Attached files
| file | filename |
|---|---|
| EX-23 - CONSENT - CENTENE CORP | exhibit23.htm |
| EX-21 - LIST OF SUBSIDIARIES - CENTENE CORP | exhibit21.htm |
| EX-12.1 - RATIO OF EARNINGS TO FIXED CHARGES - CENTENE CORP | exhibit121.htm |
| EX-31.1 - CERTIFICATION - CENTENE CORP | exhibit311.htm |
| EX-32.2 - CERTIFICATION - CENTENE CORP | exhibit322.htm |
| EX-32.1 - CERTIFICATION - CENTENE CORP | exhibit321.htm |
| EX-31.2 - CERTIFICATION - CENTENE CORP | exhibit312.htm |
| EX-10.10 - DEFERRED COMPENSATION PLAN - CENTENE CORP | exhibit1010.htm |
| EX-10.1E - CONTRACT AMENDMENT - CENTENE CORP | exhibit101e.htm |
UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
Washington, D.C. 20549
Form 10-K
(Mark One)
|
T |
ANNUAL REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the fiscal year ended December 31, 2009
or
|
£ |
TRANSITION REPORT PURSUANT TO SECTION 13 OR 15(d) OF THE SECURITIES EXCHANGE ACT OF 1934 |
For the transition period from to
Commission file number: 001-31826
Centene Corporation
(Exact name of registrant as specified in its charter)
|
Delaware |
42-1406317 | |
|
(State or other jurisdiction of
incorporation or organization) |
(I.R.S. Employer
Identification Number) | |
|
7711 Carondelet Avenue |
||
|
St. Louis, Missouri |
63105 | |
|
(Address of principal executive offices) |
(Zip Code) |
Registrant’s telephone number, including area code: (314) 725-4477
Securities registered pursuant to Section 12(b) of the Act:
|
Common Stock, $0.001 Par Value |
New York Stock Exchange | |
|
Title of Each Class |
Name of Each Exchange on Which Registered |
Securities registered pursuant to Section 12(g) of the Act:
None
(Title of Each Class)
Indicate by check mark if the registrant is a well-known seasoned issuer, as defined in Rule 405 of the Securities Act. Yes T No £
Indicate by check mark if the registrant is not required to file reports pursuant to Section 13 or Section 15(d) of the Act. Yes £ No T
Indicate by check mark whether the registrant (1) has filed all reports required to be filed by Section 13 or 15(d) of the Securities Exchange Act of 1934 during the preceding 12 months (or for such shorter period that the registrant was required to file such reports), and (2) has been subject to such filing requirements for the past 90 days. Yes T No £
Indicate by check mark whether the registrant has submitted electronically and posted on its corporate Web site every Interactive Data File required to be submitted and posted pursuant to Rule 405 of Regulation S-T during the preceding 12 months (or for such shorter period that the registrant was require to submit and post such files. Yes No
Indicate by check mark if disclosure of delinquent filers pursuant to Item 405 of Regulation S-K is not contained herein, and will not be contained, to the best of registrant’s knowledge, in definitive proxy or information statements incorporated by reference in Part III of this Form 10-K or any amendment to this Form 10-K. T
Indicate by check mark whether the registrant is a large accelerated filer, an accelerated filer, a non-accelerated filer, or a smaller reporting company. See the definitions of “large accelerated filer”, “accelerated filer” and “small reporting company” in Rule 12b-2 of the Exchange Act. Large
accelerated filer T Accelerated filer £ Non-accelerated filer £ (do not check if a smaller reporting company) Smaller reporting company £
Indicate by check mark whether the registrant is a shell company (as defined in Rule 12b-2 of the Act). Yes £ No T
The aggregate market value of the voting and non-voting common equity held by non-affiliates of the registrant, based upon the last reported sale price of the common stock on the New York Stock Exchange on June 30, 2009, was $843.5 million.
As of February 5, 2010, the registrant had 51,372,683 shares of common stock outstanding.
DOCUMENTS INCORPORATED BY REFERENCE
Portions of the Proxy Statement for the registrant’s 2010 annual meeting of stockholders are incorporated by reference in Part III, Items 10, 11, 12, 13 and 14.
|
Part I | ||||
|
Item 1. |
|
|
2 | |
|
Item 1A. |
12 | |||
|
Item 1B. |
18 | |||
|
Item 2. |
|
|
18 | |
|
Item 3. |
|
|
18 | |
|
Item 4. |
18 | |||
|
Part II | ||||
|
Item 5. |
|
|
19 | |
|
Item 6. |
|
|
20 | |
|
Item 7. |
|
|
21 | |
|
Item 7A. |
|
|
29 | |
|
Item 8. |
|
|
30 | |
|
Item 9. |
|
|
51 | |
|
Item 9A. |
|
|
51 | |
|
Item 9B. |
|
|
53 | |
|
Part III | ||||
|
Item 10. |
|
|
53 | |
|
Item 11. |
|
|
53 | |
|
Item 12. |
|
|
53 | |
|
Item 13 |
|
|
53 | |
|
Item 14. |
|
|
53 | |
|
Part IV | ||||
|
Item 15. |
|
|
54 | |
|
|
56 | |||
CAUTIONARY STATEMENT ON FORWARD-LOOKING STATEMENTS
All statements, other than statements of current or historical fact, contained in this filing are forward-looking statements. We have attempted to identify these statements by terminology including “believe,” “anticipate,” “plan,” “expect,” “estimate,” “intend,”
“seek,” “target,” “goal,” “may,” “will,” “should,” “can,” “continue” and other similar words or expressions in connection with, among other things, any discussion of future operating or financial performance. In particular, these statements include statements about our market opportunity, our growth strategy, competition, expected activities and future acquisitions, investments and the adequacy of our available
cash resources. These statements may be found in the various sections of this filing, including those entitled “Management’s Discussion and Analysis of Financial Condition and Results of Operations,” Part I, Item 1A. “Risk Factors,” and Part I, Item 3 “Legal Proceedings.” Readers are cautioned that matters subject to forward-looking statements involve known and unknown risks and uncertainties, including economic, regulatory, competitive
and other factors that may cause our or our industry’s actual results, levels of activity, performance or achievements to be materially different from any future results, levels of activity, performance or achievements expressed or implied by these forward-looking statements. These statements are not guarantees of future performance and are subject to risks, uncertainties and assumptions.
All forward-looking statements included in this filing are based on information available to us on the date of this filing. Actual results may differ from projections or estimates due to a variety of important factors, including:
|
· |
our ability to accurately predict and effectively manage health benefits and other operating expenses; |
|
· |
competition; |
|
· |
changes in healthcare practices; |
|
· |
changes in federal or state laws or regulations; |
|
· |
inflation; |
|
· |
provider contract changes; |
|
· |
new technologies; |
|
· |
reduction in provider payments by governmental payors; |
|
· |
major epidemics; |
|
· |
disasters and numerous other factors affecting the delivery and cost of healthcare; |
|
· |
the expiration, cancellation or suspension of our Medicaid managed care contracts by state governments; |
|
· |
availability of debt and equity financing, on terms that are favorable to us; and |
|
· |
general economic and market conditions. |
Item 1A “Risk Factors” of Part I of this filing contains a further discussion of these and other important factors that could cause actual results to differ from expectations. We disclaim any current intention or obligation to update or revise any forward-looking statements, whether as a result of new information, future
events or otherwise. Due to these important factors and risks, we cannot give assurances with respect to our future premium levels or our ability to control our future medical costs.
PART I
OVERVIEW
We are a multi-line healthcare enterprise operating in two segments: Medicaid Managed Care and Specialty Services. Our Medicaid Managed Care segment provides Medicaid and Medicaid-related health plan coverage to individuals through government subsidized programs, including Medicaid, the State Children’s Health Insurance Program,
or CHIP, Foster Care, Medicare Special Needs Plans and the Supplemental Security Income Program, also known as the Aged, Blind or Disabled Program, or collectively ABD. Our health plans in Florida, Georgia, Indiana, Ohio, South Carolina, Texas and Wisconsin are included in the Medicaid Managed Care segment. As of December 31, 2009, Medicaid accounted for 74% of our at-risk membership, while CHIP (also including Foster Care) and ABD (also including Medicare) accounted for 18% and 6%, respectively. Other
state programs in Massachusetts represent the remaining 2% at-risk membership. Our Specialty Services segment provides specialty services, including behavioral health, individual health insurance, life and health management, long-term care programs, managed vision, telehealth services, and pharmacy benefits management to state programs, healthcare organizations, employer groups and other commercial organizations, as well as to our own subsidiaries. Our health plans in Arizona, which is operated
by our long-term care company, and Massachusetts, which is operated by our individual health insurance provider, are included in the Specialty Services segment. Our Specialty Services segment also provides a full range of healthcare solutions for the rising number of uninsured Americans.
We expect to complete the sale of certain assets of University Health Plans, Inc., or UHP, our New Jersey health plan, during the first quarter of 2010. This sale is discussed in detail under the caption “Discontinued Operations” under “Item 7. Management’s Discussion and Analysis of Financial Condition
and Results of Operations.” Accordingly, our New Jersey health plan operations are reported as discontinued operations for all periods presented in our consolidated financial statements. The following discussion and analysis is presented primarily in the context of continuing operations unless otherwise identified.
Our at-risk managed care membership totaled approximately 1.5 million as of December 31, 2009. For the year ended December 31, 2009, our revenues and net earnings from continuing operations were $4.1 billion and $86.1 million, respectively, and our total cash flow from operations was $248.2 million.
In November 2009, the Mississippi Division of Medicaid selected Centene as one of two organizations to participate in the Mississippi Coordinated Access Network, a program for Mississippi Medicaid beneficiaries. We are continuing to work with Mississippi to execute a contract in which we will serve eligible members throughout the state, as
Magnolia Health Plan, and expect to execute the contract and begin managing care for ABD members in Mississippi in 2010.
We provide member-focused services through locally based staff by assisting in accessing care, coordinating referrals to related health and social services and addressing member concerns and questions. We also provide education and outreach programs to inform and assist members in accessing quality, appropriate healthcare services. We
believe our local approach to managing our health plans, including provider and member services, enables us to provide accessible, quality, culturally-sensitive healthcare coverage to our communities. Our health management, educational and other initiatives are designed to help members best utilize the healthcare system to ensure they receive appropriate, medically necessary services and effective management of routine, severe and chronic health problems, resulting in better health outcomes. We
combine our decentralized local approach for care with a centralized infrastructure of support functions such as finance, information systems and claims processing.
Our initial health plan commenced operations in Wisconsin in 1984. We were organized in Wisconsin in 1993 as a holding company for our initial health plan and reincorporated in Delaware in 2001. Our corporate office is located at 7711 Carondelet Avenue, St. Louis, Missouri 63105, and our telephone number is (314) 725-4477. Our
stock is publicly traded on the New York Stock Exchange under the ticker symbol “CNC.”
INDUSTRY
We provide our services to the uninsured primarily through Medicaid, CHIP, Foster Care, ABD, Medicare and other state programs for the uninsured. The federal Centers for Medicare and Medicaid Services, or CMS, estimated the total Medicaid market was approximately $329 billion in 2007, and estimate the market will grow to $800 billion
by 2018. According to the most recent information provided by the Kaiser Commission on Medicaid and the Uninsured, Medicaid spending increased by 7.9% in fiscal 2009 and states appropriated an increase of 6.3% for Medicaid in fiscal 2010 budgets.
Established in 1965, Medicaid is the largest publicly funded program in the United States, and provides health insurance to low-income families and individuals with disabilities. Authorized by Title XIX of the Social Security Act, Medicaid is an entitlement program funded jointly by the federal and state governments and administered
by the states. The majority of funding is provided at the federal level. Each state establishes its own eligibility standards, benefit packages, payment rates and program administration within federal standards. As a result, there are 56 Medicaid programs— one for each U.S. state, each U.S. territory and the District of Columbia. Many states have selected Medicaid managed care as a means of delivering quality healthcare and controlling costs, including states
that automatically enroll Medicaid recipients who don’t select a health plan. We refer to these states as mandated managed care states. Eligibility is based on a combination of household income and assets, often determined by an income level relative to the federal poverty level. Historically, children have represented the largest eligibility group.
Established in 1972, and authorized by Title XVI of the Social Security Act, ABD covers low-income persons with chronic physical disabilities or behavioral health impairments. ABD beneficiaries represent a growing portion of all Medicaid recipients. In addition, ABD recipients typically utilize more services because
of their critical health issues.
The Balanced Budget Act of 1997 created CHIP to help states expand coverage primarily to children whose families earned too much to qualify for Medicaid, yet not enough to afford private health insurance. Some states include the parents of these children in their CHIP programs. CHIP is the single largest expansion of
health insurance coverage for children since the enactment of Medicaid. Costs related to the largest eligibility group, children, are primarily composed of pediatrics and family care. These costs tend to be more predictable than other healthcare issues which predominantly affect the adult population.
A portion of Medicaid beneficiaries are dual eligibles, low-income seniors and people with disabilities who are enrolled in both Medicaid and Medicare. According to the Kaiser Commission on Medicaid and the Uninsured, there were approximately 8.8 million dual eligible enrollees in 2009. These dual eligibles may receive
assistance from Medicaid for Medicaid benefits, such as nursing home care and/or assistance with Medicare premiums and cost sharing. Dual eligibles also use more services due to their tendency to have more chronic health issues. We serve dual eligibles through our ABD and long-term care programs, and beginning in 2008, through Special Needs Plans.
While Medicaid programs have directed funds to many individuals who cannot afford or otherwise maintain health insurance coverage, they did not initially address the inefficient and costly manner in which the Medicaid population tends to access healthcare. Medicaid recipients in non-managed care programs typically have not sought
preventive care or routine treatment for chronic conditions, such as asthma and diabetes. Rather, they have sought healthcare in hospital emergency rooms, which tends to be more expensive. As a result, many states have found that the costs of providing Medicaid benefits have increased while the medical outcomes for the recipients remained unsatisfactory.
Since the early 1980s, increasing healthcare costs, combined with significant growth in the number of Medicaid recipients, have led many states to establish Medicaid managed care initiatives. Additionally, a number of states are designing programs to cover the rising number of uninsured Americans. The Kaiser Commission
on Medicaid and the Uninsured estimated there were over 46 million Americans in 2008 that lacked health insurance. We expect that continued pressure on states’ Medicaid budgets will cause public policy to recognize the value of managed care as a means of delivering quality healthcare and effectively controlling costs. A growing number of states have mandated that their Medicaid recipients enroll in managed care plans. Other states are considering moving to a mandated managed
care approach. As a result, a significant market opportunity exists for managed care organizations with operations and programs focused on the distinct socio-economic, cultural and healthcare needs of the uninsured population and the Medicaid, CHIP, Foster Care and ABD populations. We believe our approach and strategy enable us to be a growing participant in this market.
OUR COMPETITIVE STRENGTHS
Our multi-line managed care approach is based on the following key attributes:
|
· |
Strong Historic Operating Performance. We have increased revenues as we have grown in existing markets, expanded into new markets and broadened our product offerings. We entered the Wisconsin market in 1984, the Indiana market in 1995, the Texas market in 1999, the Arizona
market in 2003, the Ohio market in 2004, the Georgia market in 2006, the South Carolina market in 2007 and the Florida and Massachusetts markets in 2009. We have increased our membership through participation in new programs in existing states. For example, in 2008, we began operations in the Texas Foster Care program and began serving Acute Care members in Yavapai county of Arizona. We have also increased membership by acquiring Medicaid businesses, contracts and other related assets from competitors in existing
markets, most recently in Florida and South Carolina in 2009. Our at-risk membership totaled approximately 1.5 million as of December 31, 2009. For the year ended December 31, 2009, we had revenues of $4.1 billion, representing a 39% Compound Annual Growth Rate, or CAGR, since the year ended December 31, 2005. We generated total cash flow from operations of $248.2 million and net earnings of $86.1 million for the year ended December
31, 2009. |
|
· |
Medicaid Expertise. Over the last 25 years, we have developed a specialized Medicaid expertise that has helped us establish and maintain relationships with members, providers and state governments. We have implemented programs developed to achieve savings for state governments
and improve medical outcomes for members by reducing inappropriate emergency room use, inpatient days and high cost interventions, as well as by managing care of chronic illnesses. Our experience in working with state regulators helps us implement and deliver programs and services efficiently and affords us opportunities to provide input regarding Medicaid industry practices and policies in the states in which we operate. We work with state agencies on redefining benefits, eligibility requirements
and provider fee schedules in order to maximize the number of uninsured individuals covered through Medicaid, CHIP, Foster Care and ABD and expand these types of benefits offered. Our approach is to accomplish this while maintaining adequate levels of provider compensation and protecting our profitability. |
|
· |
Diversified Business Lines. We continue to broaden our service offerings to address areas that we believe have been traditionally underserved by Medicaid managed care organizations. In addition to our Medicaid and Medicaid-related managed care services, our service offerings
include behavioral health, individual health insurance, life and health management, long-term care programs, managed vision, telehealth services and pharmacy benefits management. Through the utilization of a multi-business line approach, we are able to improve quality of care, improve outcomes, and diversify our revenues and help control our medical costs. |
|
· |
Localized Approach with Centralized Support Infrastructure. We take a localized approach to managing our subsidiaries, including provider and member services. This approach enables us to facilitate access by our members to high quality, culturally sensitive healthcare services. Our
systems and procedures have been designed to address these community-specific challenges through outreach, education, transportation and other member support activities. For example, our community outreach programs work with our members and their communities to promote health and self-improvement through employment and education on how best to access care. We complement this localized approach with a centralized infrastructure of support functions such as finance, information systems and
claims processing, which allows us to minimize general and administrative expenses and to integrate and realize synergies from acquisitions. We believe this combined approach allows us to efficiently integrate new business opportunities in both Medicaid and specialty services while maintaining our local accountability and improved access. |
|
· |
Specialized and Scalable Systems and Technology. Through our specialized information systems, we work to strengthen relationships with providers and states which help us grow our membership base. We continue to develop our specialized information systems which allow us to support
our core processing functions under a set of integrated databases, designed to be both replicable and scalable. Physicians can use claims, utilization and membership data to manage their practices more efficiently, and they also benefit from our timely payments. State agencies can use data from our information systems to demonstrate that their Medicaid populations receive quality healthcare in an efficient manner. These systems also help identify needs for new healthcare and specialty
programs. We have the ability to leverage our platform for one state configuration into new states or for health plan acquisitions. Our ability to access data and translate it into meaningful information is essential to operating across a multi-state service area in a cost-effective manner. |
OUR BUSINESS STRATEGY
Our objective is to become the leading multi-line healthcare enterprise focusing on the uninsured population and state funded healthcare initiatives. We intend to achieve this objective by implementing the following key components of our strategy:
|
· |
Increase Penetration of Existing State Markets. We seek to continue to increase our Medicaid membership in states in which we currently operate through alliances with key providers, outreach efforts, development and implementation of community-specific products and acquisitions.
In 2006, we were awarded two regions in connection with Ohio’s statewide restructuring of its Medicaid managed care program, expanding the number of counties we serve from three to 27. We also were awarded a Medicaid ABD contract in Ohio. In Texas, we expanded our operations to the Corpus Christi market in 2006, began managing care for ABD recipients in February 2007 and began operations in the Foster Care program in April 2008. In Arizona, we began serving members of a long-term care plan in 2006 and within
an acute care plan in 2008. In 2008, we began serving Medicare members within Special Needs Plans in Arizona, Ohio, Texas and Wisconsin. We may also increase membership by acquiring Medicaid businesses, contracts and other related assets from our competitors in our existing markets or by enlisting additional providers. For example, in 2009, we acquired certain Medicaid-related assets in Florida and South Carolina. |
|
· |
Diversify Business Lines. We seek to broaden our business lines into areas that complement our existing business to enable us to grow and diversify our revenue. We are constantly evaluating new opportunities for expansion both domestically and abroad. For instance, in
July 2008, we completed the acquisition of Celtic Insurance Company, a national individual health insurance provider, in October 2006, we commenced operations under our managed care program contracts to provide long-term care services in Arizona, and in January 2006, we completed the acquisition of US Script, a pharmacy benefits manager. We are also considering other premium based or fee-for-service lines of business that would provide additional diversity. We employ a disciplined acquisition strategy that is
based on defined criteria including internal rate of return, accretion to earnings per share, market leadership and compatibility with our information systems. We engage our executives in the relevant operational units or functional areas to ensure consistency between the diligence and integration process. |
|
· |
Address Emerging State Needs. We work to assist the states in which we operate in addressing the operating challenges they face. We seek to assist the states in balancing premium rates, benefit levels, member eligibility, policies and practices, and provider compensation.
For example, in 2008, we began operating under a contract with the Texas Health and Human Services Commission for Comprehensive Health Care for Children in Foster Care, a new statewide program providing managed care services to participants in the Texas Foster Care program. By helping states structure an appropriate level and range of Medicaid, CHIP and specialty services, we seek to ensure that we are able to continue to provide those services on terms that achieve targeted gross margins, provide an acceptable
return and grow our business. |
|
· |
Develop and Acquire Additional State Markets. We continue to leverage our experience to identify and develop new markets by seeking both to acquire existing business and to build our own operations. We expect to focus expansion in states where Medicaid recipients are
mandated to enroll in managed care organizations, because we believe member enrollment levels are more predictable in these states. In addition, we focus on states where managed care programs can help address states’ financial needs. For example, effective June 1, 2006, we began managing care for Medicaid and CHIP members in Georgia. In 2007, we entered the South Carolina market and we participated in the state’s conversion to at-risk managed care. In February 2009, we began
managed care operations in Florida through conversion of members in certain counties from Access Health Solutions to at-risk managed care in Sunshine State Health Plan, through our new state contract. In July 2009, we began operating under our contract in Massachusetts to manage healthcare services operating as CeltiCare Health Plan of Massachusetts. In 2010, we expect to begin managing care for ABD members in Mississippi. |
|
· |
Leverage Established Infrastructure to Enhance Operating Efficiencies. We intend to continue to invest in infrastructure to further drive efficiencies in operations and to add functionality to improve the service provided to members and other organizations at a low cost.
Information technology, or IT, investments complement our overall efficiency goals by increasing the automated processing of transactions and growing the base of decision-making analytical tools. Our centralized functions enable us to add members and markets quickly and economically. |
|
· |
Maintain Operational Discipline. We monitor our cost trends, operating performance, regulatory relationships and the Medicaid political environment in our existing markets. We seek to operate in markets that allow us to meet our internal metrics including membership
growth, plan size, market leadership and operating efficiency. We may divest contracts or health plans in markets where the state’s Medicaid environment, over a long-term basis, does not allow us to meet our targeted performance levels. We use multiple techniques to monitor and reduce our medical costs, including on-site hospital review by staff nurses and involvement of medical management and finance personnel in significant cases. Our management team regularly evaluates the financial impact of proposed
changes in provider relationships, contracts, swings in membership and mix of members, potential state rate changes and cost reduction initiatives. |
We have regulated subsidiaries offering healthcare services in each state we serve. The table below provides summary data for the state markets we currently serve:
|
State |
Local Health Plan Name |
|
First Year of Operations Under the Company |
|
Counties Served at December 31, 2009 |
|
Market Share (1) |
At-risk Managed Care Membership at
December 31, 2009 |
| ||
|
Arizona |
Bridgeway Health Solutions (2) |
2008 |
4 |
1.5% |
18,100 |
||||||
|
Florida |
Sunshine State Health Plan |
2009 |
9 |
9.9% |
102,600 |
||||||
|
Georgia |
Peach State Health Plan |
2006 |
90 |
28.0% |
309,700 |
||||||
|
Indiana |
Managed Health Services |
1995 |
92 |
31.9% |
208,100 |
||||||
|
Ohio |
Buckeye Community Health Plan |
2004 |
43 |
10.1% |
150,800 |
||||||
|
Massachusetts |
CeltiCare Health Plan |
2009 |
14 |
(3) |
27,800 |
||||||
|
South Carolina |
Absolute Total Care |
2007 |
42 |
10.4% |
48,600 |
||||||
|
Texas |
Superior HealthPlan |
1999 |
239 |
22.2% |
455,100 |
||||||
|
Wisconsin |
Managed Health Services |
1984 |
33 |
21.0% |
134,800 |
||||||
|
566 |
1,455,600 |
||||||||||
|
(1) |
Represents Medicaid and CHIP membership as of December 31, 2009 as a percentage of total eligible Medicaid and CHIP members in each state. ABD programs are excluded. |
|
(2) |
Represents the acute care and Medicare business under Bridgeway Health Solutions. |
|
(3) |
CeltiCare Health Plan manages members under the state Commonwealth Care Bridge program and Commonwealth Care program with market share of 100% and less than 0.1% , respectively. |
All of our revenue is derived from operations within the United States and its territories. We generally receive a fixed premium per member per month pursuant to our state contracts. Our medical costs have a seasonality component due to cyclical illness, for example cold and flu season, resulting in higher medical expenses
beginning in the fourth quarter and continuing throughout the first quarter of each year. Our managed care subsidiaries in Georgia, Ohio, and Texas had revenues from their respective state governments that each exceeded 10% of our consolidated total revenues in 2009. Other financial information about our segments is found in Note 21, Segment Information, of our Notes to Consolidated Financial Statements and “Management’s
Discussion and Analysis of Financial Condition and Results of Operations” included elsewhere in this Annual Report on Form 10-K.
