collections from payors that are not significant or have not entered into a contract with us. All contractual adjustments regardless of type of payor or method of calculation are reviewed and compared to actual experience on a periodic basis. |
|||
| Accounts receivable primarily consist of amounts due from third party payors, institutions, pharmacies, and patients. Amounts we receive for the treatment of patients covered by HMOs, PPOs and other private insurers are generally less than our established billing rates. We include contractual allowances as a reduction to revenues in our financial statements based on payor specific identification and payor specific factors for rate increases and denials. |
||||
49
Index to Financial Statements
| Balance Sheet or Income Statement |
Assumption / Approach
Used share) |
Sensitivity Analysis (dollar amounts in thousands, except per | ||||||||
| Revenue recognition / Net Patient Service Revenues (continued) |
||||||||||
| Governmental payors | Governmental payors | |||||||||
| Included in the Healthcare Facilities Segment’s Medicare and Medicaid net revenues for fiscal 2011 are reimbursements under the Electronic Health Records (“EHR”) provisions of the Health Information Technology for Economic and Clinical Health Act (the “HITECH Act”). The HITECH Act was enacted into law on February 17, 2009 as part of the American Recovery and Reinvestment Act of 2009 (“ARRA”). EHR reimbursements included in Healthcare Facilities Segment net revenues for fiscal 2011 are as follows: |
The majority of services performed on Medicare and Medicaid patients are reimbursed at predetermined reimbursement rates. The differences between the established billing rates (i.e., gross charges) and the predetermined reimbursement rates are recorded as contractual discounts and deducted from gross charges. Under this prospective reimbursement system, there is no adjustment or settlement of the difference between the actual cost to provide the service and the predetermined reimbursement rates. |
Because the laws and regulations governing the Medicare and Medicaid programs are complex and subject to change, the estimates of contractual discounts we record could change by material amounts. Adjustments related to final settlements for revenues retrospectively increased our revenues by the following amounts:
2011—$766; 2010—$1,194; and 2009—$233. | ||||||||
| 2011 | ||||||||||
| Medicare |
$ | 7,683 | ||||||||
| Medicaid |
1,243 | |||||||||
|
|
|
|||||||||
| Total |
$ | 8,926 | ||||||||
|
|
|
|||||||||
| Discounts for retrospectively cost-based revenues, which were more prevalent in periods before 2000, are estimated based on historical and current factors and are adjusted in future periods when settlements of filed cost reports are received. |
||||||||||
| Final settlements under all programs are subject to adjustment based on administrative review and audit by third party intermediaries, which can take several years to resolve completely. |
||||||||||
| Commercial Insurance | Commercial Insurance | |||||||||
| For most managed care plans, contractual allowances estimated at the time of service are adjusted to actual contractual allowances as cash is received and claims are reconciled. We evaluate the following criteria in developing |
If our overall estimated contractual discount percentage on all of our commercial revenues during 2011 were changed by 1%, our 2011 after-tax income from continuing operations would change by approximately $256. | |||||||||
50
Index to Financial Statements
| Balance Sheet or Income Statement |
Assumption / Approach
Used share) |
Sensitivity Analysis (dollar amounts in thousands, except per | ||||||||||
| Revenue recognition / Net Patient Service Revenues (continued) |
|
|||||||||||
| the estimated contractual allowance percentages: historical contractual allowance trends based on actual claims paid by managed care payors; review of contractual allowance information reflecting current contract terms; consideration and analysis of changes in payor mix reimbursement levels; and other issues that may impact contractual allowances. |
This is only one example of reasonably possible sensitivity scenarios. The process of determining the allowance requires us to estimate the amount expected to be received and requires a high degree of judgment. It is impacted by changes in managed care contracts and other related factors. | |||||||||||
| A significant increase in our estimate of contractual discounts would lower our earnings. This would adversely affect our results of operations, financial condition, liquidity and future access to capital. | ||||||||||||
| Goodwill, other intangible assets and accounting for business combinations | ||||||||||||
| Goodwill represents the excess of the purchase price over the fair value of the net assets (including separately identified intangible assets) of acquired companies. The Company has two reportable business segments that with goodwill. Our goodwill by business segment included in our consolidated balance sheets as of June 30 for the following years was as follows:
|
|
In accordance with FASB Accounting Standards Codification (“ASC”) 350-10, “Intangibles—Goodwill and Other,” (“ASC 350-10”) goodwill and intangible assets with indefinite lives are reviewed by us at least annually for impairment. For purposes of these analyses, our estimate of fair value is based on the income approach, which estimates the fair value based on our future discounted cash flows. Our estimate of future discounted cash flows is based on assumptions and projections we believe to be currently reasonable and supportable. If we determine the carrying value of goodwill or other intangible assets to be impaired, then we reduce the carrying value. |
As part of the fiscal 2011 goodwill and intangibles impairment analysis, the Company recognized that there has been significant declines in net revenue during FY 2011 for the Specialty Pharmacy Segment. The analysis resulted in a $6,048 goodwill impairment charge for fiscal 2011. Additionally, the Company recognized a $3,400 impairment charge to trade name and a $3,899 impairment charge to customer relationships for the fiscal year ended June 30, 2011. | |||||||||
| 2011 | 2010 | |||||||||||
| Healthcare Facilities |
$2,515 | $2,515 | ||||||||||
| Pharmacy |
461 | 6,509 | ||||||||||
|
|
|
|
|
|||||||||
| Total Goodwill |
$2,976 | $9,024 | ||||||||||
|
|
|
|
|
|||||||||
|
The goodwill resulted from the 2004 acquisition of HealthMont, Inc. and the 2008 acquisition of Carmichael.
|
|
|||||||||||
| The Company’s intangible assets relate to Certificates of Need (“CON”), non-competition agreements, trade name, customer relationships and Medicare licenses. |
The purchase price of acquisitions is allocated to the assets acquired and liabilities assumed based upon their respective fair values and are subject to change during the |
|||||||||||
51
Index to Financial Statements
| Balance Sheet or Income Statement |
Assumption / Approach
Used share) |
Sensitivity Analysis (dollar amounts in thousands, except per | ||||||||||
| Goodwill, other intangible assets and accounting for business combinations (continued) | ||||||||||||
| CON, Non-competition agreements, customer relationships, and Medicare licenses are amortized over the terms of the agreements. The trade name has been determined to have an indefinite life and, accordingly, is not amortized. Our other intangible assets by business segment included in our consolidated balance sheets as of June 30 for the following years was as follows:
|
|
twelve month period subsequent to the acquisition date. We engage independent third-party valuation firms to assist us in determining the fair values of assets acquired and liabilities assumed at the time of acquisition. Such valuations require us to make significant estimates and assumptions, including projections of future events and operating performance.
Fair value estimates are derived from independent appraisals, established market values of comparable assets, or internal calculations of estimated future net cash flows. Our estimate of future cash flows is based on assumptions and projections we believe to be currently reasonable and supportable. Our assumptions take into account revenue and expense growth rates, patient volumes, changes in payor mix, and changes in legislation and other payor payment patterns. |
||||||||||
| 2011 | 2010 | |||||||||||
| Healthcare Facilities |
||||||||||||
| Certificates of Need |
$ | 630 | $ | 630 | ||||||||
| Noncompetition agreements |
83 | 83 | ||||||||||
|
|
|
|
|
|||||||||
| 713 | 713 | |||||||||||
| Accumulated amortization |
(280 | ) | (226 | ) | ||||||||
|
|
|
|
|
|||||||||
| $ | 433 | $ | 487 | |||||||||
|
|
|
|
|
|||||||||
| Pharmacy |
||||||||||||
| Trade name |
$ | 2,000 | $ | 5,400 | ||||||||
| Customer relationships |
1,089 | 6,400 | ||||||||||
| Medicare License |
769 | 769 | ||||||||||
|
|
|
|
|
|||||||||
| 3,858 | 12,569 | |||||||||||
| Accumulated amortization |
(453 | ) | (1,280 | ) | ||||||||
|
|
|
|
|
|||||||||
| $ | 3,405 | $ | 11,289 | |||||||||
|
|
|
|
|
|||||||||
| Total |
$ | 3,838 | $ | 11,776 | ||||||||
|
|
|
|
|
|||||||||
| Professional and general liability claims | ||||||||||||
| We are subject to potential medical malpractice lawsuits and other claims as part of providing healthcare services. To mitigate a portion of this risk, we have maintained insurance for individual malpractice claims exceeding a self-insured retention amount. For the periods March 1, 2008 to February 28, 2009, March 1, 2009 to February 2010, March 1, 2010 to |
The reserve for professional and general liability claims is based upon independent actuarial calculations, which consider historical claims data, demographic considerations, severity factors and other actuarial assumptions in the determination of reserve estimates. |
Actuarial calculations include a large number of variables that may significantly impact the estimate of ultimate losses recorded during a reporting period. In determining loss estimates, professional judgment is used by each actuary by selecting factors that are considered appropriate by the actuary for our specific circumstances. | ||||||||||
52
Index to Financial Statements
| Balance Sheet or Income Statement Caption/Nature of Critical Estimate Item (dollar amounts in thousands, except per |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per | ||
| Professional and general liability claims (continued) | ||||
| February 28, 2011 and March 1, 2011 to February 28, 2012 our self-insured retention level was $1,000 on individual malpractice claims.
Each year, we obtain quotes from various malpractice insurers with respect to the cost of obtaining medical malpractice insurance coverage. We compare these quotes to our most recent actuarially determined estimates of losses at various self-insured retention levels. Accordingly, changes in insurance costs affect the self-insurance retention level we choose each year. As insurance costs increase, we may accept a higher level of risk in self-insured retention levels.
The reserve for professional and general liability claims included in our consolidated balance sheets as of June 30 was as follows:
2011—$4,143; and 2010—$3,343.
The total expense for professional and general liability coverage, included in our consolidated results of operations, was as follows:
2011—$ 1,968; 2010—$ 1,495; and 2009—$1,962. |
The reserve for professional and general liability claims reflects the current estimate of all outstanding losses, including incurred but not reported losses, based upon actuarial calculations as of the balance sheet date. The loss estimates included in the actuarial calculations may change in the future based upon updated facts and circumstances.
We revise our reserve estimation process by obtaining independent actuarial calculations quarterly. Our estimated reserve for professional and general liability claims will be significantly affected if current and future claims differ from historical trends. While we monitor reported claims closely and consider potential outcomes as estimated by our independent actuaries when determining our professional and general liability reserves, the complexity of the claims, the extended period of time to settle the claims and the wide range of potential outcomes complicates the estimation process. In addition, certain states, including Georgia, have passed varying forms of tort reform which attempt to limit the number and types of claims and the amount of some medical malpractice awards. If enacted limitations remain in place or if similar laws are passed in the states where our hospitals are located, our loss estimates could decrease. Conversely, liberalization of the number and type of claims and damage awards permitted under any such law applicable to our operations could cause our loss estimates to increase. |
Changes in assumptions used by our independent actuary with respect to demographics and geography, industry trends, development patterns and judgmental selection of other factors may impact our recorded reserve levels and our results of operations.
Changes in our initial estimates of professional and general liability claims are non-cash charges and accordingly, there would be no material impact currently on our liquidity or capital resources. | ||
53
Index to Financial Statements
| Balance Sheet or Income Statement Caption/Nature of Critical Estimate Item (dollar amounts in thousands, except per |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per | ||
| Accounting for income taxes | ||||
| Deferred tax assets generally represent items that will result in a tax deduction in future years for which we have already recorded the tax benefit in our income statement. We assess the likelihood that deferred tax assets will be recovered from future taxable income. To the extent we believe that recovery is not probable, a valuation allowance is established. To the extent we establish a valuation allowance or increase this allowance, we must include an expense as part of the income tax provision in our results of operations. Our net deferred tax asset balance (net of valuation allowance) in our consolidated balance sheets as of June 30 for the following years was as follows:
2011—$8,372; and 2010—$4,405.
Our valuation allowances for deferred tax assets in our consolidated balance sheets as of June 30 for the following years were as follows:
2011—$2,078; and 2010—$1,350.
In addition, significant judgment is required in determining and assessing the impact of certain tax-related contingencies. We establish accruals when, despite our belief that our tax return positions are fully supportable, it is probable that we have incurred a loss related to tax contingencies and the loss or range of loss can be reasonably estimated.
We adjust the accruals related to tax contingencies as part of our provision for income taxes in our results of operations based upon changing facts and circumstances, such as the progress of a tax audit, development of industry related examination |
The first step in determining the deferred tax asset valuation allowance is identifying reporting jurisdictions where we have a history of tax and operating losses or are projected to have losses in future periods as a result of changes in operational performance. We then determine if a valuation allowance should be established against the deferred tax assets for that reporting jurisdiction.
The second step is to determine the amount of the valuation allowance. We will generally establish a valuation allowance equal to the net deferred tax asset (deferred tax assets less deferred tax liabilities) related to the jurisdiction identified in the first step of the analysis. In certain cases, we may not reduce the valuation allowance by the amount of the deferred tax liabilities depending on the nature and timing of future taxable income attributable to deferred tax liabilities.
In assessing tax contingencies, we identify tax issues that we believe may be challenged upon examination by the taxing authorities. We also assess the likelihood of sustaining tax benefits associated with tax planning strategies and reduce tax benefits based on management’s judgment regarding such likelihood. We compute the tax on each contingency. We then determine the amount of loss, or reduction in tax benefits based upon the foregoing and reflect such amount as a component of the provision for income taxes in the reporting period. |
Our deferred tax assets are $10,450 and our deferred tax liabilities are $0 at June 30, 2011, excluding the impact of valuation allowances. The Company believes that the likelihood of our not realizing the federal tax benefit of our net deferred tax assets is remote.
The IRS may propose adjustments for items we have failed to identify as tax contingencies. If the IRS were to propose and sustain assessments equal to 10% of our taxable loss for 2011, we would incur approximately $403 of additional tax benefit for 2011 plus applicable penalties and interest. | ||
54
Index to Financial Statements
| Balance Sheet or Income Statement Caption/Nature of Critical Estimate Item (dollar amounts in thousands, except per |
Assumption / Approach Used (dollar amounts in thousands, except per |
Sensitivity Analysis (dollar amounts in thousands, except per | ||
| Accounting for income taxes (continued) |
||||
| issues, as well as legislative, regulatory or judicial developments. A number of years may elapse before a particular matter, for which we have established an accrual, is audited and resolved. |
During each reporting period, we assess the facts and circumstances related to recorded tax contingencies. If tax contingencies are no longer deemed probable based upon new facts and circumstances, the contingency is reflected as a reduction of the provision for income taxes in the current period. |
|||
55
Index to Financial Statements
Financial Summary
The results of continuing operations shown in the historical summary below are for our two business segments, Healthcare Facilities and Specialty Pharmacy.
| Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Net Revenues—Healthcare Facilities |
$ | 141,241 | $ | 140,204 | $ | 135,431 | ||||||
| Net Revenues—Specialty Pharmacy |
39,920 | 42,962 | 46,130 | |||||||||
|
|
|
|
|
|
|
|||||||
| Total Net Revenues |
181,161 | 183,166 | 181,561 | |||||||||
| Costs and expenses |
(176,545 | ) | (182,452 | ) | (175,975 | ) | ||||||
| Impairment of goodwill and intangible assets |
(13,347 | ) | — | — | ||||||||
| Impairment of construction in progress |
— | (1,202 | ) | (433 | ) | |||||||
| Gain on Sale of Home Health businesses |
— | 2,342 | — | |||||||||
|
|
|
|
|
|
|
|||||||
| Operating Profit |
(8,731 | ) | 1,854 | 5,153 | ||||||||
| Interest Expense |
(7,433 | ) | (3,471 | ) | (3,765 | ) | ||||||
| Interest Income |
5 | 14 | 50 | |||||||||
| Gains of sale of assets |
— | — | 180 | |||||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from continuing operations before income taxes |
$ | (16,159 | ) | $ | (1,603 | ) | $ | 1,618 | ||||
|
|
|
|
|
|
|
|||||||
| Healthcare Facilities Segment: |
||||||||||||
| Admissions |
6,197 | 6,818 | 7,683 | |||||||||
|
|
|
|
|
|
|
|||||||
| Equivalent Admissions |
18,702 | 20,062 | 20,343 | |||||||||
|
|
|
|
|
|
|
|||||||
| Surgeries |
2,635 | 3,301 | 3,069 | |||||||||
|
|
|
|
|
|
|
|||||||
| Revenue per Equivalent Admission |
$ | 7,552 | $ | 6,989 | $ | 6,657 | ||||||
|
|
|
|
|
|
|
|||||||
Equivalent admissions—Equivalent admissions is used by management (and certain investors) as a general approximation of combined inpatient and outpatient volume. Equivalent admissions are computed by multiplying admissions (inpatient volume) by the sum of gross inpatient revenues and gross outpatient revenues and dividing the result by gross inpatient revenues. The equivalent admissions computation is intended to relate outpatient revenues to the volume measure (admissions) used to measure inpatient volume to result in a general approximation of combined inpatient and outpatient volume (equivalent admissions).
Results of Operations
Our net revenues are from our two business segments, Healthcare Facilities and Specialty Pharmacy.
Healthcare Facilities Segment
Net revenue for the year ended June 30, 2011 were $141,241 with a total of 18,702 equivalent admissions and revenues per equivalent admission of $7,552 compared to net revenues of $140,204, a total of 20,062 equivalent admissions and revenues per equivalent admission of $6,989 for the year ended June 30, 2010.
The 0.7% increase in net revenues for the year ended June 30, 2011 was due primarily to decreased self pay and commercial and other revenues offset by increases in Medicare and Medicaid revenues due to receipt of Electronic Health Records (“EHR”) incentive reimbursement. Net revenues for the fiscal year ended June 30, 2011 included revenues of $766 for the settlements and filings of prior year Medicare and Medicaid cost reports compared to net revenue of $1,194 for the fiscal year ended June 30, 2010. Net revenue for the fiscal year ended June 30, 2011 and 2010, included net revenues of $1,201 and $3,091 respectively, from state indigent care programs. Net outpatient service revenues decreased $7,927, an 11.8% decrease from last year to $59,299, and decreased to 42.0% of net revenues from 48.0% last year.
56
Index to Financial Statements
Included in the in net revenues for the fiscal year ended June 30, 2011 is approximately $8,926 for EHR incentive reimbursement. The Health Information Technology for Economic and Clinical Health Act (the “HITECH Act”) was enacted into law on February 17, 2009 as part of the American Recovery and Reinvestment Act of 2009 (“ARRA”). The HITECH Act includes provisions designed to increase the use of Electronic Health Records by both physicians and hospitals. Beginning with federal fiscal year 2011 and extending through federal fiscal year 2016, eligible hospitals and critical access hospitals CAH participating in the Medicare and Medicaid programs are eligible for reimbursement incentives based on successfully demonstrating meaningful use of its certified EHR technology. Conversely, those hospitals that do not successfully demonstrate meaningful use of EHR technology are subject to reductions in reimbursements beginning in FY 2015. On July 13, 2010, the DHHS released final meaningful use regulations. Meaningful use criteria are divided into three distinct stages: I, II and III. The final rules specify the initial criteria for: physicians, eligible hospitals, and CAHs necessary to qualify for incentive payments; calculation of the incentive payment amounts; payment adjustments under Medicare for covered professional services and inpatient hospital services; eligible hospitals and CAHs failing to demonstrate meaningful use of certified EHR technology; and other program participation requirements.
The final rule set the earliest interim payment date for the incentive payment at May 2011. This was a delay from the initial October 2010 date: however, the first year of the Medicare portion of the program is defined as the Federal government fiscal year October 1, 2010 to September 30, 2011. The Medicaid portion of the program will be administered by the various state authorities based upon the criteria in the final rules.
Attestation of meaningful use requirements for the first year (October 1, 2010 – September 30, 2011) began on April 18, 2011. Each of SunLink’s six hospitals and its formerly owned Chilton Medical Center registered for the program with the Centers for Medicare and Medicaid Services (“CMS”) and on April 18, 2011 all successfully attested compliance with Part I of the Medicare EHR incentive program for such first year.
As of June 30, 2011, SunLink has received $7,731 in EHR Medicare incentive reimbursement for the six hospitals for fiscal the year then ended and $790, or 75%, for its formerly owned Chilton Medical Center in accordance with the sale agreement. The Company also accrued Medicaid EHR reimbursement for Mississippi and Missouri of $277 and $825, respectively, and $141 for its formerly owned Chilton Medical Center. No amount has been accrued for Georgia Medicaid EHR incentive payments since the reimbursement program has not yet been established by the state. The amounts accrued are the estimates of the incentive payments for the periods earned through June 30, 2011.
Net revenues for the year ended June 30, 2010 were $140,204 with a total of 20,062 equivalent admissions and revenues per equivalent admission of $6,989 compared to net revenues of $135,431, a total of 20,343 equivalent admissions and revenues per equivalent admission of $6,657 for the year ended June 30, 2009. The 3.5% increase in net revenues for the year ended June 30, 2010 was due primarily to increased self pay and commercial and other revenues offset by decreases in Medicare and Medicaid revenues, a 5.0% increase in net revenues per equivalent admission and increased revenue from settlements and filings of prior year Medicare and Medicaid cost reports. Net revenues for the fiscal year ended June 30, 2010 included revenues of $1,194 for the settlements and filings of prior year Medicare and Medicaid cost reports compared to net revenue of $233 for the fiscal year ended June 30, 2009. Self-pay revenues increased due to fewer patients having insurance and increased deductibles and co-insurance for insured patients. Self-pay revenues increased 30.5% in the fiscal year ended June 30, 2010 and commercial revenues increased 1.6%. Net revenue for the fiscal year ended June 30, 2010 and 2009, included net revenues of $3,091 and $2,878 respectively, from state indigent care programs. Net outpatient service revenues increased $3,536, a 5.6% increase from the prior year to $67,225, and increased to 48.0% of net revenues from 47.0% the prior year.
