Attached files
| file | filename |
|---|---|
| 8-K - 8-K - Innoviva, Inc. | a10-10395_28k.htm |
Exhibit 99.1
|
289 |
Vilanterol trifenatate (VI; GW642444M), a novel inhaled long-acting beta2 adrenoceptor agonist (LABA), at single doses of 25, 50 and 100mcg, is well tolerated and demonstrates prolonged bronchodilation in asthmatic patients |
|
|
Kempsford RD, Norris V, Siederer SK |
GlaxoSmithKline R&D, Stockley Park, Middlesex, UB11 1BT, United Kingdom |
ABSTRACT
Rationale: GW642444 is a novel inhaled LABA with inherent 24 hour activity in vitro in development for once-daily administration as monotherapy (for COPD) and in combination with an inhaled corticosteroid (for both COPD and asthma). This study was conducted to determine the safety, tolerability, pharmacokinetics and duration of action (FEV1 over 24h) of single doses of GW642444 in asthma patients.
Methods: This was a double-blind, placebo-controlled, crossover study. Male (n=22) mild to moderate persistent asthma patients (mean (range) age 37 years (21–60), forced expiratory volume in 1 second (FEV1) % predicted 78.6% (60.2–104.3) and FEV1 reversibility 18.5% (11.7–34.1)) received single inhaled doses of GW642444 (25, 50 and 100mcg) or placebo. Adverse events (AEs), vital signs, ECG (12-lead ECG and Holter monitoring), FEV1 and GW642444 plasma pharmacokinetics (AUC, Cmax and Tmax) were determined up to 24h after dosing.
Results: GW642444 (25–100mcg) was well tolerated in asthma patients. The incidence and severity of AEs was comparable to placebo. There were no serious AEs. One patient was withdrawn after 25mcg GW642444 (elevated heart rate associated with an upper respiratory tract infection) and one after placebo (asymptomatic ventricular tachycardia). Following GW642444 administration there were no clinically significant abnormalities in vital signs, 12-lead ECG, QTc, Holter ECG, blood glucose or potassium. All GW642444 doses produced increases in FEV1 from as early as 5min after dosing (up to 288mL vs placebo; 95% CI: 196, 380) which were maintained up to 24h post-dose. At 23–24h after dosing with GW642444 25, 50 and 100mcg mean FEV1 (difference from placebo (95% CI)) values were 273mL (178, 369), 242mL (156, 328) and 321mL (233, 410), respectively indicating a 24h duration of action. GW642444 was rapidly absorbed into plasma (median Tmax at 10min) with systemic exposure increasing in an approximately dose proportional manner across the GW642444 dose range (25–100mcg).
Conclusions: Single doses of inhaled GW642444 (25–100mcg) were well tolerated in patients with mild to moderate persistent asthma with no clinically significant unwanted systemic effects. GW642444 produced a rapid and prolonged bronchodilation over 24h suggesting the potential for once daily administration in asthma.
INTRODUCTION
· Vilanterol trifenatate (VI; GW642444M) is an inhaled long-acting beta2 agonist (LABA) with inherent 24h activity in vitro which is in development for once-daily administration as monotherapy (for COPD) and in combination with the inhaled corticosteroid fluticasone furoate (for both COPD and asthma).
· This study was conducted to determine the safety, tolerability, pharmacokinetics and duration of action (FEV1 over 24h) of single doses of VI in asthma patients.
OBJECTIVES
Primary
· To evaluate the safety and tolerability of single inhaled doses of VI (25, 50 and 100mcg) in patients with persistent asthma.
Secondary
· To determine the rate of onset, duration and extent of bronchodilation of single inhaled doses of VI (25, 50 and 100mcg) in patients with persistent asthma.
· To evaluate the extra-pulmonary pharmacodynamic effects of single inhaled doses of VI (25, 50 and 100mcg) in patients with persistent asthma.
· To evaluate the systemic pharmacokinetics of single inhaled doses of VI (25, 50 and 100mcg) in patients with persistent asthma.