MEDICAID MANAGED CARE
Benefits to States
Our ability to establish and maintain a leadership position in the markets we serve results primarily from our demonstrated success in providing quality care while reducing and managing costs, and from our specialized programs in working with state governments. Among the benefits we are able to provide to the states with which
we contract are:
|
· |
Significant cost savings compared to state paid reimbursement for services. We bring bottom-line management experience to our health plans. On the administrative and management side, we bring experience including quality of care improvement methods, utilization management procedures,
an efficient claims payment system, and provider performance reporting, as well as managers and staff experienced in using these key elements to improve the quality of and access to care. |
|
· |
Data-driven approaches to balance cost and verify eligibility. Our Medicaid health plans have conducted enrollment processing and activities for state programs since 1984. We seek to ensure effective enrollment procedures that move members into the plan, then educate them and
ensure they receive needed services as quickly as possible. Our IT department has created mapping/translation programs for loading membership and linking membership eligibility status to all of Centene’s subsystems. |
|
· |
Establishment of realistic and meaningful expectations for quality deliverables. We have collaborated with state agencies in redefining benefits, eligibility requirements and provider fee schedules with the goal of maximizing the number of individuals covered through Medicaid, CHIP, Foster
Care and ABD programs. |
|
· |
Managed care expertise in government subsidized programs. Our expertise in Medicaid has helped us establish and maintain strong relationships with our constituent communities of members, providers and state governments. We provide access to services through local providers and
staff that focus on the cultural norms of their individual communities. To that end, systems and procedures have been designed to address community-specific challenges through outreach, education, transportation and other member support activities. |
|
· |
Improved medical outcomes. We have implemented programs developed to achieve savings for state governments and improve medical outcomes for members by reducing inappropriate emergency room use, inpatient days and high cost interventions, as well as by managing care of chronic illness. |
|
· |
Timely payment of provider claims. We are committed to ensuring that our information systems and claims payment systems meet or exceed state requirements. We continuously endeavor to update our systems and processes to improve the timeliness of our provider payments. |
|
· |
Cost saving outreach and specialty programs. Our health plans have adopted a physician-driven approach where network providers are actively engaged in developing and implementing healthcare delivery policies and strategies. This approach is designed to eliminate unnecessary
costs, improve services to members and simplify the administrative burdens placed on providers. |
|
· |
Responsible collection and dissemination of utilization data. We gather utilization data from multiple sources, allowing for an integrated view of our members’ utilization of services. These sources include medical, vision and behavioral health claims and encounter data,
pharmacy data, dental vendor claims and authorization data from the authorization and case management system utilized by us to coordinate care. |
|
· |
Timely and accurate reporting. Our information systems have reporting capabilities which have been instrumental in identifying the need for new and/or improved healthcare and specialty programs. For state agencies, our reporting capability is important in demonstrating an auditable
program. |
|
· |
Fraud and abuse prevention. We have several systems in place to help identify, detect and investigate potential waste, abuse and fraud including pre and post payment software. We collaborate with state and federal agencies and assist with investigation requests. We
use nationally recognized standards to benchmark our processes. |
Member Programs and Services
We recognize the importance of member-focused delivery of quality managed care services. Our locally-based staff assists members in accessing care, coordinating referrals to related health and social services and addressing member concerns and questions. While covered healthcare benefits vary from state to state, our
health plans generally provide the following services:
|
Ÿ |
primary and specialty physician care |
Ÿ |
transportation assistance | |
|
Ÿ |
inpatient and outpatient hospital care |
Ÿ |
vision care | |
|
Ÿ |
emergency and urgent care |
Ÿ |
dental care | |
|
Ÿ |
prenatal care |
Ÿ |
immunizations | |
|
Ÿ |
laboratory and x-ray services |
Ÿ |
prescriptions and limited over-the-counter drugs | |
|
Ÿ |
home health and durable medical equipment |
Ÿ |
therapies | |
|
Ÿ |
behavioral health and substance abuse services |
Ÿ |
social work services | |
|
Ÿ |
24-hour nurse advice line |
|
We also provide the following education and outreach programs to inform and assist members in accessing quality, appropriate healthcare services in an efficient manner:
|
Ÿ |
Fluvention is an outreach program aimed at educating members on preventing the transmission of the influenza virus by encouraging members to get the seasonal influenza vaccines and take everyday precautions to prevent illness. We use an integrated communications approach including direct mail, phone
calls, providing information via health plan websites and posting information in provider offices. The health plans also conduct general community awareness through public service announcements on television and radio. During 2009, we targeted education efforts related to health hygiene, preventative care and the benefits of obtaining appropriate care of their condition, for groups that are at higher-risk for contracting the H1N1 influenza virus, including pregnant women, children from six
months old up to 24-year-old adults, as well as adults with chronic health conditions. Incentives in the form of gift cards were given to members who received both flu vaccines. |
|
Ÿ |
MemberConnections is a community face-to-face outreach and education program designed to create a link between the member and the provider and help identify potential challenges or risk elements to a member’s health, such as nutritional challenges and health education shortcomings. MemberConnections
representatives also contact new members by phone or mail to discuss managed care, the Medicaid program and our services. Our MemberConnections representatives make home visits, conduct educational programs and represent our health plans at community events such as health fairs. |
|
Ÿ |
Connections Plus is a cell phone program developed for high-risk members who have limited or no access to a safe, reliable telephone. The program puts free, preprogrammed cell phones into the hands of eligible members. This program seeks to eliminate lack of safe, reliable access
to a telephone as a barrier to coordinating care, thus reducing avoidable adverse events such as inappropriate emergency room utilization, hospital admissions and premature birth. Members are identified through case management activities or through a referral. Connections Plus is available to high-risk members in all Centene health plans. Connections Plus has been recognized as a URAC Best Practice 2009 Silver Medalist and is included in the NCQA Quality Profiles Manual
for 2009. |
|
Ÿ |
Start Smart For Your Baby is a prenatal and infant health program designed to increase the percentage of pregnant women receiving early prenatal care, reduce the incidence of low birth weight babies, identify high risk pregnancies, increase participation in the federal Women, Infant and Children
program, prevent hospital admissions in the first year of life and increase well-child visits. The program includes risk assessments, education through face-to-face meetings and materials, behavior modification plans, assistance in selecting a provider for the infant and scheduling newborn follow-up visits. Start Smart was named a 2009 NCQA Best Practice. |
|
Ÿ |
EPSDT Case Management is a preventive care program designed to educate our members on the benefits of Early and Periodic Screening, Diagnosis and Treatment, or EPSDT, services. We have a systematic program of communicating, tracking, outreach, reporting and follow-through that promotes
state EPSDT programs. |
|
Ÿ |
Life and Health Management Programs are designed to help members understand their disease and treatment plan and improve their wellness in a cost effective manner. These programs address medical conditions that are common within the Medicaid population such as asthma, diabetes and pregnancy. Our
Specialty Services segment manages many of our life and health management programs. Our ABD program uses a proprietary assessment tool that effectively identifies barriers to care, unmet functional needs, available social supports and the existence of behavioral health conditions that impede a member’s ability to maintain a proper health status. Care coordinators develop individual care plans with the member and healthcare providers ensuring the full integration of behavioral, social
and acute care services. These care plans, while specific to an ABD member, incorporate “Condition Specific” practices in collaboration with physician partners and community resources. |
|
Ÿ |
The Kids' Club is aimed at educating child members on a variety of health topics. Our health plans are reaching out directly to children with newsletters, contests and other innovative events, such as readings with the author of "The Adventures of Thumbs Up Johnnie.” The Kids' Club
is initially focusing on the childhood obesity epidemic - obesity rates for children doubled in the past two decades and tripled for adolescents during the same period - with educational information encouraging proper eating and exercise habits. We have sponsored the creation of a book with Michelle Bain titled "Thumbs Up Johnnie & the SUPER Centeam 5- Adventures Through FITROPOLIS!" which is intended to educate children on the importance of living an active and healthy life. |
Providers
For each of our service areas, we establish a provider network consisting of primary and specialty care physicians, hospitals and ancillary providers. As of December 31, 2009, the health plans we currently operate contracted with the following number of physicians and hospitals:
|
|
Primary Care
Physicians |
|
Specialty Care
Physicians |
|
Hospitals | |
|
Arizona |
303 |
2,170 |
8 | |||
|
Florida |
922 |
2,032 |
57 | |||
|
Georgia |
2,992 |
9,569 |
123 | |||
|
Indiana |
|
1,016 |
|
4,087 |
|
93 |
|
Massachusetts |
1,083 |
4,132 |
31 | |||
|
Ohio |
|
2,359 |
|
9,262 |
|
140 |
|
South Carolina |
1,172 |
2,933 |
37 | |||
|
Texas |
|
8,243 |
|
20,786 |
|
395 |
|
Wisconsin |
|
2,103 |
|
5,770 |
|
64 |
|
Total |
20,193 |
60,741 |
948 |
Our network of primary care physicians is a critical component in care delivery, management of costs and the attraction and retention of new members. Primary care physicians include family and general practitioners, pediatricians, internal medicine physicians and obstetricians and gynecologists. Specialty care physicians
provide medical care to members generally upon referral by the primary care physicians. Specialty care physicians include, but are not limited to, orthopedic surgeons, cardiologists and otolaryngologists. We also provide education and outreach programs to inform and assist members in accessing quality, appropriate healthcare services.
Our health plans facilitate access to healthcare services for our members primarily through contracts with our providers. Our contracts with primary and specialty care physicians and hospitals usually are for one to two-year periods and renew automatically for successive one-year terms, but generally are subject to termination
by either party upon 90 to 120 days prior written notice. In the absence of a contract, we typically pay providers at state Medicaid reimbursement levels. We pay hospitals under a variety of methods, including fee-for-services, per diems, diagnostic related groups and case rates. We pay physicians under a fee-for-service, capitation arrangement, or risk-sharing arrangement.
|
|
|
|
Ÿ |
Under our fee-for-service contracts with physicians, particularly specialty care physicians, we pay a negotiated fee for covered services. This model is characterized as having no financial risk for the physician. In addition, this model requires management oversight because our total cost may increase as the units of services increase
or as more expensive services replace less expensive services. We have prior authorization procedures in place that are intended to make sure that certain high cost diagnostic and other services are medically appropriate. |
|
Ÿ |
Under our capitated contracts, primary care physicians are paid a monthly fee for each of our members assigned to his or her practice for all ambulatory care. In return for this payment, these physicians provide all primary care and preventive services, including primary care office visits and EPSDT services, and are at risk for all costs associated
with such services. If these physicians also provide non-capitated services to their assigned members, they may receive payment under fee-for-service arrangements at standard Medicaid rates. |
|
Ÿ |
Under risk-sharing arrangements, physicians are paid under a capitated or fee-for-service arrangement. The arrangement, however, contains provisions for additional bonus to the physicians or reimbursement from the physicians based upon cost and quality factors. We often refer to these arrangements as Model 1 contracts. |
We work with physicians to help them operate efficiently by providing financial and utilization information, physician and patient educational programs and disease and medical management programs. Our programs are also designed to help the physicians coordinate care outside of their offices. In addition, we are governed
by state prompt payment policies.
We believe our collaborative approach with physicians gives us a competitive advantage in entering new markets. Our physicians serve on local committees that assist us in implementing preventive care programs, managing costs and improving the overall quality of care delivered to our members, while also simplifying the administrative
burdens on our providers. This approach has enabled us to strengthen our provider networks through improved physician recruitment and retention that, in turn, have helped to increase our membership base. The following are among the services we provide to support physicians:
|
|
|
|
|
Ÿ |
Customized Utilization Reports provide certain of our contracted physicians with information that enables them to run their practices more efficiently and focuses them on specific patient needs. For example, quarterly detail reports update physicians on their status within their risk pools. Equivalency reports provide physicians with financial
comparisons of capitated versus fee-for-service arrangements. |
|
|
Ÿ |
Case Management Support helps the physician coordinate specialty care and ancillary services for patients with complex conditions and direct members to appropriate community resources to address both their health and socio-economic needs. |
|
|
|
|
|
Ÿ |
Web-based Claims and Eligibility Resources have been implemented in selected markets to provide physicians with on-line access to perform claims and eligibility inquiries. |
|
|
|
Our contracted physicians also benefit from several of the services offered to our members, including the MemberConnections, EPSDT case management and health management programs. For example, the MemberConnections staff facilitates doctor/patient relationships by connecting members with physicians, the EPSDT programs encourage
routine checkups for children with their physicians and the health management programs assist physicians in managing their patients with chronic disease.
Where appropriate, our health plans contract with our specialty services organizations to provide services and programs such as behavioral health, health management, managed vision, telehealth services, pharmacy benefit management, and treatment compliance. When necessary, we also contract with third-party providers on a negotiated
fee arrangement for physical therapy, home healthcare, diagnostic laboratory tests, x-ray examinations, ambulance services and durable medical equipment. Additionally, we contract with dental vendors in markets where routine dental care is a covered benefit.
Quality Management
Our medical management programs focus on improving quality of care in areas that have the greatest impact on our members. We employ strategies, including health management and complex case management, that are adjusted for implementation in our individual markets by a system of physician committees chaired by local physician leaders. This
process promotes physician participation and support, both critical factors in the success of any clinical quality improvement program.
We have implemented specialized information systems to support our medical quality management activities. Information is drawn from our data warehouse, clinical databases and our membership and claims processing system, to identify opportunities to improve care and to track the outcomes of the interventions implemented to achieve
those improvements. Some examples of these intervention programs include:
|
· |
appropriate leveling of care for neonatal intensive care unit hospital admissions, other inpatient hospital admissions, and observation admissions, in accordance with Interqual criteria; |
|
· |
tightening of our pre-authorization list and more stringent review of durable medical equipment and injectibles; |
|
· |
emergency department, or ED, program designed to collaboratively work with hospitals to steer non-emergency care away from the costly ED setting (through patient education, on-site alternative urgent care settings, etc.); |
|
· |
increase emphasis on case management and clinical rounding where case managers are nurses or social workers who are employed by the health plan to assist selected patients with the coordination of healthcare services in order to meet a patient's specific healthcare needs; |
|
· |
incorporation of disease management, which is a comprehensive, multidisciplinary, collaborative approach to chronic illnesses such as asthma and diabetes; and |
|
· |
Start Smart For Your Baby, a prenatal case management program aimed at helping women with high-risk pregnancies deliver full-term, healthy infants. |
We provide reporting on a regular basis using our data warehouse. State and Health Employer Data and Information Set reporting constitutes the core of the information base that drives our clinical quality performance efforts. This reporting is monitored by Plan Quality Improvement Committees and our corporate medical
management team.
In an effort to ensure the quality of our provider networks, we undertake to verify the credentials and background of our providers using standards that are supported by the National Committee for Quality Assurance.
Information Technology
The ability to access data and translate it into meaningful information is essential to operating across a multi-state service area in a cost-effective manner. Our centralized information systems, which are located in St. Louis, Missouri, support our core processing functions under a set of integrated databases and are designed
to be both replicable and scalable to accommodate organic growth and growth from acquisitions. We continue to enhance our systems in order to leverage the platform we have developed for our existing states for configuration into new states or health plan acquisitions.
Our predictive modeling technology enables the medical management operations to proactively case and disease manage specific high risk members. It can recommend medical care opportunities using a mix of company defined algorithms and evidence based medical guidelines. Interventions are determined by the clinical indicators,
the ability to improve health outcomes, and the risk profile of members.
Our integrated approach helps to assure that consistent sources of claim and member information are provided across all of our health plans. Our membership and claims processing system is capable of expanding to support additional members in an efficient manner. We have a disaster recovery and business resumption plan
developed and implemented in conjunction with a third party. This plan allows us complete access to the business resumption centers and hot-site facilities provided under the business resumption plan.
SPECIALTY COMPANIES
Our specialty companies are a key component of our healthcare enterprise and complement our core Medicaid Managed Care business. Specialty services diversify our revenue stream, provide higher quality health outcomes to our membership and others, and assist in controlling costs. Our specialty services are provided primarily
through the following businesses:
|
Ÿ |
Behavioral Health. Cenpatico Behavioral Health, or Cenpatico, manages behavioral healthcare for members via a contracted network of providers. Cenpatico works with providers to determine the best services to help people overcome mental illness and lead productive lives. Our
networks feature a full range of services and levels of care to help people with mental illness reach their recovery and wellness goals. We also run school-based programs in Arizona that focus on students with special needs including speech therapy services. We acquired Cenpatico in 2003. |
|
Ÿ |
Individual and State Sponsored Health Insurance. Celtic Insurance Company, or Celtic, is a national healthcare provider licensed in 49 states offering high-quality, affordable health insurance to individual customers and their families. Sold online and through independent insurance
agents nationwide, Celtic’s portfolio of major medical plans is designed to meet the diverse needs of the uninsured at all budget and benefit levels. Celtic also offers a standalone guaranteed-issue medical conversion program to self-funded employer groups, stop-loss and fully-insured group carriers, managed care plans, and HMO reinsurers. We acquired Celtic in July 2008. In 2009, CeltiCare of Massachusetts was formed to provide state sponsored health insurance to the uninsured who do not qualify
for Medicaid. |
|
Ÿ |
Life and Health Management. Nurtur Health specializes in implementing life and health management programs that encourage healthy behaviors, promote healthier workplaces, improve productivity and reduce healthcare costs. Health risk appraisals, biometric screenings, online and
telephonic wellness programs, disease management and work-life services are areas of focus. Nurtur Health uses telephonic health coaching, in-home and online interaction and informatics processes to deliver effective clinical results, enhanced patient-provider satisfaction and cost reductions in its health management operations. Nurtur Health was formed in December 2007 through the combination of three entities we acquired from
July 2005 through November 2007. |
|
Ÿ |
Long-term Care and Acute Care. Bridgeway Health Solutions, or Bridgeway, provides long-term care services to the elderly and people with disabilities that meet income and resources requirements who are at risk of being or are institutionalized. Bridgeway has long-term members
in the Maricopa, Yuma and La Paz counties of Arizona. Bridgeway participates with community groups to address situations that might be barriers to quality care and independent living. Bridgeway commenced long-term care operations in 2006. Bridgeway also provides acute care services to members in the Yavapai county of Arizona. These services include emergency and physician services, limited dental and rehabilitative services and other maternal and child health services. Bridgeway
commenced acute care operations in October 2008. |
|
Ÿ |
Managed Vision. OptiCare manages vision benefits for members via a contracted network of providers. OptiCare offers a variety of vision plan designs to help meet the needs of is members and clinics. OptiCare provides a range of products and services so that clients
can implement a vision plan to fit their needs and patients can be treated at appropriate levels of care. We acquired the managed vision business of OptiCare Health Systems, Inc. in 2006. |
|
Ÿ |
Telehealth Services. NurseWise and Nurse Response provide a toll-free nurse triage line 24 hours per day, 7 days per week, 52 weeks per year. Our members call one number and reach bilingual customer service representatives and nursing staff who provide health education, triage
advice and offer continuous access to health plan functions. Additionally, our representatives verify eligibility, confirm primary care provider assignments and provide benefit and network referral coordination for members and providers after business hours. Our staff can arrange for urgent pharmacy refills, transportation and qualified behavioral health professionals for crisis stabilization assessments. Call volume is based on membership levels and seasonal variation. NurseWise
commenced operations in 1998. |
|
Ÿ |
Pharmacy Benefits Management. US Script is a pharmacy benefits manager that administers pharmacy benefits and processes pharmacy claims via its proprietary claims processing software. US Script has developed and administers a contracted national network of retail pharmacies. We
acquired US Script in 2006. |
CORPORATE COMPLIANCE
Our Corporate Ethics and Compliance Program was first established in 1998 and provides methods by which we further enhance operations, safeguard against fraud and abuse, improve access to quality care and help assure that our values are reflected in everything we do.
The two primary standards by which corporate compliance programs in the healthcare industry are measured are the 1991 Federal Organizational Sentencing Guidelines and the “Compliance Program Guidance” series issued by the Office of the Inspector General, or OIG, of the Department of Health and Human Services. Our program
contains each of the seven elements suggested by the Sentencing Guidelines and the OIG guidance. These key components are:
|
Ÿ |
written standards of conduct; |
|
Ÿ |
designation of a corporate compliance officer and compliance committee; |
|
Ÿ |
effective training and education; |
|
Ÿ |
effective lines for reporting and communication; |
|
Ÿ |
enforcement of standards through disciplinary guidelines and actions; |
|
Ÿ |
internal monitoring and auditing; and |
|
Ÿ |
prompt response to detected offenses and development of corrective action plans. |
Our internal Corporate Compliance website, accessible by all employees, contains our Business Ethics and Conduct Policy, our Mission, Values and Philosophies and Compliance Programs, a company-wide policy and procedure database and our toll-free hotline to allow employees or other persons to report suspected incidents of fraud, abuse or other
violations. The audit committee and the board of directors review a compliance report on a quarterly basis.
COMPETITION
We continue to face varying and increasing levels of competition as we expand in our existing service areas or enter new markets, as federal regulations require at least two competitors in each service area. Healthcare reform proposals may cause a number of commercial managed care organizations to decide to enter or exit the Medicaid
market.
In our business, our principal competitors for state contracts, members and providers consist of the following types of organizations:
|
Ÿ |
Medicaid Managed Care Organizations focus on providing healthcare services to Medicaid recipients. These organizations consist of national and regional organizations, as well as smaller organizations that operate in one city or state and are owned by providers, primarily hospitals. |
|
Ÿ |
National and Regional Commercial Managed Care Organizations have Medicaid members in addition to members in private commercial plans. Some of these organizations offer a range of specialty services including pharmacy benefits management, behavioral health management, health management,
and nurse triage call support centers. |
|
Ÿ |
Primary Care Case Management Programs are programs established by the states through contracts with primary care providers. Under these programs, physicians provide primary care services to Medicaid recipients, as well as limited medical management oversight. |
We compete with other managed care organizations and specialty companies for state contracts. In order to grant a contract, state governments consider many factors. These factors include quality of care, financial requirements, an ability to deliver services and establish provider networks and infrastructure. In
addition, our specialty companies also compete with other providers, such as disease management companies, individual health insurance companies, and pharmacy benefits managers for non-governmental contracts.
We also compete to enroll new members and retain existing members. People who wish to enroll in a managed healthcare plan or to change healthcare plans typically choose a plan based on the quality of care and services offered, ease of access to services, a specific provider being part of the network and the availability of supplemental
benefits.
We also compete with other managed care organizations to enter into contracts with physicians, physician groups and other providers. We believe the factors that providers consider in deciding whether to contract with us include existing and potential member volume, reimbursement rates, medical management programs, speed of reimbursement
and administrative service capabilities. See “Risk Factors — Competition may limit our ability to increase penetration of the markets that we serve.”
REGULATION
Our Medicaid, Medicare and Specialty operations are regulated at both state and federal levels. Government regulation of the provision of healthcare products and services is a changing area of law that varies from jurisdiction to jurisdiction. Regulatory agencies generally have discretion to issue regulations and interpret
and enforce laws and rules. Changes in applicable laws and rules also may occur periodically.
Our regulated subsidiaries are licensed to operate as health maintenance organizations and/or insurance companies in their respective states. In each of the jurisdictions in which we operate, we are regulated by the relevant health, insurance and/or human services departments that oversee the activities of managed care organizations
providing or arranging to provide services to Medicaid enrollees.
The process for obtaining authorization to operate as a managed care organization is complex and requires us to demonstrate to the regulators of the adequacy of the health plan’s organizational structure, financial resources, utilization review, quality assurance programs, complaint procedures, provider network adequacy and procedures
for covering emergency medical conditions. Under both state managed care organization statutes and state insurance laws, our health plan subsidiaries, as well as our specialty companies, must comply with minimum statutory capital requirements or other financial requirements, such as deposit and reserve requirements. Insurance regulations may also require prior state approval of acquisitions of other managed care organizations’ businesses and the payment of dividends, as well as notice
for loans or the transfer of funds. Our subsidiaries are also subject to periodic reporting requirements. In addition, each health plan and individual health insurance provider must meet criteria to secure the approval of state regulatory authorities before implementing operational changes, including the development of new product offerings and, in some states, the expansion of service areas.
States have adopted a number of regulations that may affect our business and results of operations. These regulations in certain states include:
|
Ÿ |
premium taxes or similar assessments; |
|
Ÿ |
stringent prompt-pay laws; |
|
Ÿ |
disclosure requirements regarding provider fee schedules and coding procedures; and |
|
Ÿ |
programs to monitor and supervise the activities and financial solvency of provider groups. |
State Contracts
In addition to being a licensed health maintenance organization, in order to be a Medicaid Managed Care organization in each of the states in which we operate, we must operate under a contract with the state’s Medicaid agency. States generally use either a formal proposal process, reviewing a number of bidders, or award individual
contracts to qualified applicants that apply for entry to the program. We receive monthly payments based on specified capitation rates determined on an actuarial basis. These rates differ by membership category and by state depending on the specific benefits and policies adopted by each state.
Our contracts with the states and regulatory provisions applicable to us generally set forth the requirements for operating in the Medicaid sector, including provisions relating to:
|
Ÿ eligibility, enrollment and disenrollment processes; |
Ÿ health education and wellness and prevention programs; | |
|
Ÿ covered services; |
Ÿ timeliness of claims payment; | |
|
Ÿ eligible providers; |
Ÿ financial standards; | |
|
Ÿ subcontractors; |
Ÿ safeguarding of member information; | |
|
Ÿ record-keeping and record retention; |
Ÿ fraud and abuse detection and reporting; | |
|
Ÿ periodic financial and informational reporting; |
Ÿ grievance procedures; and | |
|
Ÿ quality assurance; |
Ÿ organization and administrative systems. |
A health plan or individual health insurance providers’ compliance with these requirements is subject to monitoring by state regulators and by CMS. A health plan is also subject to periodic comprehensive quality assurance evaluations by a third-party reviewing organization and generally by the insurance department of the
jurisdiction that licenses the health plan. A health plan or individual health insurance provider must also submit reports to various regulatory agencies, including quarterly and annual statutory financial statements and utilization reports.
The table below sets forth the term of our state contracts and provides details regarding related renewal or extension and termination provisions as of December 31, 2009.
|
State Contract |
|
Expiration Date |
|
Renewal or Extension by the State |
Termination by the State | |
|
Arizona – Acute Care |
September 30, 2011 |
May be extended for up to two additional one-year terms. |
May be terminated for convenience or an event of default. | |||
|
Arizona – Behavioral Health |
June 30, 2010 |
Renewable through the state’s reprocurement process.1 |
May be terminated for convenience or an event of default. | |||
|
Arizona – Long-term Care |
September 30, 2010 |
May be extended for up to one additional year. |
May be terminated for convenience, an event of default or lack of funding. | |||
|
Arizona – Special Needs Plan (Medicare) |
December 31, 2010 |
Renewable annually for successive 12-month periods. |
May be terminated by an event of default. | |||
|
Florida – Medicaid & ABD |
August 31, 2012 |
Renewable through the state’s recertification process. |
May be terminated for an event of default or lack of federal funding. | |||
|
Georgia – Medicaid & CHIP |
June 30, 2010 |
Renewable for two additional one-year terms. |
May be terminated for an event of default or significant changes in circumstances. | |||
|
Indiana – Medicaid & CHIP |
December 31, 2010 |
Renewable through the state’s recertification process. 2 |
May be terminated for convenience or an event of default. | |||
|
Kansas – Behavioral Health |
June 30, 2010 |
May be extended for up to two additional one-year terms. |
May be terminated for cause, or without cause for lack of funding. | |||
|
Massachusetts – Commonwealth Care |
June 30, 2010 |
Renewable through the state’s recertification process. |
May be terminated for convenience or an event of default. | |||
|
Massachusetts – Commonwealth Care Bridge |
June 30, 2010 |
Renewable through the state’s recertification process. |
May be terminated for convenience or an event of default. | |||
|
Ohio – Medicaid & CHIP |
June 30, 2010 |
Renewable annually for successive 12-month periods. |
May be terminated for an event of default. | |||
|
Ohio – Aged, Blind or Disabled (ABD) |
June 30, 2010 |
Renewable annually for successive 12-month periods. |
May be terminated for an event of default. | |||
|
Ohio – Special Needs Plan (Medicare) |
December 31, 2010 |
Renewable annually for successive 12-month periods. |
May be terminated by an event of default. | |||
|
South Carolina – Medicaid & ABD |
March 31, 2010 |
Renewable for successive 24-month periods. |
May be terminated for convenience or an event of default. | |||
|
South Carolina – CHIP |
March 31, 2010 |
Renewable through the state’s recertification process. |
May be terminated for convenience, an event of default or lack of federal funding. | |||
|
Texas – Medicaid, CHIP & ABD |
August 31, 2010 |
May be extended for up to four additional years. |
May be terminated for convenience, an event of default or lack of federal funding. | |||
|
Texas – Exclusive Provider Organization (CHIP) |
August 31, 2010 |
Coverage for the CHIP members continues under the new CHIP Rural Service Area contract discussed below. 3 |
May be terminated upon any event of default or in the event of lack of state or federal funding. | |||
|
Texas – CHIP Rural Service Area |
August 31, 2013 |
May be extended for up to five additional years. 3 |
May be terminated upon any event of default or in the event of lack of state or federal funding. | |||
|
Texas – Foster Care |
August 31, 2010 |
May be extended for up to four and a half additional years. |
May be terminated for convenience, an event of default, or non-appropriation of funds. | |||
|
Texas – Special Needs Plan (Medicare) |
December 31, 2010 |
Renewable annually for successive 12-month periods. |
May be terminated by an event of default. | |||
|
Wisconsin – Medicaid, CHIP & ABD 4 |
December 31, 2011 |
Renewable through the state’s recertification process. 4 |
May be terminated if a change in state or federal laws, rules or regulations materially affects either party’s right or responsibilities or for an event of default or lack of funding. | |||
|
Wisconsin – Medicaid & CHIP 5 |
July 31, 2010 5 |
Subject to the state’s reprocurement process. 5 |
Subject to the state’s reprocurement process. 5 | |||
|
Wisconsin – Network Health Plan Subcontract |
December 31, 2011 |
Renews automatically for successive five-year terms. |
May be terminated upon two-years notice prior to the end of the then current term or if a change in state or federal laws, rules or regulations materially affects either party’s rights or responsibilities under the contract, or if Network Health Plan’s contract with the State is terminated. | |||
|
Wisconsin – Special Needs Plan (Medicare) |
December 31, 2010 |
Renewable annually for successive 12-month periods. |
May be terminated by an event of default. |
_________________________________________
1 The Arizona Behavioral Health contract renewal is currently in process under the state’s reprocurement process.
2 The Indiana Medicaid and CHIP contract is subject to a reprocurement process with a contract effective date of January 1, 2011.
3 The Texas CHIP Rural Service Area (RSA) contract covers CHIP members previously included under the Exclusive Provider Organization (EPO) contract. The CHIP RSA contract has a start date of September 1, 2010. Under the previous EPO contract,
we were the sole provider of services. Under the new RSA contract, members have the option to select either our plan or the new alternate plan provided by another carrier.
4 The current contract excludes coverage for Medicaid and CHIP members in six counties (Kenosha, Milwaukee, Ozaukee, Racine, Washington and Waukesha). The state has not yet determined the process for renewal and if it will require requalification or
a complete reprocurement submission.
5 The contract covers six counties carved out by the state for Medicaid and CHIP members (Kenosha, Milwaukee, Ozaukee, Racine, Washington and Waukesha). This contract extension is in place to cover members in these counties until the later of July 31,
2010 or at a date which the state has awarded membership under the reprocurement currently in process.