The recruitment of new doctors and spending for capital improvements have contributed to the increase in Healthcare Facilities net revenues in the years ended June 30, 2011, 2010 and 2009, respectively. We experienced a net loss of four doctors during the fiscal year ended June 30, 2011, added three net new doctors during the fiscal year ended June 30, 2010, and added two net new doctors during the fiscal year ended June 30, 2009. During the fiscal year ended June 30, 2011, SunLink expensed $333 on physician guarantees and recruiting
57
Index to Financial Statements
expenses compared to $596 last year. We also have expended approximately $6,830 for capital expenditures to upgrade services and facilities since July 1, 2008. We believe the upgraded services and facilities contributed to the increase in net revenue per equivalent admission for the years ended June 30, 2011 and 2010, respectively, compared to the prior years. We continue to seek increased patient volume by attracting additional physicians to our hospitals, upgrading the services offered by our hospitals on an as needed basis and improving our hospitals’ physical facilities based on the availability of capital resources and our assessment of expected return on capital.
The following table sets forth the percentage of net patient revenues, including EHR incentive reimbursements for fiscal year 2011, from major payors for the Healthcare Facilities Segment for the periods indicated:
| Fiscal Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Source |
||||||||||||
| Medicare |
43.2 | % | 39.1 | % | 40.2 | % | ||||||
| Medicaid |
14.3 | % | 12.9 | % | 14.9 | % | ||||||
| Self pay |
15.0 | % | 17.3 | % | 13.6 | % | ||||||
| Commercial Insurance & Other |
27.5 | % | 30.7 | % | 31.3 | % | ||||||
|
|
|
|
|
|
|
|||||||
| 100.0 | % | 100.0 | % | 100.0 | % | |||||||
|
|
|
|
|
|
|
|||||||
The increase in net revenues for the year ended June 30, 2011 was due to increased Medicare and Medicaid revenues offset by decreases in self pay and commercial and other revenues. Medicare net revenues increased $6,102, an 11.1% increase from last year, and 4.1% as a percentage of total net revenues in fiscal year 2011 compared to fiscal year 2010. This increase was due to $7,682 of EHR incentive reimbursements recorded in net revenues for fiscal year 2011. Medicaid net revenues increased $2,066, an 11.4% increase from last year, and increased 1.4% as a percentage of total net revenues in fiscal year 2011 compared to fiscal year 2010. The increase in fiscal year 2011 was due to Medicaid EHR incentive reimbursements of $1,243 recorded in net revenue for fiscal year 2011. Commercial Insurance and Other decreased $4,291, a 10.0% decrease from last year to $38,823 for the fiscal year ended June 30, 2011 and decreased to 27.8% of net revenues from 30.7% last year. Self-pay revenues decreased $2,990, a 12.4% decrease from last year to $21,127 for the fiscal year ended June 30, 2011 and decreased to 15.1% of net revenues from 17.2% last year. The changes were due primarily to increased patients without medical insurance and increased deductibles and co-insurance required for insured patients.
Specialty Pharmacy Segment
Net revenues were $39,920, $42,962 and $46,130 for the fiscal years ended June 30, 2011, 2010 and 2009, respectively. Fiscal 2011 net revenues decreased $3,042, or 7.1%, as compared to fiscal 2010 net revenues primarily as a result of the loss of certain direct contracts for institutional pharmacy products and services of $2,731 and a decrease in durable medical equipment sales of $532. The decrease resulted from a decrease in pharmacy revenue, primarily due to lower sales of pharmacy products due to the loss of supply arrangements with two long-term care facilities compared to the prior year. Fiscal 2010 net revenues decreased $3,168, or 6.9%, as compared to the fiscal prior year. The decrease resulted from decreases in pharmacy net revenues, primarily one infusion therapy drug prescribed for premature babies at high risk for lung disease, and durable medical equipment sales. During Fiscal 2010, Louisiana Medicaid, the major payor for this infusion therapy drug, reduced the utilization of the drug, thereby reducing net revenues of the Specialty Pharmacy Segment by $4,315 for Fiscal 2010.
58
Index to Financial Statements
Healthcare Facilities Segment Cost and Expenses
Costs and expenses for our Healthcare Facilities, including depreciation and amortization, were $129,943, $135,206, and $126,691, for the fiscal years ended June 30, 2011, 2010 and 2009, respectively.
| Cost and Expenses as a % of Net Revenue Years Ended June 30, |
||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Salaries, wages and benefits |
44.2 | % | 45.5 | % | 45.6 | % | ||||||
| Provision for bad debts |
13.0 | % | 15.0 | % | 13.7 | % | ||||||
| Supplies |
9.1 | % | 10.0 | % | 9.7 | % | ||||||
| Purchased services |
7.0 | % | 6.9 | % | 6.9 | % | ||||||
| Other operating expenses |
13.6 | % | 12.9 | % | 12.0 | % | ||||||
| Rent and lease expense |
1.9 | % | 1.8 | % | 1.8 | % | ||||||
| Depreciation and amortization expense |
3.0 | % | 3.4 | % | 3.6 | % | ||||||
Salaries, wages and benefits expense as a percentage of total net revenues decreased in the year ended June 30, 2011 compared to the prior year due to fewer employed physicians. At June 30, 2011 there were 28 employed physicians compared to 37 at June 30, 2010.
Provision for bad debts decreased as a percentage of net revenue in the year ended June 30, 2011 compared to the prior year due lower self-pay net revenues. Self-pay revenues decreased $2,990 or 12.4% in the current fiscal year. Provision for bad debts increased as a percentage of net revenue in the year ended June 30, 2010 compared to the prior year due to fewer people being eligible for Medicaid due to more stringent Medicaid requirements, increased coinsurance and deductible amounts that insured persons have to pay, overall decreased collections as a percentage of revenues and higher self-pay net revenues. Self-pay revenues increased $5,638 or 30.5% in the fiscal year 2010.
Other operating expenses increased as a percentage of net revenues in the year ended June 30, 2011 compared to the prior year due to increased insurance expense. The increase in other operating expenses was also due to recording a new healthcare provider tax for our three Georgia healthcare facilities as other expense. Provider tax recorded in other expense was $2,814 and $2,075 for the fiscal years ended June 30, 2011 and 2010, respectively. States in which the Company operates hospitals have imposed and increased their provider tax in the last two years.
Other operating expenses increased as a percentage of net revenues in the year ended June 30, 2010 compared to the prior year due to recording state provider tax as other expense in 2010. For the fiscal year ended June 30, 2010, the Missouri and Mississippi hospitals paid state provider tax totaling $2,064, which is included in other operating expenses as opposed to Medicaid contractual allowances where they had been classified in prior years. The reclassification was done to more properly show these taxes as expenses for providing patient care.
Depreciation and amortization expense was $4,209, $4,719, and $4,917 for the years ended June 30, 2011, 2010 and, 2009, respectively. The decrease in fiscal year 2011 depreciation and amortization expense compared to fiscal year 2010 resulted from assets being fully depreciated in the current year as compared to prior years.
59
Index to Financial Statements
Specialty Pharmacy Segment Cost and Expenses
Cost and expenses for our Specialty Pharmacy Segment, including depreciation and amortization, was $41,036, $43,383 and $44,334 for the fiscal years ended June 30, 2011, 2010 and 2009, respectively.
| Cost and Expenses as a % of Net Revenue Years Ended June 30, |
||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Cost of goods sold |
69.7 | % | 68.8 | % | 67.1 | % | ||||||
| Salaries, wages and benefits |
17.4 | % | 16.3 | % | 14.6 | % | ||||||
| Provision for bad debts |
3.2 | % | 3.5 | % | 5.1 | % | ||||||
| Supplies |
0.5 | % | 0.6 | % | 0.4 | % | ||||||
| Purchased services |
3.7 | % | 4.1 | % | 2.4 | % | ||||||
| Other operating expenses |
3.6 | % | 3.2 | % | 2.8 | % | ||||||
| Rent and lease expense |
0.8 | % | 0.6 | % | 0.6 | % | ||||||
| Depreciation and amortization expense |
3.9 | % | 3.8 | % | 3.3 | % | ||||||
Cost of goods sold as a percent of net revenues increased in the fiscal year ended June 30, 2011 as compared to the prior year due to changes in sales product mix, offset slightly by favorable pricing negotiations and discounts earned with certain suppliers. Generally, Medicare and Medicaid reimbursement rates decreased in fiscal 2011 as compared to the prior year. Salaries, wages and benefits increased as a percent of net revenues in fiscal 2011 as compared to the prior year primarily due to increased staffing in the accounting and business office areas needed for implementing new software systems and implementing and improving system controls and procedures as a result of changes in the operations effected by management. Purchased services decreased as a percent of net revenues in fiscal 2011 as compared to the prior year due to reductions in the use of accounting consulting services and legal costs as compared to the prior year. The provision for bad debts as a percent of net revenues decreased during fiscal 2011 as the improved controls and procedures in the business office increased collections of accounts receivable resulting in lower uncollectible account write-offs.
Corporate Overhead Costs and Expenses
Cost and expenses for Corporate Overhead including depreciation and amortization, was $5,566, $5,065 and $5,382 for the fiscal years ended June 30, 2011, 2010 and 2009, respectively. The increase in the fiscal year ended June 30, 2011 from the prior year was due to $483 of severance expense paid for four corporate employees. The decrease in the fiscal year ended June 30, 2010 from the prior year was due to decreased legal and audit expenses, decreased directors’ fees and stock option compensation expense, partially offset by increased depreciation expense.
Impairment of Goodwill and Intangible Assets
As part of the fiscal 2011 goodwill and intangibles impairment analysis, the Company recognized that there has been slower than anticipated growth in from the Specialty Pharmacy Segment. The analysis resulted in a $6,048 goodwill impairment charge for fiscal 2011. Additionally, the Company recognized a $3,400 impairment charge to trade name and a $3,899 impairment charge to customer relationships for the fiscal year ended June 30, 2011.
Impairment of Goodwill and Intangible Assets
As part of the fiscal 2011 goodwill and intangibles impairment analysis, the Company recognized that there has been a continuing decline in the revenues and operating profit from the Specialty Pharmacy Segment. The analysis resulted in a $6,048 goodwill impairment charge for fiscal 2011 for goodwill resulting from the April 2008 acquisition of Carmichael. Additionally, the Company recognized a $3,400 impairment charge to trade name and a $3,899 impairment charge to customer relationships acquired in the April 2008 acquisition of Carmichael for the fiscal year ended June 30, 2011. Declines in pharmacy products and services revenues during the fiscal year ended June 30, 2011 resulted from the loss of direct sales contracts for institutional pharmacy
60
Index to Financial Statements
products and lower retail demand. Eight long-term care facilities converted their supply contracts to pharmacy management contracts in the fourth quarter of fiscal 2011 and these pharmacy management contracts yield lower operating profit margins for Carmichael. The continuing depressed local economy of Carmichael’s service area has resulted in lower sales for retail pharmacy and durable medical equipment products and we have projected these lower sales volumes will continue.
The following table summarizes goodwill and intangible asset impairment charges for the fiscal year ended June 30, 2011:
| June 30, 2011 |
||||
| Specialty Pharmacy Segment |
||||
| Goodwill |
$ | 6,048 | ||
| Intangible assets |
||||
| Trade Name |
3,400 | |||
| Customer Relationships |
3,899 | |||
|
|
|
|||
| Total |
$ | 13,347 | ||
|
|
|
|||
Impairment of Construction in Progress
In August 2007, the Company received final approval of a Certificate of Need (“CON”) application with the State of Georgia to build a replacement hospital in Ellijay, Georgia and incurred CON application costs, land use, architecture and building consultants costs which were capitalized as construction in progress. SunLink exercised its option to purchase land in Ellijay to build the replacement hospital; however, the owner failed to close. We are currently in litigation with the owner and are pursuing a claim for damages against the owner based upon the owner’s failure to close the sale as agreed. The outcome of the litigation is uncertain. During the year ended June 30, 2009, SunLink expensed $433 of costs which had been capitalized relating to the land. During the fiscal year ended June 30, 2010, an additional $1,202 that had been incurred and capitalized prior to June 30, 2009 was expensed. These capitalized costs relate to CON, architecture and building consultants costs for the projected building site. The project to build a replacement hospital in Ellijay, Georgia at a site other than the existing hospital location is now considered remote due to the difficulty in obtaining a suitable building site. The Company is considering alternatives for upgrading the facilities at the existing hospital site.
Operating Profit
Operating loss was $8,731 for the year ended June 30, 2011 and operating income was $1,854 and $5,153 for the years ended June 30, 2010 and, 2009, respectively. The operating loss in the year ended June 30, 2011 compared to the prior year was due to an impairment charge of $6,508 against goodwill and $7,299 against intangible assets associated with the Specialty Pharmacy Segment. The decrease in operating profit in the year ended June 30, 2010 compared to the prior year was due to a decrease in net revenues for the Specialty Pharmacy Segment, an increase in cost and expenses, especially provision for bad debts and other operating expenses and an increase in the impairment of construction in process offset by the gain on sale of three home health businesses included in operating profit.
Interest expense was $7,433, $3,471, and $3,765 for the years ended June 30, 2011, 2010 and, 2009, respectively. The increase in fiscal years 2011 interest expense resulted from 1,485 in waiver fees paid as required under the Credit Facility Waiver, $990 of increased deferred financing cost amortization this year resulting from the change in the termination date of the Credit Facility from April 2017 to September 2011 and increased rates charged as a result of the Credit Facility Waiver. As of June 30, 2011 and 2010, our outstanding balance on our credit agreement was $31,853 and $33,386, respectively. The outstanding balance on our revolving line of credit was $5,300 and $0 as of June 30, 2011 and 2010, respectively.
We recorded income tax benefit of $5,607 ($5,514 federal tax benefit and $93 state tax benefit) for the year ended June 30, 2011 compared to income tax benefit of $745 ($581 federal tax benefit and $164 state tax benefit) for the year ended June 30, 2010 and income tax expense of $813 ($788 federal and $25 state tax expense) for
61
Index to Financial Statements
the year ended June 30, 2009. The $5,514 federal tax benefit for the year ended June 30, 2011 included a $4,515 deferred tax benefit. The deferred tax benefit resulted primarily from impairment of goodwill and intangible assets of the Specialty Pharmacy Segment during the fourth quarter of fiscal year 2011. The $581 federal tax expense for the year ended June 30, 2010 included a $1,495 deferred tax benefit. The $788 federal tax expense for the year ended June 30, 2009 included a $1,428 deferred tax benefit. We had an estimated net operating loss carry-forward for federal income tax purposes of approximately $6,150 at June 30, 2011. Use of this net operating loss carry-forward is subject to the limitation provisions of Internal Revenue Code Section 382. As a result, not all of the net operating loss carry-forward is available to offset federal taxable income in the current year. We have provided a valuation allowance for $2,078 of our $8,372 gross deferred tax asset (the majority of which is the net operating loss carry-forward for federal income tax purposes). Based upon management’s assessment that it was more likely than not that a portion of its deferred tax asset (primarily its net operating losses subject to limitation) would not be recovered, the Company established a valuation allowance for the portion of the domestic tax asset which may not be utilized.
Loss from continuing operations was $10,552 ($1.30 loss per fully diluted share) for the year ended June 30, 2011 compared to loss from continuing operations of $858 ($0.11 loss per fully diluted share) for the year ended June 30, 2010 and earnings from continuing operations of $1,618 ($0.10 per fully diluted share) for the year ended June 30, 2009. Loss from continuing operations in fiscal 2011 resulted from an impairment charge of $6,048 against goodwill and $7,299 against intangible assets associated with the Specialty Pharmacy Segment, decreased net revenues for the Specialty Pharmacy Segment and an increase in interest expense partially offset by the EHR incentive reimbursements. Loss from continuing operations in fiscal 2010 resulted from an increase in cost and expenses, especially provision for bad debts, other operating expenses and the increased impairment of construction in progress partially offset by the gain on sale of three home health businesses included in operating profit. Earnings from continuing operations in fiscal 2009 decreased from fiscal 2008 due to increased operating profit which resulted from settlements and filings of prior year Medicare and Medicaid cost reports and the reversal of the lease guarantee obligation recorded during the Healthmont acquisition.
Loss from discontinued operations of $163 for the year ended June 30, 2011 primarily resulted from $228 of earnings after tax expense attributable to our former Mountainside operations, due to the settlement of a lawsuit, $55 of losses after tax benefit resulting from domestic pension items and $336 of losses after tax expense from our formerly owned Chilton Medical Center resulting from $724 of pre-tax loss from operations offset by $438 related to the pre-tax gain on the sale of the operations of Chilton Medical Center. Earnings from discontinued operations of $960 for the year ended June 30, 2010 primarily resulted from $1,493 of after tax expense attributable to our former Mountainside operations, $400 of losses after tax benefit attributable to our former KRUG UK operations, primarily due to legal expenses, $61 of losses after tax benefit resulting from domestic pension items and $72 of losses after tax benefit from operations of our formerly owned Chilton Medical Center. Earnings from discontinued operations of $107 for the year ended June 30, 2009 resulted from $77 of losses after tax benefit from Mountainside, $135 of losses after tax benefit from KRUG UK, primarily due to legal expenses, $33 of losses after tax benefit resulting from domestic pension items offset by $262 of earnings after tax expense from operations of our formerly owned Chilton Medical Center.
Net loss for the year ended June 30, 2011 was $10,715 ($1.32 loss per fully diluted share) compared to net earnings of $102 ($0.01 per fully diluted share) for the year ended June 30, 2010 and $912 ($0.11 per fully diluted share) for the year ended June 30, 2009.
Earnings before income taxes, interest, depreciation and amortization
Earnings before income taxes, interest, depreciation and amortization (“EBITDA”) represent the sum of income before income taxes, interest, depreciation and amortization. We understand that certain industry analysts and investors generally consider EBITDA to be one measure of the liquidity of a company, and it is presented to assist analysts and investors in analyzing the ability of a company to generate cash, service debt and meet capital requirements. We believe increased EBITDA is an indicator of improved ability to service existing debt and to satisfy capital requirements. EBITDA, however, is not a measure of financial performance under accounting principles generally accepted in the United States of America and should not be considered an alternative to net
62
Index to Financial Statements
income as a measure of operating performance or to cash liquidity. Because EBITDA is not a measure determined in accordance with accounting principles generally accepted in the United States of America and is thus susceptible to varying calculations, EBITDA, as presented, may not be comparable to other similarly titled measures of other corporations. Where we adjust EBITDA for non-cash charges we refer to such measurement as “Adjusted EBITDA”, which we report on a company wide basis. Non-cash adjustments in Adjusted EBITDA are not intended to be identified or characterized in any respect as “non-recurring, infrequent or unusual,” if we believe such charge is reasonably likely to recur within two years, or if there was a similar charge (or gain) within the prior two years. Where we report Adjusted EBITDA, we typically also report Hospital Facilities Segment Adjusted EBITDA and Specialty Pharmacy Segment Adjusted EBITDA which is the EBITDA for the applicable segments without any allocation of corporate overhead, which we report as a separate line item, and without any allocation of the non-cash adjustments, which we also report as a separate line item in Adjusted EBITDA. Net cash provided by operations for the years ended June 30, 2011, 2010 and 2009, respectively, is shown below.
| Years ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Healthcare Facilities Adjusted EBITDA |
$ | 15,507 | $ | 10,915 | $ | 13,672 | ||||||
| Specialty Pharmacy Adjusted EBITDA |
446 | 1,218 | 3,394 | |||||||||
| Corporate overhead costs |
(5,106 | ) | (4,616 | ) | (5,017 | ) | ||||||
| Taxes and net interest expense |
(1,966 | ) | (2,815 | ) | (4,668 | ) | ||||||
| Other non-cash expenses and net changes in operating assets and liabilities |
(4,102 | ) | (774 | ) | (2,951 | ) | ||||||
|
|
|
|
|
|
|
|||||||
| Net cash provided by operations |
$ | 4,779 | $ | 3,928 | $ | 4,430 | ||||||
|
|
|
|
|
|
|
|||||||
Liquidity and Capital Resources
We generated $4,779 of cash from operations during the year ended June 30, 2011 compared to $3,928 from operations during the prior year. Cash was generated from receipt of $8,521 in EHR incentive reimbursements in May 2011.
We generated $3,928 of cash from operations during the year ended June 30, 2010 compared to $4,430 from operations during the comparable period of the prior year. Cash was generated from net earnings, non-cash expenses of impairment of construction in process and depreciation, and cash provided by discontinued operations partially offset by decreased accounts payable and accrued expenses.
SunLink expended $2,844, $2,502 and $1,484 for capital expenditures at our Healthcare Facilities and Specialty Pharmacy Segments during the years ended June 30, 2011, 2010 and 2009, respectively. We believe an attractive and up-to-date physical facilities assist in recruiting quality staff and physicians, as well as attracting patients, and the capital expenditures in fiscal year 2011 related primarily to information technology capital for the Healthcare Facilities and Specialty Pharmacy Segments.
SunLink’s Credit Facility at June 30, 2011 is comprised of a revolving line of credit of up to $9,000 with an interest rate at LIBOR plus 10.5% (13.25% at June 30, 2011) (the “Revolving Loan”) of which $5,300 was outstanding and a Term Loan with an outstanding balance of $29,086 with an interest rate at LIBOR plus 12.07% (14.82% at June 30, 2011) (the “Term Loan”). A modification to the Credit Facility was entered into on July 28, 2011 (“July 2011 Modification”) at which time SunLink made an $8,000 prepayment of the Term Loan and paid a modification fee of $131. The source of the repayment was $2,500 of proceeds from a private placement of SunLink common shares primarily to directors and affiliates and $5,500 of operating funds. Under the July 2011 Modification, the interest rate under the Revolving Loan was adjusted to LIBOR plus 8.875%, or 11.625% and the interest rate under the Term Loan was adjusted to LIBOR plus 10.82%, or 13.57%. The termination date of the Credit Facility was changed to January 1, 2013. The maximum availability of the Revolving Loan is $9,000
63
Index to Financial Statements
and is keyed to the calculated net collectible value of eligible accounts receivable. The financial covenants were also adjusted in the July 2011 Modification. The Credit Facility is secured by a first priority security interest in substantially all real and personal property of the Company and its consolidated domestic subsidiaries, including a pledge of all of the equity interests in such subsidiaries.