METHODS
· This was a randomized, double-blind, placebo-controlled, crossover study.
· Male, currently non-smoking patients with clinically stable (within 4 weeks of screening) mild to moderate persistent asthma, a screening pre-bronchodilator FEV1 >60% predicted(1), able to demonstrate reversibility to 400mcg albuterol (salbutamol) (FEV1 increase of >12% and >200mL over baseline) and receiving 200–500mcg/day fluticasone propionate or equivalent.
· LABAs, tiotropium and oral leukotriene inhibitors were prohibited from 1 week before screening until follow-up. Inhaled albuterol could be used during the study but had to be withheld for at least 6h before screening and before each dose of study drug.
· Each patient received single inhaled doses of VI (25, 50 and 100mcg) and placebo as a dry powder from a DISKUS™ device (AM dosing) on separate occasions 7–14 days apart.
· FEV1, heart rate (HR), 12-lead ECG (QTc(F) interval), plasma vilanterol concentrations and whole blood potassium and glucose were measured pre-dose and at intervals up to 24h after dosing.
· Adverse events (AEs) were recorded, pre- and post-dose laboratory safety screens were performed and cardiac Holter ECG monitoring was conducted for 24h after each dose.
RESULTS
Demographics
· Patient demographics are given in Table 1. Twenty-two male patients with persistent asthma participated in the study with 21, 21, 19 and 20 patients receiving placebo and 25, 50 and 100mcg VI, respectively.
Table 1. Demographic details
|
Age, years mean (range) |
36.9 (21–60) |
|
Sex, n (%) male: |
22 (100) |
|
Body mass index in kg/m2, mean (range) |
25.05 (19.3–29.7) |
|
Height in cm, mean (range) |
178.6 (166–191) |
|
Weight in kg, mean (range) |
79.9 (60.4–96.2) |
|
FEV1 % predicted, mean (range) |
78.6 (60.2–104.3) |
|
FEV1 % reversibility, mean (range) |
18.5 (11.7–34.1) |
Safety and tolerability
· Single doses of VI (25–100mcg) were well tolerated in patients with persistent asthma.
· Two patients were withdrawn prematurely. One patient experienced asymptomatic ventricular tachycardia (recorded in the Holter ECG) 24h after receiving placebo. A further patient experienced an increased HR 6–12h after receiving 25mcg VI. The increase just exceeded protocol-defined stopping criteria (115bpm and/or and increase of 40bpm) and the patient was withdrawn. The increase in HR had a temporal relationship with the development of an URT infection and was considered by the Investigator to be unrelated to the study drug.
· A summary of the most frequently reported AEs is given in Table 2. These were all of mild or moderate intensity. The most frequently reported AE was headache which was reported with a similar incidence after placebo and VI. There were no reports of tremor.
· Following VI administration there were no clinically significant abnormalities in vital signs, 12-lead ECG, QTcF, Holter ECG, blood glucose or potassium.
Table 2. Most frequently reported adverse events (reported by more than one patient)
|
|
|
|
|
VI dose |
|
||||
|
|
|
Placebo |
|
25mcg |
|
50mcg |
|
100mcg |
|
|
|
|
(N=21) |
|
(N=21) |
|
(N=19) |
|
(N=20) |
|
|
Adverse event |
|
N (%) |
|
N (%) |
|
N (%) |
|
N (%) |
|
|
Any event |
|
9 (43) |
|
12 (57) |
|
3 (16) |
|
6 (30) |
|
|
Headache |
|
3 (14) |
|
4 (19) |
|
1 (5) |
|
3 (15) |
|
|
Chest discomfort |
|
1 (5) |
|
0 |
|
0 |
|
1 (5) |
|
|
Application site rash |
|
0 |
|
1 (5) |
|
0 |
|
1 (5) |
|
|
Cough |
|
1 (5) |
|
1 (5) |
|
0 |
|
0 |
|
|
Urinary tract infection |
|
1 (5) |
|
1 (5) |
|
0 |
|
0 |
|
|
Ventricular extrasystoles |
|
1 (5) |
|
1 (5) |
|
0 |
|
0 |
|
|
Nasopharyngitis |
|
1 (5) |
|
0 |
|
0 |
|
0 |
|
|
Nausea |
|
0 |
|
1 (5) |
|
1 (5) |
|
0 |
|
Systemic pharmacodynamics
· All VI doses produced increases in FEV1 from as early as 5min after dosing which were maintained up to 24h post dose (Table 3; Figure 1).