HIPAA and HITECH
In 1996, Congress enacted the Health Insurance Portability and Accountability Act of 1996, or HIPAA. The Act is designed to improve the portability and continuity of health insurance coverage and simplify the administration of health insurance claims. Among the main requirements of HIPAA are the “Administrative
Simplification” provisions which include: standards for processing health insurance claims and related transactions (Transactions Standards); requirements for protecting the privacy and security of medical records and other personal health information (Privacy Rule); and standards and specifications for safeguarding personal health information which is maintained, stored or transmitted in electronic format (Security Rule). The Health Information Technology for Economic and Clinical Health (HITECH)
Act, which was enacted as part of the American Reinvestment and Recovery Act of 2009, amended certain provisions of HIPAA and introduced new data security obligations for covered entities and their business associates. HITECH also mandates individual notification in instances of data breach, provides enhanced penalties for HIPAA violations, and grants enforcement authority to states’ Attorneys General in addition to the HHS Office of Civil Rights.
The Privacy Rule and HITECH regulations establish requirements to protect the privacy of medical records and other personal health information maintained and used by healthcare providers, health plans, healthcare clearinghouses, and their business associates. Among numerous other requirements, the privacy regulations:
|
· |
limit certain uses and disclosures of private health information, and require patient authorizations for such uses and disclosures of private health information; |
|
· |
guarantee patients the right to access their medical records and to know who else has accessed them; |
|
· |
limit most disclosure of health information to the minimum needed for the intended purpose; |
|
· |
establish procedures to ensure the protection of private health information; |
|
· |
authorize access to records by researchers and others; |
|
· |
establish requirements for breach notification; and |
|
· |
impose criminal and civil sanctions for improper uses or disclosures of health information. |
The Security Rule requires healthcare providers, health plans, healthcare clearinghouses, and their business associates to implement administrative, physical and technical safeguards to ensure the privacy and confidentiality of personal health information when it is electronically stored, maintained or transmitted, through such devices as
user authentication mechanisms and system activity audits. The HITECH Act established a federal requirement for notification when the security of personal health information is breached. In addition there is a patchwork of states laws that have been adopted to provide for, among other things, private rights of action for breaches of data security and mandatory notification to persons whose identifiable information is obtained without authorization.
The requirements of the Transactions Standards apply to certain healthcare related transactions conducted using “electronic media.” Since “electronic media” is defined broadly to include “transmissions that are physically moved from one location to another using magnetic tape, disk or compact disk media,”
many communications are considered to be electronically transmitted. Under HIPAA, health plans are required to have the capacity to accept and send all covered transactions in a standardized electronic format. Penalties can be imposed for failure to comply with these requirements.
The preemption provisions of HIPAA provide that the federal standards will not preempt state laws that are more stringent than the related federal requirements. In addition, the Secretary of HHS may grant exceptions allowing state laws to prevail if one or more of a number of conditions are met, including but not limited to the
following:
|
· |
the state law is necessary to prevent fraud and abuse associated with the provision of and payment for healthcare; |
|
· |
the state law is necessary to ensure appropriate state regulation of insurance and health plans; |
|
· |
the state law is necessary for state reporting on healthcare delivery or costs; or |
|
· |
the state law addresses controlled substances. |
We have implemented processes, policies and procedures to comply with HIPAA and HITECH, including administrative, technical and physical safeguards to prevent against electronic data breach, education and training for employees in specific practices designed to help ensure against unauthorized use or access to personal health information,
and training on procedures for reporting a suspected breach. In addition, our corporate privacy officer and health plan privacy officials serve as resources to employees to address any questions or concerns they may have.
Patients’ Rights Legislation
Although no federal legislation has been enacted, patients’ rights legislation is frequently proposed in Congress. If enacted, this type of legislation could expand our potential exposure to lawsuits and increase our regulatory compliance costs. Depending on the final form of any enacted patients’ rights
legislation, such legislation could, among other things, expose us to liability for economic and punitive damages for making determinations that deny benefits or delay beneficiaries’ receipt of benefits as a result of our medical necessity or other coverage determinations. We cannot predict when or whether patients’ rights legislation will be enacted into law or, if enacted, what final form such legislation might take.
Other Fraud and Abuse Laws
Investigating and prosecuting healthcare fraud and abuse became a top priority for law enforcement entities in the last decade. The focus of these efforts has been directed at participants in public government healthcare programs such as Medicaid. The laws and regulations relating to Medicaid fraud and abuse and the
contractual requirements applicable to health plans participating in these programs are complex and changing and may require substantial resources.
EMPLOYEES
As of December 31, 2009, we had approximately 3,900 employees. None of our employees are represented by a union. We believe our relationships with our employees are good.
EXECUTIVE OFFICERS OF THE REGISTRANT
The following table sets forth information regarding our executive officers, including their ages, at January 31, 2010:
|
Name |
|
Age |
|
Position |
|
Michael F. Neidorff |
|
67 |
|
Chairman and Chief Executive Officer |
|
Mark W. Eggert |
48 |
Executive Vice President, Health Plan Business Unit | ||
|
Carol E. Goldman |
|
52 |
|
Executive Vice President and Chief Administrative Officer |
|
Jason M. Harrold |
40 |
Senior Vice President, Specialty Business Unit | ||
|
Jesse N. Hunter |
34 |
Executive Vice President, Corporate Development | ||
|
Donald G. Imholz |
57 |
Executive Vice President and Chief Information Officer | ||
|
Edmund E. Kroll |
50 |
Senior Vice President, Finance and Investor Relations | ||
|
Frederick J. Manning |
62 |
Executive Vice President, Celtic Insurance Company | ||
|
William N. Scheffel |
|
56 |
|
Executive Vice President, Chief Financial Officer and Treasurer |
|
Jeffrey A. Schwaneke |
34 |
Vice President, Corporate Controller and Chief Accounting Officer | ||
|
Toni Simonetti |
53 |
Senior Vice President, Public Affairs | ||
|
Keith H. Williamson |
57 |
Senior Vice President, General Counsel and Secretary |
Michael F. Neidorff. Mr. Neidorff has served as our Chairman and Chief Executive Officer since May 2004. From May 1996 to May 2004, Mr. Neidorff served as President, Chief Executive Officer and as a member of our board of directors. From 1995 to 1996,
Mr. Neidorff served as a Regional Vice President of Coventry Corporation, a publicly-traded managed care organization, and as the President and Chief Executive Officer of one of its subsidiaries, Group Health Plan, Inc. From 1985 to 1995, Mr. Neidorff served as the President and Chief Executive Officer of Physicians Health Plan of Greater St. Louis, a subsidiary of United Healthcare Corp., a publicly-traded managed care organization now known as UnitedHealth Group Incorporated. Mr. Neidorff also serves
as a director of Brown Shoe Company, Inc., a publicly-traded footwear company with global operations.
Mark W. Eggert. Mr. Eggert has served as our Executive Vice President, Health Plan Business Unit since November 2007. From January 1999 to November 2007, Mr. Eggert served as the Associate Vice Chancellor and Deputy General Counsel at Washington University, where
he oversaw the legal affairs of the School of Medicine.
Carol E. Goldman. Ms. Goldman has served as Executive Vice President and Chief Administrative Officer since June 2007. From July 2002 to June 2007, she served as our Senior Vice President, Chief Administrative Officer. From September 2001 to July 2002,
Ms. Goldman served as our Plan Director of Human Resources. From 1998 to August 2001, Ms. Goldman was Human Resources Manager at Mallinckrodt Inc., a medical device and pharmaceutical company.
Jason M. Harrold. Mr. Harrold has served as our Senior Vice President, Specialty Business Unit since August 2009. He served as President of OptiCare from July 2000 to August 2009. From July 1996 to July 2000, Mr. Harrold held various positions of increasing
responsibility at OptiCare including Vice President of Operations and Chief Operating Officer.
Jesse N. Hunter. Mr. Hunter has served as our Executive Vice President, Corporate Development since April 2008. He served as our Senior Vice President, Corporate Development from April 2007 to April 2008. He served as our Vice President, Corporate Development
from December 2006 to April 2007. From October 2004 to December 2006, he served as our Vice President, Mergers & Acquisitions. From July 2003 until October 2004, he served as the Director of Mergers & Acquisitions and from February 2002 until July 2003, he served as the Manager of Mergers & Acquisitions.
Donald G. Imholz. Mr. Imholz has served as our Executive Vice President and Chief Information Officer since December 2009. Mr. Imholz served as our Senior Vice President and Chief Information Officer from September 2008 to December 2009. From January
2008 to September 2008, Mr. Imholz was an independent consultant working for clients across a variety of industries. From January 1975 to January 2008, Mr. Imholz was with The Boeing Company and served as Vice President of Information Technology from 2002 to January 2008. In that role, Mr. Imholz was responsible for all application development and support worldwide.
Edmund E. Kroll. Mr. Kroll has served as our Senior Vice President, Finance and Investor Relations since May 2007. From June 1997 to November 2006, Mr. Kroll served as Managing Director at Cowen and Company LLC, where his research coverage focused on the managed
care industry, including the Company.
Frederick J. Manning. Mr. Manning has served as our Executive Vice President, Celtic Insurance Company since July 2008. From 1978 to July 2008, Mr. Manning served as Chief Executive Officer and Chairman of the Board of Celtic Insurance Company.
William N. Scheffel. Mr. Scheffel has served as our Executive Vice President, Chief Financial Officer and Treasurer since May 2009. He served as our Executive Vice President, Specialty Business Unit from June 2007 to May 2009. From May 2005 to June 2007, he served
as our Senior Vice President, Specialty Business Unit. From December 2003 until May 2005, he served as our Senior Vice President and Controller. From July 2002 to October 2003, Mr. Scheffel was a partner with Ernst & Young LLP. From 1975 to July 2002, Mr. Scheffel was with Arthur Andersen LLP.
Jeffrey A. Schwaneke. Mr. Schwaneke has served as our Vice President, Corporate Controller since July 2008 and Chief Accounting Officer since September 2008. He previously served as Vice President, Controller and Chief Accounting Officer at Novelis Inc. from October
2007 to July 2008, and Assistant Corporate Controller from May 2006 to September 2007. Mr. Schwaneke served as Segment Controller for SPX Corporation from January 2005 to April 2006. Mr. Schwaneke served as Corporate Controller at Marley Cooling Technologies, a segment of SPX Corporation, from March 2004 to December 2004 and Director of Financial Reporting from November 2002 to February 2004.
Toni Simonetti. Ms. Simonetti has served as our Senior Vice President, Public Affairs since December 2009. She previously served as Vice President, Global Communications at GMAC Financial Services from July 2004 to June 2009. From December 1999 to September 2006,
Ms. Simonetti served as Executive Director, Financial Communications and Global Media Relations at General Motors Corporation.
Keith H. Williamson. Mr. Williamson has served as our Senior Vice President, General Counsel since November 2006 and as our Secretary since February 2007. From 1988 until November 2006, he served at Pitney Bowes Inc. in various legal and executive roles, the last
seven years as a Division President. Mr. Williamson also serves as a director of PPL Corporation, a publicly-traded energy and utility holding company.
Available Information
We are subject to the reporting and information requirements of the Securities Exchange Act of 1934, as amended (Exchange Act) and, as a result, we file periodic reports and other information with the Securities and Exchange Commission, or SEC. We make these filings available on our website free of charge, the URL of which is http://www.centene.com,
as soon as reasonably practicable after we electronically file such material with, or furnish it to, the SEC. The SEC maintains a website (http://www.sec.gov) that contains our annual, quarterly and current reports and other information we file electronically with the SEC. You can read and copy any materials we file with the SEC at the SEC’s Public Reference Room at 100 F Street, N.E., Room 1850, Washington, D.C. 20549. You may obtain information on the operation of the Public Reference
Room by calling the SEC at 1-800-SEC-0330. Information on our website does not constitute part of this Annual Report on Form 10-K.
FACTORS THAT MAY AFFECT FUTURE RESULTS AND THE
TRADING PRICE OF OUR COMMON STOCK
You should carefully consider the risks described below before making an investment decision. The trading price of our common stock could decline due to any of these risks, in which case you could lose all or part of your investment. You should also refer to the other information in this filing, including our consolidated
financial statements and related notes. The risks and uncertainties described below are those that we currently believe may materially affect our Company. Additional risks and uncertainties that we are unaware of or that we currently deem immaterial also may become important factors that affect our Company.
Risks Related to Being a Regulated Entity
Reduction in Medicaid, CHIP and ABD funding could substantially reduce our profitability.
Most of our revenues come from Medicaid, CHIP and ABD premiums. The base premium rate paid by each state differs, depending on a combination of factors such as defined upper payment limits, a member’s health status, age, gender, county or region, benefit mix and member eligibility categories. Future levels of Medicaid, CHIP and ABD
funding and premium rates may be affected by continuing government efforts to contain healthcare costs and may further be affected by state and federal budgetary constraints. Additionally, state and federal entities may make changes to the design of their Medicaid programs resulting in the cancellation or modification of these programs.
For example, in August 2007, the Centers for Medicare & Medicaid Services, or CMS, published a final rule regarding the estimation and recovery of improper payments made under Medicaid and CHIP. This rule requires a CMS contractor to sample selected states each year to estimate improper payments in Medicaid and CHIP and create national
and state specific error rates. States must provide information to measure improper payments in Medicaid and CHIP for managed care and fee-for-service. Each state will be selected for review once every three years for each program. States are required to repay CMS the federal share of any overpayments identified. CMS published a proposed rule on July 15, 2009 that would make certain changes to the previously published rule. Among other things, the proposed changes establish a process for appealing error determinations.
The changes will not become effective until the final rule is published. We cannot predict whether a final rule will become effective and if it does, what impact it will have on the states with which we have contracts.
The American Reinvestment and Recovery Act of 2009, which was signed into law on February 17, 2009, provides $87 billion in additional federal Medicaid funding for states’ Medicaid expenditures between October 1, 2008 and December 31, 2010. Under this Act, states meeting certain eligibility requirements will temporarily receive additional
money in the form of an increase in the federal medical assistance percentage (FMAP). Thus, for a limited period of time, the share of Medicaid costs that are paid for by the federal government will go up, and each state’s share will go down. We cannot predict whether states are, or will remain, eligible to receive the additional federal Medicaid funding, or whether the states will have sufficient funds for their Medicaid programs.
States also periodically consider reducing or reallocating the amount of money they spend for Medicaid, CHIP, Foster Care and ABD. The current adverse economic conditions have, and are expected to continue to, put pressures on state budgets as tax and other state revenues decrease while the Medicaid eligible population increases, creating
more need for funding. We anticipate this will require government agencies with whom we contract to find funding alternatives, which may result in reductions in funding for current programs and program expansions, contraction of covered benefits, limited or no premium rate increases or premium decreases. In recent years, the majority of states have implemented measures to restrict Medicaid, CHIP, Foster Care and ABD costs and eligibility. If any state in which we operate were to decrease premiums paid to us,
or pay us less than the amount necessary to keep pace with our cost trends, it could have a material adverse effect on our revenues and operating results.
Changes to Medicaid, CHIP, Foster Care and ABD programs could reduce the number of persons enrolled in or eligible for these programs, reduce the amount of reimbursement or payment levels, or increase our administrative or healthcare costs under these programs, all of which could have a negative impact on our business. We believe that reductions
in Medicaid, CHIP, Foster Care and ABD payments could substantially reduce our profitability. Further, our contracts with the states are subject to cancellation by the state after a short notice period in the event of unavailability of state funds.
If CHIP is not reauthorized or states face shortfalls, our business could suffer.
Federal support for CHIP has been authorized through 2013. We cannot be certain that CHIP will be reauthorized when current funding expires in 2013, and if it is, what changes might be made to the program following reauthorization. Thus, we cannot predict the impact that reauthorization will have on our business.
States receive matching funds from the federal government to pay for their CHIP programs, which matching funds have a per state annual cap. Because of funding caps, there is a risk that states could experience shortfalls in future years, which could have an impact on our ability to receive amounts owed to us from states in which we have CHIP
contracts.
If any of our state contracts are terminated or are not renewed, our business will suffer.
We provide managed care programs and selected services to individuals receiving benefits under federal assistance programs, including Medicaid, CHIP and ABD. We provide those healthcare services under contracts with regulatory entities in the areas in which we operate. Our contracts with various states are generally intended to run for one
or two years and may be extended for one or two additional years if the state or its agent elects to do so. Our current contracts are set to expire or renew between March 31, 2010 and August 31, 2013. When our contracts expire, they may be opened for bidding by competing healthcare providers. There is no guarantee that our contracts will be renewed or extended. For example, on August 25, 2006, we received notification from the Kansas Health Policy Authority that FirstGuard Health Plan Kansas, Inc.’s contract
with the State would not be renewed or extended, and as a result, our contract ended on December 31, 2006. Further, our contracts with the states are subject to cancellation by the state after a short notice period in the event of unavailability of state funds. For example, the Indiana contract under which we operate can be terminated by the State without cause. Our contracts could also be terminated if we fail to perform in accordance with the standards set by state regulatory agencies. If any of our contracts
are terminated, not renewed, renewed on less favorable terms, or not renewed on a timely basis, our business will suffer, and our financial position, results of operations or cash flows may be materially affected.
If we are unable to participate in CHIP programs, our growth rate may be limited.
CHIP is a federal initiative designed to provide coverage for low-income children not otherwise covered by Medicaid or other insurance programs. The programs vary significantly from state to state. Participation in CHIP programs is an important part of our growth strategy. If states do not allow us to participate or if we fail to win bids
to participate, our growth strategy may be materially and adversely affected.
Changes in government regulations designed to protect the financial interests of providers and members rather than our investors could force us to change how we operate and could harm our business.
Our business is extensively regulated by the states in which we operate and by the federal government. The applicable laws and regulations are subject to frequent change and generally are intended to benefit and protect the financial interests of health plan providers and members rather than investors. The enactment of new laws and rules
or changes to existing laws and rules or the interpretation of such laws and rules could, among other things:
• force us to restructure our relationships with providers within our network;
• require us to implement additional or different programs and systems;
• mandate minimum medical expense levels as a percentage of premium revenues;
• restrict revenue and enrollment growth;
• require us to develop plans to guard against the financial insolvency of our providers;
• increase our healthcare and administrative costs;
• impose additional capital and reserve requirements; and
• increase or change our liability to members in the event of malpractice by our providers.
For example, Congress is currently considering health care reform legislation. We cannot predict the impact of any such legislation, if adopted, on our business.
The pending health care reform legislation could harm our business.
Congress is currently considering legislation that could significantly reform the U.S. health care system. We cannot predict whether any legislation will be passed and if it is, what impact it will have on our business. If any reforms are implemented that reduce Medicaid or CHIP spending or the payments we receive from states or increase
taxes on HMOs or MCOs, our business could suffer.
Regulations may decrease the profitability of our health plans.
Certain states have enacted regulations which require us to maintain a minimum health benefits ratio, or establish limits on our profitability. Other states require us to meet certain performance and quality metrics in order to receive our full contractual revenue. In certain circumstances, our plans may be required to pay a rebate to the
state in the event profits exceed established levels. These regulatory requirements, changes in these requirements or the adoption of similar requirements by other regulators may limit our ability to increase our overall profits as a percentage of revenues. Certain states, including but not limited to Georgia, Indiana, New Jersey, Texas and Wisconsin have implemented prompt-payment laws and are enforcing penalty provisions for failure to pay claims in a timely manner. Failure to meet these requirements can result
in financial fines and penalties. In addition, states may attempt to reduce their contract premium rates if regulators perceive our health benefits ratio as too low. Any of these regulatory actions could harm our financial position, results of operations or cash flows. Certain states also impose marketing restrictions on us which may constrain our membership growth and our ability to increase our revenues.
We face periodic reviews, audits and investigations under our contracts with state government agencies, and these audits could have adverse findings, which may negatively impact our business.
We contract with various state governmental agencies to provide managed healthcare services. Pursuant to these contracts, we are subject to various reviews, audits and investigations to verify our compliance with the contracts and applicable laws and regulations. Any adverse review, audit or investigation could result in:
• cancellation of our contracts;
• refunding of amounts we have been paid pursuant to our contracts;
• imposition of fines, penalties and other sanctions on us;
• loss of our right to participate in various markets;
• increased difficulty in selling our products and services; and
• loss of one or more of our licenses.
Failure to comply with government regulations could subject us to civil and criminal penalties.
Federal and state governments have enacted fraud and abuse laws and other laws to protect patients’ privacy and access to healthcare. In some states, we may be subject to regulation by more than one governmental authority, which may impose overlapping or inconsistent regulations. Violation of these and other laws or regulations governing
our operations or the operations of our providers could result in the imposition of civil or criminal penalties, the cancellation of our contracts to provide services, the suspension or revocation of our licenses or our exclusion from participating in the Medicaid, CHIP, Foster Care and ABD programs. If we were to become subject to these penalties or exclusions as the result of our actions or omissions or our inability to monitor the compliance of our providers, it would negatively affect our ability to operate
our business.
HIPAA broadened the scope of fraud and abuse laws applicable to healthcare companies. HIPAA created civil penalties for, among other things, billing for medically unnecessary goods or services. HIPAA established new enforcement mechanisms to combat fraud and abuse, including civil and, in some instances, criminal penalties for failure to
comply with specific standards relating to the privacy, security and electronic transmission of most individually identifiable health information. The HITECH Act expanded the scope of these provisions by mandating individual notification in instances of data breach, providing enhanced penalties for HIPAA violations, and granting enforcement authority to states’ Attorneys General in addition to the HHS Office of Civil Rights. It is possible that Congress may enact additional legislation in the future to
increase penalties and to create a private right of action under HIPAA, which could entitle patients to seek monetary damages for violations of the privacy rules.
We may incur significant costs as a result of compliance with government regulations, and our management will be required to devote time to compliance.
Many aspects of our business are affected by government laws and regulations. The issuance of new regulations, or judicial or regulatory guidance regarding existing regulations, could require changes to many of the procedures we currently use to conduct our business, which may lead to additional costs that we have not yet identified. We do
not know whether, or the extent to which, we will be able to recover from the states our costs of complying with these new regulations. The costs of any such future compliance efforts could have a material adverse effect on our business. We have already expended significant time, effort and financial resources to comply with the privacy and security requirements of HIPAA and will have to expend additional time and financial resources to comply with the HIPAA provisions contained in the American Recovery and Reinvestment
Act of 2009. We cannot predict whether states will enact stricter laws governing the privacy and security of electronic health information. If any new requirements are enacted at the state or federal level, compliance would likely require additional expenditures and management time.
In addition, the Sarbanes-Oxley Act of 2002, as well as rules subsequently implemented by the SEC and the New York Stock Exchange, or the NYSE, have imposed various requirements on public companies, including requiring changes in corporate governance practices. Our management and other personnel will continue to devote time to these compliance
initiatives.
The Sarbanes-Oxley Act requires, among other things, that we maintain effective internal control over financial reporting. In particular, we must perform system and process evaluation and testing of our internal control over financial reporting to allow management to report on the effectiveness of our internal control over our financial reporting
as required by Section 404 of the Sarbanes-Oxley Act. Our testing, or the subsequent testing by our independent registered public accounting firm, may reveal deficiencies in our internal control over financial reporting that are deemed to be material weaknesses. Our compliance with Section 404 causes us to incur substantial expense and management effort. Moreover, if we are not able to comply with the requirements of Section 404, or if we or our independent registered public accounting firm identifies deficiencies
in our internal control over financial reporting that are deemed to be material weaknesses, the market price of our stock could decline and we could be subject to sanctions or investigations by the NYSE, SEC or other regulatory authorities, which would require additional financial and management resources.
Changes in healthcare law and benefits may reduce our profitability.
Numerous proposals relating to changes in healthcare law have been introduced, some of which have been passed by Congress and the states in which we operate or may operate in the future. Changes in applicable laws and regulations are continually being considered, and interpretations of existing laws and rules may also change from time to
time. We are unable to predict what regulatory changes may occur or what effect any particular change may have on our business. For example, these changes could reduce the number of persons enrolled or eligible to enroll in Medicaid, reduce the reimbursement or payment levels for medical services or reduce benefits included in Medicaid coverage. For example, some states, including Indiana and Ohio have removed, and others could consider removing, pharmacy coverage from the services covered by managed care entities.
We are also unable to predict whether new laws or proposals will favor or hinder the growth of managed healthcare in general. Legislation or regulations that require us to change our current manner of operation, benefits provided or our contract arrangements may seriously harm our operations and financial results.
If a state fails to renew a required federal waiver for mandated Medicaid enrollment into managed care or such application is denied, our membership in that state will likely decrease.
States may administer Medicaid managed care programs pursuant to demonstration programs or required waivers of federal Medicaid standards. Waivers and demonstration programs are generally approved for two year periods and can be renewed on an ongoing basis if the state applies. We have no control over this renewal process. If a state does
not renew such a waiver or demonstration program or the Federal government denies a state’s application for renewal, membership in our health plan in the state could decrease and our business could suffer.
Changes in federal funding mechanisms may reduce our profitability.
Changes in funding for Medicaid may affect our business. For example, on May 29, 2007, CMS issued a final rule that would reduce states’ use of intergovernmental transfers for the states’ share of Medicaid program funding. By restricting the use of intergovernmental transfers, this rule may restrict some states’ funding
for Medicaid, which could adversely affect our growth, operations and financial performance. On May 23, 2008, the United States District Court for the District of Columbia vacated the final rule as improperly promulgated. The American Recovery and Reinvestment Tax Act of 2009 indicates Congressional intent is that final regulations should not be promulgated. We cannot predict whether the rule will ever be finalized or otherwise implemented and if it is, what impact it will have on our business.
Legislative changes in the Medicare program may also affect our business. For example, the Medicare Prescription Drug, Improvement and Modernization Act of 2003 revised cost-sharing requirements for some beneficiaries and requires states to reimburse the federal Medicare program for costs of prescription drug coverage provided to beneficiaries
who are enrolled simultaneously in both the Medicaid and Medicare programs. In addition, the Medicare prescription drug benefit interrupted the distribution of prescription drugs to many beneficiaries simultaneously enrolled in both Medicaid and Medicare, prompting several states to pay for prescription drugs on an unbudgeted, emergency basis without any assurance of receiving reimbursement from the federal Medicaid program. These expenses may cause some states to divert funds originally intended for other Medicaid
services which could adversely affect our growth, operations and financial performance.
If state regulatory agencies require a statutory capital level higher than the state regulations, we may be required to make additional capital contributions.
Our operations are conducted through our wholly owned subsidiaries, which include health maintenance organizations, or HMOs, and managed care organizations, or MCOs. HMOs and MCOs are subject to state regulations that, among other things, require the maintenance of minimum levels of statutory capital, as defined by each state. Additionally,
state regulatory agencies may require, at their discretion, individual HMOs to maintain statutory capital levels higher than the state regulations. If this were to occur to one of our subsidiaries, we may be required to make additional capital contributions to the affected subsidiary. Any additional capital contribution made to one of the affected subsidiaries could have a material adverse effect on our liquidity and our ability to grow.
If state regulators do not approve payments of dividends and distributions by our subsidiaries to us, we may not have sufficient funds to implement our business strategy.
We principally operate through our health plan subsidiaries. If funds normally available to us become limited in the future, we may need to rely on dividends and distributions from our subsidiaries to fund our operations. These subsidiaries are subject to regulations that limit the amount of dividends and distributions that can be paid to
us without prior approval of, or notification to, state regulators. If these regulators were to deny our subsidiaries’ request to pay dividends to us, the funds available to us would be limited, which could harm our ability to implement our business strategy.
Risks Related to Our Business
Ineffectiveness of state-operated systems and subcontractors could adversely affect our business.
Our health plans rely on other state-operated systems or sub-contractors to qualify, solicit, educate and assign eligible members into the health plans. The effectiveness of these state operations and sub-contractors can have a material effect on a health plan’s enrollment in a particular month or over an extended period. When a state
implements new programs to determine eligibility, new processes to assign or enroll eligible members into health plans, or chooses new contractors, there is an increased potential for an unanticipated impact on the overall number of members assigned into the health plans.
Failure to accurately predict our medical expenses could negatively affect our financial position, results of operations or cash flows.
Our medical expense includes claims reported but not yet paid, or inventory, estimates for claims incurred but not reported, or IBNR, and estimates for the costs necessary to process unpaid claims at the end of each period. Our development of the medical claims liability estimate is a continuous process which we monitor and refine on a monthly
basis as claims receipts and payment information becomes available. As more complete information becomes available, we adjust the amount of the estimate, and include the changes in estimates in medical expense in the period in which the changes are identified.
We can not be sure that our medical claims liability estimates are adequate or that adjustments to those
estimates will not unfavorably impact our results of operations. For example, in the three months ended June 30, 2006 we adjusted IBNR by $9.7 million for adverse medical costs development from the first quarter of 2006.