The Credit Facility contains various terms and conditions, including operational and financial restrictions and limitations, and affirmative and negative covenants. The covenants include financial covenants measured on a quarterly basis which require SunLink to comply with maximum leverage and minimum fixed charge ratios, maximum capital expenditure amounts, collateral value to loan amount and liquidity and cash flow measures, all as defined in the Credit Facility. Although SunLink was not in compliance with certain of the financial covenants contained in the Credit Facility at June 30, 2011, the Credit Facility was subsequently amended by the July 2011 Modification to change the affected covenants so as to bring us into compliance. At June 30, 2011, SunLink was in compliance with the financial covenants of the Credit Facility as modified in the July 28, 2011 modification. We believe that the Company should be able to continue in compliance with the revised levels of financial covenants and terms in the Credit Facility during the fiscal year ending June 30, 2012, but there is no assurance that the Company will remain in compliance with all of the terms and conditions of the Credit Facility in subsequent fiscal quarters. The July 28, 2011 modification includes other conditions related to Term Loan reductions by September 30, 2011 and December 31, 2011 which if not met may increase the interest rate for both the Term Loan and the Revolving Loan by an additional 0.5% over the prescribed interest rate for the remainder of the agreement. If the Term Loan reduction covenants are met, the interest rate for both the Term Loan and the Revolving Loan may decrease by an additional 1.25% over the prescribed interest rate for the remainder of the agreement. If we fail to remain in compliance with the Credit Facility, we would cease to have a right to draw on the revolving line of credit facility and the lenders would, among other things, be entitled to call a default and demand repayment of the indebtedness outstanding. If SunLink or its applicable subsidiaries experience a material adverse change in their business, assets, financial condition, management or operations, or if the value of the collateral securing the Credit Facility decreases, we may be unable to draw on the credit facility.
We believe we have adequate financing and liquidity to support our current level of operations through the next twelve months under the Credit Facility if we remain in compliance with all the current terms as modified. Failure to remain in compliance with all the terms of the Credit Facility could have adverse material effects on the Company. Our primary sources of liquidity are cash generated from continuing operations and availability under Revolving Loan component of the Credit Facility. The total availability of credit under the Revolving Loan is keyed to the level of SunLink’s calculated net collectible value of eligible accounts receivable, which was $7,860 of which $5,300 was outstanding at June 30, 2011. The current remaining availability under the Revolving Loan could be adversely affected by, among other things, the risk, uncertainties and other factors listed at the beginning of Item 7, as well as lower earnings due to lower demand for our services by patients, changes in patient mix and changes in terms and levels of government and private reimbursement for services. Cash generated from operations could be adversely affected by, among other things, the risks, uncertainties and other factors listed at the beginning of Item 7, as well as lower patient demand for our services, higher operating costs (including, but not limited to, salaries, wages and benefits, provisions for bad debts, general liability and other insurance costs, cost of pharmaceutical drugs and other operating expenses) or by changes in terms and levels of government and private reimbursement for services, and the regulatory environment of the community hospital segment.
64
Index to Financial Statements
Contractual Obligations, Commitments and Contingencies
Contractual obligations related to long-term debt, non-cancelable operating leases and interest on outstanding debt from continuing operations at June 30, 2011 is shown in the following table. The interest on variable interest debt is calculated at the interest rate in effect at June 30, 2011.
| Payments due in: |
Long-Term Debt |
Subordinated Long-Term Debt |
Operating Leases |
Interest on Long-Term Debt |
Interest on Subordinated Long-Term Debt |
|||||||||||||||
| 1 year |
$ | 1,814 | $ | 300 | $ | 2,749 | $ | 3,079 | $ | 188 | ||||||||||
| 2 years |
27,409 | 300 | 1,249 | 1,343 | 164 | |||||||||||||||
| 3 years |
32 | 300 | 771 | 1 | 140 | |||||||||||||||
| 4 years |
— | 1,597 | 594 | — | 64 | |||||||||||||||
| 5 years |
— | — | 373 | — | — | |||||||||||||||
| More than 5 years |
— | — | 700 | — | — | |||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|||||||||||
| $ | 29,255 | $ | 2,497 | $ | 6,436 | $ | 4,423 | $ | 556 | |||||||||||
|
|
|
|
|
|
|
|
|
|
|
|||||||||||
At June 30, 2011, SunLink had guarantee agreements with three physicians. A physician with whom a guarantee agreement is made generally agrees to maintain his or her practice within a hospital geographic area for a specific period (normally three years) or be liable to repay all or a portion of the guarantee received. The physician’s liability for any guarantee repayment due to non-compliance with the provisions of a guarantee agreement generally is collateralized by the physician’s patient accounts receivable and/or a promissory note from the physician. All potential payments payable under the three guarantees have been paid as of June 30, 2011. SunLink expensed $333, $596, and $750, for the fiscal years ended June 30, 2011, 2010 and 2009, respectively. There were no remaining non-cancelable commitments under guarantee agreements with physicians as of June 30, 2011.
At June 30, 2011, we had outstanding long-term debt of $29,255 of which $29,086 was incurred in connection with the Credit Facility and $169 was related to capital leases. At June 30, 2010, we had outstanding long-term debt of $30,887 of which $30,836 was incurred in connection with the Credit Facility and $51 was related to capital leases.
On December 7, 2007, Southern Health Corporation of Ellijay, Inc. (“SHC-Ellijay”) filed a Complaint against James P. Garrett and Roberta Mundy, both individually and as Fiduciary of the Estate of Randy Mundy (collectively, “Defendants”), seeking specific performance of an Option Agreement (the “Option Agreement”) dated April 17, 2007, between SHC-Ellijay, Mr. Garrett, and Ms. Mundy as Executrix of the Estate of Randy Mundy for the sale of approximately 24.74 acres of real property located in Gilmer County, Georgia, and recovery of SHC-Ellijay’s damages suffered as a result of Defendants’ failure to close the transaction in accordance with the Option Agreement. SHC-Ellijay also stated alternative claims for breach of the Option Agreement and fraud, along with claims to recover attorney’s fees and punitive damages.
In January 2008, the Mundys filed a motion to strike, motion to dismiss, answer, affirmative defenses, and a counterclaim against SHC-Ellijay. On March 3, 2009, SHC-Ellijay filed a First Amended and Restated Complaint for Damages, which effectively dropped the cause of action for specific performance of the Option Agreement. On May 7, 2009, Mr. Garrett and Ms. Mundy served a motion for summary judgment on all counts and causes of action stated in the First Amended Complaint. The court has postponed consideration of the defendants’ motion for summary judgment and SHC-Ellijay’s response thereto until after a discovery dispute between the parties has been resolved.
In July 2011, SHC-Ellijay filed a reply brief in further support of its motion for partial summary judgment on the complaint and full summary judgment on the Defendants’ counterclaims and brief in opposition to Defendants’ cross motion for summary judgment. The summary judgment motions remain pending.
65
Index to Financial Statements
SunLink denies that it has any liability to the Mundys and intends to vigorously defend the claims asserted against SunLink by the Mundys complaint and to vigorously pursue its claims against the Mundys. While the ultimate outcome and materiality of the litigation cannot be determined, in management’s opinion the litigation will not have a material adverse effect on SunLink’s financial condition or results of operations.
SunLink is a party to claims and litigation incidental to its business, for which it is not currently possible to determine the ultimate liability, if any. Based on an evaluation of information currently available and consultation with legal counsel, management believes that resolution of such claims and litigation is not likely to have a material effect on the financial position, cash flows, or results of operations of the Company. The Company expenses legal costs as they are incurred.
Sarbanes-Oxley Section 404
This Annual Report on Form 10-K does not include an attestation report of our registered public accounting firm regarding internal controls over financial reporting. Management’s report was not subject to attestation by our independent registered public accounting firm pursuant to the permanent exemption for non-accelerated filers from the internal control audit requirement of Section 404(b) of the Sarbanes-Oxley Act of 2002 (“SOX”) enacted under Section 989G of the Dodd-Frank Wall Street Reform and Consumer Protection Act.
Recent Accounting Pronouncements
In June 2009, the FASB issued SFAS No. 168, The FASB Accounting Standards Codification™ and the Hierarchy of Generally Accepted Accounting Principles (ASC 105, Generally Accepted Accounting Principles) “ASC 105”. ASC 105 replaces SFAS No. 162, The Hierarchy of Generally Accepted Accounting Principles, and establishes the FASB Accounting Standards Codification™ (“Codification”) as the source of authoritative accounting principles recognized by the FASB to be applied by nongovernmental entities in the preparation of financial statements in conformity with GAAP. On the effective date of this Statement, the Codification superseded all then-existing non-SEC accounting and reporting standards. ASC 105 became effective for financial statements issued for interim and annual periods ending after September 15, 2009. The Codification is effective for the accompanying interim financial statements and the principal impact is limited to disclosures as all future references to authoritative literature will be referenced in accordance with the Codification.
In July 2011, the FASB issued ASU 2011-7, Health Care Entities (Topic 954)—Presentation and Disclosure of Patient Service Revenue, Provision for Bad Debts, and the Allowance for Doubtful Accounts for Certain Health Care Entities (“ASU 2011-7”). In accordance with ASU 2011-7, the Company will be required to present its provision for doubtful accounts related to patient service revenue as a deduction from revenue, similar to contractual discounts. Accordingly, the Company’s revenues will be required to be reported net of both contractual discounts as well as its provision for doubtful accounts related to patient service revenues. Additionally, ASU 2011-7 will require the Company to make certain additional disclosures designed to help users understand how contractual discounts and bad debts affect recorded revenue in both interim and annual financial statements. ASU 2011-7 is required to be applied retrospectively and is effective for public companies for fiscal years beginning after December 15, 2011, and interim periods within those fiscal years. Early adoption is permitted. The adoption of ASU 2011-7 is not expected to impact the Company’s financial position, results of operations or cash flows although it will change the presentation of the Company’s revenues on its statements of operations as well as requiring additional disclosures.
In June 2011, the FASB issued ASU 2011-5, Comprehensive Income (Topic 220)—Presentation of Comprehensive Income (“ASU 2011-5”). ASU 2011-5 eliminates the Company’s currently elected option to present components of other comprehensive income as part of the statement of changes in stockholders’ equity. Instead, ASU 2011-5 requires that all non-owner changes in stockholders’ equity be presented either in a single continuous statement of comprehensive income or in two separate but consecutive statements. ASU 2011-5 is required to be applied retrospectively and is effective for public companies for fiscal years beginning after
66
Index to Financial Statements
December 15, 2011, and interim periods within those fiscal years. Early adoption is permitted. The Company anticipates applying the provisions of ASU 2011-5 for its fiscal year ending June 30, 2012. The adoption of ASU 2011-5 is not expected to impact the Company’s financial position, results of operations or cash flows prospectively.
In September 2006, the FASB issued new accounting guidance related to fair value measurements and related disclosures. This new guidance defined fair value, established a framework for measuring fair value, and expanded disclosures about fair value measurements. We adopted this new guidance on July 1, 2008, as required for our financial assets and financial liabilities. However, the FASB deferred the effective date of this new guidance for one year as it related to fair value measurement requirements for nonfinancial assets and liabilities that are recognized or disclosed at fair value on a recurring basis. We adopted these remaining provisions on July 1, 2009. The adoption of this accounting guidance did not have a material impact on our consolidated financial statements.
In December 2007, the FASB issued new accounting guidance related to the accounting for non controlling interests in consolidated financial statements. This guidance established accounting and reporting standards for the noncontrolling interest in a subsidiary and for the deconsolidation of a subsidiary. This guidance required that noncontrolling interests in subsidiaries be reported in the equity section of the controlling company’s balance sheet. It also changed the manner in which the net income of the subsidiary is reported and disclosed in the controlling company’s income statement. This guidance is effective for fiscal years beginning after December 15, 2008. We adopted this guidance on July 1, 2009 and reclassified minority interest to the equity section of the balance sheet. (See Note 12—Noncontrolling Interest)
Related Party Transactions
A director of the Company and the Company’s secretary are members of two different law firms, each of which provides services to SunLink. We have paid an aggregate of $896, $585, and $1,154 to these law firms in the fiscal years ended June 30, 2011, 2010 and 2009, respectively.
Inflation
During periods of inflation and labor shortages, employee wages increase and suppliers pass along rising costs to us in the form of higher prices for their supplies and services. We have not always been able to offset increases in operating costs by increasing prices for our services and products or by implementing cost control measures. We are unable to predict our ability to control future cost increases or offset future cost increases by passing along the increased cost to customers.
| Item 7A. | Quantitative and Qualitative Disclosures about Market Risk |
We are exposed to interest rate changes, primarily as a result of borrowing under our Credit Facility. There was $29,086 in borrowings outstanding at June 30, 2011 under the Credit Facility at interest rates based upon LIBOR. A one percent change in the LIBOR rate would result in a change in interest expense of $290 on an annual basis. No action has been taken to mitigate our exposure to interest rate market risk and we are not a party to any interest rate market risk management activities.
67
Index to Financial Statements
| Item 8. | Financial Statements and Supplementary Data |
Index to Financial Statements and Supplementary Data
| Page | ||||
| F-1 | ||||
| F-2 | ||||
| F-3 | ||||
| F-4 | ||||
| Consolidated Statements of Cash Flows—for each of the three years ended June 30, 2011, 2010 and 2009 |
F-5 | |||
| F-6 | ||||
| Item 9. | Changes in and Disagreements with Accountants on Accounting and Financial Disclosure |
None.
| Item 9A. | Controls and Procedures |
Disclosure Controls and Procedures—We maintain controls and procedures designed to ensure that we are able to collect the information we are required to disclose in the reports we file with the SEC, and to process, summarize and disclose this information within the time periods specified in the rules of the SEC.
Our management, with the participation of our Chief Executive Officer and Chief Financial Officer, has evaluated the effectiveness of disclosure controls and procedures (as such term is defined in Rules 13a-15(e) and 15d-15(e) under the Securities and Exchange Act of 1934 as amended (the “Exchange Act”)) as of the end of the period covered by this report. Based on such evaluation, our Chief Executive Officer and Chief Financial Officer have concluded that, as of the end of such period, our disclosure controls and procedures are effective.
Changes in Internal Controls over Financial Reporting—There were no changes to our internal control over financial reporting during the year ended June 30, 2011 that materially affected, or are reasonably likely to materially affect, our internal control over financial reporting.
| Item 9B. | Other Information |
None.
68
Index to Financial Statements
PART III
| Item 10. | Directors, Executive Officers and Corporate Governance |
Audit Committee Financial Expert
We have a separately-designated standing audit committee established in accordance with section 3(a)(58)(A) of the Securities Exchange Act of 1934. The members of our Committee are Messrs. Ford (Chairman) and Hall and Ms. Brenner. All three members of the committee are independent as defined in Section 121 (A) of the NYSE Amex stock exchange’s listing standards. Our Board of Directors has determined that we have at least one “audit committee financial expert” as defined under Item 401(h) of Regulation S-K serving on our audit committee. Mr. Ford is an “audit committee financial expert” and is independent as defined under the applicable SEC and NYSE Amex Equities exchange rules.
Code of Ethics
We have adopted a Code of Ethics (SunLink Health Systems, Inc. Code of Conduct) within the meaning of Item 406(b) of Regulation S-K. The Code of Ethics applies to all employees including our principal executive officer, principal financial officer and principal accounting officer. The Code of Ethics is publicly available on our website at www.sunlinkhealth.com or upon request by writing to us. If we make substantial amendments to our Code of Ethics or grant any waiver for the three previously named individuals, including any implicit waivers, we will disclose the nature of such amendment or waiver on our website or in a report on Form 8-K within five days of such amendment or waiver.
Other Information
Certain information required by this Item 10 will be set forth in the Company’s Proxy Statement for its Annual Meeting of Shareholders scheduled to be held on November 14, 2011, except for certain information concerning the executive officers of the Company which is set forth in Part I of this Report.
| Item 11. | Executive Compensation |
The information required by this Item 11 will be set forth in the Company’s Proxy Statement for its Annual Meeting of Shareholders scheduled to be held on November 7, 2011, and is incorporated herein by this reference.
| Item 12. | Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters |
The information required by this Item 12 will be set forth in the Company’s Proxy Statement for its Annual Meeting of Shareholders scheduled to be held on November 7, 2011, and is incorporated herein by this reference.
| Item 13. | Certain Relationships and Related Transactions and Director Independence |
The information required by this Item 13 will be set forth in the Company’s Proxy Statement for its Annual Meeting of Shareholders scheduled to be held on November 7, 2011, and is incorporated herein by this reference.
| Item 14. | Principal Accounting Fees and Services |
The information required by this Item 14 will be set forth in the Company’s Proxy Statement for its Annual Meeting of Shareholders scheduled to be held on November 7, 2011, and is incorporated herein by this reference.
69
Index to Financial Statements
PART IV
| Item 15. | Exhibits, Financial Statement Schedules and Reports on Form 8-K |
(a) (1) Financial Statements
The following consolidated financial statements of the Company and its subsidiaries are set forth in Item 8 of this Annual Report on Form 10-K.
| Report of Independent Registered Public Accounting Firm. |
||
| Consolidated Balance Sheets—June 30, 2011 and 2010. |
||
| Consolidated Statements of Earnings and Loss—For the Years Ended June 30, 2011, 2010 and 2009. |
||
| Consolidated Statements of Shareholders’ Equity—For the Years Ended June 30, 2011, 2010 and 2009. |
||
| Consolidated Statements of Cash Flows—For the Years Ended June 30, 2011, 2010 and 2009. |
||
| Notes to Consolidated Financial Statements—For the Years Ended June 30, 2011, 2010 and 2009. |
||
(a) (2) Financial Statement Schedules
| Report of Independent Registered Public Accounting Firm |
At page 74 of this Report. | |||
| Schedule II Valuation and Qualifying Accounts |
At page 75 of this Report. |
The information required to be submitted in Schedules I, III, IV and V for SunLink Health Systems, Inc. and its consolidated subsidiaries has either been shown in the financial statements or notes, or is not applicable or not required under Regulation S-X and, therefore, has been omitted.
(a) (3) See Item 15(b) below. Each management contract or compensatory plan or arrangement required to be filed as an Exhibit is identified below by an asterisk.