· There were no significant effects on HR, QTc(F), blood potassium or glucose at VI doses up to 50mcg. Small but statistically significant effects on HR and QTc(F) were seen at the 100mcg VI dose (Table 4).
Table 3. FEV1 (mL) difference from placebo at 5 min and 23–24h following single dose VI (25–100mcg) in asthma patients
|
|
|
|
|
Difference |
|
95% |
|
|
|
|
|
|
(mL) in |
|
confidence |
|
|
|
|
Time post |
|
adjusted |
|
interval of |
|
|
Comparison |
|
dose |
|
means (SE) |
|
means |
|
|
25mcg–placebo |
|
5 min |
|
216 (46) |
|
124, 308 |
|
|
50mcg–placebo |
|
5 min |
|
210 (47) |
|
117, 303 |
|
|
100mcg–placebo |
|
5 min |
|
288 (46) |
|
196, 380 |
|
|
25mcg–placebo |
|
23–24h |
|
273 (48) |
|
178, 369 |
|
|
50mcg–placebo |
|
23–24h |
|
242 (43) |
|
156, 328 |
|
|
100mcg–placebo |
|
23–24h |
|
321 (46) |
|
233, 410 |
|
Figure 1. Mean FEV1 profile (0–24h) following single dose VI (25, 50 and 100mcg) and placebo in asthma patients
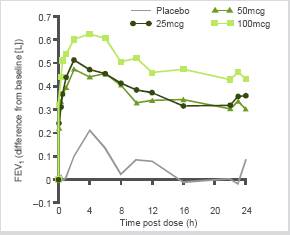
Pharmacokinetics
· Vilanterol was rapidly absorbed into plasma; median Tmax was achieved 10min post-dose (Table 5).
· Plasma vilanterol concentrations rapidly declined from peak and were generally below limits of quantification (30pg/mL) beyond 4h post-inhalation (Figure 2). At the lowest dose to produce bronchodilation (25mcg), systemic exposure was generally non-quantifiable beyond 1h post-dose (Table 5, Figure 2).
· Approximately dose proportional increases in systemic exposure were observed as VI dose was escalated from 25 to 100mcg (Table 5, Figure 2).
· Systemic exposure was consistent with that reported in COPD patients(2).