Additionally, when we commence operations in a new state or region, we have limited information with which to estimate our medical claims liability. For example, we commenced operations in South Carolina in December 2007, began our Foster Care program in Texas in April 2008, commenced operations in Florida in February 2009 and in Massachusetts
in July 2009, and expect to commence operations in Mississippi in 2010. For a period of time after the inception of business in these states, we base our estimates on state-provided historical actuarial data and limited actual incurred and received claims.
From time to time in the past, our actual results have varied from our estimates, particularly in times of significant changes in the number of our members. The accuracy of our medical claims liability estimate may also affect our ability to take timely corrective actions, further harming our results.
Receipt of inadequate or significantly delayed premiums would negatively affect our revenues and profitability.
Our premium revenues consist of fixed monthly payments per member and supplemental payments for other services such as maternity deliveries. These premiums are fixed by contract, and we are obligated during the contract periods to provide healthcare services as established by the state governments. We use a large portion of our revenues to
pay the costs of healthcare services delivered to our members. If premiums do not increase when expenses related to medical services rise, our earnings will be affected negatively. In addition, our actual medical services costs may exceed our estimates, which would cause our health benefits ratio, or our expenses related to medical services as a percentage of premium revenue, to increase and our profits to decline. In addition, it is possible for a state to increase the rates payable to the hospitals without
granting a corresponding increase in premiums to us. If this were to occur in one or more of the states in which we operate, our profitability would be harmed. In addition, if there is a significant delay in our receipt of premiums to offset previously incurred health benefits costs, our earnings could be negatively impacted.
In some instances, our base premiums are subject to an adjustment, or risk score, based on the acuity of our membership. Generally, the risk score is determined by the State analyzing encounter submissions of processed claims data to determine the acuity of our membership relative to the entire state’s Medicaid membership. The risk
score is dependent on several factors including our providers’ completeness and quality of claims submission, our processing of the claim, submission of the processed claims in the form of encounters to the states’ encounter systems and the states’ acceptance and analysis of the encounter data. If the risk scores assigned to our premiums that are risk adjusted are not adequate or do not appropriately reflect the acuity of our membership, our earnings will be affected negatively.
Failure to effectively manage our medical costs or related administrative costs or uncontrollable epidemic or pandemic costs would reduce our profitability.
Our profitability depends, to a significant degree, on our ability to predict and effectively manage expenses related to health benefits. We have less control over the costs related to medical services than we do over our general and administrative expenses. Because of the narrow margins of our health plan business, relatively small changes
in our health benefits ratio can create significant changes in our financial results. Changes in healthcare regulations and practices, the level of use of healthcare services, hospital costs, pharmaceutical costs, major epidemics or pandemics, new medical technologies and other external factors, including general economic conditions such as inflation levels, are beyond our control and could reduce our ability to predict and effectively control the costs of providing health benefits. In 2009, the H1N1 influenza
pandemic resulted in heightened costs due to increased physician visits and increased utilization of hospital emergency rooms and pharmaceutical costs. We cannot predict what impact the H1N1 influenza virus or any other epidemic or pandemic will have on our costs in the future. Additionally, we may not be able to manage costs effectively in the future. If our costs related to health benefits increase, our profits could be reduced or we may not remain profitable.
Our investment portfolio may suffer losses from reductions in market interest rates and changes in market conditions which could materially and adversely affect our results of operations or liquidity.
As of December 31, 2009, we had $440.5 million in cash, cash equivalents and short-term investments and $545.6 million of long-term investments and restricted deposits. We maintain an investment portfolio of cash equivalents and short-term and long-term investments in a variety
of securities which may include asset backed securities, bank deposits, commercial paper, certificates of deposit, money market funds, municipal bonds, corporate bonds, instruments of the U.S. Treasury, insurance contracts and equity securities. These investments are subject to general credit, liquidity, market and interest rate risks. Substantially all of these securities are subject to interest rate and credit risk and will decline in value if interest rates increase or one of the issuers’ credit ratings
is reduced. As a result, we may experience a reduction in value or loss of liquidity of our investments, which may have a negative adverse effect on our results of operations, liquidity and financial condition. For example, in the third quarter of 2008, we recorded a loss on investments of approximately $4.5 million due to a loss in a money market fund.
Our investments in state and municipal securities are not guaranteed by the United States government which could materially and adversely affect our results of operations or liquidity.
As of December 31, 2009, we had $345.6 million of investments in state and municipal securities. These securities are not guaranteed by the United States government. State and municipal securities are subject to additional credit risk based upon each local municipality’s
tax revenues and financial stability. As a result, we may experience a reduction in value or loss of liquidity of our investments, which may have a negative adverse effect on our results of operations, liquidity and financial condition.
Difficulties in executing our acquisition strategy could adversely affect our business.
Historically, the acquisition of Medicaid and specialty services businesses, contract rights and related assets of other health plans both in our existing service areas and in new markets has accounted for a significant amount of our growth. Many of the other potential purchasers have greater financial resources than we have. In addition,
many of the sellers are interested either in (a) selling, along with their Medicaid assets, other assets in which we do not have an interest or (b) selling their companies, including their liabilities, as opposed to the assets of their ongoing businesses.
We generally are required to obtain regulatory approval from one or more state agencies when making acquisitions. In the case of an acquisition of a business located in a state in which we do not currently operate, we would be required to obtain the necessary licenses to operate in that state. In addition, even if we already operate in a
state in which we acquire a new business, we would be required to obtain additional regulatory approval if the acquisition would result in our operating in an area of the state in which we did not operate previously, and we could be required to renegotiate provider contracts of the acquired business. We cannot provide any assurance that we would be able to comply with these regulatory requirements for an acquisition in a timely manner, or at all. In deciding whether to approve a proposed acquisition, state regulators
may consider a number of factors outside our control, including giving preference to competing offers made by locally owned entities or by not-for-profit entities.
We also may be unable to obtain sufficient additional capital resources for future acquisitions. If we are unable to effectively execute our acquisition strategy, our future growth will suffer and our results of operations could be harmed.
Execution of our growth strategy may increase costs or liabilities, or create disruptions in our business.
We pursue acquisitions of other companies or businesses from time to time. Although we review the records of companies or businesses we plan to acquire, even an in-depth review of records may not reveal existing or potential problems or permit us to become familiar enough with a business to assess fully its capabilities and deficiencies.
As a result, we may assume unanticipated liabilities or adverse operating conditions, or an acquisition may not perform as well as expected. We face the risk that the returns on acquisitions will not support the expenditures or indebtedness incurred to acquire such businesses, or the capital expenditures needed to develop such businesses. We also face the risk that we will not be able to integrate acquisitions into our existing operations effectively without substantial expense, delay or other operational or
financial problems. Integration may be hindered by, among other things, differing procedures, including internal controls, business practices and technology systems. We may need to divert more management resources to integration than we planned, which may adversely affect our ability to pursue other profitable activities.
In addition to the difficulties we may face in identifying and consummating acquisitions, we will also be required to integrate and consolidate any acquired business or assets with our existing operations. This may include the integration of:
• additional personnel who are not familiar with our operations and corporate culture;
• provider networks that may operate on different terms than our existing networks;
• existing members, who may decide to switch to another healthcare plan; and
• disparate administrative, accounting and finance, and information systems.
Additionally, our growth strategy includes start-up operations in new markets or new products in existing markets. We may incur significant expenses prior to commencement of operations and the receipt of revenue. As a result, these start-up operations may decrease our profitability. In the event we pursue any opportunity to diversify our
business internationally, we would become subject to additional risks, including, but not limited to, political risk, an unfamiliar regulatory regime, currency exchange risk and exchange controls, cultural and language differences, foreign tax issues, and different labor laws and practices.
Accordingly, we may be unable to identify, consummate and integrate future acquisitions or start-up
operations successfully or operate acquired or new businesses profitably.
Acquisitions of unfamiliar new businesses could negatively impact our business.
We are subject to the expenditures and risks associated with entering into any new line of business. Our failure to properly manage these expenditures and risks could have a negative impact on our overall business. For example, effective July 2008, we completed the previously announced acquisition of Celtic Group, Inc., the parent company
of Celtic Insurance Company, or Celtic. Celtic is a national individual health insurance provider that provides health insurance to individual customers and their families. While we believe that the addition of Celtic will be complementary to our business, we have not previously operated in the individual health care industry.
If competing managed care programs are unwilling to purchase specialty services from us, we may not be able to successfully implement our strategy of diversifying our business lines.
We are seeking to diversify our business lines into areas that complement our Medicaid business in order to grow our revenue stream and balance our dependence on Medicaid risk reimbursement. In order to diversify our business, we must succeed in selling the services of our specialty subsidiaries not only to our managed care plans, but to
programs operated by third-parties. Some of these third-party programs may compete with us in some markets, and they therefore may be unwilling to purchase specialty services from us. In any event, the offering of these services will require marketing activities that differ significantly from the manner in which we seek to increase revenues from our Medicaid programs. Our inability to market specialty services to other programs may impair our ability to execute our business strategy.
Failure to achieve timely profitability in any business would negatively affect our results of operations.
Start-up costs associated with a new business can be substantial. For example, in order to obtain a certificate of authority in most jurisdictions, we must first establish a provider network, have systems in place and demonstrate our ability to obtain a state contract and process claims. If we were unsuccessful in obtaining the necessary
license, winning the bid to provide service or attracting members in numbers sufficient to cover our costs, any new business of ours would fail. We also could be obligated by the state to continue to provide services for some period of time without sufficient revenue to cover our ongoing costs or recover start-up costs. The expenses associated with starting up a new business could have a significant impact on our results of operations if we are unable to achieve profitable operations in a timely fashion.
Adverse credit market conditions may have a material adverse affect on our liquidity or our ability to obtain credit on acceptable terms.
The securities and credit markets have been experiencing extreme volatility and disruption over the past several years. The availability of credit, from virtually all types of lenders, has been restricted. Such conditions may persist throughout 2010 and beyond. In the event we need access to additional capital to pay our operating expenses,
make payments on our indebtedness, pay capital expenditures, including costs related to our corporate headquarters’ project, or fund acquisitions, our ability to obtain such capital may be limited and the cost of any such capital may be significant, particularly if we are unable to access our existing credit facility.
Our access to additional financing will depend on a variety of factors such as prevailing economic and credit market conditions, the general availability of credit, the overall availability of credit to our industry, our credit ratings and credit capacity, and perceptions of our financial prospects. Similarly, our access to funds may be impaired
if regulatory authorities or rating agencies take negative actions against us. If a combination of these factors were to occur, our internal sources of liquidity may prove to be insufficient, and in such case, we may not be able to successfully obtain additional financing on favorable terms or at all. We believe that if credit could be obtained, the terms and costs of such credit could be significantly less favorable to us than what was obtained in our most recent financings.
We derive a majority of our premium revenues from operations in a small number of states, and our financial position, results of operations or cash flows would be materially affected by a decrease in premium revenues or profitability in any one of those states.
Operations in a few states have accounted for most of our premium revenues to date. If we were unable to continue to operate in any of our current states or if our current operations in any portion of one of those states were significantly curtailed, our revenues could decrease materially. Our Medicaid contract with Kansas, which terminated
December 31, 2006, together with our Medicaid contract with Missouri, accounted for $317.0 million in revenue for the year ended December 31, 2006. Our reliance on operations in a limited number of states could cause our revenue and profitability to change suddenly and unexpectedly depending on legislative or other governmental or regulatory actions and decisions, economic conditions and similar factors in those states. For example, states we currently serve may bid out their Medicaid program through a Request
for Proposal, or RFP, process. Our inability to continue to operate in any of the states in which we operate would harm our business.
Competition may limit our ability to increase penetration of the markets that we serve.
We compete for members principally on the basis of size and quality of provider network, benefits provided and quality of service. We compete with numerous types of competitors, including other health plans and traditional state Medicaid programs that reimburse providers as care is provided. In addition, current focus on health care reform
and potential growth in our segment may attract new competitors. Subject to limited exceptions by federally approved state applications, the federal government requires that there be choices for Medicaid recipients among managed care programs. Voluntary programs, increases in the number of competitors and mandated competition may limit our ability to increase our market share.
Some of the health plans with which we compete have greater financial and other resources and offer a broader scope of products than we do. In addition, significant merger and acquisition activity has occurred in the managed care industry, as well as in industries that act as suppliers to us, such as the hospital, physician, pharmaceutical,
medical device and health information systems businesses. To the extent that competition intensifies in any market that we serve, our ability to retain or increase members and providers, or maintain or increase our revenue growth, pricing flexibility and control over medical cost trends may be adversely affected.
In addition, in order to increase our membership in the markets we currently serve, we believe that we must continue to develop and implement community-specific products, alliances with key providers and localized outreach and educational programs. If we are unable to develop and implement these initiatives, or if our competitors are more
successful than we are in doing so, we may not be able to further penetrate our existing markets.
If we are unable to maintain relationships with our provider networks, our profitability may be harmed.
Our profitability depends, in large part, upon our ability to contract favorably with hospitals, physicians and other healthcare providers. Our provider arrangements with our primary care physicians, specialists and hospitals generally may be cancelled by either party without cause upon 90 to 120 days prior written notice. We cannot provide
any assurance that we will be able to continue to renew our existing contracts or enter into new contracts enabling us to service our members profitably.
From time to time providers assert or threaten to assert claims seeking to terminate non-cancelable agreements due to alleged actions or inactions by us. Even if these allegations represent attempts to avoid or renegotiate contractual terms that have become economically disadvantageous to the providers, it is possible that in the future a
provider may pursue such a claim successfully. In addition, we are aware that other managed care organizations have been subject to class action suits by physicians with respect to claim payment procedures, and we may be subject to similar claims. Regardless of whether any claims brought against us are successful or have merit, they will still be time-consuming and costly and could distract our management’s attention. As a result, we may incur significant expenses and may be unable to operate our business
effectively.
We will be required to establish acceptable provider networks prior to entering new markets. We may be unable to enter into agreements with providers in new markets on a timely basis or under favorable terms. If we are unable to retain our current provider contracts or enter into new provider contracts timely or on favorable terms, our profitability
will be harmed.
We may be unable to attract and retain key personnel.
We are highly dependent on our ability to attract and retain qualified personnel to operate and expand our business. If we lose one or more members of our senior management team, including our chief executive officer, Michael F. Neidorff, who has been instrumental in developing our business strategy and forging our business relationships,
our business and financial position, results of operations or cash flows could be harmed. Our ability to replace any departed members of our senior management or other key employees may be difficult and may take an extended period of time because of the limited number of individuals in the Medicaid managed care and specialty services industry with the breadth of skills and experience required to operate and successfully expand a business such as ours. Competition to hire from this limited pool is intense, and
we may be unable to hire, train, retain or motivate these personnel.
Negative publicity regarding the managed care industry may harm our business and financial position, results of operations or cash flows.
The managed care industry has received negative publicity. This publicity has led to increased legislation, regulation, review of industry practices and private litigation in the commercial sector. These factors may adversely affect our ability to market our services, require us to change our services, and increase the regulatory burdens
under which we operate. Any of these factors may increase the costs of doing business and adversely affect our financial position, results of operations or cash flows.
Claims relating to medical malpractice could cause us to incur significant expenses.
Our providers and employees involved in medical care decisions may be subject to medical malpractice claims. In addition, some states, including Texas, have adopted legislation that permits managed care organizations to be held liable for negligent treatment decisions or benefits coverage determinations. Claims of this nature, if successful,
could result in substantial damage awards against us and our providers that could exceed the limits of any applicable insurance coverage. Therefore, successful malpractice or tort claims asserted against us, our providers or our employees could adversely affect our financial condition and profitability. Even if any claims brought against us are unsuccessful or without merit, they would still be time consuming and costly and could distract our management’s attention. As a result, we may incur significant
expenses and may be unable to operate our business effectively.
Loss of providers due to increased insurance costs could adversely affect our business.
Our providers routinely purchase insurance to help protect themselves against medical malpractice claims. In recent years, the costs of maintaining commercially reasonable levels of such insurance have increased dramatically, and these costs are expected to increase to even greater levels in the future. As a result of the level of these costs,
providers may decide to leave the practice of medicine or to limit their practice to certain areas, which may not address the needs of Medicaid participants. We rely on retaining a sufficient number of providers in order to maintain a certain level of service. If a significant number of our providers exit our provider networks or the practice of medicine generally, we may be unable to replace them in a timely manner, if at all, and our business could be adversely affected.
Growth in the number of Medicaid-eligible persons during economic downturns could cause our financial position, results of operations or cash flows to suffer if state and federal budgets decrease or do not increase.
Less favorable economic conditions may cause our membership to increase as more people become eligible to receive Medicaid benefits. During such economic downturns, however, state and federal budgets could decrease, causing states to attempt to cut healthcare programs, benefits and rates. We cannot predict the impact of changes in the United
States economic environment or other economic or political events, including acts of terrorism or related military action, on federal or state funding of healthcare programs or on the size of the population eligible for the programs we operate. If federal funding decreases or remains unchanged while our membership increases, our results of operations will suffer.
Growth in the number of Medicaid-eligible persons may be countercyclical, which could cause our financial position, results of operations or cash flows to suffer when general economic conditions are improving.
Historically, the number of persons eligible to receive Medicaid benefits has increased more rapidly during periods of rising unemployment, corresponding to less favorable general economic conditions. Conversely, this number may grow more slowly or even decline if economic conditions improve. Therefore, improvements in general economic conditions
may cause our membership levels to decrease, thereby causing our financial position, results of operations or cash flows to suffer, which could lead to decreases in our stock price during periods in which stock prices in general are increasing.
If we are unable to integrate and manage our information systems effectively, our operations could be disrupted.
Our operations depend significantly on effective information systems. The information gathered and processed by our information systems assists us in, among other things, monitoring utilization and other cost factors, processing provider claims, and providing data to our regulators. Our providers also depend upon our information systems for
membership verifications, claims status and other information.
Our information systems and applications require continual maintenance, upgrading and enhancement to meet our operational needs and regulatory requirements. Moreover, our acquisition activity requires frequent transitions to or from, and the integration of, various information systems. We regularly upgrade and expand our information systems’
capabilities. If we experience difficulties with the transition to or from information systems or are unable to properly maintain or expand our information systems, we could suffer, among other things, from operational disruptions, loss of existing members and difficulty in attracting new members, regulatory problems and increases in administrative expenses. In addition, our ability to integrate and manage our information systems may be impaired as the result of events outside our control, including acts of nature,
such as earthquakes or fires, or acts of terrorists.
We rely on the accuracy of eligibility lists provided by state governments. Inaccuracies in those lists would negatively affect our results of operations.
Premium payments to us are based upon eligibility lists produced by state governments. From time to time, states require us to reimburse them for premiums paid to us based on an eligibility list that a state later discovers contains individuals who are not in fact eligible for a government sponsored program or are eligible for a different
premium category or a different program. Alternatively, a state could fail to pay us for members for whom we are entitled to payment. Our results of operations would be adversely affected as a result of such reimbursement to the state if we had made related payments to providers and were unable to recoup such payments from the providers.
We may not be able to obtain or maintain adequate insurance.
We maintain liability insurance, subject to limits and deductibles, for claims that could result from providing or failing to provide managed care and related services. These claims could be substantial. We believe that our present insurance coverage and reserves are adequate to cover currently estimated exposures. We cannot provide any assurance
that we will be able to obtain adequate insurance coverage in the future at acceptable costs or that we will not incur significant liabilities in excess of policy limits.
From time to time, we may become involved in costly and time-consuming litigation and other regulatory proceedings, which require significant attention from our management.
We are a defendant from time to time in lawsuits and regulatory actions relating to our business. Due to the inherent uncertainties of litigation and regulatory proceedings, we cannot accurately predict the ultimate outcome of any such proceedings. An unfavorable outcome could have a material adverse impact on our business and financial position,
results of operations or cash flows. In addition, regardless of the outcome of any litigation or regulatory proceedings, such proceedings are costly and time consuming and require significant attention from our management. For example, we have in the past, or may be subject to in the future, securities class action lawsuits, IRS examinations or similar regulatory actions. Any such matters could harm our business and financial position, results of operations or cash flows.
An unauthorized disclosure of sensitive or confidential member information could have an adverse effect on our business.
As part of our normal operations, we collect, process and retain confidential member information. We are subject to various federal and state laws and rules regarding the use and disclosure of confidential member information, including HIPAA and the Gramm-Leach-Bliley Act. The American Recovery and Reinvestment Act of 2009 further expands
the coverage of HIPAA by, among other things, extending the privacy and security provisions, requiring new disclosures if a data breach occurs, mandating new regulations around electronic medical records, expanding enforcement mechanisms, allowing the state Attorneys General to bring enforcement actions and increasing penalties for violations. Despite the security measures we have in place to ensure compliance with applicable laws and rules, our facilities and systems, and those of our third party service providers,
may be vulnerable to security breaches, acts of vandalism, computer viruses, misplaced or lost data, programming and/or human errors or other similar events. Any security breach involving the misappropriation, loss or other unauthorized disclosure or use of confidential member information, whether by us or a third party, could have a material adverse effect on our business, financial condition, cash flows, or results of operations.
If we are unable to complete the previously announced sale of certain assets of our New Jersey health plan in a timely manner, our business could suffer.
On November 20, 2008, we announced that we had entered into an agreement with Amerigroup Corporation, or Amerigroup, to sell certain assets of our subsidiary University Health Plans, Inc. in the State of New Jersey to Amerigroup. The agreement contains a number of conditions to closing, including (i) the approval of regulators in New Jersey,
(ii) the lack of a material adverse effect, and (iii) other customary conditions. On December 31, 2008, we announced that we had received a termination notice from Amerigroup relating to the New Jersey transaction. On October 23, 2009, we entered into a settlement agreement with Amerigroup resolving all claims, and expect to complete the sale in the first quarter of 2010. However, if we are unable to complete the sale of our New Jersey business, our results of operations could be negatively impacted.
Risks related to our corporate headquarters’ project could harm our financial position, results of operations or cash flows.
In 2008 and 2009, our capital expenditures included costs associated with the construction of a real estate development on the property adjoining our corporate office, which we believe is necessary to accommodate our growing business. We are currently a joint venture partner in an entity that is developing the properties. If the entity is
unable to complete the development or if the entity delays or abandons the real estate project, it may have an adverse impact on our financial position, results of operations or cash flows. For example, in 2007 we abandoned a previously planned redevelopment project and recorded a pre-tax impairment charge of $7.2 million. Our operations and efficiency could also be impacted if the development is not completed as there is limited office space for us to expand in the market near our existing headquarters as our
business continues to grow.
None.
We own our corporate office headquarters building located in St. Louis, Missouri. During 2008 and 2009, our capital expenditures included costs for the construction of a new real estate development on the property adjoining our corporate office, which we believe is necessary to accommodate our growing business.
We generally lease space in the states where our health plans, specialty companies and claims processing facilities operate. We are required by various insurance and regulatory authorities to have offices in the service areas where we provide benefits. We believe our current facilities are adequate to meet our operational
needs for the foreseeable future.
In May 2008, the Internal Revenue Service, or IRS, began an audit of our 2006 and 2007 tax returns. As a result of this audit, the IRS has initially denied the $34.9 million tax benefit we recognized for the abandonment of the FirstGuard stock in 2007. We are proceeding with the appeals process and believe that it is
more likely than not that our tax position will be upheld. Accordingly, we have not made any adjustments to our reserve for uncertain tax positions related to this issue.
We routinely are subjected to legal proceedings in the normal course of business. While the ultimate resolution of such matters is uncertain, we do not expect the results of any of these matters individually, or in the aggregate, to have a material effect on our financial position or results of operations.
None.
PART II
Item 5. Market for Registrant’s Common Equity, Related Stockholder Matters and Issuer
Purchases of Equity Securities
Market for Common Stock; Dividends
Our common stock has been traded and quoted on the New York Stock Exchange under the symbol “CNC” since October 16, 2003.
|
|
2009 Stock Price |
|
2008 Stock Price | |||||||||
|
|
High |
|
Low |
|
High |
|
Low | |||||
|
First Quarter |
|
$ |
22.50 |
|
$ |
15.00 |
|
$ |
28.49 |
|
$ |
13.58 |
|
Second Quarter |
|
21.00 |
|
17.29 |
|
21.70 |
|
13.10 | ||||
|
Third Quarter |
|
20.48 |
|
16.89 |
|
24.67 |
|
16.40 | ||||
|
Fourth Quarter |
|
22.02 |
|
17.25 |
|
21.61 |
|
15.23 | ||||
As of February 5, 2010, there were 55 holders of record of our common stock.
We have never declared any cash dividends on our capital stock and currently anticipate that we will retain any future earnings for the development, operation and expansion of our business.
Issuer Purchases of Equity Securities
On October 26, 2009, the Company’s Board of Directors extended the Company’s stock repurchase program. The program authorizes the repurchase of up to 4,000,000 shares of the Company’s common stock from time to time on the open market or through privately negotiated transactions. No duration has been
placed on the repurchase program and the Company reserves the right to discontinue the repurchase program at any time. During the year ended December 31, 2009, we repurchased 332,595 shares at an aggregate cost of $6.3 million. During the quarter ended December 31, 2009, with the exception of the 40,117 shares footnoted below, we did not repurchase any shares other than through this publicly announced program.
|
Issuer Purchases of Equity Securities
Fourth Quarter 2009 | |||||||||||
|
Period |
Total Number of Shares Purchased |
Average Price Per Share |
Total Number of Shares
Purchased as Part of Publicly
Announced Plans or Programs |
Maximum Number of Shares
that May Yet Be Purchased Under
the Plans or Programs | |||||||
|
October 1 – October 31, 2009 |
299 |
$ |
18.65 |
— |
1,667,724 | ||||||
|
November 1 – November 30, 2009 |
4,869 |
18.29 |
— |
1,667,724 | |||||||
|
December 1 – December 31, 2009 |
34,949 |
19.17 |
— |
1,667,724 | |||||||
|
TOTAL |
|
40,117 |
1 |
$ |
19.06 |
|
— |
1,667,724 | |||
________________
1 Shares acquired represent shares relinquished to the Company by certain employees for payment of taxes upon vesting of restricted stock units.
Stock Performance Graphs
The graph below compares the cumulative total stockholder return on our common stock for the period from December 31, 2004 to December 31, 2009 with the cumulative total return of the New York Stock Exchange Composite Index and the Morgan Stanley Health Care Payor Index over the same period. The graph assumes an investment of $100
on December 31, 2004 in our common stock (at the last reported sale price on such day), the New York Stock Exchange Composite Index and the Morgan Stanley Health Care Payor Index and assumes the reinvestment of any dividends.