(b) Exhibits
The following exhibits are filed with this Form 10-K or incorporated herein by reference from the document set forth next to the exhibit in the list below. Exhibit numbers refer to Item 601 of Regulation S-K:
| 2.1 | Asset Purchase Agreement, dated April 9, 2004, by and among Piedmont Mountainside Hospital, Inc., Piedmont Medical Center, Inc., Southern Health Corporation of Jasper, Inc., Southern Health Corporation, SunLink Healthcare Corp. and SunLink Health Systems, Inc. (incorporated by reference from Exhibit 2.1 of the Company’s Report on Form 8-K filed April 14, 2004). (Commission File No. 04731963) | |||
| 3.1 | Amended Articles of Incorporation of SunLink Health Systems, Inc. (incorporated by reference from Exhibit 3.1 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 3.2 | Code of Regulations of SunLink Health Systems, Inc., as amended (incorporated by reference from Exhibit 3.2 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 3.3 | Certificate of Amendment to Amend Article Fourth of the Amended Articles of Incorporation of SunLink Health Systems, Inc. dated February 13, 2004 (incorporated by reference from Exhibit 3.1 of the Company’s Report on Form 10-Q for the quarter ended December 31, 2003). (Commission File No. 04610446) | |||
| 4.1 | Shareholder Rights Agreement dated as of February 8, 2004, between SunLink Health Systems, Inc. and Wachovia Bank, N.A., as Rights Agent (incorporated by reference from Exhibit 4.1 of the Company’s Report on Form 8-K filed February 10, 2004). (Commission File No. 04582922) | |||
70
Index to Financial Statements
| 10.1* | 2001 Long-Term Stock Option Plan (incorporated by reference from Exhibit 10.5 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 10.2* | 2001 Outside Directors’ Stock Ownership and Stock Option Plan (incorporated by reference from Exhibit 10.6 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 10.3* | Employment Letter, dated April 30, 2001, by and between SunLink Health Systems, Inc. and Mark Stockslager (incorporated by reference from Exhibit 10.29 of SunLink’s Form 10-Q for the quarter ended September 30, 2005). (Commission File No. 051197210) | |||
| 10.4 | Stock Purchase Agreement among SunLink Homecare Services, LLC, Carmichael’s Cashway Pharmacy, Inc., Theodore S. Carmichael and Judy Chiasson Carmichael dated April 22, 2008 (the “Carmichael Agreement”) (incorporated by reference from Exhibit 10.28 of the Company’s Report on Form 8-K filed April 29, 2008). (Commission File No. 08787122) | |||
| 10.5* | Amended and Restated Employment Agreement, dated July 1, 2005, between Robert M. Thornton, Jr. and SunLink Health Systems, Inc. (incorporated by reference from Exhibit 99.1 of the Company’s Report on Form 8-K filed December 23, 2005). (Commission File No. 051285094) | |||
| 10.6 | Credit Agreement between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., Southern Health Corporation of Jasper, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink Homecare Services, LLC, KRUG Properties, Inc., Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC dated April 23, 2008 (incorporated by reference from Exhibit 10.29 of the Company’s Report on Form 8-K filed April 29, 2008). (Commission File No. 08787122) | |||
| 10.7* | 2005 Equity Incentive Plan (incorporated by reference from Exhibit 99.1 of the Company’s Registration Statement on Form S-8 filed September 20, 2006). (Commission File No. 061100389) | |||
| 10.8 | Agreement of Understanding, dated June 28, 2007, between Christopher H. B. Mills and SunLink Health Systems, Inc. (incorporated by reference from Exhibit 99.2 of the Company’s Report on Form 8-K filed July 16, 2007). (Commission File No. 07982325) | |||
| 10.9* | Employment Letter dated September 30, 2002, by and between SunLink Healthcare Corp. and Jack M. Spurr, Jr. (incorporated by reference from Exhibit 10.27 of the Company’s Report on Form 10-K dated September 24, 2007). (Commission File No. 017732454) | |||
| 10.10 | Amended and Restated Credit Agreement between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., Southern Health Corporation of Jasper, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink Homecare Services, LLC, KRUG Properties, Inc., Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC and Union Bank of California, N.A. dated August 1, 2008 (incorporated by reference from the Company’s Annual Report on Form 10-K for the year ended June 30, 2009). (Commission File No. 081091964) | |||
| 10.11* | Executive Bonus Plan for 2009 (incorporated by reference from Exhibit 10.13 of the Company’s Report on Form 8-K filed November 18, 2008). (Commission File No. 081199137) | |||
| 10.12 | Letter Agreement regarding the Carmichael Agreement dated March 3, 2009 (incorporated by reference from Exhibit 99.1 to Current Report on Form 8-K filed March 30, 2009). (Commission File No. 09696285) | |||
71
Index to Financial Statements
| 10.13 | Limited Waiver Agreement Under Amended and Restated Credit Agreement between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., Southern Health Corporation of Jasper, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink Homecare Services, LLC, KRUG Properties, Inc., Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC dated September 27, 2010 (incorporated by reference from the Company’s Annual Report on Form 10-K for the year ended June 30, 2010). (Commission File No. 101119914) | |||
| 10.14 | Limited Consent and Modification of Loan Documents between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink ScriptsRX, LLC, Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC dated March 1, 2011 (incorporated by reference from the Company’s Quarterly Report on Form 10-Q for the quarter ended March 31, 2011). (Commission File No. 11842673) | |||
| 10.15 | Purchase and Sale Agreement between Central Alabama Medical Associates, LLC and Clanton Hospital, LLC dated March 1, 2011 (incorporated by reference from the Company’s Quarterly Report on Form 10-Q for the quarter ended March 31, 2011). (Commission File No. 11842673) | |||
| 10.16 | Third Modification to Loan Documents between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink ScriptsRX, LLC, Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc., and Chatham Credit Management III, LLC dated July 28, 2011 (incorporated by reference from Exhibit 10.9 to Current Report on Form 8-K filed August 1, 2011). (Commission File No. 111000498) | |||
| 10.17 | Lease Agreement between Central Alabama Medical Associates, LLC and Clanton Hospital, LLC dated March 1, 2011. | |||
| 10.18 | * | Management Services Agreement dated November 15, 2010, by and between SunLink Health Systems, Inc. and Centric Management Services Co., LLC. | ||
| 10.19 | * | Employment letter dated September 23, 2010 with an effective date of September 30, 2010, by and between SunLink ScriptsRx, LLC and Byron D. Finn. | ||
| 21.1 | List of Subsidiaries. | |||
| 23.1 | Consent of Cherry, Bekaert & Holland, L.L.P. | |||
| 31.1 | Chief Executive Officer’s Certification Pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934. | |||
| 31.2 | Chief Financial Officer’s Certification Pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934. | |||
| 32.1 | Chief Executive Officer’s Certification Pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002. | |||
| 32.2 | Chief Financial Officer’s Certification Pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002. | |||
| * | Management contract or compensatory plan or arrangement. |
72
Index to Financial Statements
SIGNATURES
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, SunLink Health Systems, Inc. has duly caused this Report to be signed on its behalf by the undersigned, thereunto duly authorized, on this 26th day of September, 2011.
| SUNLINK HEALTH SYSTEMS, INC. | ||
| By: | /s/ ROBERT M. THORNTON, JR. | |
| Robert M. Thornton, Jr. Chairman and Chief Executive Officer | ||
Pursuant to the requirements of the Securities Exchange Act of 1934, this Report has been signed below by the following persons on behalf of SunLink Health Systems, Inc. and in the capacities and on the dates indicated:
| Name |
Title |
Date | ||
| /s/ ROBERT M. THORNTON, JR. Robert M. Thornton, Jr. |
Director, Chairman, President and Chief Executive Officer (principal executive officer) |
September 26, 2011 | ||
| /s/ MARK J. STOCKSLAGER Mark J. Stockslager |
Chief Financial Officer and Principal Accounting Officer (principal accounting officer) |
September 26, 2011 | ||
| /s/ STEVEN J. BAILEYS, D.D.S. Steven J. Baileys, D.D.S. |
Director |
September 26, 2011 | ||
| /s/ KAREN B. BRENNER Karen B. Brenner |
Director |
September 26, 2011 | ||
| /s/ GENE E. BURLESON Gene E. Burleson |
Director |
September 26, 2011 | ||
| /s/ C. MICHAEL FORD C. Michael Ford |
Director |
September 26, 2011 | ||
| /s/ MICHAEL HALL Michael Hall |
Director |
September 26, 2011 | ||
| /s/ CHRISTOPHER H. B. MILLS Christopher H. B. Mills |
Director |
September 26, 2011 | ||
| /s/ HOWARD E. TURNER Howard E. Turner |
Director |
September 26, 2011 | ||
73
Index to Financial Statements
REPORT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM
Board of Directors and Shareholders of
SunLink Health Systems, Inc.
We have audited the consolidated financial statements of SunLink Health Systems, Inc. and subsidiaries (the “Company”) as of June 30, 2011 and 2010 and for each of the years in the three-year period ended June 30, 2011 and have issued our report thereon dated September 26, 2011; such consolidated financial statements and report are included elsewhere in this Form 10-K. Our audits also included the consolidated financial statement schedules of the Company, listed in Item 15 for each of the years in the three-year period ended June 30, 2011. These consolidated financial statement schedules are the responsibility of the Company’s management. Our responsibility is to express an opinion based on our audits. In our opinion, such consolidated financial statement schedules, when considered in relation to the basic consolidated financial statements taken as a whole, present fairly in all material respects the information set forth therein.
/s/Cherry, Bekaert & Holland, L.L.P.
Atlanta, Georgia
September 26, 2011
74
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC. AND SUBSIDIARIES
SCHEDULE II—VALUATION AND QUALIFYING ACCOUNTS
(amounts in thousands)
| Column A |
Column B | Column C | Column D | Column E | ||||||||||||||||
| Allowance for Accounts |
Balance at Beginning Of Year |
Charged to Cost and Expenses |
Currency Translation/ Acquisition/ (Disposition) |
Deductions from Reserves |
Balance at End of Year |
|||||||||||||||
| Year Ended June 30, 2011 |
$ | 14,725 | $ | 19,690 | $ | (2,305 | ) | $ | (19,793 | ) | $ | 12,317 | ||||||||
| Year Ended June 30, 2010 |
$ | 12,795 | $ | 22,592 | $ | — | $ | (20,662 | ) | $ | 14,725 | |||||||||
| Year Ended June 30, 2009 |
$ | 14,138 | $ | 20,934 | $ | — | $ | (22,277 | ) | $ | 12,795 | |||||||||
| Deferred Income Tax Asset Valuation Allowance |
Balance at Beginning Of Year |
Charged to Cost and Expenses/ (Benefit) |
Currency Translation/ Acquisition/ (Disposition) |
Deductions from Reserves |
Balance at End of Year |
|||||||||||||||
| Year Ended June 30, 2011 |
$ | 1,350 | $ | 4,515 | $ | — | $ | (3,778 | ) | $ | 2,087 | |||||||||
| Year Ended June 30, 2010 |
$ | 2,724 | $ | (1,495 | ) | $ | — | $ | 121 | $ | 1,350 | |||||||||
| Year Ended June 30, 2009 |
$ | 2,810 | $ | (1,428 | ) | $ | — | $ | 1,342 | $ | 2,724 | |||||||||
75
Index to Financial Statements
INDEX TO EXHIBITS
| 2.1 | Asset Purchase Agreement, dated April 9, 2004, by and among Piedmont Mountainside Hospital, Inc., Piedmont Medical Center, Inc., Southern Health Corporation of Jasper, Inc., Southern Health Corporation, SunLink Healthcare Corp. and SunLink Health Systems, Inc. (incorporated by reference from Exhibit 2.1 of the Company’s Report on Form 8-K filed April 14, 2004). (Commission File No. 04731963) | |||
| 3.1 | Amended Articles of Incorporation of SunLink Health Systems, Inc. (incorporated by reference from Exhibit 3.1 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 3.2 | Code of Regulations of SunLink Health Systems, Inc., as amended (incorporated by reference from Exhibit 3.2 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 3.3 | Certificate of Amendment to Amend Article Fourth of the Amended Articles of Incorporation of SunLink Health
Systems, Inc. dated February 13, 2004 (incorporated by reference from Exhibit 3.1 of the Company’s Report on Form 10-Q for the quarter ended December 31, 2003). (Commission | |||
| 4.1 | Shareholder Rights Agreement dated as of February 8, 2004, between SunLink Health Systems, Inc. and Wachovia Bank, N.A., as Rights Agent (incorporated by reference from Exhibit 4.1 of the Company’s Report on Form 8-K filed February 10, 2004). (Commission File No. 04582922) | |||
| 10.1* | 2001 Long-Term Stock Option Plan (incorporated by reference from Exhibit 10.5 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 10.2* | 2001 Outside Directors’ Stock Ownership and Stock Option Plan (incorporated by reference from Exhibit 10.6 of the Company’s Report on Form 10-Q for the quarter ended September 30, 2001). (Commission File No. 1789180) | |||
| 10.3* | Employment Letter, dated April 30, 2001, by and between SunLink Health Systems, Inc. and Mark Stockslager (incorporated by reference from Exhibit 10.29 of SunLink’s Form 10-Q for the quarter ended September 30, 2005). (Commission File No. 051197210) | |||
| 10.4 | Stock Purchase Agreement among SunLink Homecare Services, LLC, Carmichael’s Cashway Pharmacy, Inc., Theodore S. Carmichael and Judy Chiasson Carmichael dated April 22, 2008 (the “Carmichael Agreement”) (incorporated by reference from Exhibit 10.28 of the Company’s Report on Form 8-K filed April 29, 2008). (Commission File No. 08787122) | |||
| 10.5* | Amended and Restated Employment Agreement, dated July 1, 2005, between Robert M. Thornton, Jr. and SunLink Health Systems, Inc. (incorporated by reference from Exhibit 99.1 of the Company’s Report on Form 8-K filed December 23, 2005). (Commission File No. 051285094) | |||
| 10.6 | Credit Agreement between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., Southern Health Corporation of Jasper, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink Homecare Services, LLC, KRUG Properties, Inc., Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC dated April 23, 2008 (incorporated by reference from Exhibit 10.29 of the Company’s Report on Form 8-K filed April 29, 2008). (Commission File No. 08787122) | |||
| 10.7* | 2005 Equity Incentive Plan (incorporated by reference from Exhibit 99.1 of the Company’s Registration Statement on Form S-8 filed September 20, 2006). (Commission File No. 061100389) | |||
76
Index to Financial Statements
| 10.8 | Agreement of Understanding, dated June 28, 2007, between Christopher H. B. Mills and SunLink Health Systems, Inc. (incorporated by reference from Exhibit 99.2 of the Company’s Report on Form 8-K filed July 16, 2007). (Commission File No. 07982325) | |||
| 10.9* | Employment Letter dated September 30, 2002, by and between SunLink Healthcare Corp. and Jack M. Spurr, Jr. (incorporated by reference from Exhibit 10.27 of the Company’s Report on Form 10-K dated September 24, 2007). (Commission File No. 017732454) | |||
| 10.10 | Amended and Restated Credit Agreement between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., Southern Health Corporation of Jasper, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink Homecare Services, LLC, KRUG Properties, Inc., Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC and Union Bank of California, N.A. dated August 1, 2008 (incorporated by reference from the Company’s Annual Report on Form 10-K for the year ended June 30, 2009). (Commission File No. 081091964) | |||
| 10.11* | Executive Bonus Plan for 2009 (incorporated by reference from Exhibit 10.13 of the Company’s Report on Form 8-K filed November 18, 2008). (Commission File No. 081199137) | |||
| 10.12 | Letter Agreement regarding the Carmichael Agreement dated March 3, 2009 (incorporated by reference from Exhibit 99.1 to Current Report on Form 8-K filed March 30, 2009). (Commission File No. 09696285) | |||
| 10.13 | Limited Waiver Agreement Under Amended and Restated Credit Agreement between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., Southern Health Corporation of Jasper, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink Homecare Services, LLC, KRUG Properties, Inc., Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC dated September 27, 2010 (incorporated by reference from the Company’s Annual Report on Form 10-K for the year ended June 30, 2010). (Commission File No. 101119914) | |||
| 10.14 | Limited Consent and Modification of Loan Documents between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink ScriptsRX, LLC, Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc. and Chatham Credit Management III, LLC dated March 1, 2011 (incorporated by reference from the Company’s Quarterly Report on Form 10-Q for the quarter ended March 31, 2011). (Commission File No. 11842673) | |||
| 10.15 | Purchase and Sale Agreement between Central Alabama Medical Associates, LLC and Clanton Hospital, LLC dated March 1, 2011 (incorporated by reference from the Company’s Quarterly Report on Form 10-Q for the quarter ended March 31, 2011). (Commission File No. 11842673) | |||
77
Index to Financial Statements
| 10.16 | Third Modification to Loan Documents between SunLink Health Systems, Inc., SunLink Healthcare LLC, Dexter Hospital LLC, Clanton Hospital LLC, Southern Health Corporation of Ellijay, Inc., | |||
| Southern Health Corporation of Dahlonega, LLC, Southern Health Corporation of Houston, Inc., HealthMont of Georgia, Inc., HealthMont, LLC, HealthMont of Missouri, LLC, SunLink Services, Inc., SunLink ScriptsRX, LLC, Central Alabama Medical Associates, LLC, Dahlonega Clinic, LLC, Carmichael’s Cashway Pharmacy, Inc., Carmichael’s Nutritional Distributor, Inc., Breath of Life Home Health Equipment, Inc., and Chatham Credit Management III, LLC dated July 28, 2011 (incorporated by reference from Exhibit 10.9 to Current Report on Form 8-K filed August 1, 2011). (Commission File No. 111000498) | ||||
| 10.17 | Lease Agreement between Central Alabama Medical Associates, LLC and Clanton Hospital, LLC dated March 1, 2011. | |||
| 10.18 | * | Management Services Agreement dated November 15, 2010, by and between SunLink Health Systems, Inc. and Centric Management Services Co., LLC. | ||
| 10.19 | * | Employment letter dated September 23, 2010 with an effective date of September 30, 2010, by and between SunLink ScriptsRx, LLC and Byron D. Finn. | ||
| 21.1 | List of Subsidiaries. | |||
| 23.1 | Consent of Cherry, Bekaert & Holland, L.L.P. | |||
| 31.1 | Chief Executive Officer’s Certification Pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934. | |||
| 31.2 | Chief Financial Officer’s Certification Pursuant to Rule 13a-14(a) of the Securities Exchange Act of 1934. | |||
| 32.1 | Chief Executive Officer’s Certification Pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002. | |||
| 32.2 | Chief Financial Officer’s Certification Pursuant to 18 U.S.C. Section 1350, as adopted pursuant to Section 906 of the Sarbanes-Oxley Act of 2002. | |||
| * | Management contract or compensatory plan or arrangement. |
78
Index to Financial Statements
REPORT OF INDEPENDENT REGISTERED PUBLIC ACCOUNTING FIRM
Board of Directors and Shareholders of
SunLink Health Systems, Inc.
We have audited the accompanying consolidated balance sheets of SunLink Health Systems, Inc. and subsidiaries (the “Company”) as of June 30, 2011 and 2010 and the related consolidated statements of operations, shareholders’ equity, and cash flows for each of the years in the three-year period ended June 30, 2011. These consolidated financial statements are the responsibility of the Company’s management. Our responsibility is to express an opinion on these consolidated financial statements based on our audits.
We conducted our audits in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the consolidated financial statements are free of material misstatement. The Company is not required to have, nor were we engaged to perform, an audit of its internal control over financial reporting. Our audits included consideration of internal control over financial reporting as a basis for designing audit procedures that are appropriate in the circumstances, but not for the purpose of expressing an opinion on the effectiveness of the Company’s internal control over financial reporting. Accordingly, we express no such opinion. An audit also includes examining, on a test basis, evidence supporting the amounts and disclosures in the consolidated financial statements, assessing the accounting principles used and significant estimates made by management, as well as evaluating the overall financial statement presentation. We believe that our audits provide a reasonable basis for our opinion.
In our opinion, the consolidated financial statements referred to above present fairly, in all material respects, the consolidated financial position of the Company as of June 30, 2011 and 2010, and the consolidated results of its operations and its cash flows for each of the years in the three-year period ended June 30, 2011, in conformity with accounting principles generally accepted in the United States of America.
/s/Cherry, Bekaert & Holland, L.L.P.
Atlanta, Georgia
September 26, 2011
F-1
Index to Financial Statements
CONSOLIDATED BALANCE SHEETS
JUNE 30, 2011 AND 2010
| 2011 | 2010 | |||||||
| ASSETS | ||||||||
| CURRENT ASSETS: |
||||||||
| Cash and cash equivalents |
$ | 7,250 | $ | 1,704 | ||||
| Receivables—net |
16,302 | 16,036 | ||||||
| Inventory |
4,717 | 4,510 | ||||||
| Income tax receivable |
1,526 | 345 | ||||||
| Deferred income tax asset |
5,586 | 6,030 | ||||||
| Medicaid Electronic Health Records incentive reimbursement receivable |
1,243 | — | ||||||
| Prepaid expense and other |
4,447 | 4,161 | ||||||
| Current assets of Chilton Medical Center |
— | 1,848 | ||||||
|
|
|
|
|
|||||
| Total current assets |
41,071 | 34,634 | ||||||
| PROPERTY, PLANT AND EQUIPMENT—At cost |
||||||||
| Land |
2,229 | 2,229 | ||||||
| Buildings and improvements |
32,365 | 31,939 | ||||||
| Equipment and fixtures |
40,428 | 38,306 | ||||||
|
|
|
|
|
|||||
| 75,022 | 72,474 | |||||||
| Less accumulated depreciation |
36,503 | 31,118 | ||||||
|
|
|
|
|
|||||
| Property, plant and equipment—net |
38,519 | 41,356 | ||||||
| NONCURRENT ASSETS: |
||||||||
| Intangible assets—net |
3,838 | 11,776 | ||||||
| Goodwill |
2,976 | 9,024 | ||||||
| Deferred income tax asset |
2,786 | — | ||||||
| Other noncurrent assets |
346 | 1,700 | ||||||
|
|
|
|
|
|||||
| Total noncurrent assets |
9,946 | 22,500 | ||||||
|
|
|
|
|
|||||
| TOTAL ASSETS |
$ | 89,536 | $ | 98,490 | ||||
|
|
|
|
|
|||||
| LIABILITIES AND SHAREHOLDERS’ EQUITY | ||||||||
| CURRENT LIABILITIES: |
||||||||
| Accounts payable |
$ | 7,509 | $ | 7,605 | ||||
| Revolving advances |
5,300 | — | ||||||
| Current maturities of long-term debt |
1,814 | 1,797 | ||||||
| Current maturities of subordinated long-term debt |
300 | 300 | ||||||
| Accrued payroll and related taxes |
5,064 | 4,734 | ||||||
| Deferred revenue—Medicare Electronic Health Records incentive reimbursement |
839 | — | ||||||
| Income taxes |
— | 607 | ||||||
| Current liabilities of Chilton Medical Center |
— | 1,704 | ||||||
| Other accrued expenses |
2,824 | 2,359 | ||||||
|
|
|
|
|
|||||
| Total current liabilities |
23,650 | 19,106 | ||||||
| LONG-TERM LIABILITIES: |
||||||||
| Long-term debt |
27,441 | 29,090 | ||||||
| Subordinated long-term debt |
2,197 | 2,250 | ||||||
| Noncurrent deferred income tax liabilities |
— | 1,625 | ||||||
| Noncurrent liability for professional liability risks |
3,583 | 2,956 | ||||||
| Other noncurrent liabilities |
1,209 | 771 | ||||||
|
|
|
|
|
|||||
| Total long-term liabilities |
34,430 | 36,692 | ||||||
|
|
|
|
|
|||||
| COMMITMENTS AND CONTINGENCIES |
||||||||
| SHAREHOLDERS’ EQUITY: |
||||||||
| Preferred Shares, authorized and unissued, 2,000 shares |
— | — | ||||||
| Common Shares, no par value; authorized, 12,000 shares; issued and outstanding, 8,120 shares at June 30, 2011 and 8,079 shares at June 30, 2010 |
4,060 | 4,039 | ||||||
| Additional paid-in capital |
11,751 | 11,701 | ||||||
| Retained earnings |
15,850 | 26,565 | ||||||
| Accumulated other comprehensive loss |
(278 | ) | (301 | ) | ||||
|
|
|
|
|
|||||
| Total Parent Company Shareholders’ Equity |
31,383 | 42,004 | ||||||
| Noncontrolling interest |
73 | 688 | ||||||
|
|
|
|
|
|||||
| Total Shareholders’ Equity |
31,456 | 42,692 | ||||||
|
|
|
|
|
|||||
| TOTAL LIABILITIES AND SHAREHOLDERS’ EQUITY |
$ | 89,536 | $ | 98,490 | ||||
|
|
|
|
|
|||||
See notes to consolidated financial statements.