Table 4. Summary of extra-pulmonary pharmacodynamic data following single dose VI (25–100mcg) in asthma patients
|
|
|
|
|
|
|
95% |
|
|
|
|
|
|
Difference |
|
Confidence |
|
|
|
|
Comparison |
|
in adjusted |
|
interval of |
|
|
Parameter |
|
(test–ref) |
|
means (SE) |
|
Means |
|
|
Maximum heart rate (0–4h) (bpm) |
|
25mcg–placebo |
|
–3.2 (2.0) |
|
–7.2, 0.8 |
|
|
|
|
50mcg–placebo |
|
2.1 (1.9) |
|
–1.6, 5.8 |
|
|
|
|
100mcg–placebo |
|
5.1 (1.9) |
|
1.3, 8.9 |
|
|
|
|
|
|
|
|
|
|
|
Maximum QTc(F) (0–4h) (msec) |
|
25mcg–placebo |
|
2.3 (2.6) |
|
–3.0, 7.6 |
|
|
|
|
50mcg–placebo |
|
4.3 (2.4) |
|
–0.5, 9.0 |
|
|
|
|
100mcg–placebo |
|
9.8 (2.5) |
|
4.8, 14.7 |
|
|
|
|
|
|
|
|
|
|
|
Minimum potassium (0–4h) (mmol/L) |
|
25mcg–placebo |
|
0.1 (0.1) |
|
–0.1, 0.2 |
|
|
|
|
50mcg–placebo |
|
–0.1 (0.1) |
|
–0.3, 0.1 |
|
|
|
|
100mcg–placebo |
|
0.0 (0.1) |
|
–0.2, 0.2 |
|
|
|
|
|
|
|
|
|
|
|
Maximum glucose (0–4h) (mmol/L) |
|
25mcg–placebo |
|
0.0 (0.1) |
|
–0.3, 0.2 |
|
|
|
|
50mcg–placebo |
|
0.3 (0.1) |
|
0.0, 0.5 |
|
|
|
|
100mcg–placebo |
|
0.1 (0.1) |
|
–0.2, 0.3 |
|
Table 5. Summary of vilanterol pharmacokinetic parameters in asthma patients
|
VI |
|
|
|
|
|
|
|
|
|
|
|
|
Dose |
|
|
|
Cmax |
|
Tmax |
|
AUC (0–t) |
|
Tlast |
|
|
(mcg) |
|
N (n) |
|
(pg/mL)(a) |
|
(h)(b) |
|
(pg.h/mL)(a) |
|
(h)(b) |
|
|
25 |
|
21 (19) |
|
95.4 |
|
0.17 |
|
70.5 |
|
1.00 |
|
|
|
|
|
|
(114) |
|
(0.1–1.0) |
|
(72.8)(c) |
|
(0.2–4.1) |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
50 |
|
19 (19) |
|
204.8 |
|
0.17 |
|
143.3 |
|
2.00 |
|
|
|
|
|
|
(43.1) |
|
(0.1–0.3) |
|
(51.3) |
|
(0.7–4.1) |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
100 |
|
20 (20) |
|
344.6 |
|
0.17 |
|
440.7 |
|
4.05 |
|
|
|
|
|
|
(78.9) |
|
(0.1–1.1) |
|
(127.4) |
|
(0.8–24.2) |
|
N: represents the number of patients in the pharmacokinetic concentration population
n: represented the number of patients in the pharmacokinetic parameter population
(a)Geometric mean (CV%)
(b)Median (range)
(c)n=17
Figure 2. Median vilanterol plasma concentrations following single dose VI (25, 50 and 100mcg) in asthma patients
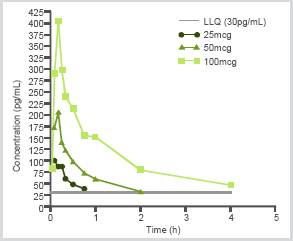
CONCLUSIONS
· Single doses of inhaled vilanterol trifenatate (25–100mcg) were well tolerated in patients with mild to moderate persistent asthma with no clinically significant unwanted systemic effects.
· Vilanterol trifenatate (25–100mcg) produced a rapid and prolonged bronchodilation over 24h suggesting the potential for once-daily administration in asthma.
REFERENCES
(1) Global Initiative for Asthma (GINA). Canada 2006. http://ginasthma.org.
(2) Kempsford RD, et al. Presented at ATS International Conference, New Orleans, May 14–19, 2010. Abstract 4977.
ACKNOWLEDGEMENTS
· This study was sponsored by GlaxoSmithKline (ClinicalTrials.gov: NCT00463697; protocol number B2C106996).
· Editorial support was provided by Geoffrey Weller and David Cutler at Gardiner-Caldwell Communications Ltd and was funded by GlaxoSmithKline.
· The study was conducted in the UK by MEU (Manchester), Parexel (Harrow) and Quintiles GDRU (London).
|
|
Presented at the Annual Conference of the American Thoracic Society (ATS), New Orleans, LA, USA, 14–19 May 2010 |