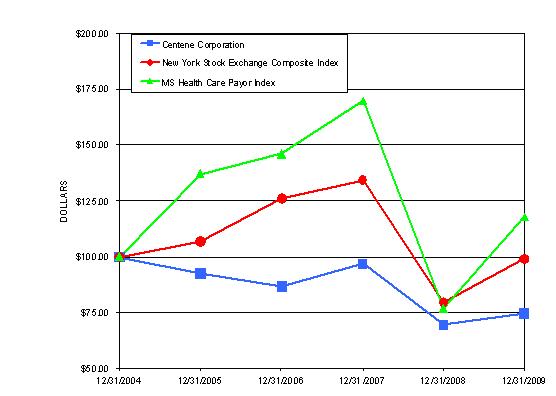
|
12/31/2004 |
12/31/2005 |
12/31/2006 |
12/31/2007 |
12/31/2008 |
12/31/2009 | |
|
Centene Corporation |
$ 100.00 |
$ 92.73 |
$ 86.67 |
$ 96.79 |
$ 69.52 |
$ 74.67 |
|
New York Stock Exchange Composite Index |
$ 100.00 |
$ 106.95 |
$ 126.05 |
$ 134.35 |
$ 79.41 |
$ 99.10 |
|
MS Health Care Payor Index |
$ 100.00 |
$ 137.12 |
$ 146.24 |
$ 169.92 |
$ 76.79 |
$ 117.80 |
Item 6. Selected Financial Data
The following selected consolidated financial data should be read in conjunction with the consolidated financial statements and related notes and “Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations” included in our Annual Report on Form 10-K. The assets, liabilities and
results of operations of FirstGuard and University Health Plans have been classified as discontinued operations for all periods presented. The data for the years ended December 31, 2009, 2008 and 2007 and as of December 31, 2009 and 2008 are derived from consolidated financial statements included elsewhere in this filing. The data for the years ended December 31, 2006 and 2005 and as of December 31, 2007, 2006 and 2005 are derived from consolidated financial statements not included in this
filing.
|
|
Year Ended December 31, |
|||||||||||||||||||
|
|
2009 |
2008 |
2007 |
20061 |
2005 |
|||||||||||||||
|
(In thousands, except share data) |
||||||||||||||||||||
|
|
||||||||||||||||||||
|
Revenues: |
|
|||||||||||||||||||
|
Premium |
|
$ |
3,786,525 |
$ |
3,199,360 |
$ |
2,611,953 |
$ |
1,707,439 |
$ |
1,095,308 |
|||||||||
|
Service |
|
91,758 |
74,953 |
80,508 |
79,159 |
13,456 |
||||||||||||||
|
Premium and service revenues |
3,878,283 |
3,274,313 |
2,692,461 |
1,786,598 |
1,108,764 |
|||||||||||||||
|
Premium tax |
224,581 |
90,202 |
76,567 |
35,848 |
6,079 |
|||||||||||||||
|
Total revenues |
|
4,102,864 |
3,364,515 |
2,769,028 |
1,822,446 |
1,114,843 |
||||||||||||||
|
Expenses: |
|
|||||||||||||||||||
|
Medical costs |
|
3,163,523 |
2,640,335 |
2,190,898 |
1,436,371 |
897,077 |
||||||||||||||
|
Cost of services |
|
60,789 |
56,920 |
61,348 |
60,287 |
5,608 |
||||||||||||||
|
General and administrative expenses |
|
514,529 |
444,733 |
384,970 |
267,712 |
162,432 |
||||||||||||||
|
Premium tax expense |
225,888 |
90,966 |
76,567 |
35,848 |
6,079 |
|||||||||||||||
|
Total operating expenses |
|
3,964,729 |
3,232,954 |
2,713,783 |
1,800,218 |
1,071,196 |
||||||||||||||
|
Earnings from operations |
|
138,135 |
131,561 |
55,245 |
22,228 |
43,647 |
||||||||||||||
|
Other income (expense): |
|
|||||||||||||||||||
|
Investment and other income |
|
15,691 |
21,728 |
24,452 |
15,511 |
8,417 |
||||||||||||||
|
Interest expense |
|
(16,318 |
) |
(16,673 |
) |
(15,626 |
) |
(10,574 |
) |
(3,985 |
) | |||||||||
|
Earnings from continuing operations, before income tax expense |
|
137,508 |
136,616 |
64,071 |
27,165 |
48,079 |
||||||||||||||
|
Income tax expense |
|
48,841 |
52,435 |
23,031 |
9,565 |
17,242 |
||||||||||||||
|
Earnings from continuing operations, net of income tax expense |
88,667 |
84,181 |
41,040 |
17,600 |
30,837 |
|||||||||||||||
|
Discontinued operations, net of income tax (benefit) expense of $(1,204), $(281), $(31,563), $12,412, and $12,982, respectively |
(2,422 |
) |
(684 |
) |
32,362 |
(61,229 |
) |
24,795 |
||||||||||||
|
Net earnings (loss) |
86,245 |
83,497 |
73,402 |
(43,629 |
) |
55,632 |
||||||||||||||
|
Noncontrolling interest |
2,574 |
— |
— |
— |
— |
|||||||||||||||
|
Net earnings (loss) attributable to Centene Corporation |
|
$ |
83,671 |
$ |
83,497 |
$ |
73,402 |
$ |
(43,629 |
) |
$ |
55,632 |
||||||||
|
Amounts attributable to Centene Corporation common shareholders: |
||||||||||||||||||||
|
Earnings from continuing operations, net of income tax expense |
$ |
86,093 |
$ |
84,181 |
$ |
41,040 |
$ |
17,600 |
$ |
30,837 |
||||||||||
|
Discontinued operations, net of income tax (benefit) expense |
(2,422 |
) |
(684 |
) |
32,362 |
(61,229 |
) |
24,795 |
||||||||||||
|
Net earnings (loss) |
$ |
83,671 |
$ |
83,497 |
$ |
73,402 |
$ |
(43,629 |
) |
$ |
55,632 |
|||||||||
|
Net earnings (loss) per common share attributable to Centene Corporation: |
|
|||||||||||||||||||
|
Basic: |
||||||||||||||||||||
|
Continuing operations |
|
$ |
2.00 |
$ |
1.95 |
$ |
0.95 |
$ |
0.41 |
$ |
0.73 |
|||||||||
|
Discontinued operations |
|
(0.06 |
) |
(0.02 |
) |
0.74 |
(1.42 |
) |
0.58 |
|||||||||||
|
Basic earnings (loss) per common share |
|
$ |
1.94 |
$ |
1.93 |
$ |
1.69 |
$ |
(1.01 |
) |
$ |
1.31 |
||||||||
|
Diluted: |
|
|||||||||||||||||||
|
Continuing operations |
|
$ |
1.94 |
$ |
1.90 |
$ |
0.92 |
$ |
0.39 |
$ |
0.69 |
|||||||||
|
Discontinued operations |
|
(0.05 |
) |
(0.02 |
) |
0.72 |
(1.37 |
) |
0.55 |
|||||||||||
|
Diluted earnings (loss) per common share |
|
$ |
1.89 |
$ |
1.88 |
$ |
1.64 |
$ |
(0.98 |
) |
$ |
1.24 |
||||||||
|
Weighted average number of common shares outstanding: |
|
|||||||||||||||||||
|
Basic |
|
43,034,791 |
43,275,187 |
43,539,950 |
43,160,860 |
42,312,522 |
||||||||||||||
|
Diluted |
|
44,316,467 |
44,398,955 |
44,823,082 |
44,613,622 |
45,027,633 |
||||||||||||||
___________________________________________
1 2006 results for discontinued operations include a goodwill impairment charge of $81,098 and other non-cash impairment charges of $7,170 for the FirstGuard reporting unit.
|
|
December 31, |
|||||||||||||||||||
|
|
2009 |
2008 |
2007 |
2006 |
2005 |
|||||||||||||||
|
|
(In thousands) |
|||||||||||||||||||
|
Consolidated Balance Sheet Data: |
|
|||||||||||||||||||
|
Cash and cash equivalents |
|
$ |
400,951 |
$ |
370,999 |
$ |
267,305 |
$ |
237,514 |
$ |
112,269 |
|||||||||
|
Investments and restricted deposits |
585,183 |
451,058 |
369,545 |
174,431 |
163,489 |
|||||||||||||||
|
Total assets |
|
1,702,364 |
1,451,152 |
1,121,824 |
894,980 |
668,030 |
||||||||||||||
|
Medical claims liability |
470,932 |
384,360 |
323,741 |
241,073 |
123,102 |
|||||||||||||||
|
Long-term debt |
|
307,085 |
264,637 |
206,406 |
174,646 |
92,448 |
||||||||||||||
|
Total stockholders’ equity |
|
619,427 |
501,272 |
415,047 |
326,423 |
352,048 |
||||||||||||||
Item 7. Management’s Discussion and Analysis of Financial Condition and Results of Operations
The following discussion of our financial condition and results of operations should be read in conjunction with our consolidated financial statements and the related notes included elsewhere in this filing. The discussion contains forward-looking statements that involve known and unknown risks and uncertainties,
including those set forth under Part I, Item 1A.“Risk Factors” of this Form 10-K.
Our MD&A includes the following sections:
|
· |
Overview |
|
· |
Membership |
|
· |
Results of Continuing Operations |
|
· |
Liquidity and Capital Resources |
|
· |
Contractual Obligations |
|
· |
Regulatory Capital and Dividend Restrictions |
|
· |
Recent Accounting Pronouncements |
|
· |
Critical Accounting Policies and Estimates |
OVERVIEW
We are a multi-line healthcare enterprise operating in two segments: Medicaid Managed Care and Specialty Services. Our Medicaid Managed Care segment provides Medicaid and Medicaid-related health plan coverage to individuals through government subsidized programs, including Medicaid, the State Children’s Health Insurance Program,
or CHIP, Foster Care, Medicare Special Needs Plans and the Supplemental Security Income Program, also known as the Aged, Blind or Disabled Program, or collectively ABD. Our health plans in Florida, Georgia, Indiana, Ohio, South Carolina, Texas and Wisconsin are included in the Medicaid Managed Care segment. Our Specialty Services segment provides specialty services, including behavioral health, individual health insurance, life and health management, long-term care programs, managed vision,
telehealth services, and pharmacy benefits management to state programs, healthcare organizations, employer groups and other commercial organizations, as well as to our own subsidiaries. Our health plans in Arizona, which is operated by our long-term care company, and Massachusetts, which is operated by our individual health insurance provider, are included in the Specialty Services segment. Our Specialty Services segment also provides a full range of healthcare solutions for the rising
number of uninsured Americans.
We expect to complete the sale of certain assets of University Health Plans, Inc, or UHP, our New Jersey health plan, in the first quarter of 2010. Unless specifically noted, the discussions below are in the context of continuing operations, and therefore, exclude UHP. The results of operations for UHP are classified
as discontinued operations for all periods presented.
The first quarter of 2008 included $20.8 million of premium revenue for the Georgia premium rate increase related to the period from July 1, 2007 through December 31, 2007. All 2008 ratios and year over year changes discussed below are inclusive of this revenue.
Our financial performance for 2009 is summarized as follows:
|
— |
Year-end at-risk managed care membership of 1,455,600. |
|
— |
Premium and service revenues of $3.9 billion. |
|
— |
Health Benefits Ratio of 83.5%. |
|
— |
General and Administrative expense ratio of 13.3%. |
|
— |
Diluted net earnings per share of $1.94. |
|
— |
Total operating cash flows of $248.2 million, or 2.9 times net earnings. |
The following new contracts and acquisitions contributed to our revenue and membership growth over the last two years:
|
— |
In July 2009, we began operating in Massachusetts to manage healthcare services for members under the state’s Commonwealth Care program and in October 2009 under the Commonwealth Care Bridge program, operating as CeltiCare Health Plan of Massachusetts. At December 31, 2009, we served 27,800 members. |
|
— |
In March 2009, we completed an acquisition of certain assets in South Carolina. We now serve 48,600 at-risk members in South Carolina at December 31, 2009. |
|
— |
In February 2009, we began converting non-risk managed care membership in Florida from Access Health Solutions LLC, or Access, to our new subsidiary, Sunshine State Health Plan on an at-risk basis. Additionally, we also completed an acquisition of certain assets in Florida, adding to our membership. At December 31, 2009, we served
102,600 members on an at-risk basis while Access served 59,700 members on a non-risk basis. Beginning January 1, 2009, we have presented our investment in Access as a consolidated subsidiary. |
|
— |
In October 2008, we began operating under our contract in Arizona to provide Acute Care services in Yavapai county. |
|
— |
Effective July 2008, we completed the acquisition of Celtic, a health insurance carrier focused on the individual health insurance market. |
|
— |
In April 2008, we began operating under our new contract in Texas to provide statewide managed care services to participants in the Texas Foster Care program. |
We expect our revenue and membership base to continue to grow in 2010. The following factors contribute to our growth potential in 2010:
|
— |
In November 2009, we announced we were selected to provide managed care services in Mississippi to Medicaid recipients through the Mississippi Coordinated Access Network (MississippiCan) program. We are working with the State and currently expect a 2010 start date. |
|
— |
In February 2010, we announced a definitive agreement to acquire certain Medicaid assets in South Carolina. The transaction is expected to close in the third quarter of 2010 and add revenues of $55 to $65 million for 2010. |
|
— |
Full year impact of our new health plan in Massachusetts, continued membership conversion in Florida, and the full year impact in 2010 of membership growth experienced during 2009. |
|
— |
Our revenue in 2010 will be adversely affected by the removal of pharmacy benefits from our contracted services (pharmacy carve-outs) in two states in 2010. |
MEMBERSHIP
From December 31, 2007 to December 31, 2009, we increased our at-risk managed care membership by 38.1%. The following table sets forth our membership by state for our managed care organizations:
|
December 31, | ||||||
|
2009 |
2008 |
2007 | ||||
|
Arizona |
18,100 |
14,900 |
— | |||
|
Florida |
102,600 |
— |
— | |||
|
Georgia |
309,700 |
288,300 |
287,900 | |||
|
Indiana |
|
208,100 |
|
175,300 |
|
154,600 |
|
Massachusetts |
27,800 |
— |
— | |||
|
Ohio |
|
150,800 |
|
133,400 |
|
128,700 |
|
South Carolina |
48,600 |
31,300 |
100 | |||
|
Texas |
|
455,100 |
|
428,000 |
|
351,000 |
|
Wisconsin |
|
134,800 |
|
124,800 |
|
131,900 |
|
Total at-risk membership |
1,455,600 |
1,196,000 |
1,054,200 | |||
|
Non-risk membership |
63,700 |
3,700 |
35,100 | |||
|
Total |
|
1,519,300 |
|
1,199,700 |
|
1,089,300 |
The following table sets forth our membership by line of business:
|
|
December 31, | |||||
|
|
2009 |
|
2008 |
|
2007 | |
|
Medicaid |
|
1,081,400 |
|
877,400 |
|
779,300 |
|
CHIP & Foster Care |
|
263,600 |
|
257,300 |
|
214,600 |
|
ABD & Medicare |
82,800 |
61,300 |
60,300 | |||
|
Other State programs |
|
27,800 |
|
— |
— | |
|
Total at-risk membership |
1,455,600 |
1,196,000 |
1,054,200 | |||
|
Non-risk membership |
63,700 |
3,700 |
35,100 | |||
|
Total |
|
1,519,300 |
|
1,199,700 |
|
1,089,300 |
The following table provides supplemental information of other membership categories:
|
December 31, | ||||||
|
2009 |
2008 |
2007 | ||||
|
Cenpatico Behavioral Health: |
||||||
|
Kansas |
|
41,400 |
|
41,100 |
|
39,000 |
|
Arizona |
|
120,100 |
|
105,000 |
|
99,900 |
|
Bridgeway: |
||||||
|
Long-term Care |
|
2,600 |
|
2,100 |
|
1,600 |
From December 31, 2008 to December 31, 2009 our membership increased in all of our states as a result of:
|
· |
strong organic growth as a result of general economic conditions; |
|
· |
acquisitions in Florida and South Carolina; |
|
· |
the conversion of non-risk membership from Access to at-risk under Sunshine State Health Plan in Florida; and |
|
· |
expansion into Massachusetts under the state Commonwealth Care Bridge and Commonwealth Care programs. |
From December 31, 2007 to December 31, 2008 our membership increased as a result of:
|
· |
organic growth in Arizona, Indiana and Texas; |
|
· |
the addition of the Foster Care program in Texas; |
|
· |
temporary eligibility determinations and network expansions in Indiana; |
|
· |
expansion of our Arizona health plan into Yavapai county in October 2008; and |
|
· |
the conversion of non-risk membership in South Carolina as additional counties converted to at-risk. |
Our membership decreased in Wisconsin due to the termination of certain provider contracts.
RESULTS OF CONTINUING OPERATIONS
The following discussion and analysis is based on our consolidated statements of operations, which reflect our results of operations for the years ended December 31, 2009, 2008 and 2007, as prepared in accordance with generally accepted accounting principles in the United States, or GAAP.
Summarized comparative financial data for 2009, 2008 and 2007 are as follows ($ in millions):
|
2009 |
2008 |
2007 |
% Change 2008 - 2009 |
% Change 2007 - 2008 |
||||||||||||||||
|
Premium |
$ | 3,786.5 | $ | 3,199.3 | $ | 2,611.9 | 18.4 | % | 22.5 | % | ||||||||||
|
Service |
91.8 | 75.0 | 80.5 | 22.4 | % | (6.9 | )% | |||||||||||||
|
Premium and service revenues |
3,878.3 | 3,274.3 | 2,692.4 | 18.4 | % | 21.6 | % | |||||||||||||
|
Premium tax |
224.6 | 90.2 | 76.6 | 149.0 | % | 17.8 | % | |||||||||||||
|
Total revenues |
4,102.9 | 3,364.5 | 2,769.0 | 21.9 | % | 21.5 | % | |||||||||||||
|
Medical costs |
3,163.5 | 2,640.3 | 2,190.9 | 19.8 | % | 20.5 | % | |||||||||||||
|
Cost of services |
60.8 | 56.9 | 61.3 | 6.8 | % | (7.2 | )% | |||||||||||||
|
General and administrative expenses |
514.6 | 444.7 | 385.0 | 15.7 | % | 15.5 | % | |||||||||||||
|
Premium tax expense |
225.9 | 91.0 | 76.6 | 148.3 | % | 18.8 | % | |||||||||||||
|
Earnings from operations |
138.1 | 131.6 | 55.2 | 5.0 | % | 138.1 | % | |||||||||||||
|
Investment and other income, net |
(0.6 | ) | 5.0 | 8.8 | (112.4 | )% | (42.7 | )% | ||||||||||||
|
Earnings from continuing operations, before income tax expense |
137.5 | 136.6 | 64.0 | 0.7 | % | 113.2 | % | |||||||||||||
|
Income tax expense |
48.8 | 52.4 | 23.0 | (6.9 | )% | 127.7 | % | |||||||||||||
|
Earnings from continuing operations, net of income tax expense |
88.7 | 84.2 | 41.0 | 5.3 | % | 105.1 | % | |||||||||||||
|
Discontinued operations, net of income tax (benefit) expense of $(1.2), $(0.3) and $(31.6) respectively |
(2.4 | ) | (0.7 | ) | 32.4 | 254.1 | % | (102.1 | )% | |||||||||||
|
Net earnings (loss) |
86.3 | 83.5 | 73.4 | 3.3 | % | 13.8 | % | |||||||||||||
|
Noncontrolling interest |
2.6 | — | — | — | — | |||||||||||||||
|
Net earnings attributable to Centene Corporation |
$ | 83.7 | $ | 83.5 | $ | 73.4 | 0.2 | % | 13.8 | % | ||||||||||
|
Amounts attributable to Centene Corporation common shareholders: |
||||||||||||||||||||
|
Earnings from continuing operations, net of income tax expense |
$ | 86.1 | $ | 84.2 | $ | 41.0 | 2.3 | % | 105.1 | % | ||||||||||
|
Discontinued operations, net of income tax (benefit) expense |
(2.4 | ) | (0.7 | ) | 32.4 | 254.1 | % | (102.1 | )% | |||||||||||
|
Net earnings |
$ | 83.7 | $ | 83.5 | $ | 73.4 | 0.2 | % | 13.8 | % | ||||||||||
|
Diluted earnings (loss) per common share attributable to Centene Corporation: |
||||||||||||||||||||
|
Continuing operations |
$ | 1.94 | $ | 1.90 | $ | 0.92 | 2.1 | % | 106.5 | % | ||||||||||
|
Discontinued operations |
(0.05 | ) | (0.02 | ) | 0.72 | (150.0 | )% | (102.8 | )% | |||||||||||
|
Total diluted earnings (loss) per common share |
$ | 1.89 | $ | 1.88 | $ | 1.64 | 0.5 | % | 14.6 | % | ||||||||||
Revenues and Revenue Recognition
Our health plans generate revenues primarily from premiums we receive from the states in which we operate. We receive a fixed premium per member per month pursuant to our state contracts. We generally receive premium payments during the month we provide services and recognize premium revenue during the period in which
we are obligated to provide services to our members. In some instances, our base premiums are subject to an adjustment, or risk score, based on the acuity of our membership. Generally, the risk score is determined by the state analyzing encounter submissions of processed claims data to determine the acuity of our membership relative to the entire state’s Medicaid membership. Some contracts allow for additional premium associated with certain supplemental services provided
such as maternity deliveries. Revenues are recorded based on membership and eligibility data provided by the states, which may be adjusted by the states for updates to this data. These eligibility adjustments have been immaterial in relation to total revenue recorded and are reflected in the period known.
Our specialty companies generate revenues under contracts with state programs, healthcare organizations, and other commercial organizations, as well as from our own subsidiaries. Revenues are recognized when the related services are provided or as ratably earned over the covered period of services.
Premium and service revenues collected in advance are recorded as unearned revenue. For performance-based contracts, we do not recognize revenue subject to refund until data is sufficient to measure performance. Premium and service revenues due to us are recorded as premium and related receivables and are recorded net
of an allowance based on historical trends and our management’s judgment on the collectibility of these accounts. As we generally receive payments during the month in which services are provided, the allowance is typically not significant in comparison to total revenues and does not have a material impact on the presentation of our financial condition or results of operations.
Some states enact premium taxes, similar assessments and provider pass-through payments, collectively, premium taxes, and these taxes are recorded as a component of revenues as well as operating expenses. In 2009, one of the states in which we operate increased their premium which was required to be passed through to hospitals
in the state. For the year ended December 31, 2009, this pass-through totaled $132.9 million and increased our premium tax revenue and expense. We exclude premium taxes from our key ratios as we believe the premium tax is, in essence, a pass-through of costs and not indicative of our operating performance.
Premium and service revenues increased 18.4% in 2009 over 2008 as a result of membership growth in all our states discussed under the heading “Membership”, the effect of a full year of the Celtic acquisition in July 2008, and premium rate increases. The premium rates specified in our state contracts are generally updated
on an annual basis through contract amendments. In 2009, we received premium rate increases in certain markets which yielded a 2.9% composite increase across all of our markets.
Premium and service revenues increased 21.6% in 2008 over 2007 as a result of membership growth in Arizona, Indiana and Texas, the Celtic acquisition in July 2008, and premium rate increases. In 2008, we received premium rate increases in certain markets which yield a 2.7% composite increase across all of our markets.
In November 2007, we received a contract amendment from the State of Georgia providing for an effective premium rate increase in Georgia of approximately 3.8% effective July 1, 2007. We executed this amendment on November 16, 2007. The State of Georgia returned the fully executed contract in January 2008 and, accordingly,
we recorded the additional revenue, retroactive to July 1, 2007, in the first quarter of 2008. The premium revenue, related to the period from July 1, 2007 to December 31, 2007, totals approximately $20.8 million.
Contract amendments related to rate increases for the Georgia health plan effective July 1, 2008 and 2009 were not fully executed until the respective fourth quarters and accordingly, the premium revenue from July 1 to September 30 was recorded in the fourth quarter in each respective year.
Operating Expenses
Medical Costs
Medical costs include payments to physicians, hospitals, and other providers for healthcare and specialty services claims. Medical costs also include estimates of medical expenses incurred but not yet reported, or IBNR, and estimates of the cost to process unpaid claims. We use our judgment to determine the assumptions to be used in the calculation
of the required IBNR estimate. The assumptions we consider include, without limitation, claims receipt and payment experience (and variations in that experience), changes in membership, provider billing practices, healthcare service utilization trends, cost trends, product mix, seasonality, prior authorization of medical services, benefit changes, known outbreaks of disease or increased incidence of illness such as influenza, provider contract changes, changes to Medicaid fee schedules, and the incidence
of high dollar or catastrophic claims.
Our development of the IBNR estimate is a continuous process which we monitor and refine on a monthly basis as claims receipts and payment information becomes available. As more complete information becomes available, we adjust the amount of the estimate, and include the changes in estimates in medical expense in the period in
which the changes are identified.
Additionally, we contract with independent actuaries to review our estimates on a quarterly basis. The independent actuaries provide us with a review letter that includes the results of their analysis of our medical claims liability. We do not solely rely on their report to adjust our claims liability. We utilize their
calculation of our claims liability only as additional information, together with management’s judgment to determine the assumptions to be used in the calculation of our liability for medical costs.
While we believe our IBNR estimate is appropriate, it is possible future events could require us to make significant adjustments for revisions to these estimates. Accordingly, we can not assure you that healthcare claim costs will not materially differ from our estimates.
Results of operations depend on our ability to manage expenses associated with health benefits and to accurately predict costs incurred. The health benefits ratio, or HBR, represents medical costs as a percentage of premium revenues (excluding premium taxes) and reflects the direct relationship between the premium received and the medical
services provided. The table below depicts the HBR for our external membership by member category:
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Medicaid and CHIP |
84.6 | % | 80.6 | % | 82.8 | % | ||||||
|
ABD and Medicare |
81.1 | 91.1 | 91.4 | |||||||||
|
Specialty Services |
80.2 | 83.8 | 78.4 | |||||||||
|
Total |
83.5 | 82.5 | 83.9 | |||||||||
The consolidated HBR for the year ended December 31, 2009 was 83.5%, an increase of 1.0% over 2008. The increase in the total HBR in 2009 as compared to 2008 is due to the effect of the following items:
|
Ÿ |
recording the Georgia premium rate increase for the period from July 1, 2007 to December 31, 2007 during the first quarter of 2008 had the effect of decreasing the HBR in 2008 by 0.6%; |
|
Ÿ |
a March 1, 2009 rate decrease for our CHIP/Perinate product in Texas which brought the HBR more in line with our normal range; |
|
Ÿ |
higher HBR in our Florida market; and |
|
Ÿ |
additional costs related to the flu. |
These factors were partially offset by reductions in the HBR for our ABD product, particularly due to provider network improvements and exiting certain markets in Ohio, and growth in our South Carolina ABD membership which operates at a lower HBR than our normal range. The decrease in our ABD HBR lowered our total HBR by 1.7% for
the year ended December 31, 2009.
The consolidated HBR for the year ended December 31, 2008 was 82.5%, a decrease of 1.4% over 2007. The decrease for the year ended December 31, 2008 over 2007 is due to the effect of recording the Georgia premium rate increase for the period to July 1, 2007 to December 31, 2007 in 2008.
Cost of Services
Cost of services expense includes the pharmaceutical costs associated with our pharmacy benefit manager’s external revenues. Cost of services also includes all direct costs to support the functions responsible for generation of our services revenues. These expenses consist of the salaries and wages of the professionals and teachers
who provide the services and expenses associated with facilities and equipment used to provide services.
General and Administrative Expenses
General and administrative expenses, or G&A, primarily reflect wages and benefits, including stock compensation expense, and other administrative costs associated with our health plans, specialty companies and centralized functions that support all of our business units. Our major centralized functions are finance, information systems
and claims processing. G&A increased in both the years ended December 31, 2009 and December 31, 2008 primarily due to expenses for additional staff and facilities to support our growth. G&A also increased in 2009 as result of the consolidation of Access. Additionally, G&A increased in 2008 as a result of the acquisition of Celtic. G&A expenses also include business expansion costs, such as wages and benefits for administrative personnel, contracting costs, and
information technology buildouts, incurred prior to the commencement of a new contract or state health plan. For example, we incurred business expansion costs for the Foster Care product in Texas in 2008 and Massachusetts in 2009. Our G&A in 2010 will include business expansion costs associated with our new contract in Mississippi.
The G&A expense ratio represents G&A expenses as a percentage of premium and service revenues, and reflects the relationship between revenues earned and the costs necessary to earn those revenues. The consolidated G&A expense ratio for the years ended December 31, 2009, 2008 and 2007 were 13.3%, 13.6% and 14.3%, respectively. The
decrease in the ratio in 2009 primarily reflects the leveraging of our expenses over higher revenues, partially offset by the effect of the acquisition of Celtic, our business expansion costs for Florida, Massachusetts and Mississippi and the consolidation of Access.
Other Income (Expense)
|
|
The following table summarizes the components of investment and other income, net ($ in millions): |
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Investment income |
$ | 15.7 | $ | 19.8 | $ | 23.9 | ||||||
|
Reserve Primary fund loss |
— | (4.5 | ) | — | ||||||||
|
Earnings from equity method investee |
— | 6.4 | 0.5 | |||||||||
|
Interest expense |
(16.3 | ) | (16.7 | ) | (15.6 | ) | ||||||
|
Investment and other income, net |
$ | (0.6 | ) | $ | 5.0 | $ | 8.8 | |||||
Other income (expense) consists principally of investment income from cash and investments, earnings in equity method investments, and interest expense on debt. Decreases in investment income in 2009 and 2008 reflect the decline in market interest rates. The 2008 results included a loss of $4.5 million related to our investment
in the Reserve Primary money market fund whose Net Asset Value fell below $1.00 per share. As of December 31, 2009, the carrying amount of our investment in the Reserve Primary money market fund was $2.4 million. In January 2010, we received a distribution from the fund of $5.4 million and will record a gain of $3.0 million in the first quarter of 2010. Earnings from equity method investee decreased due to the
inclusion of investment in Access as a consolidated subsidiary beginning in 2009. Interest expense was relatively stable reflecting modest increases in debt balances offset by the decline in market interest rates associated with variable rate debt.
Income Tax Expense
The effective tax rate in 2009 was 35.5% compared to 38.4% in 2008 and 35.9% in 2007. The decrease in 2009 was primarily due to the effect of the inclusion of the noncontrolling interest in consolidated subsidiaries (for which we are not required to provide income taxes) and an increase in 2008 due to a change in the estimated benefit
to be realized from New Jersey state net operating loss carryforwards. Excluding the effect of the noncontrolling interest, our effective tax rate would have been 36.2% in 2009. The increase in 2008 from 2007 was due to higher state taxes as a result of a change in the estimated benefit to be realized from New Jersey state net operating loss carryforwards.