F-2
Index to Financial Statements
CONSOLIDATED STATEMENTS OF EARNINGS AND LOSS
FOR THE YEARS ENDED JUNE 30, 2011, 2010 AND 2009
(All amounts in thousands, except per share amounts)
| Years Ended | ||||||||||||
| June 30, 2011 |
June 30, 2010 |
June 30, 2009 |
||||||||||
| Net revenues |
$ | 181,161 | $ | 183,166 | $ | 181,561 | ||||||
| Costs and expenses: |
||||||||||||
| Cost of goods sold |
27,835 | 29,539 | 31,766 | |||||||||
| Salaries, wages and benefits |
72,711 | 73,522 | 71,636 | |||||||||
| Provision for bad debts |
19,690 | 22,592 | 19,735 | |||||||||
| Supplies |
13,040 | 14,224 | 13,251 | |||||||||
| Purchased services |
11,426 | 11,418 | 10,453 | |||||||||
| Other operating expenses |
22,440 | 21,404 | 19,399 | |||||||||
| Rents and leases expense |
3,172 | 2,950 | 2,839 | |||||||||
| Impairment of goodwill and intangible assets |
13,347 | — | — | |||||||||
| Impairment of construction in progress |
— | 1,202 | 433 | |||||||||
| Depreciation and amortization |
6,231 | 6,803 | 6,896 | |||||||||
| Gain on sale of Home Health Businesses |
— | (2,342 | ) | — | ||||||||
|
|
|
|
|
|
|
|||||||
| Operating profit (loss) |
(8,731 | ) | 1,854 | 5,153 | ||||||||
| Other income (expense): |
||||||||||||
| Interest expense |
(7,433 | ) | (3,471 | ) | (3,765 | ) | ||||||
| Interest income |
5 | 14 | 50 | |||||||||
| Gain on sale of assets |
— | — | 180 | |||||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from continuing operations before income taxes |
(16,159 | ) | (1,603 | ) | 1,618 | |||||||
| Income tax expense (benefit) |
(5,607 | ) | (745 | ) | 813 | |||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from continuing operations |
(10,552 | ) | (858 | ) | 805 | |||||||
| Earnings (loss) from discontinued operations, net of income taxes |
(163 | ) | 960 | 107 | ||||||||
|
|
|
|
|
|
|
|||||||
| Net earnings (loss) |
$ | (10,715 | ) | $ | 102 | $ | 912 | |||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) per share: |
||||||||||||
| Continuing operations: |
||||||||||||
| Basic |
$ | (1.30 | ) | $ | (0.11 | ) | $ | 0.10 | ||||
|
|
|
|
|
|
|
|||||||
| Diluted |
$ | (1.30 | ) | $ | (0.11 | ) | $ | 0.10 | ||||
|
|
|
|
|
|
|
|||||||
| Discontinued operations: |
||||||||||||
| Basic |
$ | (0.02 | ) | $ | 0.12 | $ | 0.01 | |||||
|
|
|
|
|
|
|
|||||||
| Diluted |
$ | (0.02 | ) | $ | 0.12 | $ | 0.01 | |||||
|
|
|
|
|
|
|
|||||||
| Net earnings (loss): |
||||||||||||
| Basic |
$ | (1.32 | ) | $ | 0.01 | $ | 0.11 | |||||
|
|
|
|
|
|
|
|||||||
| Diluted |
$ | (1.32 | ) | $ | 0.01 | $ | 0.11 | |||||
|
|
|
|
|
|
|
|||||||
| Weighted-average common shares outstanding: |
||||||||||||
| Basic |
8,094 | 8,052 | 7,975 | |||||||||
|
|
|
|
|
|
|
|||||||
| Diluted |
8,094 | 8,052 | 8,019 | |||||||||
|
|
|
|
|
|
|
|||||||
See notes to consolidated financial statements.
F-3
Index to Financial Statements
CONSOLIDATED STATEMENTS OF SHAREHOLDERS’ EQUITY
FOR THE YEARS ENDED JUNE 30, 2011, 2010 AND 2009
(All amounts in thousands)
| Common Shares |
Additional Paid-in Capital |
Retained Earnings |
Accumulated Other Comprehensive Income (Loss) |
Noncontrolling Interest |
Total Shareholders’ Equity |
|||||||||||||||||||||||
| Shares | Amount | |||||||||||||||||||||||||||
| JULY 1, 2008 |
7,932 | $ | 3,966 | $ | 11,310 | $ | 25,551 | $ | (583 | ) | $ | 615 | $ | 40,859 | ||||||||||||||
| Net earnings |
— | — | — | 912 | — | — | 912 | |||||||||||||||||||||
| Foreign currency translation adjustment |
— | — | — | — | 281 | — | 281 | |||||||||||||||||||||
| Minimum pension liability adjustment, net of tax of $12 |
(35 | ) | — | (35 | ) | |||||||||||||||||||||||
|
|
|
|||||||||||||||||||||||||||
| Total comprehensive income |
1,158 | |||||||||||||||||||||||||||
| Share-based compensation |
— | — | 190 | — | — | — | 190 | |||||||||||||||||||||
| Common shares issued |
118 | 59 | 126 | — | — | — | 185 | |||||||||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||||
| JUNE 30, 2009 |
8,050 | 4,025 | 11,626 | 26,463 | (337 | ) | 615 | 42,392 | ||||||||||||||||||||
| Net earnings |
— | — | — | 102 | — | 102 | ||||||||||||||||||||||
| Foreign currency translation adjustment |
— | — | — | — | 46 | 46 | ||||||||||||||||||||||
| Minimum pension liability adjustment, net of tax of $21 |
(10 | ) | (10 | ) | ||||||||||||||||||||||||
|
|
|
|||||||||||||||||||||||||||
| Total comprehensive income |
138 | |||||||||||||||||||||||||||
| Share-based compensation |
— | — | 40 | — | — | — | 40 | |||||||||||||||||||||
| Common shares issued |
29 | 14 | 35 | — | — | — | 49 | |||||||||||||||||||||
| Sale of noncontrolling interest |
— | — | — | — | — | 73 | 73 | |||||||||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||||
| JUNE 30, 2010 |
8,079 | 4,039 | 11,701 | 26,565 | (301 | ) | 688 | 42,692 | ||||||||||||||||||||
| Net loss |
— | — | — | (10,715 | ) | — | — | (10,715 | ) | |||||||||||||||||||
| Minimum pension liability adjustment, net of tax of $6 |
23 | 23 | ||||||||||||||||||||||||||
|
|
|
|||||||||||||||||||||||||||
| Total comprehensive loss |
(10,692 | ) | ||||||||||||||||||||||||||
| Share-based compensation |
— | — | 6 | — | — | — | 6 | |||||||||||||||||||||
| Common shares issued |
41 | 21 | 44 | — | — | — | 65 | |||||||||||||||||||||
| Change in noncontrolling interest |
— | — | — | — | — | (615 | ) | (615 | ) | |||||||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||||
| JUNE 30, 2011 |
8,120 | $ | 4,060 | $ | 11,751 | $ | 15,850 | $ | (278 | ) | $ | 73 | $ | 31,456 | ||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||||
See notes to consolidated financial statements.
F-4
Index to Financial Statements
CONSOLIDATED STATEMENTS OF CASH FLOWS
FOR THE YEARS ENDED JUNE 30, 2011, 2010 AND 2009
(All amounts in thousands)
| Years Ended | ||||||||||||
| June 30, 2011 |
June 30, 2010 |
June 30, 2009 |
||||||||||
| CASH FLOWS FROM OPERATING ACTIVITIES |
||||||||||||
| Net earnings (loss) |
(10,715 | ) | 102 | 912 | ||||||||
| Adjustments to reconcile net earnings (loss) to net cash provided by operating activities: |
||||||||||||
| Depreciation and amortization |
6,231 | 6,803 | 6,896 | |||||||||
| Stock-based compensation |
6 | 41 | 190 | |||||||||
| Impairment of goodwill and intangible assets |
13,347 | — | — | |||||||||
| Impairment of construction in process |
— | 1,202 | 433 | |||||||||
| Gain on sale of Chilton Medical Center |
(438 | ) | — | — | ||||||||
| Gain on sale of Home Health businesses |
— | (2,342 | ) | — | ||||||||
| Gain on sale of assets |
— | — | (180 | ) | ||||||||
| Change in assets and liabilities: |
||||||||||||
| Receivables |
(265 | ) | 3,430 | (1,306 | ) | |||||||
| Inventory |
(206 | ) | (70 | ) | (31 | ) | ||||||
| Prepaid expenses and other assets |
849 | (589 | ) | 20 | ||||||||
| Accounts payable and accrued expenses |
1,775 | (1,053 | ) | (101 | ) | |||||||
| Income taxes |
(1,788 | ) | (1,058 | ) | 1,110 | |||||||
| Deferred income taxes |
(3,967 | ) | (735 | ) | (1,353 | ) | ||||||
| Third-party payor settlements including electronic health records reimbursement |
(194 | ) | (602 | ) | (1,529 | ) | ||||||
| Net activities of discontinued operations |
144 | (1,201 | ) | (631 | ) | |||||||
|
|
|
|
|
|
|
|||||||
| Net cash provided by operating activities |
4,779 | 3,928 | 4,430 | |||||||||
| CASH FLOWS FROM INVESTING ACTIVITIES |
||||||||||||
| Expenditures for property, plant and equipment |
(2,640 | ) | (2,502 | ) | (1,571 | ) | ||||||
| Proceeds from sale of Home Health businesses |
— | 3,300 | — | |||||||||
| Proceeds from sale of property, plant and equipment |
— | — | 522 | |||||||||
| Proceeds from sale of noncontrolling interest |
— | 73 | — | |||||||||
|
|
|
|
|
|
|
|||||||
| Net cash provided by (used in) investing activities |
(2,640 | ) | 871 | (1,049 | ) | |||||||
| CASH FLOWS FROM FINANCING ACTIVITIES: |
||||||||||||
| Proceeds from issuance of common shares |
65 | 49 | 185 | |||||||||
| Payment of long-term debt |
(1,958 | ) | (2,108 | ) | (2,418 | ) | ||||||
| Revolving advances, net |
5,300 | (3,400 | ) | (500 | ) | |||||||
|
|
|
|
|
|
|
|||||||
| Net cash provided by (used in) financing activities |
3,407 | (5,459 | ) | (2,733 | ) | |||||||
| NET INCREASE (DECREASE) IN CASH AND CASH EQUIVALENTS |
5,546 | (660 | ) | 648 | ||||||||
| CASH AND CASH EQUIVALENTS: |
||||||||||||
| Beginning of year |
1,704 | 2,364 | 1,716 | |||||||||
|
|
|
|
|
|
|
|||||||
| End of year |
$ | 7,250 | $ | 1,704 | $ | 2,364 | ||||||
|
|
|
|
|
|
|
|||||||
| SUPPLEMENTAL DISCLOSURE OF CASH FLOW INFORMATION |
||||||||||||
| Cash paid for: |
||||||||||||
| Income taxes |
$ | 356 | $ | 1,548 | $ | 1,358 | ||||||
|
|
|
|
|
|
|
|||||||
| Interest |
$ | 4,025 | $ | 3,103 | $ | 3,395 | ||||||
|
|
|
|
|
|
|
|||||||
| Non-cash investing and financing activities: |
||||||||||||
| Assets acquired under capital lease obligation |
$ | 205 | $ | — | $ | 133 | ||||||
|
|
|
|
|
|
|
|||||||
| Long-term debt issued as payment-in-kind for interest payable |
$ | 247 | $ | — | $ | — | ||||||
|
|
|
|
|
|
|
|||||||
See notes to consolidated financial statements.
F-5
Index to Financial Statements
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
AS OF AND FOR THE YEARS ENDED JUNE 30, 2011, 2010 and 2009
(All amounts in thousands, except share and per share amounts)
| 1. | BUSINESS OPERATIONS |
SunLink Health Systems, Inc. (“SunLink”, “we”, “our”, “ours”, “us” or the “Company”) is a provider of healthcare services in certain markets in the United States. SunLink’s business is composed of two business segments:
| • | Healthcare Facilities, which consists of |
| – | Our six community hospitals which have a total of 342 licensed beds; |
| – | Our three nursing homes, each of which is located adjacent to a corresponding SunLink community hospital which have a total of 261 licensed beds; and |
| – | Our one home health agency which operates for a corresponding SunLink community hospital. |
| • | Specialty Pharmacy, which consists of |
| – | Specialty pharmacy services; |
| – | Durable medical equipment; |
| – | Institutional pharmacy services; and |
| – | Retail pharmacy products and services, all of which are conducted in rural markets. |
SunLink has conducted its healthcare facilities business since 2001 and its specialty pharmacy operations since April 2008. Our Specialty Pharmacy Segment currently is operated through Carmichael’s Cashway Pharmacy, Inc. (“Carmichael”), a subsidiary of our SunLink ScriptsRx, LLC subsidiary, and is composed of a specialty pharmacy business acquired in April 2008 with four service lines.
On April 8, 2011, SunLink Health Systems, Inc. announced that it has reached a preliminary agreement and executed a letter of intent with Foundation HealthCare Affiliates, LLC (“Foundation”) and New Age Fuel, Inc. (“New Age”), and Foundation Investment Affiliates I, LLC (“FIA”) for the non-cash merger of certain Foundation and New Age, FIA, subsidiaries and affiliates with and into newly formed acquisition subsidiaries of SunLink. The contemplated transaction is subject to a number of conditions, including completion of due diligence by each of the parties, negotiation and execution of a definitive merger agreement and consent of lenders. The subsidiaries and affiliates of Foundation contemplated to be merged into the SunLink acquisition subsidiaries per the letter of intent own minority equity interests in and manage 14 ambulatory surgery centers in seven states (Louisiana, Maryland, New Jersey, Ohio, Oklahoma, Pennsylvania and Texas), own a majority interest in and manage one general acute care hospital and manage a second acute care hospital, both of which are located in Texas. Three medical real properties, which are occupied by Foundation entities as well as other tenants in Oklahoma, are majority owned by New Age and FIA and would also be merged into the SunLink acquisition subsidiaries.
Under the Letter of Intent, the merger consideration to be issued by SunLink to the owners and affiliates of Foundation and New Age was contemplated to consist of approximately 1,560,000 SunLink common shares, approximately 133,000 shares of SunLink’s non-voting cumulative 5% Series A Preferred Stock, liquidation value $100.00 per share; approximately 277,000 shares of SunLink’s non-voting non-cumulative 4% Series B Preferred Stock, liquidation value $100.00 per share; and 3,000,000 Series A Warrants each of which would entitle the holder for three years to buy one SunLink common share at an exercise price of $6.00. In connection with the mergers, as was contemplated under the Letter of intent, SunLink would declare a stock dividend,
F-6
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
issuing to its existing holders of common shares (as of a record date to be established), approximately 133,600 shares of its Series A Preferred Stock, approximately 79,900 shares of its Series B Preferred Stock, and 3,000,000 Series B Warrants each of which will entitle the holder for three years to buy one SunLink common share at an exercise price of $6.50.
Subsequent to execution of the letter of intent, SunLink effected a private placement of 1.3 million plus common shares at an average of approximately $1.90 per share with certain of its officers and directors and/or their affiliates. The proceeds of the private placement of approximately $2,500 were used, together with other available operating funds, to make an $8,000 pre-payment on the term loan outstanding under SunLink’s 2008 Credit Facility in order to, among other things, obtain the extension of the maturity of that facility and adjust certain financial covenants to bring SunLink into compliance thereunder. Given the inadequate number of authorized but unissued SunLink common shares presently remaining after the private placement, it is currently anticipated that, among other things, the merger consideration consisting of SunLink preferred shares will be correspondingly increased and the composition of the Foundation, New Age and FIA, subsidiaries and affiliates to be merged will be modified in certain particulars to be agreed.
No approval by the shareholders of SunLink is required for the proposed mergers. However, the Series B Preferred Stock will be automatically converted into common shares of SunLink at a to be agreed conversion price , such conversion to be effected upon receipt of approval of the common shareholders of SunLink. Similarly, the Series A and Series B Warrants would not be exercisable unless and until the exercise of such warrants for SunLink common shares is approved by the common shareholders of SunLink. Promptly following closing of the mergers, SunLink intends to seek such approval by its common shareholders of conversion of the Series B Preferred Stock into SunLink common shares and of the right of the holders to the exercise of the Series A and Series B Warrants after the mergers.
Upon completion of the mergers, the combined company would expect to change its name to Foundation SunLink Healthcare Affiliates, Inc. In addition, it is anticipated that two persons designated by Foundation/New Age will join the board of directors of SunLink. Foundation SunLink is intended to be a premier healthcare facilities company positioned to respond to the changing marketplace developing under healthcare reform. Foundation SunLink’s mission will be to more closely align the interests of physicians, hospitals and related healthcare facilities to improve the quality of care and control healthcare costs in communities it serves. It is anticipated that Foundation SunLink will focus on growth through physician-centric hospitals, surgery centers and related ancillary service providers, including its existing hospitals and surgery centers, plus the aggressive acquisition and development of additional physician-centric hospitals, surgery centers and ancillary service providers nationwide.
No definitive agreement has been executed in relation to the contemplated mergers and there can be no assurance that the proposed transactions will in fact be consummated or, if consummated, that the terms and conditions referenced herein will not be changed.
| 2. | SUMMARY OF SIGNIFICANT ACCOUNTING POLICIES |
Principles of Consolidation—The consolidated financial statements include the accounts of SunLink and its domestic and foreign subsidiaries, all of which are 100% owned except for one pharmacy segment subsidiary that is 51% owned. All significant intercompany transactions and balances have been eliminated.
Management Estimates—The preparation of financial statements in conformity with accounting principles generally accepted in the United States of America requires management to make estimates and assumptions that affect the reported amounts of assets and liabilities and disclosures of contingent assets and liabilities at the date of the financial statements and the reported amounts of revenues and expenses during the reporting period. Some
F-7
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
of the more significant estimates made by management involve reserves for adjustments to net patient service revenues, evaluation of the recoverability of assets, including accounts receivable and intangible assets, and the assessment of litigation and contingencies, including income taxes and related tax asset valuation allowances, all as discussed in more detail in the remainder of these notes to the consolidated financial statements. Actual results could differ materially from these estimates.
Net Patient Service Revenue—SunLink has agreements with third-party payors that provide for payments at amounts different from established charges. Payment arrangements vary and include prospectively determined rates per discharge, reimbursed costs, discounted charges and per diem payments. Patient service revenues are reported as services are rendered at the estimated net realizable amounts from patients, third-party payors, and others. Estimated net realizable amounts are estimated based upon contracts with third-party payors, published reimbursement rates, and historical reimbursement percentages pertaining to each payor type. Estimated reductions in revenues to reflect agreements with third-party payors and estimated retroactive adjustments under such reimbursement agreements are accrued during the period the related services are rendered and are adjusted in future periods as interim and final settlements are determined. Significant changes in reimbursement levels for services under government and private programs could significantly impact the estimates used to accrue such revenue deductions. At June 30, 2011, there were no material claims or disputes with third-party payors.
Charity Care—SunLink provides care to patients who meet certain criteria under its charity care policy without charge or at amounts less than its established rates. Because SunLink does not pursue collection of amounts determined to qualify as charity, they are not reported as revenue. SunLink provided $7,657, $5,094, and $6,319, of charity care in the fiscal years ended June 30, 2011, 2010 and 2009, respectively.
Concentrations of Credit Risk—SunLink grants unsecured credit to its patients, most of who reside in the service area of SunLink’s facilities and are insured under third-party agreements. Although SunLink’s three Georgia facilities generated approximately 57% of gross revenues for the years ended June 30, 2011, 2010 and 2009 because of the geographic diversity of SunLink’s facilities and nongovernmental third-party payors, Medicare and Medicaid accounts represent SunLink’s only significant concentrations of credit risk. For SunLink’s Healthcare Facilities Segment, Medicare net revenues were approximately 42%, 39%, and 40% of net revenues for the years ended June 30, 2011, 2010 and 2009, respectively. For SunLink’s Healthcare Facilities Segment, Medicaid was approximately 14%, 13%, and 15% of net revenues for the years ended June 30, 2011, 2010 and 2009, respectively. For SunLink’s Healthcare Facilities Segment, Medicare receivables were approximately 36% and 39% of receivables—net at June 30, 2011 and 2010, respectively, while Medicaid receivables were approximately 26% and 24% of receivables—net at June 30, 2011 and 2010, respectively.
Cash and Cash Equivalents—Cash and cash equivalents consist of highly liquid financial instruments, which have original maturities of three months or less when purchased. Cash is deposited with commercial banks and may have deposits totaling amounts in excess of the federally insured limits from time to time.
Inventory—Inventory consists of medical and pharmacy supplies. Medical supplies are valued at the lower of cost or market, using the first-in, first-out method. Pharmacy supplies are stated at the lower of cost (standard cost method), or market. Use of this method does not result in a material difference from the methods required by generally accepted accounting principles in the United States of America.
Allowance for Doubtful Accounts—Substantially all of SunLink’s receivables result from providing healthcare services to hospital facility patients and from providing pharmacy services and products to customers. Accounts receivable are reduced by an allowance for doubtful accounts estimated to become uncollectible in the future. For its Healthcare Facilities, the Company calculates an allowance percentage based generally upon its historical collection experience for each type of payor. The allowance amount is computed by applying
F-8
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
allowance percentages to receivable amounts included in specific payor categories. Significant changes in reimbursement levels for services under government and private programs could significantly impact the estimates used to determine the allowance for doubtful accounts. Accounts receivable are written off after all collection efforts have failed, normally within 120 days after the date of discharge of the patient or service to the patient or customer. For its Pharmacy Operations, the Company calculates an allowance percentage based on past credit history with customers and their current financial condition. Accounts receivable are written off against the allowance for doubtful accounts when they are deemed uncollectible.
Property, Plant, and Equipment—Property, plant, and equipment, including equipment subject to capital leases, are recorded at cost. Depreciation is recognized over the estimated useful lives of the assets, which range from 3 to 45 years, on a straight-line basis. Generally, furniture and fixtures are depreciated over 5 to 10 years, machinery and equipment over 10 years, and buildings over 25 to 45 years. Leasehold improvements and leased machinery and equipment are depreciated over the lease term or estimated useful life, whichever is shorter, of the asset and range from 5 to 15 years. For our Specialty Pharmacy Segment, durable medical equipment is depreciated over 3 years. Expenditures for major renewals and replacements are capitalized. Expenditures for maintenance and repairs are charged to operating expense as incurred. When property items are retired or otherwise disposed of, amounts applicable to such items are removed from the related asset and accumulated depreciation accounts and any resulting gain or loss is credited or charged to income. Depreciation expense totaled $5,585, $5,950, and $5,977, for the years ended June 30, 2011, 2010 and 2009, respectively.
Risk Management—SunLink is exposed to various risks of loss from medical malpractice and other claims and casualties; theft of, damage to, and destruction of assets; business interruption; errors and omissions; employee injuries and illnesses; natural disasters (including earthquakes and hurricanes); and employee health, dental and accident benefits. Commercial insurance coverage is purchased for a portion of claims arising from such matters.
When, in management’s judgment, claims are sufficiently identified, a liability is accrued for estimated costs and losses under such claims, net of estimated insurance recoveries except where applicable laws, rules or regulations require us to report the gross estimate of potential or estimated losses.
By virtue of the acquisition of its initial six hospitals, SunLink assumed responsibility for professional liability claims reported after the February 1, 2001 acquisition date and the previous owner retained responsibility for all known and filed claims prior to the acquisition date. SunLink purchased claims-made commercial insurance for acts prior to and after the acquisition date. The recorded liability for professional liability risks includes an estimate of the liability for claims incurred prior to February 1, 2001, but reported after February 1, 2001, and for claims incurred after February 1, 2001. These amounts are based on actuarially determined amounts.
In connection with the acquisition of HealthMont LLC (“HealthMont”) and its two hospitals, SunLink assumed responsibility for all professional liability claims. HealthMont had purchased claims-made commercial insurance for claims made prior to the acquisition and SunLink purchased claims-made commercial insurance for claims made after the acquisition. The recorded liability for professional liability risks includes an estimate of liability for claims assumed at the acquisition and for claims incurred after the acquisition. These amounts are based on actuarially determined amounts.
The Company self-insures for workers’ compensation risk. The estimated liability for workers’ compensation risk includes estimates of the ultimate costs for both reported claims and claims incurred but not reported. Since October 1, 2006, the Company is self-insured for employee health risks. The estimated liability for employee health risk includes estimates of the ultimate costs for both reported claims and claims incurred but not reported.
F-9
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The Company accrues an estimate of losses resulting from workers’ compensation and professional liability claims to the extent they are not covered by insurance. These accruals are estimated quarterly based upon management’s review of claims reported and historical loss data.
The Company records a liability pertaining to pending litigation if it is probable a loss has been incurred and accrues the most likely amount of loss based on the information available. If no amount within the range of losses estimated from the information available is more likely than any other amount in the range of loss, the minimum amount in the range of loss is accrued. Because of uncertainties surrounding the nature of litigation and the ultimate liability to SunLink, if any, we revise estimated losses as additional facts become known.
Long-lived Assets—SunLink periodically assesses the recoverability of assets based on its expectations of future profitability and the undiscounted cash flows of the related operations and, when circumstances dictate, adjusts the carrying value of the asset to estimated fair value. These factors, along with management’s plans with respect to the operations, are considered in assessing the recoverability of long-lived assets.
Goodwill and Intangibles—Goodwill represents the cost of acquired businesses in excess of fair value of identifiable tangible and intangible net assets purchased. Goodwill has an indefinite life and is not subject to periodic amortization. However, goodwill is tested at least annually for impairment, using a fair value methodology, in lieu of amortization. Definite-life intangible assets are amortized on a straight-line basis over their estimated useful lives, generally for periods ranging from 2 to 30 years. SunLink evaluates the reasonableness of the useful lives of intangible assets and they are tested for impairment as conditions warrant.
Income Taxes—SunLink accounts for income taxes using an asset and liability approach and the recognition of deferred tax assets and liabilities for expected future tax consequences. SunLink considers all expected future events other than proposed enactments of changes in the income tax law or rates. When management determines that it is more likely than not that a portion of or none of the net deferred tax asset will be realized through future taxable earnings or implementation of tax planning strategies, management provides a valuation allowance for the portion not expected to be realized.
Share-Based Compensation—The Company issues common share options to key employees and directors under various shareholder-approved plans. Share-based compensation expense of $6, $40 and $190 for the fiscal years ended June 30, 2011, 2010 and 2009, respectively, was recorded in salaries, wages and benefits expense for share options issued to employees and directors of the Company. The fair value of the share options was estimated using the Black-Scholes option pricing model. The historical volatility is used to calculate the estimated volatility in this model.
Fair Value of Financial Instruments—The recorded values of cash, receivables, and payables approximate their fair values because of the relatively short maturity of these instruments. Similarly, the fair value of SunLink’s long-term debt is estimated to approximate its recorded values due to its current variable interest rate.
Earnings (Loss) per Share—Earnings (loss) per common share is based on the weighted-average number of common shares and dilutive common share equivalents outstanding for each period presented, including vested and unvested shares issued under SunLink’s 1995 Incentive Stock Option Plan, 2001 Long-Term Stock Option Plan, 2001 Outside Directors’ Stock Ownership and Stock Option Plan and the 2005 Equity Incentive Plan. Common share equivalents represent the dilutive effect of the assumed exercise of the outstanding stock options.
Recent Accounting Pronouncements—In July 2011, the FASB issued ASU 2011-7, “Health Care Entities (Topic 954)—Presentation and Disclosure of Patient Service Revenue, Provision for Bad Debts, and the Allowance for Doubtful Accounts for Certain Health Care Entities” (“ASU 2011-7”). In accordance with ASU
F-10
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
2011-7, the Company will be required to present its provision for doubtful accounts related to patient service revenue as a deduction from revenue, similar to contractual discounts. Accordingly, the Company’s revenues will be required to be reported net of both contractual discounts as well as its provision for doubtful accounts related to patient service revenues. Additionally, ASU 2011-7 will require the Company to make certain additional disclosures designed to help users understand how contractual discounts and bad debts affect recorded revenue in both interim and annual financial statements. ASU 2011-7 is required to be applied retrospectively and is effective for public companies for fiscal years beginning after December 15, 2011, and interim periods within those fiscal years. Early adoption is permitted. The adoption of ASU 2011-7 is not expected to impact the Company’s financial position, results of operations or cash flows although it will change the presentation of the Company’s revenues on its statements of earnings as well as requiring additional disclosures.
In June 2011, the FASB issued ASU 2011-5, “Comprehensive Income (Topic 220)—Presentation of Comprehensive Income” (“ASU 2011-5”). ASU 2011-5 eliminates the Company’s currently elected option to present components of other comprehensive income as part of the statement of changes in stockholders’ equity. Instead, ASU 2011-5 requires that all non-owner changes in stockholders’ equity be presented either in a single continuous statement of comprehensive income or in two separate but consecutive statements. ASU 2011-5 is required to be applied retrospectively and is effective for public companies for fiscal years beginning after December 15, 2011, and interim periods within those fiscal years. Early adoption is permitted. The Company anticipates applying the provisions of ASU 2011-5 for its fiscal year ending June 30, 2012. The adoption of ASU 2011-5 is not expected to impact the Company’s financial position, results of operations or cash flows prospectively.
Reclassifications—Certain prior year amounts have been reclassified in our consolidated financial statements to conform to current year classifications. These reclassifications include reclassifying net current assets and net current liabilities of our formerly owned Chilton Medical Center on the June 30, 2010 consolidated balance sheets and results of operations of our formerly owned Chilton Medical Center from continuing operations to discontinued operations in the consolidated statement of earnings for the fiscal years ended June 30, 2010 and 2009.
| 3. | DISCONTINUED OPERATIONS |
All of the businesses discussed below are reported as discontinued operations and the consolidated financial statements for all prior periods have been adjusted to reflect this presentation.
Chilton Medical Center—On March 1, 2011, SunLink entered into an agreement to lease its owned Chilton Medical Center (“Chilton”) and to sell its 83% membership interest in Clanton Hospital LLC (“Clanton”) subsidiary, which manages Chilton, to Carraway Medical Systems, Inc. (“Carraway”). The lease agreement is for a six-year term with monthly rent of $37 and includes an option under which Carraway can purchase Chilton from SunLink. The option purchase price is $3,700, less the amount paid to purchase the 17% membership interest of Clanton that Carraway does not currently own, up to a maximum of $615. The purchase price of SunLink’s 83% membership interest in Clanton was a $1,000 six-year zero-coupon note plus a six-year 6% note for the net working capital of Clanton at purchase. If the purchase option for Chilton is exercised during the six-year term of the lease, any amount paid under the $1,000 note will be credited to the option purchase price and any remaining balance on the note will be cancelled. As a result, the note at June 30, 2011 was recorded on the balance sheet at net $0. Pursuant to the terms of the sale and lease and agreement, SunLink is entitled to receive 75% of the Electronic Health Records Medicare incentive reimbursement received by Clanton.
Housewares Segment—All claims in a liquidation proceeding with respect to SunLink’s former Housewares segment were settled on April 13, 2010. In connection with the settlement of such claim SunLink paid approximately $1,400, of which $480 was covered under a directors and officers insurance policy. The
F-11
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
Company cancelled all preferred stock of its SunLink subsidiary held by the former Housewares segment subsidiary. The pre-tax loss of $464 for the fiscal year ended June 30, 2010 resulted from legal expenses incurred.
Mountainside Medical Center—On June 1, 2004, SunLink sold its Mountainside Medical Center (“Mountainside”) hospital in Jasper, Georgia, for approximately $40,000 pursuant to the terms of an asset sale agreement. In connection with this sale, claims by the buyer and counter claims by SunLink were litigated which resulted in a judgment for SunLink. The judgment, which included damages, prejudgment interest and certain losses, was collected by SunLink in the amount of $1,246 in May 2010 and $540 in December 2010, and the parties executed a mutual release. Included in the pre-tax earnings of Mountainside for the fiscal year ended June 30, 2011 is the judgment of $540 related to the litigation with the buyer claim and SunLink’s counterclaim. Also included in pre-tax earnings for the fiscal year ended June 30, 2011 were legal expenses of $194 related to the litigation with the buyer claim and SunLink’s counterclaim. Included in the pre-tax earnings of Mountainside for the fiscal year ended June 30, 2010 is the judgment of $1,829, composed of a total of a $1,560 payment plus $266 of accrued judgment interest. Also included in pre-tax earnings for the fiscal year ended June 30, 2010 were legal expenses related to the litigation with the buyer claim and SunLink’s counterclaim.
Life Sciences and Engineering Segment—SunLink retained a defined benefit retirement plan which covered substantially all of the employees of this segment when the segment was sold in fiscal 1998. Effective February 28, 1997, the plan was amended to freeze participant benefits and close the plan to new participants. Pension expense and related tax benefit or expense is reflected in the results of operations for this segment for the fiscal years ended June 30, 2011, 2010 and 2009.
Industrial Segment—In fiscal 1989, SunLink discontinued the operations of its industrial segment and subsequently disposed of substantially all related net assets. However, potential obligations remained relating to product liability claims for products sold prior to disposal. In the fiscal year ended June 30, 2009, the loss reserve of $161 for such claims was reversed by SunLink as it was determined no loss reserve was needed.
Discontinued Operations Reserves—Over the past 22 years SunLink has discontinued operations carried on by its former Chilton Medical Center, Mountainside Medical Center and its former industrial, U.K. leisure marine, life sciences and engineering, and European child safety segments, as well as the U.K. housewares segment. SunLink’s reserves related to discontinued operations of these segments represent management’s best estimate of SunLink’s possible liability for property, product liability and other claims for which SunLink may incur liability. With the settlement of litigation related to the Housewares Segment and Mountainside during fiscal year 2010, no reserve for discontinued operations is included in the June 30, 2011 and 2010 balance sheets.
The following is a summary of the loss reserves for discontinued operations:
| Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Beginning balance |
$ | — | $ | 643 | $ | 1,326 | ||||||
| Usage |
— | (643 | ) | (443 | ) | |||||||
| Exchange differences |
— | — | (240 | ) | ||||||||
|
|
|
|
|
|
|
|||||||
| $ | — | $ | — | $ | 643 | |||||||
|
|
|
|
|
|
|
|||||||
F-12
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
Results of discontinued operations were as follows:
Discontinued Operations—Summary Statement of Earnings Information
| Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Net Revenues: |
||||||||||||
| Chilton Medical Center |
$ | 9,447 | $ | 14,615 | $ | 16,493 | ||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from discontinued operations: |
||||||||||||
| Chilton Medical Center |
||||||||||||
| Earnings (loss) from operations |
$ | (724 | ) | $ | (134 | ) | $ | 525 | ||||
| Gain on sale |
438 | — | — | |||||||||
| Income tax expense (benefit) |
50 | (62 | ) | 263 | ||||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from Chilton Medical Center after taxes |
(336 | ) | (72 | ) | 262 | |||||||
|
|
|
|
|
|
|
|||||||
| Housewares Segment: |
||||||||||||
| Loss from operations |
— | (464 | ) | (241 | ) | |||||||
| Income tax benefit |
— | (64 | ) | (106 | ) | |||||||
|
|
|
|
|
|
|
|||||||
| Loss from Housewares Segment after taxes |
— | (400 | ) | (135 | ) | |||||||
|
|
|
|
|
|
|
|||||||
| Mountainside Medical Center |
||||||||||||
| Earnings (loss) from operations |
347 | 1,731 | (139 | ) | ||||||||
| Income tax expense (benefit) |
119 | 238 | (62 | ) | ||||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from Mountainside Medical Center after taxes |
228 | 1,493 | (77 | ) | ||||||||
|
|
|
|
|
|
|
|||||||
| Life sciences and engineering segment: |
||||||||||||
| Loss from operations |
(83 | ) | (71 | ) | (58 | ) | ||||||
| Income tax benefit |
(28 | ) | (10 | ) | (25 | ) | ||||||
|
|
|
|
|
|
|
|||||||
| Loss from life sciences and engineering segment after taxes |
(55 | ) | (61 | ) | (33 | ) | ||||||
|
|
|
|
|
|
|
|||||||
| Industrial segment: |
||||||||||||
| Earnings from operations |
— | — | 161 | |||||||||
| Income tax expense |
— | — | 71 | |||||||||
|
|
|
|
|
|
|
|||||||
| Earnings from industrial segment after taxes |
— | — | 90 | |||||||||
|
|
|
|
|
|
|
|||||||
| Earnings (loss) from discontinued operations |
$ | (163 | ) | $ | 960 | $ | 107 | |||||
|
|
|
|
|
|
|
|||||||
| 4. | NET RECEIVABLES |
SunLink has agreements with third-party payors that provide for payments at amounts different from its established rates. A summary of the payment arrangements with major third-party payors follows:
Medicare—Inpatient acute care services rendered to Medicare program beneficiaries are paid at prospectively determined rates per Diagnosis Related Group. These rates vary according to a patient classification system that is based on clinical, diagnostic, and other factors. Inpatient nonacute services, certain outpatient services, and defined capital and medical education costs related to Medicare beneficiaries are paid based on a cost reimbursement methodology. Cost reimbursable items are paid at a tentative rate, with final settlement determined after submission of annual cost reports and audits thereof by the Medicare fiscal intermediary.
F-13
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
Medicaid—Inpatient and outpatient services rendered to Medicaid program beneficiaries are reimbursed either under contracted rates or reimbursed for cost reimbursable items at a tentative rate, with final settlement determined after submission of annual cost reports and audits thereof by the Medicaid fiscal intermediary.
SunLink also has entered into payment agreements with certain commercial insurance carriers, health maintenance organizations, and preferred provider organizations. The basis for payment under these agreements includes prospectively determined rates per discharge, discounts from established charges, and prospectively determined daily rates.
Summary information for receivables is as follows:
| June 30, | ||||||||
| 2011 | 2010 | |||||||
| Patient accounts receivable (net of contractual allowance) |
$ | 28,619 | $ | 30,761 | ||||
| Less allowance for doubtful accounts |
(12,317 | ) | (14,725 | ) | ||||
|
|
|
|
|
|||||
| Patient accounts receivable (net of allowances) |
$ | 16,302 | $ | 16,036 | ||||
|
|
|
|
|
|||||
Net revenues included $766, $1,194, and $233, for the years ended June 30, 2011, 2010 and 2009, respectively, for the settlements and filings of prior year Medicare and Medicaid cost reports.
| 5. | MEDICAID ELECTRONIC HEALTH RECORDS INCENTIVE REIMBURSEMENT RECEIVABLE DEFERRED REVENUE—MEDICARE ELECTRONIC HEALTH RECORDS INCENTIVE REIMBURSEMENT |
Included in net revenues for the fiscal year ended June 30, 2011 is approximately $8,926 for electronic health records (“EHR”) incentive reimbursement. The Health Information Technology for Economic and Clinical Health Act (the “HITECH Act”) was enacted into law on February 17, 2009 as part of the American Recovery and Reinvestment Act of 2009 (“ARRA”). The HITECH Act includes provisions designed to increase the use of electronic health records by both physicians and hospitals. Beginning with federal fiscal year 2011 and extending through Federal fiscal year (“FFY”) 2016, eligible hospitals and critical access hospitals (“CAH”) participating in the Medicare and Medicaid programs are eligible for reimbursement incentives based on successfully demonstrating meaningful use of its certified EHR technology. Conversely, those hospitals that do not successfully demonstrate meaningful use of EHR technology are subject to reductions in reimbursements beginning in FFY 2015. On July 13, 2010, the Department of Health and Human Services (“DHHS”) released final meaningful use regulations. Meaningful use criteria are divided into three distinct stages: I, II and III. The final rules specify the initial criteria for: physicians, eligible hospitals, and CAHs necessary to qualify for incentive payments; calculation of the incentive payment amounts; payment adjustments under Medicare for covered professional services and inpatient hospital services; eligible hospitals and CAHs which fail to demonstrate meaningful use of certified EHR technology; and other program participation requirements.
The final rule set the earliest interim payment date for the incentive payment at May 2011. This was a delay from the initial October 2010 date: however, the first year of the Medicare portion of the program is defined as the Federal government fiscal year October 1, 2010 to September 30, 2011. The Medicaid portion of the program will be administered by the various state authorities based upon the criteria in the final rules.
Attestation of meaningful use requirements for the first year (October 1, 2010—September 30, 2011) began on April 18, 2011. Each of SunLink’s six hospitals and its formerly owned Chilton Medical Center registered for the program with the Centers for Medicare and Medicaid Services (“CMS”) and on April 18, 2011 all successfully attested compliance with Part I of the Medicare EHR incentive program for such first year.
F-14
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
As of June 30, 2011, SunLink has received $7,731 in EHR Medicare incentive reimbursement for the six hospitals for the fiscal year then ended and $790 for its formerly owned Chilton Medical Center. $405 of the Medicare EHR incentive reimbursement is recorded as deferred revenue of June 30, 2011 which will be recognized in the first quarter of the Company’s fiscal year 2012 to coincide with the 2011 Federal fiscal year. The Company also accrued Medicaid EHR reimbursement for Mississippi and Missouri in the amount of $1,102 collectively and $141 for its formerly owned Chilton Medical Center. No amount has been accrued for Georgia Medicaid EHR incentive payments since the reimbursement program has not yet been established by the state. The amounts accrued are the estimates of the incentive payments for the periods earned through June 30, 2011.
| 6. | INVENTORY |
Consisted of the following:
| June 30, | ||||||||
| 2011 | 2010 | |||||||
| Healthcare Facilities Segment Supplies Inventory |
$ | 2,467 | $ | 2,374 | ||||
| Specialty Pharamcy Segment Goods Held for Sale |
2,250 | 2,136 | ||||||
|
|
|
|
|
|||||
| $ | 4,717 | $ | 4,510 | |||||
|
|
|
|
|
|||||
| 7. | GOODWILL AND INTANGIBLE ASSETS |
SunLink has goodwill related to its Healthmont and Carmichael acquisitions. We have intangible assets related to these acquisitions, as well. We also have intangible assets related to three Healthcare Facilities Segment clinic purchases.
Goodwill consists of the following:
| June 30, | ||||||||
| 2011 | 2010 | |||||||
| Healthcare Facilities Segment |
$ | 2,515 | $ | 2,515 | ||||
| Specialty Pharamcy Segment |
461 | 6,509 | ||||||
|
|
|
|
|
|||||
| $ | 2,976 | $ | 9,024 | |||||
|
|
|
|
|
|||||
F-15
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
Intangible assets consist of the following, net of amortization:
| June 30, 2011 |
June 30, 2010 |
|||||||
| Healthcare Facilities Segment |
||||||||
| Certificates of Need |
$ | 630 | $ | 630 | ||||
| Noncompetition Agreements |
83 | 83 | ||||||
|
|
|
|
|
|||||
| 713 | 713 | |||||||
| Accumulated Amortization |
(280 | ) | (226 | ) | ||||
|
|
|
|
|
|||||
| 433 | 487 | |||||||
|
|
|
|
|
|||||
| Specialty Pharmacy Segment |
||||||||
| Trade Name |
2,000 | 5,400 | ||||||
| Customer Relationships |
1,089 | 6,400 | ||||||
| Medicare License |
769 | 769 | ||||||
|
|
|
|
|
|||||
| 3,858 | 12,569 | |||||||
| Accumulated Amortization |
(453 | ) | (1,280 | ) | ||||
|
|
|
|
|
|||||
| 3,405 | 11,289 | |||||||
|
|
|
|
|
|||||
| Total |
$ | 3,838 | $ | 11,776 | ||||
|
|
|
|
|
|||||
The trade name intangible asset under the Specialty Pharmacy Segment is a non-amortizing intangible asset.