Discontinued Operations
In November 2008, we announced our intention to sell certain assets of UHP, our New Jersey health plan. Accordingly, the results of operations for UHP are reported as discontinued operations for all periods presented. We expect to complete the sale in the first quarter of 2010. UHP was previously reported
in the Medicaid Managed Care segment.
The pre-tax loss from discontinued operations was $3.6 million in 2009 and $1.0 million in 2008 compared to a pre-tax gain of $0.8 million in 2007. Legal expenses of $1.8 million and employee retention expenses of $3.6 million related to the pending sale of UHP were included in the results from discontinued operations during 2009. The
2008 results include a one-time charge of $3.7 million primarily for asset impairments and employee severance related to the sale. The assets and liabilities of the discontinued business are segregated in the consolidated balance sheet.
Net earnings from discontinued operations in 2007 included tax benefits of $32.6 million, net of asset write-offs, associated with the abandonment of the stock of our FirstGuard health plans.
Segment Results
The following table summarizes our operating results by segment ($ in millions):
|
2009 |
2008 |
2007 |
% Change
2008-2009 |
% Change
2007-2008 |
||||||||||||||||
|
Premium and Service Revenues |
||||||||||||||||||||
|
Medicaid Managed Care |
$ | 3,464.8 | $ | 2,992.3 | $ | 2,524.7 | 15.8 | % | 18.5 | % | ||||||||||
|
Specialty Services |
1,049.5 | 816.5 | 651.9 | 28.5 | % | 25.2 | % | |||||||||||||
|
Eliminations |
(636.0 | ) | (534.5 | ) | (484.2 | ) | 19.0 | % | 10.4 | % | ||||||||||
|
Consolidated Total |
$ | 3,878.3 | $ | 3,274.3 | $ | 2,692.4 | 18.4 | % | 21.6 | % | ||||||||||
|
Earnings from Operations |
||||||||||||||||||||
|
Medicaid Managed Care |
$ | 99.3 | $ | 108.4 | $ | 35.5 | (8.4 | ) % | 204.9 | % | ||||||||||
|
Specialty Services |
38.8 | 23.2 | 19.7 | 67.4 | % | 17.8 | % | |||||||||||||
|
Consolidated Total |
$ | 138.1 | $ | 131.6 | $ | 55.2 | 5.0 | % | 138.1 | % | ||||||||||
Medicaid Managed Care
Premium and service revenues increased 15.8% in 2009 due to membership growth in our states, especially Florida, Indiana, South Carolina and Texas. Premium and service revenues increased 18.5% in 2008 over 2007 due primarily to higher membership in Texas from the Foster Care product, at-risk membership growth in South Carolina,
and the effect of recording the Georgia premium rate increase of $20.8 million for the period July 1, 2007 to December 31, 2007 in 2008.
Earnings from operations decreased in 2009 from 2008 levels due to the aforementioned effect of the Georgia rate increase. Excluding the effects of recording this rate increase in 2008, earnings from operations increased 13.4% in 2009 over 2008 levels reflecting the overall growth in our membership and revenue base and improvements
in our ABD product, especially in Ohio and South Carolina, offset by a rate decrease in Texas, higher medical costs related to the flu, and a higher HBR in Florida.
Specialty Services
Premium and service revenues increased 28.5% in 2009 primarily due to a full year effect of the Celtic acquisition, the commencement of our new health plan in Massachusetts, and membership growth in our Medicaid segment and the associated specialty services provided to this increased membership. Premium and service revenues increased
25.2% in 2008 over 2007 due primarily to the acquisition of Celtic and higher membership in Texas from the Foster Care product of which behavioral health comprises a significant percentage of the overall premium for this product.
Earnings from operations increased 67.4% in 2009 from 2008 levels primarily due to the increase in revenue and leveraging of the segments infrastructure costs over this higher revenue base. Earnings from operations also increased due to a lower HBR.
LIQUIDITY AND CAPITAL RESOURCES
Shown below is a condensed schedule of cash flows for the years ended December 31, 2009, 2008 and 2007, that we use throughout our discussion of liquidity and capital resources ($ in millions).
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Net cash provided by operating activities |
$ |
248.2 |
$ |
222.0 |
$ |
202.2 |
||||||
|
Net cash used in investing activities |
(270.1 |
) |
(153.9 |
) |
(225.5 |
) | ||||||
|
Net cash provided by financing activities |
46.6 |
42.4 |
20.8 |
|||||||||
|
Net increase (decrease) in cash and cash equivalents |
$ |
24.7 |
$ |
110.5 |
$ |
(2.5 |
) | |||||
We finance our activities primarily through operating cash flows and borrowings under our revolving credit facility. Our total operating activities provided cash of $248.2 million in 2009, $222.0 million in 2008 and $202.2 million in 2007. Cash flow from operations in 2009 reflects the receipt in December 2009 of premiums
for the month of January 2010 for three of our health plans, increasing our unearned revenue at December 31, 2009 by $78.3 million as compared to the prior year end. Cash flow from operations also reflected an increase in medical claims liability primarily as a result of new business in Florida, Massachusetts and South Carolina. Cash flow from operations in 2008 reflected an increase in our Medical claims liability as a result of new business in Texas, South Carolina and Arizona. This
was partially offset by a decrease in unearned revenue resulting from a timing difference with the receipt of our December revenue for our Ohio health plan.
Our investing activities used cash of $270.1 million in 2009, $153.9 million in 2008 and $225.5 million in 2007. Cash flows from investing activities in 2009 primarily consisted of additions to the investment portfolios of our regulated subsidiaries including transfers from cash and cash equivalents to long-term investments. Cash
flows from investing activities also include the capital expenditures discussed below, membership conversion fees in Florida and acquisitions in Florida and South Carolina. Cash flows from investing activities in 2008 included the purchase price of Celtic, which we acquired on July 1, 2008, capital expenditures and our investment in the Reserve Primary fund. Our investing activities in 2007 consisted primarily of additions to the investment portfolios of our regulated subsidiaries including
transfers from cash and cash equivalents to long-term investments.
Our investment policies are designed to provide liquidity, preserve capital and maximize total return on invested assets within our guidelines. Net cash provided by and used in investing activities will fluctuate from year to year due to the timing of investment purchases, sales and maturities. As of December 31, 2009,
our investment portfolio consisted primarily of fixed-income securities with an average duration of 2.6 years. Cash is invested in investment vehicles such as municipal bonds, corporate bonds, instruments of the U.S. Treasury, insurance contracts, commercial paper, bank deposits, asset backed securities and equity securities. These securities generally are actively traded in secondary markets and the reported fair market value is determined based on recent trading activity, recent trading activity
in similar securities and other observable inputs. Our investment guidelines are compliant with the regulatory restrictions enacted in each state.
The following table summarizes our cash and investment balances as of December 31, ($ in millions):
|
2009 |
2008 |
|||||||
|
Cash, cash equivalents and short-term investments |
$ | 440.5 | $ | 480.4 | ||||
|
Long-term investments |
525.5 | 332.4 | ||||||
|
Restricted deposits |
20.1 | 9.3 | ||||||
|
Total cash, investments and restricted deposits |
$ | 986.1 | $ | 822.1 | ||||
|
Regulated cash, investments and restricted deposits |
$ | 949.9 | $ | 798.0 | ||||
|
Unregulated cash and investments |
36.2 | 24.1 | ||||||
|
Consolidated Total |
$ | 986.1 | $ | 822.1 | ||||
|
Regulated cash and investments from discontinued operations1 |
$ | 24.9 | $ | 30.1 | ||||
|
________________________ |
||||||||
| 1 Upon completion of the sale of assets of UHP and the subsequent payment of medical claims liabilities and other liabilities at the closing date, substantially all of the remaining regulated cash of UHP will be transferred to our unregulated cash. | ||||||||
We spent $83.1 million, $65.2 million and $53.9 million in 2009, 2008 and 2007, respectively, on capital assets consisting primarily of building construction, software and hardware upgrades, furniture, equipment, and leasehold improvements associated with office and market expansions. Exclusive of our real estate development discussed
below, we anticipate spending approximately $40 million on capital expenditures in 2010 primarily associated with system enhancements and market expansions.
During the second quarter of 2009, we executed an agreement as a joint venture partner in an entity that will develop property adjoining our corporate office, which we believe is necessary to accommodate our growing business. For the year ended December 31, 2009 and 2008 we had capital expenditures of $59.5 million and $27.0 million,
respectively, for costs associated with the real estate development. The development is expected to be substantially complete in 2010 and we anticipate spending approximately $100 million on capital expenditures related to the construction in 2010.
In June 2009, this joint venture executed a $95 million construction loan associated with the development. The construction loan is due June 1, 2011 and may be extended for two additional one year terms. The loan bears interest at the LIBOR rate plus 4% with a minimum rate of 5%. We and our development partner
have each guaranteed up to $65 million associated with the construction loan. The agreement contains non-financial and financial covenants, including requirements for us to maintain a specified net worth. As of December 31, 2009, there was $32.6 million outstanding under the construction loan. Additionally, the joint venture has posted a $1.75 million letter of credit to a tenant of the development, collateralized by a portion of the entity’s cash balances.
Our financing activities provided cash of $46.6 million in 2009, $42.4 million in 2008 and $20.8 million in 2007. During 2009, our financing activities primarily related to proceeds from borrowings under our $300 million credit facility and construction financing of the real estate development discussed above. During
2008, our financing activities primarily related to borrowings under our $300 million revolver and stock repurchases. During 2007, our financing activities primarily related to proceeds from issuance of $175 million in senior notes as discussed below.
At December 31, 2009, we had working capital, defined as current assets less current liabilities, of $(99.8) million, as compared to $25.4 million at December 31, 2008. We manage our short-term and long-term investments with the goal of ensuring that a sufficient portion is held in investments that are highly liquid and can be
sold to fund short-term requirements as needed. Our working capital was negative at December 31, 2009, due to our efforts to increase investment returns through purchases of investments that have maturities of greater than one year and, therefore, are classified as long-term.
At December 31, 2009, our debt to capital ratio, defined as total debt divided by the sum of total debt and total equity, was 33.2%, as compared to 34.6% at December 31, 2008. We utilize the debt to capital ratio as a measure, among others, of our leverage and financial flexibility.
On January 21, 2010, we completed the sale of an additional 5.75 million shares of common stock for $19.25 per share. Net proceeds from the sale of the additional shares were approximately $104.5 million. We used a portion of the net proceeds to repay the outstanding
indebtedness under our $300 million revolving credit loan facility ($84.0 million as of December 31, 2009). We intend to use the remaining net proceeds for general corporate purposes, which may include the repayment of indebtedness, funding for acquisitions, capital expenditures, additions to working capital and to meet statutory capital requirements in new or existing states.
We have a $300 million revolving credit agreement. Borrowings under the agreement bear interest based upon LIBOR rates, the Federal Funds Rate or the Prime Rate. There is a commitment fee on the unused portion of the agreement that ranges from 0.15% to 0.275% depending on the total debt to EBITDA ratio. The agreement
contains non-financial and financial covenants, including requirements of minimum fixed charge coverage ratios, maximum debt to EBITDA ratios and minimum net worth. The agreement will expire in September 2011. As of December 31, 2009, we had $84.0 million in borrowings outstanding under the agreement and $40.5 million in letters of credit outstanding, leaving availability of $175.5 million. As of December 31, 2009, we were in compliance with all covenants.
In 2007, we issued $175 million aggregate principal amount of our 7.25% Senior Notes due April 1, 2014, or the Notes. The Notes were registered under the Securities Act of 1933, pursuant to a registration rights agreement with the initial purchasers. The indenture governing the Notes contains non-financial and financial
covenants, including requiring a minimum fixed charge coverage ratio. Interest is paid semi-annually in April and October. As of December 31, 2009, we were in compliance with all covenants.
We have a stock repurchase program authorizing us to repurchase up to four million shares of common stock from time to time on the open market or through privately negotiated transactions. No duration has been placed on the repurchase program and we reserve the right to discontinue the repurchase program at any time. During
the year ended December 31, 2009, we repurchased 332,595 shares.
During the year ended December 31, 2009, we received dividends of $19.1 million from our regulated subsidiaries. On July 1, 2008 we completed the acquisition of Celtic for a purchase price of approximately $82.0 million, net of unregulated cash acquired. During the year ended December 31, 2008, the Company received a
dividend from Celtic of $31.4 million concurrent with the acquisition, and received an additional dividend of $17.0 million from a regulated subsidiary. During the year ended December 31, 2007, we received dividends of $35.4 million for the excess regulatory capital remaining in our Kansas and Missouri health plans and dividends of $18.5 million from other regulated subsidiaries.
Based on our operating plan, we expect that our available cash, cash equivalents and investments, cash from our operations and cash available under our credit facility and construction loan will be sufficient to finance our general operations, planned acquisition of Medicaid assets of South Carolina and capital expenditures for at least
12 months from the date of this filing.
CONTRACTUAL OBLIGATIONS
The following table summarizes future contractual obligations. These obligations contain estimates and are subject to revision under a number of circumstances. Our debt consists of borrowings from our senior notes, credit facility, mortgages, construction loan and capital leases. The purchase obligations consist
primarily of software purchase and maintenance contracts. The contractual obligations and estimated period of payment over the next five years and beyond are as follows (in thousands):
|
Payments Due by Period |
||||||||||||||||||||
|
Total |
Less Than
1 Year |
1-3
Years |
3-5
Years |
More Than
5 Years |
||||||||||||||||
|
Medical claims liability |
$ | 470,932 | $ | 470,932 | $ | — | $ | — | $ | — | ||||||||||
|
Debt |
307,731 | 646 | 117,870 | 184,258 | 4,957 | |||||||||||||||
|
Operating lease obligations |
83,350 | 20,527 | 31,314 | 17,070 | 14,439 | |||||||||||||||
|
Purchase obligations |
39,228 | 25,237 | 10,679 | 2,399 | 913 | |||||||||||||||
|
Interest on long-term debt 1 |
57,094 | 12,688 | 25,375 | 19,031 | — | |||||||||||||||
|
Reserve for uncertain tax positions |
3,991 | 2,556 | 685 | 750 | — | |||||||||||||||
|
Other long-term liabilities 2 |
55,569 | — | 14,477 | 5,400 | 35,692 | |||||||||||||||
|
Total |
$ | 1,017,895 | $ | 532,586 | $ | 200,400 | $ | 228,908 | $ | 56,001 | ||||||||||
|
________________________________
1 Interest on $175,000 Senior Notes.
2 Includes $8,932 separate account liabilities from third party reinsurance that will not be settled in cash. | ||||||||||||||||||||
REGULATORY CAPITAL AND DIVIDEND RESTRICTIONS
Our operations are conducted through our subsidiaries. As managed care organizations, these subsidiaries are subject to state regulations that, among other things, require the maintenance of minimum levels of statutory capital, as defined by each state, and restrict the timing, payment and amount of dividends and other distributions
that may be paid to us. Generally, the amount of dividend distributions that may be paid by a regulated subsidiary without prior approval by state regulatory authorities is limited based on the entity’s level of statutory net income and statutory capital and surplus.
Our subsidiaries are required to maintain minimum capital requirements prescribed by various regulatory authorities in each of the states in which we operate. As of December 31, 2009, our subsidiaries, including UHP, had aggregate statutory capital and surplus of $453.2 million, compared with the required minimum aggregate statutory
capital and surplus requirements of $286.5 million and we estimate our Risk Based Capital, or RBC, percentage to be 347% of the Authorized Control Level.
The National Association of Insurance Commissioners has adopted rules which set minimum risk-based capital requirements for insurance companies, managed care organizations and other entities bearing risk for healthcare coverage. As of December 31, 2009, each of our health plans were in compliance with the risk-based capital requirements
enacted in those states.
RECENT ACCOUNTING PRONOUNCEMENTS
Effective January 1, 2009, the Company adopted new guidance related to business combinations. The changes from the previous guidance include, but are not limited to: (1) acquisition costs are recognized separately from the acquisition; (2) known
contractual contingencies at the time of the acquisition are considered part of the liabilities acquired and and measured at their fair value; all other contingencies are part of the liabilities acquired and measured at their fair value only if it is more likely than not that they meet the definition of a liability; (3) contingent consideration based on the outcome of future events is recognized and measured at the time of the acquisition; and (4) business combinations achieved in stages (step acquisitions)
recognize the identifiable assets and liabilities, as well as noncontrolling interest, in the acquiree, at the full amounts of their fair values. The new guidance has been utilized for all acquisitions since January 1, 2009.
Effective January 1, 2009, the Company adopted new guidance related to consolidation and reporting of noncontrolling interest, which requires all entities to report noncontrolling (minority) interests in subsidiaries in the same way, that is, as equity in the consolidated financial statements. Moreover, this guidance eliminates the diversity
that existed in accounting by requiring transactions between an entity and the noncontrolling interest be treated as equity transactions.
In April 2009, new guidance was issued related to the recognition and presentation of other-than-temporary impairments. The guidance applies to fixed maturity securities only and requires separate display of losses related to credit deterioration and losses related to other market factors. When an entity does not intend
to sell the security and it is more likely than not that an entity will not have to sell the security before recovery of its cost basis, it must recognize the credit component of an other-than-temporary impairment in earnings and the remaining portion in other comprehensive income. The adoption of the guidance did not have a material effect on the Company’s financial statements.
In June 2009, new guidance was issued related to the consolidation of variable interest entities to require an analysis to determine whether a variable interest gives the Company a controlling financial interest in a variable interest entity. This guidance requires an ongoing reassessment and eliminates the quantitative approach previously
required for determining whether an entity is the primary beneficiary. This guidance is effective for fiscal years beginning after November 15, 2009 and early adoption is prohibited. The Company is currently evaluating the impact of adopting this guidance on the consolidated financial statements and related disclosures.
We have determined that all other recently issued accounting pronouncements will not have a material impact on our consolidated financial position, results of operations and cash flows, or do not apply to our operations.
CRITICAL ACCOUNTING POLICIES AND ESTIMATES
Our discussion and analysis of our results of operations and liquidity and capital resources are based on our consolidated financial statements which have been prepared in accordance with GAAP. In connection with the preparation of our consolidated financial statements, we are required to make assumptions and estimates about future
events, and apply judgments that affect the reported amounts of assets, liabilities, revenue, expenses, and the related disclosures. We base our assumptions, estimates and judgments on historical experience, current trends and other factors we believe to be relevant at the time we prepared our consolidated financial statements. On a regular basis, we review the accounting policies, assumptions, estimates and judgments to ensure that our consolidated financial statements are presented fairly
and in accordance with GAAP. However, because future events and their effects cannot be determined with certainty, actual results could differ from our assumptions and estimates, and such differences could be material.
The preparation of our consolidated financial statements in conformity with GAAP requires us to make estimates and assumptions. These estimates and assumptions affect the reported amounts of assets and liabilities and the disclosures of contingent assets and liabilities as of the date of the financial statements, and the reported
amounts of revenues and expenses during the reporting periods. Future events and their effects cannot be predicted with certainty, and accordingly, our accounting estimates require the exercise of judgment. The accounting estimates used in the preparation of our consolidated financial statements will change as new events occur, as more experience is acquired, as additional information is obtained and as our operating environment changes. We evaluate and update our assumptions
and estimates on an ongoing basis and may employ outside experts to assist in our evaluations. Actual results could differ from the estimates we have used.
Our significant accounting policies are more fully described in Note 2, Summary of Significant Accounting Policies, to our consolidated financial statements included elsewhere herein. Our accounting policies regarding medical claims liability and intangible assets are particularly
important to the portrayal of our financial position and results of operations and require the application of significant judgment by our management. As a result, they are subject to an inherent degree of uncertainty. We have reviewed these critical accounting policies and related disclosures with the Audit Committee of our board of directors.
Medical claims liability
Our medical claims liability includes claims reported but not yet paid, or inventory, estimates for claims incurred but not reported, or IBNR, and estimates for the costs necessary to process unpaid claims at the end of each period. We estimate our medical claims liability using actuarial methods that are commonly used by health
insurance actuaries and meet Actuarial Standards of Practice. These actuarial methods consider factors such as historical data for payment patterns, cost trends, product mix, seasonality, utilization of healthcare services and other relevant factors.
Actuarial Standards of Practice generally require that the medical claims liability estimates be adequate to cover obligations under moderately adverse conditions. Moderately adverse conditions are situations in which the actual claims are expected to be higher than the otherwise estimated value of such claims at the time of estimate. In
many situations, the claims amounts ultimately settled will be different than the estimate that satisfies the Actuarial Standards of Practice. We include in our IBNR an estimate for medical claims liability under moderately adverse conditions which represents the risk of adverse deviation of the estimates in our actuarial method of reserving.
We use our judgment to determine the assumptions to be used in the calculation of the required estimates. The assumptions we consider when estimating IBNR include, without limitation, claims receipt and payment experience (and variations in that experience), changes in membership,
provider billing practices, healthcare service utilization trends, cost trends, product mix, seasonality, prior authorization of medical services, benefit changes, known outbreaks of disease or increased incidence of illness such as influenza, provider contract changes, changes to Medicaid fee schedules, and the incidence of high dollar or catastrophic claims.
We apply various estimation methods depending on the claim type and the period for which claims are being estimated. For more recent periods, incurred non-inpatient claims are estimated based on historical per member per month claims experience adjusted for known factors. Incurred
hospital inpatient claims are estimated based on known inpatient utilization data and prior claims experience adjusted for known factors. For older periods, we utilize an estimated completion factor based on our historical experience to develop IBNR estimates. The completion factor is an actuarial estimate of the percentage of claims incurred during a given period that have been received or adjudicated as of the reporting period to the estimate of the total ultimate incurred costs. When
we commence operations in a new state or region, we have limited information with which to estimate our medical claims liability. See “Risk Factors – Failure to accurately predict our medical expenses could negatively affect our financial position, results of operations or cash flows.” These approaches are consistently applied to each period presented.
Additionally, we contract with independent actuaries to review our estimates on a quarterly basis. The independent actuaries provide us with a review letter that includes the results of their analysis of our medical claims liability. We do not solely rely on their report
to adjust our claims liability. We utilize their calculation of our claims liability only as additional information, together with management’s judgment to determine the assumptions to be used in the calculation of our liability for claims.
Our development of the medical claims liability estimate is a continuous process which we monitor and refine on a monthly basis as additional claims receipts and payment information becomes available. As more complete claim information becomes available, we adjust the amount of the
estimates, and include the changes in estimates in medical costs in the period in which the changes are identified. In every reporting period, our operating results include the effects of more completely developed medical claims liability estimates associated with previously reported periods. We consistently apply our reserving methodology from period to period. As additional information becomes known to us, we adjust our actuarial model accordingly to establish medical claims
liability estimates.
The paid and received completion factors, claims per member per month and per diem cost trend factors are the most significant factors affecting the IBNR estimate. The following table illustrates the sensitivity of these factors and the estimated potential impact on our operating results caused by changes in these factors based
on December 31, 2009 data:
|
Completion Factors (1): |
|
Cost Trend Factors (2): | |||||||||
|
(Decrease)
Increase
in Factors |
|
Increase
(Decrease) in
Medical Claims
Liabilities |
(Decrease)
Increase
in Factors |
|
Increase
(Decrease) in
Medical Claims
Liabilities | ||||||
|
|
(in thousands) |
|
(in thousands) | ||||||||
|
(2.0 |
)% |
$ |
53,700 |
(2.0 |
)% |
$ |
(14,600 |
) | |||
|
(1.5 |
) |
|
39,900 |
(1.5 |
) |
(10,900 |
) | ||||
|
(1.0 |
) |
|
26,400 |
(1.0 |
) |
(7,200 |
) | ||||
|
(0.5 |
) |
|
13,300 |
(0.5 |
) |
(3,700 |
) | ||||
|
0.5 |
|
(13,000 |
) |
0.5 |
3,700 |
||||||
|
1.0 |
|
(26,000 |
) |
1.0 |
7,300 |
||||||
|
1.5 |
|
(38,800 |
) |
1.5 |
11,000 |
||||||
|
2.0 |
|
(51,400 |
) |
2.0 |
14,800 |
||||||
|
(1) |
Reflects estimated potential changes in medical claims liability caused by changes in completion factors. |
|
(2) |
Reflects estimated potential changes in medical claims liability caused by changes in cost trend factors for the most recent periods. |
While we believe our estimates are appropriate, it is possible future events could require us to make significant adjustments for revisions to these estimates. For example, a 1% increase or decrease in our estimated medical claims liability would have affected net earnings by $3.0 million for the year ended December 31, 2009. The
estimates are based on our historical experience, terms of existing contracts, our observance of trends in the industry, information provided by our providers and information available from other outside sources.
The change in medical claims liability is summarized as follows (in thousands):
|
|
Year Ended December 31, |
|||||||||||
|
|
2009 |
2008 |
2007 |
|||||||||
|
Balance, January 1 |
|
$ |
384,360 |
$ |
323,741 |
$ |
241,073 |
|||||
|
Acquisitions |
|
— |
15,398 |
— |
||||||||
|
Incurred related to: |
|
|||||||||||
|
Current year |
|
3,216,533 |
2,659,036 |
2,212,901 |
||||||||
|
Prior years |
|
(53,010 |
) |
(18,701 |
) |
(22,003 |
) | |||||
|
Total incurred |
|
3,163,523 |
2,640,335 |
2,190,898 |
||||||||
|
Paid related to: |
|
|||||||||||
|
Current year |
|
2,752,983 |
2,292,150 |
1,892,233 |
||||||||
|
Prior years |
|
323,968 |
302,964 |
215,997 |
||||||||
|
Total paid |
|
3,076,951 |
2,595,114 |
2,108,230 |
||||||||
|
Balance, December 31 |
|
$ |
470,932 |
$ |
384,360 |
$ |
323,741 |
|||||
|
|
||||||||||||
|
Claims inventory, December 31 |
|
423,400 |
269,300 |
323,200 |
||||||||
|
Days in claims payable 1 |
|
50.1 |
49.9 |
49.9 |
||||||||
|
________________________
1 Days in claims payable is a calculation of medical claims liability at the end of the period divided by average expense per calendar day for the fourth quarter of each year. | ||||||||||||
The acquisition in 2008 includes reserves acquired in connection with our acquisition of Celtic.
Medical claims are usually paid within a few months of the member receiving service from the physician or other healthcare provider. As a result, the liability generally is described as having a “short-tail,” which causes less than 5% of our medical claims liability as of the end of any given year to be outstanding
the following year. We believe that substantially all the development of the estimate of medical claims liability as of December 31, 2009 will be known by the end of 2010.
Changes in estimates of incurred claims for prior years are primarily attributable to reserving under moderately adverse conditions. In addition, claims processing initiatives yielded increased claim payment recoveries and coordination of benefits related to prior year dates of service. Changes in medical utilization
and cost trends and the effect of medical management initiatives may also contribute to changes in medical claim liability estimates. While we have evidence that medical management initiatives are effective on a case by case basis, medical management initiatives primarily focus on events and behaviors prior to the incurrence of the medical event and generation of a claim. Accordingly, any change in behavior, leveling of care, or coordination of treatment occurs prior to claim generation
and as a result, the costs prior to the medical management initiative are not known by us. Additionally, certain medical management initiatives are focused on member and provider education with the intent of influencing behavior to appropriately align the medical services provided with the member’s acuity. In these cases, determining whether the medical management initiative changed the behavior cannot be determined. Because of the complexity of our business, the number
of states in which we operate, and the volume of claims that we process, we are unable to practically quantify the impact of these initiatives on our changes in estimates of IBNR.
The following medical management initiatives may have contributed to the favorable development through lower medical utilization and cost trends:
|
· |
Appropriate leveling of care for neonatal intensive care unit hospital admissions, other inpatient hospital admissions, and observation admissions, in accordance with Interqual criteria. |
|
· |
Tightening of our pre-authorization list and more stringent review of durable medical equipment and injectibles. |
|
· |
Emergency department, or ED, program designed to collaboratively work with hospitals to steer non-emergency care away from the costly ED setting (through patient education, on-site alternative urgent care settings, etc.) |
|
· |
Increase emphasis on case management and clinical rounding where case managers are nurses or social workers who are employed by the health plan to assist selected patients with the coordination of healthcare services in order to meet a patient's specific healthcare needs. |
|
· |
Incorporation of disease management which is a comprehensive, multidisciplinary, collaborative approach to chronic illnesses such as asthma. |
Goodwill and Intangible Assets
We have made several acquisitions that have resulted in our recording of intangible assets. These intangible assets primarily consist of customer relationships, purchased contract rights, provider contracts, trade names and goodwill. At December 31, 2009, we had $224.6 million of goodwill and $22.5 million of other intangible
assets.
Intangible assets are amortized using the straight-line method over the following periods:
|
Intangible Asset |
Amortization Period | |
|
Purchased contract rights |
5 – 10 years | |
|
Provider contracts |
5 – 10 years | |
|
Customer relationships |
5 – 15 years | |
|
Trade names |
15 – 20 years |
Our management evaluates whether events or circumstances have occurred that may affect the estimated useful life or the recoverability of the remaining balance of goodwill and other identifiable intangible assets. If the events or circumstances indicate that the remaining balance of the intangible asset or goodwill may be impaired,
the potential impairment will be measured based upon the difference between the carrying amount of the intangible asset or goodwill and the fair value of such asset. Our management must make assumptions and estimates, such as the discount factor, future utility and other internal and external factors, in determining the estimated fair values. While we believe these assumptions and estimates are appropriate, other assumptions and estimates could be applied and might produce significantly
different results.
Goodwill is reviewed every year during the fourth quarter for impairment. In addition, an impairment analysis of intangible assets would be performed based on other factors. These factors include significant changes in membership, state funding, medical contracts and provider networks and contracts.
Item 7A. Quantitative and Qualitative Disclosures About Market Risk
INVESTMENTS
As of December 31, 2009, we had short-term investments of $39.6 million and long-term investments of $545.6 million, including restricted deposits of $20.1 million. The short-term investments generally consist of highly liquid securities with maturities between three and 12 months. The long-term investments consist of
municipal, corporate and U.S. Agency bonds, life insurance contracts, U.S. Treasury investments, asset backed securities and equity securities and have maturities greater than one year. Restricted deposits consist of investments required by various state statutes to be deposited or pledged to state agencies. Due to the nature of the states’ requirements, these investments are classified as long-term regardless of the contractual maturity date. Our investments are subject
to interest rate risk and will decrease in value if market rates increase. Assuming a hypothetical and immediate 1% increase in market interest rates at December 31, 2009, the fair value of our fixed income investments would decrease by approximately $13.5 million. Declines in interest rates over time will reduce our investment income. For a discussion of the interest rate risk that our investments are subject to, see "Risk Factors–Risks Related to Our Business–Our
investment portfolio may suffer losses from reductions in market interest rates and changes in market conditions which could materially and adversely affect our results of operations or liquidity.”
INFLATION
While the inflation rate in 2009 for medical care costs was slightly less than that for all items, historically inflation for medical care costs has generally exceeded that for all items. We use various strategies to mitigate the negative effects of healthcare cost inflation. Specifically, our health
plans try to control medical and hospital costs through our state savings initiatives and contracts with independent providers of healthcare services. Through these contracted care providers, our health plans emphasize preventive healthcare and appropriate use of specialty and hospital services.
While we currently believe our strategies to mitigate healthcare cost inflation will continue to be successful, competitive pressures, new healthcare and pharmaceutical product introductions, demands from healthcare providers and customers, applicable regulations or other factors may affect our ability to control the impact of healthcare
cost increases.
Item 8. Financial Statements and Supplementary Data
Report of Independent Registered Public Accounting Firm
The Board of Directors and Stockholders
Centene Corporation:
We have audited the accompanying consolidated balance sheets of Centene Corporation and subsidiaries as of December 31, 2009 and 2008, and the related consolidated statements of operations, stockholders’ equity, and cash flows for each of the years in the three-year period ended December 31, 2009. These consolidated financial statements
are the responsibility of the Company’s management. Our responsibility is to express an opinion on these consolidated financial statements based on our audits.
We conducted our audits in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether the financial statements are free of material misstatement. An audit includes examining, on
a test basis, evidence supporting the amounts and disclosures in the financial statements. An audit also includes assessing the accounting principles used and significant estimates made by management, as well as evaluating the overall financial statement presentation. We believe that our audits provide a reasonable basis for our opinion.
In our opinion, the consolidated financial statements referred to above present fairly, in all material respects, the financial position of Centene Corporation and subsidiaries as of December 31, 2009 and 2008, and the results of their operations and their cash flows for each of the years in the three-year period ended December 31, 2009, in
conformity with U.S. generally accepted accounting principles.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States), Centene Corporation’s internal control over financial reporting as of December 31, 2009, based on criteria established in Internal Control - Integrated Framework issued
by the Committee of Sponsoring Organizations of the Treadway Commission (COSO), and our report dated February 21, 2010 expressed an unqualified opinion on the effectiveness of the operation of internal control over financial reporting.
KPMG LLP
St. Louis, Missouri
February 21, 2010
CENTENE CORPORATION AND SUBSIDIARIES
CONSOLIDATED BALANCE SHEETS
(In thousands, except share data)
|
December 31,
2009 |
December 31,
2008 |
|||||||
|
ASSETS |
||||||||
|
Current assets: |
||||||||
|
Cash and cash equivalents of continuing operations |
$ | 400,951 | $ | 370,999 | ||||
|
Cash and cash equivalents of discontinued operations |
2,801 | 8,100 | ||||||
|
Total cash and cash equivalents |
403,752 | 379,099 | ||||||
|
Premium and related receivables, net of allowance for uncollectible accounts of $1,338 and $1,304, respectively |
103,456 | 92,531 | ||||||
|
Short-term investments, at fair value (amortized cost $39,230 and $108,469, respectively) |
39,554 | 109,393 | ||||||
|
Other current assets |
64,866 | 75,333 | ||||||
|
Current assets of discontinued operations other than cash |
4,506 | 9,987 | ||||||
|
Total current assets |
616,134 | 666,343 | ||||||
|
Long-term investments, at fair value (amortized cost $514,256 and $329,330, respectively) |
525,497 | 332,411 | ||||||
|
Restricted deposits, at fair value (amortized cost $20,048 and $9,124, respectively) |
20,132 | 9,254 | ||||||
|
Property, software and equipment, net of accumulated depreciation of $103,883 and $74,194, respectively |
230,421 | 175,858 | ||||||
|
Goodwill |
224,587 | 163,380 | ||||||
|
Intangible assets, net |
22,479 | 17,575 | ||||||
|
Other long-term assets |
36,829 | 59,083 | ||||||
|
Long-term assets of discontinued operations |
26,285 | 27,248 | ||||||
|
Total assets |
$ | 1,702,364 | $ | 1,451,152 | ||||
|
LIABILITIES AND STOCKHOLDERS’ EQUITY |
||||||||
|
Current liabilities: |
||||||||
|
Medical claims liability |
$ | 470,932 | $ | 384,360 | ||||
|
Accounts payable and accrued expenses |
132,001 | 208,243 | ||||||
|
Unearned revenue |
91,644 | 17,107 | ||||||
|
Current portion of long-term debt |
646 | 255 | ||||||
|
Current liabilities of discontinued operations |
20,685 | 31,013 | ||||||
|
Total current liabilities |
715,908 | 640,978 | ||||||
|
Long-term debt |
307,085 | 264,637 | ||||||
|
Other long-term liabilities |
59,561 | 43,539 | ||||||
|
Long-term liabilities of discontinued operations |
383 | 726 | ||||||
|
Total liabilities |
1,082,937 | 949,880 | ||||||
|
Commitments and contingencies |
||||||||
|
Stockholders’ equity: |
||||||||
|
Common stock, $.001 par value; authorized 100,000,000 shares; issued and outstanding 45,593,383 and 45,071,179 shares, respectively |
46 | 45 | ||||||
|
Additional paid-in capital |
281,806 | 263,835 | ||||||
|
Accumulated other comprehensive income: |
||||||||
|
Unrealized gain on investments, net of tax |
7,348 | 3,152 | ||||||
|
Retained earnings |
358,907 | 275,236 | ||||||
|
Treasury stock, at cost (2,414,010 and 2,083,415 shares, respectively) |
(47,262 | ) | (40,996 | ) | ||||
|
Total Centene stockholders’ equity |
600,845 | 501,272 | ||||||
|
Noncontrolling interest |
18,582 | — | ||||||
|
Total stockholders’ equity |
619,427 | 501,272 | ||||||
|
Total liabilities and stockholders’ equity |
$ | 1,702,364 | $ | 1,451,152 | ||||
The accompanying notes to the consolidated financial statements are an integral part of these statements.
CENTENE CORPORATION AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF OPERATIONS
(In thousands, except share data)
|
Year Ended December 31, |
||||||||||||
|
|
2009 |
2008 |
2007 |
|||||||||
|
Revenues: |
|
|||||||||||
|
Premium |
|
$ |
3,786,525 |
$ |
3,199,360 |
$ |
2,611,953 |
|||||
|
Service |
|
91,758 |
74,953 |
80,508 |
||||||||
|
Premium and service revenues |
3,878,283 |
3,274,313 |
2,692,461 |
|||||||||
|
Premium tax |
224,581 |
90,202 |
76,567 |
|||||||||
|
Total revenues |
|
4,102,864 |
3,364,515 |
2,769,028 |
||||||||
|
Expenses: |
|
|||||||||||
|
Medical costs |
|
3,163,523 |
2,640,335 |
2,190,898 |
||||||||
|
Cost of services |
|
60,789 |
56,920 |
61,348 |
||||||||
|
General and administrative expenses |
|
514,529 |
444,733 |
384,970 |
||||||||
|
Premium tax expense |
225,888 |
90,966 |
76,567 |
|||||||||
|
Total operating expenses |
|
3,964,729 |
3,232,954 |
2,713,783 |
||||||||
|
Earnings from operations |
|
138,135 |
131,561 |
55,245 |
||||||||
|
Other income (expense): |
|
|||||||||||
|
Investment and other income |
|
15,691 |
21,728 |
24,452 |
||||||||
|
Interest expense |
|
(16,318 |
) |
(16,673 |
) |
(15,626 |
) | |||||
|
Earnings from continuing operations, before income tax expense |
|
137,508 |
136,616 |
64,071 |
||||||||
|
Income tax expense |
|
48,841 |
52,435 |
23,031 |
||||||||
|
Earnings from continuing operations, net of income tax expense |
88,667 |
84,181 |
41,040 |
|||||||||
|
Discontinued operations, net of income tax benefit of $(1,204), $(281) and $(31,563), respectively |
(2,422 |
) |
(684 |
) |
32,362 |
|||||||
|
Net earnings |
86,245 |
83,497 |
73,402 |
|||||||||
|
Noncontrolling interest |
2,574 |
— |
— |
|||||||||
|
Net earnings attributable to Centene Corporation |
|
$ |
83,671 |
$ |
83,497 |
$ |
73,402 |
|||||
|
Amounts attributable to Centene Corporation common shareholders: |
||||||||||||
|
Earnings from continuing operations, net of income tax expense |
$ |
86,093 |
$ |
84,181 |
$ |
41,040 |
||||||
|
Discontinued operations, net of income tax (benefit) expense |
(2,422 |
) |
(684 |
) |
32,362 |
|||||||
|
Net earnings |
$ |
83,671 |
$ |
83,497 |
$ |
73,402 |
||||||
|
Net earnings (loss) per common share attributable to Centene Corporation: |
|
|||||||||||
|
Basic: |
||||||||||||
|
Continuing operations |
|
$ |
2.00 |
$ |
1.95 |
$ |
0.95 |
|||||
|
Discontinued operations |
|
(0.06 |
) |
(0.02 |
) |
0.74 |
||||||
|
Basic earnings per common share |
|
$ |
1.94 |
$ |
1.93 |
$ |
1.69 |
|||||
|
Diluted: |
|
|||||||||||
|
Continuing operations |
|
$ |
1.94 |
$ |
1.90 |
$ |
0.92 |
|||||
|
Discontinued operations |
|
(0.05 |
) |
(0.02 |
) |
0.72 |
||||||
|
Diluted earnings per common share |
|
$ |
1.89 |
$ |
1.88 |
$ |
1.64 |
|||||
|
Weighted average number of common shares outstanding: |
|
|||||||||||
|
Basic |
|
43,034,791 |
43,275,187 |
43,539,950 |
||||||||
|
Diluted |
|
44,316,467 |
44,398,955 |
44,823,082 |
||||||||
The accompanying notes to the consolidated financial statements are an integral part of these statements
CENTENE CORPORATION AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF STOCKHOLDERS’ EQUITY
(In thousands, except share data)
|
Centene Stockholders’ Equity |
||||||||||||||||||||||||||||||
|
Common Stock |
Treasury Stock |
|||||||||||||||||||||||||||||
|
$.001 Par
Value
Shares |
Amt |
Additional
Paid-in
Capital |
Accumulated
Other
Comprehensive
Income |
Retained
Earnings |
$.001 Par
Value
Shares |
Amt |
Non
controlling
Interest |
Total |
||||||||||||||||||||||
|
Balance, December 31, 2006 |
43,766,688 |
$ |
44 |
$ |
217,284 |
$ |
(1,251) |
$ |
118,290 |
397,400 |
$ |
(7,944) |
$ |
— |
$ |
326,423 |
||||||||||||||
|
Comprehensive Earnings: |
||||||||||||||||||||||||||||||
|
Net earnings |
— |
— |
— |
— |
73,402 |
— |
— |
— |
73,402 |
|||||||||||||||||||||
|
Change in unrealized investment losses, net of $1,625 tax |
— |
— |
— |
2,822 |
— |
— |
— |
— |
2,822 |
|||||||||||||||||||||
|
Total comprehensive earnings |
— |
— |
— |
— |
— |
— |
— |
— |
76,224 |
|||||||||||||||||||||
|
Common stock issued for employee benefit plans |
765,706 |
1 |
6,113 |
— |
— |
— |
— |
— |
6,114 |
|||||||||||||||||||||
|
Common stock repurchases |
— |
— |
— |
— |
— |
467,157 |
(9,542) |
— |
(9,542 |
) | ||||||||||||||||||||
|
Stock compensation expense |
— |
— |
15,781 |
— |
— |
— |
— |
— |
15,781 |
|||||||||||||||||||||
|
Adjustment for reserve for uncertain tax positions |
47 |
47 |
||||||||||||||||||||||||||||
|
Balance, December 31, 2007 |
44,532,394 |
$ |
45 |
$ |
239,178 |
$ |
1,571 |
$ |
191,739 |
864,557 |
$ |
(17,486) |
$ |
— |
$ |
415,047 |
||||||||||||||
|
Comprehensive Earnings: |
||||||||||||||||||||||||||||||
|
Net earnings |
— |
— |
— |
— |
83,497 |
— |
— |
— |
83,497 |
|||||||||||||||||||||
|
Change in unrealized investment gains, net of $882 tax |
— |
— |
— |
1,581 |
— |
— |
— |
— |
1,581 |
|||||||||||||||||||||
|
Total comprehensive earnings |
— |
— |
— |
— |
— |
— |
— |
— |
85,078 |
|||||||||||||||||||||
|
Common stock issued for employee benefit plans |
538,785 |
— |
6,229 |
— |
— |
— |
— |
— |
6,229 |
|||||||||||||||||||||
|
Common stock repurchases |
— |
— |
— |
— |
— |
1,218,858 |
(23,510) |
— |
(23,510 |
) | ||||||||||||||||||||
|
Stock compensation expense |
— |
— |
15,328 |
— |
— |
— |
— |
— |
15,328 |
|||||||||||||||||||||
|
Excess tax benefits from stock compensation |
3,100 |
3,100 |
||||||||||||||||||||||||||||
|
Balance, December 31, 2008 |
45,071,179 |
$ |
45 |
$ |
263,835 |
$ |
3,152 |
$ |
275,236 |
2,083,415 |
$ |
(40,996) |
$ |
— |
$ |
501,272 |
||||||||||||||
|
Consolidation of Access Health Solutions LLC |
— |
— |
— |
— |
— |
— |
— |
29,144 |
29,144 |
|||||||||||||||||||||
|
Consolidation of Centene Center LLC |
— |
— |
— |
— |
— |
— |
— |
17,400 |
17,400 |
|||||||||||||||||||||
|
Comprehensive Earnings: |
||||||||||||||||||||||||||||||
|
Net earnings |
— |
— |
— |
— |
83,671 |
— |
— |
2,574 |
86,245 |
|||||||||||||||||||||
|
Change in unrealized investment gains, net of $2,663 tax |
— |
— |
— |
4,196 |
— |
— |
— |
— |
4,196 |
|||||||||||||||||||||
|
Total comprehensive earnings |
90,441 |
|||||||||||||||||||||||||||||
|
Common stock issued for employee benefit plans |
522,204 |
1 |
3,284 |
— |
— |
— |
— |
3,285 |
||||||||||||||||||||||
|
Common stock repurchases |
— |
— |
— |
— |
— |
332,595 |
(6,304) |
— |
(6,304 |
) | ||||||||||||||||||||
|
Treasury stock issued for compensation |
— |
— |
— |
— |
(2,000) |
38 |
38 |
|||||||||||||||||||||||
|
Stock compensation expense |
— |
— |
14,634 |
— |
— |
— |
— |
— |
14,634 |
|||||||||||||||||||||
|
Excess tax benefits from stock compensation |
— |
— |
53 |
— |
— |
— |
— |
— |
53 |
|||||||||||||||||||||
|
Conversion fee1 |
— |
— |
— |
— |
— |
— |
— |
(27,366) |
(27,366 |
) | ||||||||||||||||||||
|
Distributions to noncontrolling interest |
— |
— |
— |
— |
— |
— |
— |
(3,170) |
(3,170 |
) | ||||||||||||||||||||
|
Balance, December 31, 2009 |
45,593,383 |
$ |
46 |
$ |
281,806 |
$ |
7,348 |
$ |
358,907 |
2,414,010 |
$ |
(47,262) |
$ |
18,582 |
$ |
619,427 |
||||||||||||||
|
(1) |
Conversion fee represents additional purchase price to noncontrolling holders of Access Health Solutions LLC for the transfer of membership to the Company’s wholly-owned subsidiary, Sunshine State Health Plan, Inc. |
The accompanying notes to the consolidated financial statements are an integral part of these statements.
CENTENE CORPORATION AND SUBSIDIARIES
CONSOLIDATED STATEMENTS OF CASH FLOWS
(In thousands)
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Cash flows from operating activities: |
||||||||||||
|
Net earnings |
$ |
86,245 |
$ |
83,497 |
$ |
73,402 |
||||||
|
Adjustments to reconcile net earnings to net cash provided by operating activities: |
||||||||||||
|
Depreciation and amortization |
44,004 |
35,414 |
27,807 |
|||||||||
|
Stock compensation expense |
14,634 |
15,328 |
15,781 |
|||||||||
|
(Gain) loss on sale of investments, net |
(141 |
) |
4,988 |
106 |
||||||||
|
Gain on sale of FirstGuard Missouri |
— |
— |
(7,472 |
) | ||||||||
|
Impairment loss |
— |
2,546 |
7,207 |
|||||||||
|
Deferred income taxes |
3,696 |
1,286 |
(10,223 |
) | ||||||||
|
Changes in assets and liabilities: |
||||||||||||
|
Premium and related receivables |
2,379 |
(1,548 |
) |
1,663 |
||||||||
|
Other current assets |
(1,263 |
) |
(4,244 |
) |
(6,253 |
) | ||||||
|
Other assets |
9 |
(2,700 |
) |
(348 |
) | |||||||
|
Medical claims liability |
79,000 |
47,283 |
58,088 |
|||||||||
|
Unearned revenue |
78,345 |
(36,447 |
) |
10,085 |
||||||||
|
Accounts payable and accrued expenses |
(60,915 |
) |
74,166 |
29,433 |
||||||||
|
Other operating activities |
2,202 |
2,409 |
2,964 |
|||||||||
|
Net cash provided by operating activities |
248,195 |
221,978 |
202,240 |
|||||||||
|
Cash flows from investing activities: |
||||||||||||
|
Capital expenditures |
(83,113 |
) |
(65,156 |
) |
(53,937 |
) | ||||||
|
Purchase of investments |
(791,194 |
) |
(549,652 |
) |
(606,366 |
) | ||||||
|
Sales and maturities of investments |
642,783 |
546,264 |
456,738 |
|||||||||
|
Proceeds from asset sales |
— |
— |
14,102 |
|||||||||
|
Investments in acquisitions, net of cash acquired, and investment in equity method investee |
(38,563 |
) |
(85,377 |
) |
(36,001 |
) | ||||||
|
Net cash used in investing activities |
(270,087 |
) |
(153,921 |
) |
(225,464 |
) | ||||||
|
Cash flows from financing activities: |
||||||||||||
|
Proceeds from exercise of stock options |
2,365 |
5,354 |
5,464 |
|||||||||
|
Proceeds from borrowings |
659,059 |
236,005 |
212,000 |
|||||||||
|
Payment of long-term debt |
(616,219 |
) |
(178,491 |
) |
(181,981 |
) | ||||||
|
Distributions to noncontrolling interest |
(3,170 |
) |
— |
— |
||||||||
|
Contribution from noncontrolling interest |
11,219 |
— |
— |
|||||||||
|
Excess tax benefits from stock compensation |
53 |
3,100 |
— |
|||||||||
|
Common stock repurchases |
(6,304 |
) |
(23,510 |
) |
(9,541 |
) | ||||||
|
Debt issue costs |
(458 |
) |
— |
(5,181 |
) | |||||||
|
Net cash provided by financing activities |
46,545 |
42,458 |
20,761 |
|||||||||
|
Net increase (decrease) in cash and cash equivalents |
24,653 |
110,515 |
(2,463 |
) | ||||||||
|
Cash and cash equivalents, beginning of period |
379,099 |
268,584 |
271,047 |
|||||||||
|
Cash and cash equivalents, end of period |
$ |
403,752 |
$ |
379,099 |
$ |
268,584 |
||||||
|
Supplemental disclosures of cash flow information: |
||||||||||||
|
Interest paid |
$ |
15,428 |
$ |
15,312 |
$ |
11,945 |
||||||
|
Income taxes paid |
$ |
52,928 |
$ |
36,801 |
$ |
7,348 |
||||||
|
Supplemental disclosure of non-cash investing and financing activities: |
||||||||||||
|
Contribution from noncontrolling interest |
$ |
5,875 |
$ |
— |
$ |
— |
||||||
|
Property acquired under capital lease obligation |
— |
— |
1,736 |
|||||||||
The accompanying notes to the consolidated financial statements are an integral part of these statements.
CENTENE CORPORATION AND SUBSIDIARIES
NOTES TO CONSOLIDATED FINANCIAL STATEMENTS
(Dollars in thousands, except share data)
1. Organization and Operations
Centene Corporation, or the Company (or “us”, “we”, “our”), is a multi-line healthcare enterprise operating in two segments: Medicaid Managed Care and Specialty Services. The Medicaid Managed Care segment provides Medicaid and Medicaid-related health plan coverage to individuals through government
subsidized programs, including Medicaid, the State Children’s Health Insurance Program, or CHIP, Foster Care, Medicare Special Needs Plans and the Supplemental Security Income Program, also known as the Aged, Blind or Disabled Program, or collectively ABD. The health plans in Florida, Georgia, Indiana, Ohio, South Carolina, Texas and Wisconsin are included in the Medicaid Managed Care segment. The Specialty Services segment provides specialty services, including behavioral health,
individual health insurance, life and health management, long-term care programs, managed vision, telehealth services, and pharmacy benefits management to state programs, healthcare organizations, employer groups and other commercial organizations, as well as to our own subsidiaries. The health plans in Arizona, which is operated by our long-term care company, and Massachusetts, which is operated by our individual health insurance provider, are included in the Specialty Services segment. The
Specialty Services segment also provides a full range of healthcare solutions for the rising number of uninsured Americans.
2. Summary of Significant Accounting Policies
Principles of Consolidation
The accompanying consolidated financial statements include the accounts of Centene Corporation and all majority owned subsidiaries, majority-owned subsidiaries over which the Company exercises control and entities in which the Company has a controlling financial interest. All material intercompany balances and transactions have
been eliminated. As discussed below in Note 3, Discontinued Operations: University Health Plans and FirstGuard Health Plans, the assets, liabilities and results of operations of FirstGuard Kansas, FirstGuard Missouri and University Health Plans are classified as discontinued operations for all periods presented.
Beginning January 1, 2009, the Company has presented the investment in Access Health Solutions LLC, or Access, as a consolidated subsidiary in its financial statements. Prior to January 1, 2009, Access had been recorded under the equity method of accounting. We determined that we should have accounted for our investment
in Access as a consolidated subsidiary since July 1, 2007. The impact of the difference in presentation is not material to our financial statements for any period. As a result of the presentation of Access as a consolidated subsidiary beginning January 1, 2009, cash flows from investing activities increased by $4,839 to reflect the cash held by Access on January 1, 2009. The noncontrolling interest of Access is presented within stockholders’ equity.
The Company uses the cost method to account for its investment in entities that it does not control and for which it does not have the ability to exercise significant influence over operating and financial policies. These investments are recorded at the lower of their cost or fair value.
Use of Estimates
The preparation of financial statements in conformity with generally accepted accounting principles in the United States, or GAAP, requires management to make estimates and assumptions that affect the reported amounts of assets and liabilities and disclosure of contingent assets and liabilities at the date of the financial statements and
the reported amounts of revenues and expenses during the reporting period. Future events and their effects cannot be predicted with certainty; accordingly, the accounting estimates require the exercise of judgment. The accounting estimates used in the preparation of the consolidated financial statements will change as new events occur, as more experience is acquired, as additional information is obtained and as the operating environment changes. The Company evaluates and updates
its assumptions and estimates on an ongoing basis and may employ outside experts to assist in our evaluation, as considered necessary. Actual results could differ from those estimates.
Cash and Cash Equivalents
Investments with original maturities of three months or less are considered to be cash equivalents. Cash equivalents consist of commercial paper, money market funds, repurchase agreements and bank certificates of deposit and savings accounts.
The Company maintains amounts on deposit with various financial institutions, which may exceed federally insured limits. However, management periodically evaluates the credit-worthiness of those institutions, and the Company has not experienced any losses on such deposits.
Investments
Short-term investments include securities with maturities between three months and one year. Long-term investments include securities with maturities greater than one year.
Short-term and long-term investments are generally classified as available for sale and are carried at fair value. Certain equity investments are recorded using the cost method. Unrealized gains and losses on investments available for sale are excluded from earnings and reported in accumulated other comprehensive income, a
separate component of stockholders’ equity, net of income tax effects. Premiums and discounts are amortized or accreted over the life of the related security using the effective interest method. The Company monitors the difference between the cost and fair value of investments. Investments that experience a decline in value that is judged to be other than temporary are written down to fair value and a realized loss is recorded in investment and other income. To
calculate realized gains and losses on the sale of investments, the Company uses the specific amortized cost of each investment sold. Realized gains and losses are recorded in investment and other income.
Restricted Deposits
Restricted deposits consist of investments required by various state statutes to be deposited or pledged to state agencies. These investments are classified as long-term, regardless of the contractual maturity date, due to the nature of the states’ requirements. The Company is required to annually adjust the amount
of the deposit pledged to certain states.
Fair Value Measurements
In the normal course of business, the Company invests in various financial assets and incurs various financial liabilities. Fair values are disclosed for all financial instruments, whether or not such values are recognized in the Consolidated Balance Sheets. Management obtains quoted market prices and other observable inputs
for these disclosures. The carrying amounts reported in the Consolidated Balance Sheets for cash and cash equivalents, premium and related receivables, unearned revenue, accounts payable and accrued expenses, and certain other current liabilities approximate fair value because of their short-term nature.
The following methods and assumptions were used to estimate the fair value of each financial instrument:
|
· |
Available-for-sale investments and restricted deposits: The carrying amount is stated at fair value, based on quoted market prices, where available. For securities not actively traded, fair values were estimated using values obtained from independent pricing services or quoted market prices of comparable instruments. |
|
· |
Senior unsecured notes: Estimated based on third-party quoted market prices for the same or similar issues. |
|
· |
Variable rate debt: The carrying amount of our floating rate debt approximates fair value because the interest rates adjust based on market rate adjustments. |
Additional information regarding fair value measurements is included in Note 8, Fair Value Measurements.
Property, Software and Equipment
Property, software and equipment are stated at cost less accumulated depreciation. Capitalized software includes certain costs incurred in the development of internal-use software, including external direct costs of materials and services and payroll costs of employees devoted to specific software development. Depreciation
is calculated principally by the straight-line method over estimated useful lives. Leasehold improvements are depreciated using the straight-line method over the shorter of the expected useful life or the remaining term of the lease. Property, software and equipment are depreciated over the following periods:
|
Fixed Asset |
Depreciation Period | |
|
Buildings |
40 years | |
|
Computer hardware and software |
3 – 7 years | |
|
Furniture and equipment |
5 – 7 years | |
|
Leasehold improvements |
1– 10 years |
The carrying amounts of all long-lived assets are evaluated to determine if adjustment to the depreciation and amortization period or to the unamortized balance is warranted. Such evaluation is based principally on the expected utilization of the long-lived assets.