Amortization expense was $646, $854, and $919, for the fiscal years ended June 30, 2011, 2010 and 2009, respectively.
Annual amortization of amortizing intangibles for the next five years and thereafter is as follows:
| 2012 |
$ | 182 | ||
| 2013 |
169 | |||
| 2014 |
169 | |||
| 2015 |
169 | |||
| 2016 |
169 | |||
| 2017 and thereafter |
980 | |||
|
|
|
|||
| Total |
$ | 1,838 | ||
|
|
|
Impairment testing—During the fourth quarter of fiscal 2011, we completed our annual impairment testing of goodwill and certain intangible assets. The analysis resulted in a goodwill impairment charge of $6,048 related to the Specialty Pharmacy Segment for fiscal 2011. Additionally, the Company recognized a $3,400 impairment charge to trade name and a $3,899 impairment charge to customer relationships for the fiscal year ended June 30, 2011 for the Specialty Pharmacy Segment. The decline in fair value of our Specialty Pharmacy Segment below its book value was is primarily the result of lower than expected revenue and customer growth relative to the assumptions made at the acquisition date.
F-16
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The following table summarized goodwill and intangible asset impairment charges for the fiscal year ended June 30, 2011:
| June 30, | ||||
| 2011 | ||||
| Specialty Pharmacy Segment |
||||
| Goodwill |
$ | 6,048 | ||
| Intangible assets |
||||
| Trade Name |
3,400 | |||
| Customer Relationships |
3,899 | |||
|
|
|
|||
| Total |
$ | 13,347 | ||
|
|
|
|||
| 8. | LONG-TERM DEBT |
Long-term debt consisted of the following:
| June 30, | ||||||||
| 2011 | 2010 | |||||||
| Term Loan |
$ | 29,086 | $ | 30,836 | ||||
| Capital lease obligations |
169 | 51 | ||||||
|
|
|
|
|
|||||
| Total |
29,255 | 30,887 | ||||||
| Less current maturities |
(1,814 | ) | (1,797 | ) | ||||
|
|
|
|
|
|||||
| $ | 27,441 | $ | 29,090 | |||||
|
|
|
|
|
|||||
SunLink Credit Facility—On April 23, 2008, SunLink entered into a $47,000 seven-year senior secured credit facility (“Credit Facility”) comprised of a revolving line of credit of up to $12,000 (the “Revolving Loan”) and a $35,000 term loan (the “Term Loan”). The Credit Facility has subsequently been amended by three modification agreements, on September 27, 2010 (“September 2010 Modification”), March 1, 2011 (“March 2011 Modification”) and July 28, 2011 (“July 2011 Modification”). The Revolving Loan commitment was reduced to $9,000 by the September 2010 Modification. At June 30, 2011, the Revolving Loan balance was $5,300 with an interest rate at LIBOR plus 10.5% (13.25% at June 30, 2011) and the Term Loan had an outstanding balance of $29,086 with an interest rate at LIBOR plus 12.07% (14.82% at June 30, 2011). In the Credit Facility, LIBOR is defined as the Thirty-Day published rate, not to be less than 2.75%, nor more than 5.50%. The maximum availability of the Revolving Loan is keyed to the calculated net collectible value of eligible accounts receivable. Under the terms of the July 2011 Modification, SunLink made an $8,000 prepayment of the Term Loan and paid a modification fee of $131. The source of the repayment was $2,500 of proceeds from a private placement of SunLink common shares primarily to directors and affiliates and $5,500 of operating funds. Under the July 2011 Modification, the interest rate under the Revolving Loan was adjusted to LIBOR plus 8.875%, or 11.625% at July 28, 2011 and the interest rate under the Term Loan was adjusted to LIBOR plus 10.82%, or 13.57% at July 28, 2011. The termination date of the Credit Facility was changed to January 1, 2013. The termination date had been changed to September 30, 2011 in the September 2010 modification. Financing costs and expenses related to the Credit Facility of $2,522 are being amortized over the modified life of the Facility. Accumulated amortization and amortization expense was approximately $2,322 and $1,485, respectively, as of and for the fiscal year ended June 30, 2011 and $438 and $378 as of and for the fiscal year ended June 30, 2010. The increased financing cost amortization in the fiscal year ended June 30, 2011 resulted from the change in the termination date of the Credit Facility from April 2015 to September 2011 in the September 2010 modification. The Credit Facility is secured by a first priority security interest in substantially all real and personal property of the Company and its consolidated domestic subsidiaries, including a pledge of all of the equity interests in such subsidiaries.
F-17
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The Credit Facility contains various terms and conditions, including operational and financial restrictions and limitations, and affirmative and negative covenants. The covenants include financial covenants measured on a quarterly basis which require SunLink to comply with maximum leverage and minimum fixed charge ratios, maximum capital expenditure amounts, collateral value to loan amount and liquidity and cash flow measures, all as defined in the Credit Facility. Although SunLink was not in compliance with certain of the financial covenants contained in the Credit Facility at June 30, 2011, the Credit Facility was subsequently amended by the July Modification to change the affected covenants so as to bring us into compliance. We believe that the Company should be able to continue in compliance with the revised levels of financial covenants and terms in the Credit Facility during the fiscal year ending June 30, 2012, but there is no assurance that the Company will be able to do so.
In the September 2010 Modification, the termination date of the Credit Facility was changed from April 22, 2015 to September 30, 2011 and it contained conditions for waivers of the non-compliance with financial covenants for the quarters ended September 30, 2010, December 31, 2011 and March 31, 2011. The September 2010 and March 2011 Modifications also included increases to the interest rate for the Revolving Loan to LIBOR plus 6.50% from the waiver date through November 14, 2010, LIBOR plus 7.50% from November 15, 2010 to February 15, 2011, LIBOR plus 8.50% from February 16, 2011 to April 14, 2011, LIBOR plus 9.50% from April 15, 2011 to May 15, 2011, LIBOR plus 10.50% from May 16, 2011 to July 15, 2011 and LIBOR plus 11.50% from July 16, 2011 through the July 28, 2011 closing date of the July 2011 Modification. They also increased the interest rate for the Term Loan to LIBOR plus 8.07% from the September 2010 Modification date through November 14, 2010, LIBOR plus 9.07% from November 15, 2010 to February 15, 2011, LIBOR plus 10.07% from February 16, 2011 to April 15, 2011, LIBOR plus 11.07% from April 15, 2011 to May 15, 2011, LIBOR plus 12.07% from May 16, 2011 to July 15, 2011 and LIBOR plus 13.07% from July 16, 2011 through the July 28, 2011 closing date of the July 2011 Modification. Under the July 2011 Modification, the interest rate under the Revolving Loan was adjusted to LIBOR plus 8.875%, or 11.625% at July 28, 2011 and the interest rate under the Term Loan was adjusted to LIBOR plus 10.82%, or 13.57%, at July 28, 2011. A waiver fee of 2% of the current Credit Facility commitment totaling approximately $788 was due at the September 2011 Modification closing and additional waiver fees of 0.5% of the total Credit Facility commitment were paid at November 15, 2010, February 15, 2011 and May 15, 2011. The July 28, 2011 Modification includes conditions related to a September 2011 and December 2011 Term Loan Reduction Covenant which may increase the interest rate for both the Term Loan and the Revolving Loan by an additional 0.5% over the prescribed interest rate for the remainder of the agreement. If the Term Loan Reduction Covenants are met, the interest rate for both the Term Loan and the Revolving Loan may decrease by an additional 1.25% over the prescribed interest rate for the remainder of the agreement. If we fail to remain in compliance with the Credit Facility as modified, we would cease to have a right to draw on the revolving line of credit facility and the lenders would, among other things, be entitled to call a default and demand repayment of the indebtedness outstanding. If SunLink or its applicable subsidiaries experience a material adverse change in their business, assets, financial condition, management or operations, or if the value of the collateral securing the Credit Facility decreases, we may be unable to draw on the credit facility.
Annual required payments of debt for the next two years are as follows:
| 2012 |
$ | 1,814 | ||
| 2013 |
27,409 | |||
| 2014 |
32 | |||
|
|
|
|||
| Total |
$ | 29,255 | ||
|
|
|
F-18
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The contractual commitments for interest on long-term debt are shown in the following table. The interest rate on variable interest debt is calculated at the interest rate at June 30, 2011 per the July 2011 Modificiation.
| 2012 |
$ | 3,079 | ||
| 2013 |
1,343 | |||
| 2014 |
1 | |||
|
|
|
|||
| Total |
$ | 4,423 | ||
|
|
|
| 9. | SUBORDINATED LONG-TERM DEBT |
Subordinated long-term debt consisted of the following:
| June 30, | ||||||||
| 2011 | 2010 | |||||||
| Carmichael |
$ | 2,497 | $ | 2,550 | ||||
| Less current maturities |
(300 | ) | (300 | ) | ||||
|
|
|
|
|
|||||
| $ | 2,197 | $ | 2,250 | |||||
|
|
|
|
|
|||||
Carmichael Note—On April 22, 2008, SunLink Scripts Rx, LLC entered into a $3,000 promissory note agreement with an interest rate of 8% (“Carmichael Note”) with the former owners of Carmichael as part of the acquisition purchase price. The note is payable in semi-annual installments of $150 beginning on April 22, 2009 with the remaining balance of $1,200 due April 22, 2015. Interest is payable in arrears semi-annually on the six-month anniversary of the issuance of the note. The note is guaranteed by SunLink Health Systems, Inc. for the payment of principal and accrued interest. The note is subordinate to the Credit Facility.
Under the terms of the Credit Facility (see Note 8), if SunLink is in violation of certain terms and conditions of this Facility, the Company cannot make principal payments of the Carmichael Loan without permission of the Credit Facility lender.
On April 12, 2011, an amendment to the Carmichael Note (“Carmichael Note Amendment”) was entered into under which SunLink has the option to issue subordinated promissory notes to the former owners of Carmichael in payment of up to two semi-annual payments of principal and interest due under the Carmichael Note. The notes will bear an interest rate of 8% and will be due on April 22, 2015. A note of $247 was issued on April 22, 2011 for the principal and interest payment that would have been due on April 22, 2011.
Annual required payments of debt for the next five years and thereafter are as follows:
| 2012 |
$ | 300 | ||
| 2013 |
300 | |||
| 2014 |
300 | |||
| 2015 |
1,597 | |||
|
|
|
|||
| Total |
$ | 2,497 | ||
|
|
|
F-19
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The contractual commitments for interest on the subordinated long-term debt are shown in the following table:
| 2012 |
$ | 188 | ||
| 2013 |
164 | |||
| 2014 |
140 | |||
| 2015 |
64 | |||
|
|
|
|||
| Total |
$ | 556 | ||
|
|
|
| 10. | SHAREHOLDERS’ EQUITY |
Employee and Directors Stock Option Plans—On November 7, 2005, the 2005 Equity Incentive Plan was approved by SunLink’s shareholders at the Annual Meeting of Shareholders. This Plan permits the grant of options to employees, non-employee directors and service providers of SunLink for the purchase of up to 800,000 common shares plus the number of unused shares under the 2001 Plans, which is 30,675, by November 2015. This Plan restricts the number of Incentive Stock Options to 700,000 shares and Restricted Stock Awards to 200,000 shares. The combination of Incentive Stock Options and Restricted Stock Awards cannot exceed 800,000 shares plus the number of unused shares under the 2001 Plans. Each award of Restricted Shares reduces the number of share options to be granted by four option shares for each Restricted Share awarded. No options have been exercised under this Plan. Options outstanding under this Plan were 115,999, 272,999 and 275,999 at June 30, 2011, 2010 and 2009, respectively.
On August 20, 2001, the 2001 Outside Directors’ Stock Ownership and Stock Option Plan was approved by SunLink’s shareholders at the Annual Meeting of Shareholders. This Plan permitted the grant of options to outside directors of SunLink for the purchase of up to 90,000 common shares through March 2006. Options for 90,000 shares were granted by March 2006. Options for 7,500 shares have been exercised under this plan. Options outstanding under this Plan were 45,000 at June 30, 2011 and 82,500 at June 30, 2010 and 2009, respectively. No additional awards may be granted under this Plan.
On February 28, 2001, the 2001 Long-Term Stock Option Plan was approved by the Board of Directors of SunLink. The 2001 Long-Term Stock Option Plan permitted the grant of options to officers and other key employees for the purchase of up to 810,000 common shares through February 2006. Options totaling 299,734 shares under this plan have been exercised. Options outstanding under this Plan were 13,250, 38,125, and 77,300 at June 30, 2011, 2010 and 2009, respectively. No additional awards may be granted under this Plan.
SunLink’s 1995 Incentive Stock Option Plan permitted the grant of options to officers and key employees to purchase up to 250,000 common shares through May 2005. Vesting and option expiration periods for options granted were determined by the Board of Directors but could not exceed 10 years. Options for 246,000 shares have been exercised and no options for shares were outstanding at June 30, 2011. 4,000 options for shares were outstanding at June 30, 2009. No additional awards may be granted under this Plan.
F-20
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The activity of Company’s share options is shown in the following table:
| Number of Shares |
Weighted- Average Exercise Price |
Range of Exercise Prices |
||||||||||
| Options outstanding July 1, 2008 |
1,190,980 | $ | 6.20 | $ | 1.50—$10.24 | |||||||
| Granted |
28,000 | 2.51 | 2.51 | |||||||||
| Exercised |
(118,450 | ) | 1.56 | 1.05—3.00 | ||||||||
| Forfeited |
(660,731 | ) | 7.74 | 1.50—10.24 | ||||||||
|
|
|
|||||||||||
| Options outstanding June 30, 2009 |
439,799 | 6.20 | 1.50—10.24 | |||||||||
| Granted |
— | — | — | |||||||||
| Exercised |
(29,050 | ) | 1.72 | 1.50—2.50 | ||||||||
| Forfeited |
(17,125 | ) | 3.41 | 2.51—5.48 | ||||||||
|
|
|
|||||||||||
| Options outstanding June 30, 2010 |
393,624 | 5.19 | 1.50—10.24 | |||||||||
| Granted |
— | — | — | |||||||||
| Exercised |
(40,500 | ) | 1.59 | 2.65—1.50 | ||||||||
| Forfeited |
(178,875 | ) | 5.41 | 2.50—5.86 | ||||||||
|
|
|
|||||||||||
| Options outstanding June 30, 2011 |
174,249 | $ | 5.80 | $ | 2.50—$9.63 | |||||||
|
|
|
|
|
|
|
|||||||
| Options exercisable June 30, 2009 |
353,799 | $ | 4.95 | $ | 1.50—$10.24 | |||||||
|
|
|
|
|
|
|
|||||||
| Options exercisable June 30, 2010 |
348,285 | $ | 5.26 | $ | 1.50—$9.63 | |||||||
|
|
|
|
|
|
|
|||||||
| Options exercisable June 30, 2011 |
168,909 | $ | 5.91 | $ | 2.50—$9.63 | |||||||
|
|
|
|
|
|
|
|||||||
The weighted-average fair value of each option granted during the year ended June 30, 2009 was $2.51. The fair value of each stock option grant was estimated using the Black-Scholes option pricing model with the following weighted-average assumptions used for grants during the year ended June 30, 2009: estimated volatility of 57%; risk-free interest rate of 2.75%; dividend yield of 0%; and an expected life of 6 years. The historical volatility is used to calculate the estimated volatility. The expected lives of the stock option grant was determined to be the midpoint between the vesting period and the contractual term of the grants. The estimate of the forfeited options in the compensation expense calculation was determined as the weighted-average forfeitures for the last three years. For the years ended June 30, 2011, 2010 and 2009, the Company recognized $6, $40 and $190, respectively, of compensation expense for share options issued. As of June 30, 2011, there was $4 of unrecognized compensation cost related to nonvested share-based compensation arrangements granted under the Plans. That cost is expected to be recognized during the fiscal year ended June 30, 2012.
In November 2008, SunLink approved an Executive Bonus Plan for 2009 (the “Bonus Plan”), which is a variable cash incentive program designed to reward executives of SunLink and its affiliates for successful achievement of certain short-term corporate goals and objectives. The Bonus Plan was offered to all of the Company’s executive officers and certain other employees. In order to participate in the Bonus Plan, each participant agreed to relinquish any and all stock options that such participant held that had an exercise price equal to or greater than $6.00 per share. During the fiscal year ended June 30, 2009, stock options totaling 601,106 shares were relinquished under the Plan.
F-21
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
Information with respect to stock options outstanding and exercisable at June 30, 2011 is as follows:
| Exercise Prices |
Number Outstanding |
Weighted-Average Remaining Contractual Life (in years) |
Number Exercisable | |||
| $ 2.50 |
6,250 | 0.99 | 6,250 | |||
| $ 2.51 |
16,000 | 7.23 | 10,660 | |||
| $ 2.65 |
6,000 | 0.69 | 6,000 | |||
| $ 2.90 |
37,500 | 2.45 | 37,500 | |||
| $ 2.91 |
7,500 | 0.15 | 7,500 | |||
| $ 3.00 |
1,000 | 0.15 | 1,000 | |||
| $ 6.55 |
33,000 | 5.88 | 33,000 | |||
| $ 8.00 |
33,999 | 6.24 | 33,999 | |||
| $ 9.63 |
33,000 | 4.37 | 33,000 | |||
|
|
| |||||
| 174,249 | 4.41 | 168,909 | ||||
|
|
|
The total intrinsic value of options exercised during the years ended June 30, 2011, 2010 and 2009 were $1, $16, and $72, respectively. As of June 30, 2011, the aggregate intrinsic value of options outstanding and options exercisable were $0 and $0, respectively. As of June 30, 2010, the aggregate intrinsic value of options outstanding and options exercisable were $29 and $29, respectively.
Shareholder Rights Plan—On February 8, 2004, the Board of Directors of the Company declared a dividend of one Series A Voting Preferred Purchase Price Right (a “Right”) for each outstanding common share of the Company to record owners of common shares at the close of business on February 10, 2004. Shares issued subsequent to such date are issued with a Right. The Board of Directors declared these Rights to protect shareholders from coercive or otherwise unfair takeover tactics. The Rights should not interfere with any merger or other business combinations approved by the Board of Directors. The Rights expire on February 8, 2014 unless the Company redeems them at an earlier date. The Company may redeem the Rights in whole, but not in part, at a price of $0.001 per Right, at any time prior to a public announcement that a person has become an Acquiring Person.
Accumulated Other Comprehensive Income (Loss)—Information with respect to the balances of each classification within accumulated other comprehensive income (loss) is as follows:
| Foreign Currency Translation Adjustment |
Minimum Pension Liability Adjustment |
Accumulated Other Comprehensive Income (Loss) |
||||||||||
| June 30, 2008 |
$ | (327 | ) | $ | (256 | ) | $ | (583 | ) | |||
| Current period change |
281 | (35 | ) | 246 | ||||||||
|
|
|
|
|
|
|
|||||||
| June 30, 2009 |
(46 | ) | (291 | ) | (337 | ) | ||||||
| Current period change |
46 | (10 | ) | 36 | ||||||||
|
|
|
|
|
|
|
|||||||
| June 30, 2010 |
— | (301 | ) | (301 | ) | |||||||
| Current period change |
— | 23 | 23 | |||||||||
|
|
|
|
|
|
|
|||||||
| June 30, 2011 |
$ | — | $ | (278 | ) | $ | (278 | ) | ||||
|
|
|
|
|
|
|
|||||||
F-22
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
| 11. | INCOME TAXES |
The provision (benefit) for income taxes on continuing operations are as follows:
| Year ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Domestic: |
||||||||||||
| Current |
$ | (1,034 | ) | $ | 750 | $ | 2,241 | |||||
| Deferred |
(4,515 | ) | (1,495 | ) | (1,428 | ) | ||||||
|
|
|
|
|
|
|
|||||||
| Total income tax (benefit) expense |
$ | (5,549 | ) | $ | (745 | ) | $ | 813 | ||||
|
|
|
|
|
|
|
|||||||
Net deferred tax assets recorded in the balance sheets are as follows:
| June 30, | ||||||||
| 2011 | 2010 | |||||||
| Net operating loss carryforward |
$ | 3,004 | $ | 2,541 | ||||
| Depreciation expense |
(3,954 | ) | (3,671 | ) | ||||
| Allowances for receivables |
3,727 | 4,588 | ||||||
| Accrued expenses |
2,904 | 2,455 | ||||||
| Intangible assets |
4,879 | (321 | ) | |||||
| Pension liabilities |
42 | 25 | ||||||
| Other |
(152 | ) | 138 | |||||
|
|
|
|
|
|||||
| 10,450 | 5,755 | |||||||
| Less valuation allowance |
(2,078 | ) | (1,350 | ) | ||||
|
|
|
|
|
|||||
| Net deferred tax assets |
$ | 8,372 | $ | 4,405 | ||||
|
|
|
|
|
|||||
The differences between income taxes at the Federal statutory rate and the effective tax rate were as follows:
| Year ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Income tax at Federal statutory rate |
$ | (5,443 | ) | $ | (535 | ) | $ | 491 | ||||
| Changes in valuation allowance—continuing operations |
588 | (86 | ) | (78 | ) | |||||||
| U.S. state income taxes, net of federal benefit |
(755 | ) | (342 | ) | 211 | |||||||
| Share option expense |
2 | 13 | 69 | |||||||||
| Other |
59 | 205 | 120 | |||||||||
|
|
|
|
|
|
|
|||||||
| Total income tax expense (benefit)—continuing operations |
$ | (5,549 | ) | $ | (745 | ) | $ | 813 | ||||
|
|
|
|
|
|
|
|||||||
The Company provided a $2,078 deferred tax valuation allowance as of June 30, 2011 so that the net deferred tax assets were $8,372 as of June 30, 2011. Based upon management’s assessment, the Company determined that it was more likely than not that a portion of its deferred tax asset would not be recovered. The increase in the valuation allowance during the fiscal year ending June 30, 2011 resulted from reserving for certain state net operating loss carryforwards that were not reserved for in prior periods. It is more likely than not that these net operating loss carryforwards will not be realized in future years. The Company provided a $1,350 deferred tax valuation allowance as of June 30, 2010 so that the net deferred tax assets were $4,405 as June 30, 2010. The net operating loss carryforwards expire in 2023.
F-23
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The Company accounts for uncertainty in income taxes for a change in judgment related to prior years’ tax positions in the quarter of such change. Activity in the unrecognized tax benefit liability account is as follows from July 1, 2008 through June 30, 2011:
| Balance at July 1, 2008 |
$ | 58 | ||
| Additions based on tax positions related to current year |
31 | |||
| Additions for tax positions of prior years |
— | |||
| Reductions for tax positions of prior years |
(23 | ) | ||
| Settlements |
— | |||
|
|
|
|||
| Balance at July 1, 2009 |
66 | |||
| Additions based on tax positions related to current year |
35 | |||
| Additions for tax positions of prior years |
— | |||
| Reductions for tax positions of prior years |
(30 | ) | ||
| Settlements |
— | |||
|
|
|
|||
| Balance at June 30, 2010 |
71 | |||
| Additions based on tax positions related to current year |
— | |||
| Additions for tax positions of prior years |
— | |||
| Reductions for tax positions of prior years |
(34 | ) | ||
| Settlements |
— | |||
|
|
|
|||
| Balance at June 30, 2011 |
$ | 37 | ||
|
|
|
| 12. | NONCONTROLLING INTEREST |
On July 1, 2009, SunLink sold 49% of its Specialty Pharmacy operations subsidiary in Ellijay, Georgia, to an unaffiliated buyer at a sales price $76. In December 2007, the FASB issued new guidance relating to accounting for noncontrolling interests in consolidated financial statements and requires that noncontrolling interests in subsidiaries be reported in the equity section of the controlling company’s balance sheet. The Company adopted this guidance on July 1, 2009.
| 13. | EMPLOYEE BENEFITS |
Defined Benefit Plans—No defined benefit plan is maintained for employees of either the Healthcare Facilities Segment or the Specialty Pharmacy Segment. Prior to SunLink’s acquisition of its initial hospitals, it historically maintained defined benefit retirement plans covering substantially all of its employees. Effective February 28, 1997, SunLink amended its domestic retirement plan to freeze participant benefits and close the plan to new participants. Benefits under the frozen plan are based on years of service and level of earnings. SunLink funds the frozen plan, which is noncontributory, at a rate that meets or exceeds the minimum amounts required by the Employee Retirement Income Security Act of 1974.
With the sale of SunLink’s life sciences and engineering segment businesses in the fiscal year ended March 31, 1999, net pension expense is now classified as an expense of discontinued operations. During the years ended June 30, 2011 and 2010, SunLink recognized curtailment losses of $0 and $0, respectively, for partial plan settlement of pension obligations to vested former employees.
At June 30, 2011, the plan’s assets are invested 76% in cash and short term investments, 13% in equity investments and 11% in fixed income investments. The plan’s current investment policy of primarily investing in cash and short term investments is in response to the poor returns on investment of the past 5 years in the equity markets, the returns available in the fixed income markets and the possible need for immediate liquidity as
F-24
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
participants retire or withdraw from the plan. The expected return on investment of 4.0% is based upon the plan’s historical return on assets. The plan expects to pay $55, $63, $60, $66, and $71 in pension benefits in the years ending June 30, 2012 though 2016, respectively. The plan expects to pay $372 in pension benefits for the years June 30, 2017 through 2021, in the aggregate. This assumes the plan participants elect to take monthly pension benefits as opposed to a lump sum payout when they reach age 65. The Company made no contributions to the plan for the year ended June 30, 2011.
The components of net pension expense for all plans (comprised solely of a domestic plan), excluding the curtailment losses above, were as follows:
| Years Ended June 30, | ||||||||||||
| 2011 | 2010 | 2009 | ||||||||||
| Service cost |
$ | — | $ | — | $ | — | ||||||
| Interest cost |
74 | 72 | 71 | |||||||||
| Expected return on assets |
(41 | ) | (45 | ) | (49 | ) | ||||||
| Amortization of prior service cost |
55 | 44 | 36 | |||||||||
|
|
|
|
|
|
|
|||||||
| Net pension expense |
$ | 88 | $ | 71 | $ | 58 | ||||||
|
|
|
|
|
|
|
|||||||
| Weighted-average assumptions: |
||||||||||||
| Discount rate |
6.50 | % | 6.50 | % | 6.50 | % | ||||||
| Expected return on plan assets |
4.00 | % | 4.00 | % | 4.00 | % | ||||||
| Rate of compensation increase |
0.00 | % | 0.00 | % | 0.00 | % | ||||||
Summary information for the plans (comprised solely of a domestic plan) is as follows:
| 2011 | 2010 | |||||||
| Change in Benefit Obligation |
||||||||
| Benefit obligation at beginning of year |
$ | 1,159 | $ | 1,136 | ||||
| Interest cost |
74 | 72 | ||||||
| Actuarial (gain) loss |
(13 | ) | 16 | |||||
| Benefits paid |
(63 | ) | (65 | ) | ||||
|
|
|
|
|
|||||
| Benefit obligation at end of year |
$ | 1,157 | $ | 1,159 | ||||
|
|
|
|
|
|||||
| Change in Plan Assets |
||||||||
| Fair value of plan asset at beginning of year |
$ | 1,093 | $ | 1,157 | ||||
| Actual return on plan assets |
15 | 1 | ||||||
| Benefits paid |
(63 | ) | (65 | ) | ||||
|
|
|
|
|
|||||
| Fair value of plan asset at end of year |
$ | 1,045 | $ | 1,093 | ||||
|
|
|
|
|
|||||
| Funded status of the plans |
(111 | ) | (65 | ) | ||||
| Unrecognized actuarial loss |
446 | 484 | ||||||
|
|
|
|
|
|||||
| Prepaid benefit cost |
$ | 335 | $ | 419 | ||||
|
|
|
|
|
|||||
| Amounts Recognized in Consolidated Balance Sheets |
||||||||
| Prepaid benefit cost |
(111 | ) | (65 | ) | ||||
| Accumulated other comprehensive income* |
446 | 484 | ||||||
|
|
|
|
|
|||||
| Net amount recognized |
$ | 335 | $ | 419 | ||||
|
|
|
|
|
|||||
| * | Accumulated other comprehensive income represents pretax minimum pension liability adjustments. |
F-25
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
Defined Contribution Plan—SunLink has a defined contribution plan pursuant to IRS Section 401(k) covering substantially all domestic employees. SunLink matches a specified percentage of the employee’s contribution as determined periodically by its management. No match was provided for the fiscal years ended June 30, 2011 and 2010. Plan expenses for the defined contribution plan were $0, $0, and $66, for the years ended June 30, 2011, 2010 and 2009, respectively.
| 14. | COMMITMENTS AND CONTINGENCIES |
Leases—The Company leases various land, buildings, and equipment under operating lease obligations having noncancelable terms ranging from one to 14 years. Rent expense was $3,172, $2,950, and $2,839, for the years ended June 30, 2011, 2010 and 2009, respectively. Minimum lease commitments as of June 30, 2011 are as follows:
| Fiscal year ending June 30: |
||||
| 2012 |
$ | 2,749 | ||
| 2013 |
1,249 | |||
| 2014 |
771 | |||
| 2015 |
594 | |||
| 2016 and therafter |
1,073 | |||
|
|
|
|||
| $ | 6,436 | |||
|
|
|
Lease Guarantee Obligation—In the 2004 Healthmont acquisition, SunLink assumed a lease guarantee obligation of $500 for a facility the Company did not occupy. During the fiscal year ended June 30, 2009, we learned that the guarantee had been extinguished through an agreement between the leasor and the current leasee of the property. As a result, SunLink reversed the recorded liability for the guarantee of $500.
Physician Guarantees—At June 30, 2011, SunLink had guarantee agreements with three physicians. A physician with whom a guarantee agreement is made generally agrees to maintain his or her practice within a hospital geographic area for a specific period (normally three years) or be liable to repay all or a portion of the guarantee received. The physician’s liability for any guarantee repayment due to non-compliance with the provisions of a guarantee agreement generally is collateralized by the physician’s patient accounts receivable and/or a promissory note from the physician. All potential payments payable under the three guarantees have been paid as of June 30, 2011. SunLink expensed $333, $596, and $750, for the fiscal years ended June 30, 2011, 2010 and 2009, respectively. There were no remaining non-cancelable commitments under guarantee agreements with physicians as of June 30, 2011.
Litigation—The Company is a party to claims and litigation incidental to its business, for which it is not currently possible to determine the ultimate liability, if any. Based on an evaluation of information currently available and consultation with legal counsel, management believes that resolution of such claims and litigation is not likely to have a material effect on the financial position, cash flows, or results of operations of the Company. The Company expenses legal costs as they are incurred.
On December 7, 2007, Southern Health Corporation of Ellijay, Inc. (“SHC-Ellijay”), a SunLink subsidiary, filed a Complaint against James P. Garrett and Roberta Mundy, both individually and as Fiduciary of the Estate of Randy Mundy (collectively, “Defendants”), seeking specific performance of an Option Agreement (the “Option Agreement”) dated April 17, 2007, between SHC-Ellijay, Mr. Garrett, and Ms. Mundy as Executrix of the Estate of Randy Mundy for the sale of approximately 24.74 acres of real property located in Gilmer County, Georgia, and recovery of SHC-Ellijay’s damages suffered as a result of Defendants’ failure to close the transaction in accordance with the Option Agreement. SHC-Ellijay also stated alternative claims for breach of the Option Agreement and fraud, along with claims to recover attorney’s fees and punitive damages.
F-26
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
In January 2008, Ms. Mundy and Mr. Garrett filed motions to strike, motions to dismiss, answers, affirmative defenses, and counterclaims against SHC-Ellijay. On March 3, 2009, SHC-Ellijay filed a First Amended and Restated Complaint for Damages, which effectively dropped the cause of action for specific performance of the Option Agreement. On May 7, 2009, Mr. Garrett and Ms. Mundy served a motion for summary judgment on all counts and causes of action stated in the First Amended Complaint, contending that Mr. Garrett and Ms. Mundy did not intentionally breach the Option Agreement. SHC-Ellijay filed opposition papers in June 2009 and requested a continuance. The court postponed consideration of the defendants’ motion for summary judgment and SHC-Ellijay’s response thereto until after a discovery dispute between the parties was resolved and SHC-Ellijay had an opportunity to move for summary judgment. That discovery dispute was resolved and, after another discovery dispute was resolved, the parties completed discovery. Subsequent to the end of the quarter, SHC-Ellijay filed a motion for partial summary judgment on Count I of the Amended Complaint, seeking a judgment holding that Defendants willfully and intentionally breached the Option Agreement in eight ways, which would entitle SHC-Ellijay to recover damages from Defendants.
In July 2011, SHC-Ellijay filed a reply brief in further support of its motion for partial summary judgment on the complaint and full summary judgment on the Defendants’ counterclaims and brief in opposition to Defendants’ cross motion for summary judgment. The summary judgment motions remain pending.
SunLink denies that it has any liability to Mr. Garrett and Ms. Mundy and intends to vigorously defend the claims asserted against SunLink by Mr. Garrett’s and Ms. Mundy’s counterclaims and to vigorously pursue its claims against Mr. Garrett and Ms. Mundy. While the ultimate outcome and materiality of the litigation cannot be determined, in management’s opinion the litigation will not have a material adverse effect on SunLink’s financial condition or results of operations.
SunLink is a party to claims and litigation incidental to its business, for which it is not currently possible to determine the ultimate liability, if any. Based on an evaluation of information currently available and consultation with legal counsel, management believes that resolution of such claims and litigation is not likely to have a material effect on the financial position, cash flows, or results of operations of the Company. The Company expenses legal costs as they are incurred.
| 15. | RELATED PARTIES |
A director of the Company and the Company’s secretary are members of two different law firms, each of which provides services to SunLink. We have paid an aggregate of $896, $596, and $585 to these law firms in the fiscal years ended June 30, 2011, 2010 and 2009, respectively.
| 16. | SUBSEQUENT EVENTS |
On July 28, 2011, SunLink announced the private placement of approximately 1,338,000 common shares at $1.90 per share with certain of its officers and directors and/or their affiliates. The net proceeds of the private placement of approximately $2,500 were used, together with the Company’s operating funds, to make an $8,000 pre-payment on the Credit Facility Term Loan. Concurrent with and conditioned upon the Term Loan pre-payment, the Company’s lenders modified the Credit Facility to reduce the interest rate, revise certain financial and other covenants and extend the maturity date of the Credit Facility until January 1, 2013. See Note 8 “Long-Term Debt”. A special committee of the Company’s Board of Directors comprised of disinterested directors evaluated the private placement transaction and obtained an opinion of an outside advisor selected by the special committee that the price and terms of the private placement were fair from a financial point of view to the Company.
F-27
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
The Company’s Board of Directors authorized the private placement before August 31, 2011 of a total of up to 3,800,000 of the Company’s common shares at a price equal to the average closing price for the prior ten trading days (on which the Company’s shares traded) with a minimum placement of $2,500.
| 17. | FINANCIAL INFORMATION BY SEGMENTS |
Under ASC Topic No. 280, Segment Reporting, operating segments are defined as components of an enterprise about which separate financial information is available that is evaluated regularly by the chief operating decision maker, or decision-making group, in deciding how to allocate resources and in assessing performance. Our chief operating decision-making group is composed of the chief executive officer and members of senior management. Our two reportable operating segments are Healthcare Facilities and Specialty Pharmacy.
We evaluate performance of our operating segments based on revenue and operating income (loss). Segment information for the fiscal years ended June 30, 2011 and 2010 is as follows:
| 2011 |
Healthcare Facilities |
Specialty Pharmacy |
Corporate
and Other |
Total | ||||||||||||
| Net Revenues from external customers |
$ | 141,241 | $ | 39,920 | $ | — | $ | 181,161 | ||||||||
| Operating profit (loss) |
11,298 | (14,463 | ) | (5,566 | ) | (8,731 | ) | |||||||||
| Depreciation and amortization |
4,209 | 1,562 | 460 | 6,231 | ||||||||||||
| Assets |
56,196 | 11,525 | 20,771 | 88,492 | ||||||||||||
| Expenditures for property, plant and equipment |
1,299 | 751 | 794 | 2,844 | ||||||||||||
| 2010 |
||||||||||||||||
| Net Revenues from external customers |
$ | 140,204 | $ | 42,962 | $ | — | $ | 183,166 | ||||||||
| Operating profit (loss) |
7,792 | (421 | ) | (5,517 | ) | 1,854 | ||||||||||
| Depreciation and amortization |
4,719 | 1,636 | 448 | 6,803 | ||||||||||||
| Assets |
60,419 | 25,195 | 12,876 | 98,490 | ||||||||||||
| Expenditures for property, plant and equipment |
1,634 | 718 | 150 | 2,502 | ||||||||||||
F-28
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
| 18. | EARNINGS PER SHARE |
| (Share | Amounts in Thousands) |
| Years Ended June 30, | ||||||||||||||||||||||||
| 2011 | 2010 | 2009 | ||||||||||||||||||||||
| Amount | Per Share Amount |
Amount | Per Share Amount |
Amount | Per Share Amount |
|||||||||||||||||||
| Earnings (loss) from continuing operations |
$ | (10,552 | ) | $ | (858 | ) | $ | 806 | ||||||||||||||||
|
|
|
|
|
|
|
|||||||||||||||||||
| Basic: |
||||||||||||||||||||||||
| Weighted-average shares outstanding |
8,094 | $ | (1.30 | ) | 8,052 | $ | (0.11 | ) | 7,975 | $ | 0.10 | |||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||
| Diluted: |
||||||||||||||||||||||||
| Weighted-average shares outstanding |
8,094 | $ | (1.30 | ) | 8,052 | $ | (0.11 | ) | 8,019 | $ | 0.10 | |||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||
| Earnings (loss) from discontinued operations |
$ | (163 | ) | $ | 960 | $ | 107 | |||||||||||||||||
|
|
|
|
|
|
|
|||||||||||||||||||
| Basic: |
||||||||||||||||||||||||
| Weighted-average shares outstanding |
8,094 | $ | (0.02 | ) | 8,052 | $ | 0.12 | 7,975 | $ | 0.01 | ||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||
| Diluted: |
||||||||||||||||||||||||
| Weighted-average shares outstanding |
8,094 | $ | (0.02 | ) | 8,052 | $ | 0.12 | 8,019 | $ | 0.01 | ||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||
| Net Earnings (loss) |
$ | (10,715 | ) | $ | 102 | $ | 913 | |||||||||||||||||
|
|
|
|
|
|
|
|||||||||||||||||||
| Basic: |
||||||||||||||||||||||||
| Weighted-average shares outstanding |
8,094 | $ | (1.32 | ) | 8,052 | $ | 0.01 | 7,975 | $ | 0.11 | ||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||
| Diluted: |
||||||||||||||||||||||||
| Weighted-average shares outstanding |
8,094 | $ | (1.32 | ) | 8,052 | $ | 0.01 | 8,019 | $ | 0.11 | ||||||||||||||
|
|
|
|
|
|
|
|
|
|
|
|
|
|||||||||||||
| Weighted-average number of shares outstanding—basic |
8,094 | 8,052 | 7,975 | |||||||||||||||||||||
|
|
|
|
|
|
|
|||||||||||||||||||
| Effect of dilutive director, employee and guarantor options and outstanding common share warrants |
— | — | 44 | |||||||||||||||||||||
|
|
|
|
|
|
|
|||||||||||||||||||
| Weighted-average number of shares outstanding—diluted |
8,094 | 8,052 | 8,019 | |||||||||||||||||||||
|
|
|
|
|
|
|
|||||||||||||||||||
Share options of 174, 321 and 388 for the years ended June 30, 2011, 2010 and 2009, respectively, are not included in the computation of diluted earnings per share because their effect would be antidilutive.
F-29
Index to Financial Statements
SUNLINK HEALTH SYSTEMS, INC.
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS—(Continued)
| 19. | SELECTED QUARTERLY FINANCIAL DATA (UNAUDITED) |
(Share Amounts in Thousands)
The following selected quarterly data for the years ended June 30, 2011 and 2010, respectively, are unaudited.
| Fourth Quarter |
Third Quarter |
Second Quarter |
First Quarter |
|||||||||||||||
| NET REVENUE |
Year Ended June 30, 2011 | $ | 43,214 | $ | 52,028 | $ | 45,053 | $ | 40,866 | |||||||||
| Year Ended June 30, 2010 | $ | 43,615 | $ | 48,462 | $ | 46,874 | $ | 44,215 | ||||||||||
| EARNINGS (LOSS) FROM |
||||||||||||||||||
| CONTINUING OPERATIONS |
Year Ended June 30, 2011 | (8,703 | ) | 2,513 | (2,100 | ) | (2,263 | ) | ||||||||||
| Year Ended June 30, 2010 | (1,549 | ) | 468 | (281 | ) | 504 | ||||||||||||
| NET EARNINGS (LOSS) |
Year Ended June 30, 2011 | (8,864 | ) | 2,682 | (1,766 | ) | (2,768 | ) | ||||||||||
| Year Ended June 30, 2010 | (1,516 | ) | 1,646 | (524 | ) | 496 | ||||||||||||
| EARNINGS (LOSS) PER SHARE: |
||||||||||||||||||
| Continuing operations |
||||||||||||||||||
| Basic |
Year Ended June 30, 2011 | (1.07 | ) | 0.31 | (0.26 | ) | (0.28 | ) | ||||||||||
| Year Ended June 30, 2010 | (0.19 | ) | 0.06 | (0.03 | ) | 0.06 | ||||||||||||
| Diluted |
Year Ended June 30, 2011 | (1.07 | ) | 0.31 | (0.26 | ) | (0.28 | ) | ||||||||||
| Year Ended June 30, 2010 | (0.19 | ) | 0.06 | (0.03 | ) | 0.06 | ||||||||||||
| NET EARNINGS (LOSS): |
||||||||||||||||||
| Basic |
Year Ended June 30, 2011 | (1.09 | ) | 0.33 | (0.22 | ) | (0.34 | ) | ||||||||||
| Year Ended June 30, 2010 | (0.19 | ) | 0.20 | (0.07 | ) | 0.06 | ||||||||||||
| Diluted |
Year Ended June 30, 2011 | (1.09 | ) | 0.33 | (0.22 | ) | (0.34 | ) | ||||||||||
| Year Ended June 30, 2010 | (0.19 | ) | 0.20 | (0.07 | ) | 0.06 | ||||||||||||
| WEIGHTED-AVERAGE COMMON SHARES OUTSTANDING: |
||||||||||||||||||
| Basic |
Year Ended June 30, 2011 | 8,119 | 8,095 | 8,082 | 8,081 | |||||||||||||
| Year Ended June 30, 2010 | 8,058 | 8,057 | 8,050 | 8,050 | ||||||||||||||
| Diluted |
Year Ended June 30, 2011 | 8,119 | 8,097 | 8,082 | 8,081 | |||||||||||||
| Year Ended June 30, 2010 | 8,058 | 8,069 | 8,050 | 8,070 | ||||||||||||||
F-30