The Company retains fully depreciated assets in property and accumulated depreciation accounts until it removes them from service. In the case of sale, retirement, or disposal, the asset cost and related accumulated depreciation balance is removed from the respective account, and the resulting net amount, less any proceeds, is
included as a component of earnings from operations in the consolidated statements of operations.
The Company tests for impairment of long-lived assets, including intangible assets, whenever events or changes in circumstances indicate that the carrying value of an asset or asset group (hereinafter referred to as “asset group”) may not be recoverable by comparing the sum of the estimated undiscounted future cash flows expected
to result from use of the asset group and its eventual disposition to the carrying value. Such factors include, but are not limited to, significant changes in membership, state funding, state contracts and provider networks and contracts. If the sum of the estimated undiscounted future cash flows is less than the carrying value, an impairment determination is required. The amount of impairment is calculated by subtracting the fair value of the asset group from the carrying value
of the asset group. An impairment charge, if any, is recognized within earnings from operations.
Goodwill and Intangible Assets
Intangible assets represent assets acquired in purchase transactions and consist primarily of customer relationships, purchased contract rights, provider contracts, trade names and goodwill. Intangible assets are amortized using the straight-line method over the following periods:
|
Intangible Asset |
Amortization Period | |
|
Purchased contract rights |
5 – 10 years | |
|
Provider contracts |
5 – 10 years | |
|
Customer relationships |
5 – 15 years | |
|
Trade names |
15 – 20 years |
The Company tests goodwill for impairment using a fair value approach. The Company is required to test for impairment at least annually, absent some triggering event that would require an impairment assessment. Absent any impairment indicators, the Company performs its goodwill impairment testing during the fourth quarter
of each year.
The Company recognizes an impairment charge for any amount by which the carrying amount of goodwill exceeds its implied fair value. The Company presents a goodwill impairment charge as a separate line item within earnings from operations in the consolidated statements of operations, unless the goodwill impairment is associated
with a discontinued operation. In that case, the Company includes the goodwill impairment charge, on a net-of-tax basis, within the results of discontinued operations.
The Company uses discounted cash flows to establish the fair value as of the testing date. The discounted cash flow approach includes many assumptions related to future growth rates, discount factors, future tax rates, etc. Changes in economic and operating conditions impacting these assumptions could result in goodwill
impairment in future periods. When available and as appropriate, the Company uses comparative market multiples to corroborate discounted cash flow results.
Medical Claims Liability
Medical claims liability includes claims reported but not yet paid, or inventory, estimates for claims incurred but not reported, or IBNR, and estimates for the costs necessary to process unpaid claims at the end of each period. The Company estimates its medical claims liability using actuarial methods that are commonly used by
health insurance actuaries and meet Actuarial Standards of Practice. These actuarial methods consider factors such as historical data for payment patterns, cost trends, product mix, seasonality, utilization of healthcare services and other relevant factors.
Actuarial Standards of Practice generally require that the medical claims liability estimates be adequate to cover obligations under moderately adverse conditions. Moderately adverse conditions are situations in which the actual claims are expected to be higher than the otherwise estimated value of such claims at the time of estimate. In
many situations, the claims amounts ultimately settled will be different than the estimate that satisfies the Actuarial Standards of Practice. The Company includes in its IBNR an estimate for medical claims liability under moderately adverse conditions which represents the risk of adverse deviation of the estimates in its actuarial method of reserving.
The Company uses its judgment to determine the assumptions to be used in the calculation of the required estimates. The assumptions it considers when estimating IBNR include, without limitation, claims receipt and payment experience (and variations in that experience), changes in
membership, provider billing practices, healthcare service utilization trends, cost trends, product mix, seasonality, prior authorization of medical services, benefit changes, known outbreaks of disease or increased incidence of illness such as influenza, provider contract changes, changes to Medicaid fee schedules, and the incidence of high dollar or catastrophic claims.
The Company’s development of the medical claims liability estimate is a continuous process which it monitors and refines on a monthly basis as additional claims receipts and payment information becomes available. As more complete claim information becomes available, the Company adjusts the amount of the estimates, and includes
the changes in estimates in medical costs in the period in which the changes are identified. In every reporting period, the operating results include the effects of more completely developed medical claims liability estimates associated with previously reported periods. The Company consistently applies its reserving methodology from period to period. As additional information becomes known, it adjusts the actuarial model accordingly to establish medical claims liability estimates.
The Company periodically reviews actual and anticipated experience compared to the assumptions used to establish medical costs. The Company establishes premium deficiency reserves if actual and anticipated experience indicates that existing policy liabilities together
with the present value of future gross premiums will not be sufficient to cover the present value of future benefits, settlement and maintenance costs.
Revenue Recognition
The Company’s Medicaid Managed Care segment generates revenues primarily from premiums received from the states in which it operates health plans. The Company receives a fixed premium per member per month pursuant to its state contracts. The Company generally receives premium payments during the month it provides
services and recognizes premium revenue during the period in which it is obligated to provide services to its members. In some instances, the Company’s base premiums are subject to an adjustment, or risk score, based on the acuity of its membership. Generally, the risk score is determined by the State analyzing encounter submissions of processed claims data to determine the acuity of the Company’s membership relative to the entire state’s Medicaid membership. Some
states enact premium taxes, similar assessments and provider pass-through payments, collectively premium taxes, and these taxes are recorded as a separate component of both revenues and operating expenses. Some contracts allow for additional premium related to certain supplemental services provided such as maternity deliveries. Revenues are recorded based on membership and eligibility data provided by the states, which may be adjusted by the states for updates to this data. These
eligibility adjustments have been immaterial in relation to total revenue recorded and are reflected in the period known.
The Company’s Specialty Services segment generates revenues under contracts with state programs, individuals, healthcare organizations and other commercial organizations, as well as from the Company’s own subsidiaries. Revenues are recognized when the related services are provided or as ratably earned over the covered
period of service.
Premium and services revenues collected in advance are recorded as unearned revenue. For performance-based contracts the Company does not recognize revenue subject to refund until data is sufficient to measure performance. Premiums and service revenues due to the Company are recorded as premium and related receivables
and are recorded net of an allowance based on historical trends and management’s judgment on the collectibility of these accounts. As the Company generally receives payments during the month in which services are provided, the allowance is typically not significant in comparison to total revenues and does not have a material impact on the presentation of the financial condition or results of operations. Activity in the allowance for uncollectible accounts for the years ended December
31, is summarized below:
|
|
2009 |
2008 |
2007 |
|||||||||
|
Allowances, beginning of year |
|
$ |
1,304 |
$ |
467 |
$ |
155 |
|||||
|
Amounts charged to expense |
285 |
1,142 |
435 |
|||||||||
|
Write-offs of uncollectible receivables |
|
(251 |
) |
(305 |
) |
(123 |
) | |||||
|
Allowances, end of year |
|
$ |
1,338 |
$ |
1,304 |
$ |
467 |
|||||
Significant Customers
Centene receives the majority of its revenues under contracts or subcontracts with state Medicaid managed care programs. The current contracts, which expire on various dates between March 31, 2010 and August 31, 2013, are expected to be renewed. States whose aggregate annual contract value exceeded 10% of annual revenues
and the respective percentage of the Company’s total revenues for the years ended December 31, are as follows:
|
2009 |
2008 |
2007 | ||||||||
|
Georgia |
19% |
Georgia |
23% |
Georgia |
25% | |||||
|
Ohio |
14% |
Ohio |
16% |
Indiana |
12% | |||||
|
Texas |
30% |
Texas |
33% |
Texas |
26% | |||||
|
Wisconsin |
11% | |||||||||
|
Ohio |
17% | |||||||||
Reinsurance
Centene's subsidiaries report reinsurance premiums as medical costs, while related reinsurance recoveries are reported as deductions from medical costs. The Company limits its risk of catastrophic losses by maintaining high deductible reinsurance coverage.
Other Income (Expense)
Other income (expense) consists principally of investment income, interest expense and equity method earnings from investments. Investment income is derived from the Company’s cash, cash equivalents, restricted deposits and investments. Interest expense relates to borrowings under the senior notes, credit facilities,
interest on capital leases and credit facility fees.
Income Taxes
Deferred tax assets and liabilities are recorded for the future tax consequences attributable to differences between the financial statement carrying amounts of existing assets and liabilities and their respective tax bases. Deferred tax assets and liabilities are measured using enacted tax rates expected to apply to taxable income
in the years in which those temporary differences are expected to be recovered or settled. The effect on deferred tax assets and liabilities of a change in tax rates is recognized in income in the period that includes the enactment date of the tax rate change.
Valuation allowances are provided when it is considered more likely than not that deferred tax assets will not be realized. In determining if a deductible temporary difference or net operating loss can be realized, the Company considers future reversals of existing taxable temporary differences, future taxable income, taxable income
in prior carryback periods and tax planning strategies.
Contingencies
The Company accrues for loss contingencies associated with outstanding litigation, claims and assessments for which it has determined it is probable that a loss contingency exists and the amount of loss can be reasonably estimated. The Company expenses professional fees associated with litigation claims and assessments as incurred.
Stock Based Compensation
The fair value of the Company’s employee share options and similar instruments are estimated using the Black-Scholes option-pricing model. That cost is recognized over the period during which an employee is required to provide service in exchange for the award. Excess tax benefits related to stock compensation
are presented as a cash inflow from financing activities.
Additional information regarding the stock option plans is included in Note 16, Stock Incentive Plans.
Reclassifications
Certain amounts in the consolidated financial statements have been reclassified to conform to the 2009 presentation. These reclassifications, primarily related to the reclassification of certain pharmacy liabilities from accounts payable and accrued expenses to medical claims liability, have no effect on net earnings or stockholders’
equity as previously reported.
Recent Accounting Pronouncements
Effective January 1, 2009, the Company adopted new guidance related to business combinations. The changes from the previous guidance include, but are not limited to: (1) acquisition costs are recognized separately from the acquisition; (2) known contractual
contingencies at the time of the acquisition are considered part of the liabilities acquired and and measured at their fair value; all other contingencies are part of the liabilities acquired and measured at their fair value only if it is more likely than not that they meet the definition of a liability; (3) contingent consideration based on the outcome of future events is recognized and measured at the time of the acquisition; and (4) business combinations achieved in stages (step acquisitions) recognize
the identifiable assets and liabilities, as well as noncontrolling interest, in the acquiree, at the full amounts of their fair values. The new guidance has been utilized for all acquisitions since January 1, 2009.
Effective January 1, 2009, the Company adopted new guidance related to consolidation and reporting of noncontrolling interest, which requires all entities to report noncontrolling (minority) interests in subsidiaries in the same way, that is, as equity in the consolidated financial statements. Moreover, this guidance eliminates the diversity
that existed in accounting by requiring transactions between the Company and the noncontrolling interest be treated as equity transactions. As discussed in Note 2, Summary of Significant Accounting Policies, and Note 6, Centene Center LLC, the noncontrolling interest in Access and Centene Center LLC is presented within stockholders’ equity.
In April 2009, new guidance was issued related to the recognition and presentation of other-than-temporary impairments. The guidance applies to fixed maturity securities only and requires separate display of losses related to credit deterioration and losses related to other market factors. When an entity does not intend
to sell the security and it is more likely than not that an entity will not have to sell the security before recovery of its cost basis, it must recognize the credit component of an other-than-temporary impairment in earnings and the remaining portion in other comprehensive income. The adoption of the guidance did not have a material effect on the Company’s financial statements.
In June 2009, new guidance was issued related to the consolidation of variable interest entities to require an analysis to determine whether a variable interest gives the Company a controlling financial interest in a variable interest entity. This guidance requires an ongoing reassessment and eliminates the quantitative approach previously
required for determining whether an entity is the primary beneficiary. This guidance is effective for fiscal years beginning after November 15, 2009 and early adoption is prohibited. The Company is currently evaluating the impact of adopting this guidance on the consolidated financial statements and related disclosures.
The Company has determined that all other recently issued accounting guidance will not have a material impact on its consolidated financial position, results of operations and cash flows, or do not apply to its operations.
3. Discontinued Operations: University Health Plans and FirstGuard Health Plans
University Health Plans
In November 2008, the Company announced its intention to sell certain assets of its New Jersey health plan, University Health Plans, Inc, or UHP. Accordingly, the results of operations of UHP are presented as discontinued operations for all periods presented. The assets, liabilities and results of operations of UHP were
classified as discontinued operations for all periods presented beginning in December 2008. UHP was previously reported in the Medicaid Managed Care segment. The Company expects the sale to be completed during the first quarter of 2010.
In 2008, as a result of the plan to sell certain assets of UHP, the Company conducted an impairment analysis of the assets of UHP. The impairment analysis resulted in an impairment charge for fixed assets of $2,546. During the year ended December 31, 2009 and 2008, the Company incurred exit costs consisting primarily
of lease termination fees and employee severance. The change in exit cost liability for UHP is summarized as follows:
|
2009 |
2008 |
|||||||
|
Balance, January 1, |
$ |
1,110 |
$ |
— |
||||
|
Incurred |
3,140 |
1,110 |
||||||
|
Paid |
(1,257 |
) |
— |
|||||
|
Balance, December 31, |
$ |
2,993 |
$ |
1,110 |
||||
FirstGuard Health Plans
In 2006, FirstGuard Health Plan Kansas, Inc., or FirstGuard Kansas, a wholly owned subsidiary, received notification that its Medicaid contract scheduled to terminate December 31, 2006 would not be renewed. In 2006, the Company also evaluated its strategic alternatives for its Missouri subsidiary, FirstGuard Health Plan, Inc.,
or FirstGuard Missouri, and decided to divest the business. FirstGuard was previously reported in the Medicaid Managed Care segment.
The sale of the operating assets of FirstGuard Missouri was completed effective February 1, 2007, resulting in a gain on the sale of $7,472 in 2007. Goodwill associated with FirstGuard written off as part of the transaction was $5,995. In 2007, the Company abandoned the stock of FirstGuard Kansas and FirstGuard Missouri
to an unrelated entity. As a result of that abandonment, the Company recognized expense of $2,298 for the write-off of the remaining assets in that entity. The Company also recognized a $34,856 tax benefit for the tax deduction associated with the basis of that stock.
The Company has incurred FirstGuard exit costs consisting primarily of lease termination fees and employee severance costs. The Company also contributed $3,000 of the sale proceeds received in the second quarter of 2007 to its charitable foundation and recorded the contribution as General and Administrative expense. The change
in exit cost liability for FirstGuard is summarized as follows:
|
2008 |
2007 |
|||||||
|
Balance, January 1, |
$ |
125 |
$ |
3,027 |
||||
|
Incurred |
76 |
2,531 |
||||||
|
Paid |
(201 |
) |
(5,433 |
) | ||||
|
Balance, December 31, |
$ |
— |
$ |
125 |
||||
Financial Summary
Operating results for the discontinued operations are as follows:
|
Year Ended December 31, |
||||||||||||
|
|
2009 |
2008 |
2007 |
|||||||||
|
Revenues |
|
$ |
145,097 |
$ |
150,638 |
$ |
156,952 |
|||||
|
Earnings (loss) before income taxes |
|
$ |
(3,626 |
) |
|
$ |
(965 |
) |
|
$ |
799 |
|
|
Net earnings (loss) |
|
$ |
(2,422 |
) |
|
$ |
(684 |
) |
|
$ |
32,362 |
|
Assets and liabilities of the discontinued operations are as follows:
|
December 31, |
||||||||
|
2009 |
2008 |
|||||||
|
Current assets |
$ | 7,307 | $ | 18,087 | ||||
|
Long term investments and restricted deposits |
22,139 | 22,008 | ||||||
|
Goodwill |
2,168 | 2,168 | ||||||
|
Other intangible assets, net |
1,552 | 1,552 | ||||||
|
Other assets |
426 | 1,520 | ||||||
|
Assets of discontinued operations |
$ | 33,592 | $ | 45,335 | ||||
|
December 31, |
||||||||
|
2009 |
2008 |
|||||||
|
Medical claims liability |
$ | 17,718 | $ | 25,290 | ||||
|
Accounts payable and accrued expenses |
2,967 | 5,723 | ||||||
|
Other liabilities |
383 | 726 | ||||||
|
Liabilities of discontinued operations |
$ | 21,068 | $ | 31,739 | ||||
4. Restructuring
In the fourth quarter of 2007, the Company abandoned its previously planned redevelopment project in Clayton, Missouri, related to a corporate office expansion. As a result, the Company conducted an impairment analysis of the related real estate and capitalized construction costs and recorded an impairment charge of $7,207. The
impairment charges were recorded as General and Administrative expense under the Medicaid Managed Care segment. Also in the fourth quarter of 2007, the Company completed an organizational realignment, resulting in the elimination of approximately 35 positions. Accordingly, the Company recorded $2,185 in severance costs. This expense was recorded as General and Administrative expense under the Medicaid Managed Care segment. At December 31, 2009, the Company did not have
any remaining liability for these costs.
The Company did not recognize any restructuring charges during the years ended December 31, 2009 or December 31, 2008.
5. Acquisitions
2009 Acquisitions
|
· |
Access. In July 2007, the Company acquired a 49% ownership interest in Access, a Medicaid managed care entity in Florida. The Company accounted for its investment in Access using the equity method of accounting through December 31, 2008. During the quarter ended
March 31, 2009, the Company began presenting its investment in Access as a consolidated subsidiary in its financial statements. The consolidation of Access resulted in goodwill of approximately $43,400, and other identified intangible assets of approximately $5,400. In 2009, the Company paid an additional $33,927 conversion fee for the transfer of membership from Access to the Company’s wholly-owned subsidiary, Sunshine State Health Plan, Inc. |
|
· |
Additional 2009 Acquisitions. The Company acquired assets of the following entities: Pediatric Associates LLC, effective February 2009, Amerigroup Community Care of South Carolina, Inc., effective March 2009 and InSpeech, Inc., effective July 2009. The
Company paid a total of approximately $12,500 in cash for these acquisitions. Goodwill of approximately $9,500 and other identifiable intangible assets of approximately $1,500 were included in the Medicaid Managed Care segment and other identifiable intangible assets of $1,700 were included in the Specialty Services segment, all of which is deductible for income tax purposes. |
2008 Acquisitions
|
Ÿ |
Celtic Insurance Company. On July 1, 2008, the Company acquired Celtic Insurance Company, or Celtic, a health insurance carrier focused on the individual health insurance market. The Company paid approximately $82,100 in
cash and related transaction costs, net of unregulated cash acquired. In conjunction with the closing of the acquisition, Celtic paid to the Company an extraordinary dividend of $31,411 in July 2008. The results of operations for Celtic are included in the Specialty Services segment of the consolidated financial statements since July 1, 2008. |
The Company allocated total consideration paid to the assets acquired and liabilities assumed based on its estimates of fair value using methodologies and assumptions that it believed were reasonable. The purchase price allocation resulted in estimated identifiable intangible assets, associated deferred tax liabilities and goodwill
of $8,600, $3,000 and $24,300, respectively. The identifiable intangible assets have estimated useful lives ranging from seven to 15 years. The acquired goodwill is not deductible for income tax purposes.
2007 Acquisitions
|
Ÿ |
2007 Acquisitions. The Company acquired 100% of the following entities: PhyTrust of South Carolina, LLC, effective April 20, 2007; Physician’s Choice, LLC, effective October 2007; and Work Life Innovations, effective November 30, 2007. The Company paid a total of $11,300
in cash and related transaction costs for these acquisitions. PhyTrust of South Carolina and Physician’s Choice, LLC, both with Medicaid members in South Carolina, are included in the Medicaid Managed Care segment. Work Life Innovations, a health and wellness consulting company, is included in the Specialty Services segment. For these acquisitions, goodwill of $8,343 and $2,739 was allocated to the Medicaid Managed Care segment and the Specialty Services segment, respectively,
all of which is deductible for income tax purposes. |
Pro forma disclosures related to these acquisitions have been excluded as immaterial.
6. Centene Center LLC
In June 2009, the Company executed an agreement as a 50% joint venture partner in a real estate development entity, Centene Center LLC, associated with the construction of a real estate development to include the Company’s corporate headquarters. Centene Center LLC is a variable interest entity, or VIE, and the Company concluded
it was the primary beneficiary. Accordingly, the Company’s consolidated financial statements include the accounts of Centene Center LLC. The Company’s interest in Centene Center LLC includes an initial equity investment of $17,400. Centene Center LLC has posted a $1,750 letter of credit to a tenant of the development, collateralized by a portion of the entity’s cash balances. The assets and liabilities of Centene Center LLC as of December 31, 2009
are as follows (on a 100% basis):
|
Total Assets |
$ | 97,134 | ||
|
Total Liabilities |
$ | 62,326 | ||
|
Equity |
||||
|
Centene Corporation (50% ownership) |
$ | 17,404 | ||
|
Joint venture partners (50% ownership) |
17,404 | |||
|
Total equity |
$ | 34,808 | ||
|
Total Liabilities and Equity |
$ | 97,134 |
As part of financing the real estate development, the joint venture executed a $95,000 construction loan due June 1, 2011, which may be extended for two additional one year terms. The Company and its development partner have guaranteed up to $65,000 each associated with this construction loan. As of December 31, 2009,
there was $32,559 outstanding under this loan and the Company has capitalized $116 of interest in 2009. Additional information regarding the construction loan is included in Note 13, Debt.
7. Short-term and Long-term Investments and Restricted Deposits
Short-term and long-term investments and restricted deposits by investment type consist of the following:
|
December 31, 2009 |
December 31, 2008 |
|||||||||||||||||||||||||||||||
|
Amortized
Cost |
Gross
Unrealized
Gains |
Gross
Unrealized
Losses |
Fair
Value |
Amortized
Cost |
Gross
Unrealized
Gains |
Gross
Unrealized
Losses |
Fair
Value |
|||||||||||||||||||||||||
|
U.S. Treasury securities |
$ | 27,080 | $ | 213 | $ | (5 | ) | $ | 27,288 | $ | 4,054 | $ | 130 | $ | — | $ | 4,184 | |||||||||||||||
|
Corporate securities |
165,720 | 581 | (940 | ) | 165,361 | 47,733 | 74 | (1,154 | ) | 46,653 | ||||||||||||||||||||||
|
State and municipal securities |
333,955 | 11,628 | (31 | ) | 345,552 | 360,638 | 5,964 | (11 | ) | 366,591 | ||||||||||||||||||||||
|
Equity securities |
9,751 | 312 | (170 | ) | 9,893 | 7,183 | 17 | (885 | ) | 6,315 | ||||||||||||||||||||||
|
Reserve Primary fund |
2,444 | — | — | 2,444 | 12,988 | — | — | 12,988 | ||||||||||||||||||||||||
|
Life insurance contracts |
14,650 | — | — | 14,650 | 14,327 | — | — | 14,327 | ||||||||||||||||||||||||
|
Asset backed securities |
19,934 | 61 | — | 19,995 | — | — | — | — | ||||||||||||||||||||||||
|
Total |
$ | 573,534 | $ | 12,795 | $ | (1,146 | ) | $ | 585,183 | $ | 446,923 | $ | 6,185 | $ | (2,050 | ) | $ | 451,058 | ||||||||||||||
The Company’s investments are classified as available for sale with the exception of life insurance contracts and certain cost method investments. The Company monitors investments for other than temporary impairment. Certain investments have experienced a decline in fair value due to changes in credit quality,
market interest rates and/or general economic conditions. Based on management’s intent and ability to not sell these investments prior to their anticipated recovery, no other than temporary impairment has been recorded. Investments in a gross unrealized loss position are as follows:
|
December 31, 2009 |
December 31, 2008 |
|||||||||||||||||||||||||||||||
|
Less Than 12 Months |
12 Months or More |
Less Than 12 Months |
12 Months or More |
|||||||||||||||||||||||||||||
|
Unrealized Losses |
Fair
Value |
Unrealized
Losses |
Fair
Value |
Unrealized Losses |
Fair
Value |
Unrealized
Losses |
Fair
Value |
|||||||||||||||||||||||||
|
U.S. Treasury securities |
$ | (5 | ) | $ | 785 | $ | — | $ | — | $ | — | $ | 314 | $ | — | $ | — | |||||||||||||||
|
Corporate securities |
(901 | ) | 99,418 | (39 | ) | 892 | (1,071 | ) | 20,898 | (83 | ) | 2,072 | ||||||||||||||||||||
|
State and municipal securities |
(31 | ) | 9,683 | — | — | (9 | ) | 3,798 | (2 | ) | 101 | |||||||||||||||||||||
|
Equity securities |
(84 | ) | 527 | (86 | ) | 629 | (885 | ) | 2,658 | — | — | |||||||||||||||||||||
|
Asset backed securities |
— | — | — | — | — | — | — | — | ||||||||||||||||||||||||
|
Total |
$ | (1,021 | ) | $ | 110,413 | $ | (125 | ) | $ | 1,521 | $ | (1,965 | ) | $ | 27,668 | $ | (85 | ) | $ | 2,173 | ||||||||||||
The contractual maturities of short-term and long-term investments and restricted deposits as of December 31, 2009, are as follows:
|
Investments |
Restricted Deposits |
|||||||||||||||
|
Amortized
Cost |
Fair
Value |
Amortized
Cost |
Fair
Value |
|||||||||||||
|
One year or less |
$ | 39,230 | $ | 39,554 | $ | 17,737 | $ | 17,758 | ||||||||
|
One year through five years |
456,041 | 467,112 | 2,311 | 2,374 | ||||||||||||
|
Five years through ten years |
28,597 | 28,780 | — | — | ||||||||||||
|
Greater than ten years |
29,618 | 29,605 | — | — | ||||||||||||
|
Total |
$ | 553,486 | $ | 565,051 | $ | 20,048 | $ | 20,132 | ||||||||
The contractual maturities of short-term and long-term investments and restricted deposits as of December 31, 2008, are as follows:
|
Investments |
Restricted Deposits |
|||||||||||||||
|
Amortized
Cost |
Fair
Value |
Amortized
Cost |
Fair
Value |
|||||||||||||
|
One year or less |
$ | 108,469 | $ | 109,393 | $ | 6,038 | $ | 6,044 | ||||||||
|
One year through five years |
181,958 | 185,867 | 3,086 | 3,210 | ||||||||||||
|
Five years through ten years |
56,936 | 56,188 | — | — | ||||||||||||
|
Greater than ten years |
90,436 | 90,356 | — | — | ||||||||||||
|
Total |
$ | 437,799 | $ | 441,804 | $ | 9,124 | $ | 9,254 | ||||||||
Actual maturities may differ from contractual maturities due to call or prepayment options. Asset backed securities are included in the one year through five years category, while equity securities and life insurance contracts are included in the five years through ten years category. The Company has an option
to redeem at amortized cost substantially all of the securities included in the Greater than ten years category listed above.
The Company’s gross recorded realized gains and losses on investments for the years ended December 31, were as follows:
|
|
2009 |
2008 |
2007 |
|||||||||
|
Gross realized gains |
|
$ |
1,252 |
$ |
1,364 |
$ |
325 |
|||||
|
Gross realized losses |
|
(1,111 |
) |
(5,654 |
) |
(372 |
) | |||||
|
Net realized gains (losses) |
|
$ |
141 |
$ |
(4,290 |
) |
$ |
(47 |
) | |||
Investment and other income in the third quarter of 2008 included a loss on investments of $4,457. The loss was primarily due to investments in the Reserve Primary money market fund (Reserve Fund) whose Net Asset Value fell below $1.00 per share. Money market funds are generally recorded in Cash and cash equivalents
in the Company's balance sheet, however, the investment in the Reserve Fund is recorded in Short-term investments due to the restrictions placed on redemptions imposed by the fund. As of December 31, 2009, the Company's short term investment balance includes $2,444 for the Reserve Fund.
Additional information regarding investments is included in Note 8, Fair Value Measurements.
8. Fair Value Measurements
Assets and liabilities recorded at fair value in the consolidated balance sheets are categorized based upon the extent to which the fair value estimates are based upon observable or unobservable inputs. Level inputs are as follows:
|
Level Input: |
|
Input Definition: |
|
Level I |
|
Inputs are unadjusted, quoted prices for identical assets or liabilities in active markets at the measurement date. |
|
Level II |
|
Inputs other than quoted prices included in Level I that are observable for the asset or liability through corroboration with market data at the measurement date. |
|
Level III |
|
Unobservable inputs that reflect management’s best estimate of what market participants would use in pricing the asset or liability at the measurement date. |
The following table summarizes fair value measurements by level at December 31, 2009 for assets and liabilities measured at fair value on a recurring basis:
|
Level I |
Level II |
Level III |
Total |
|||||||||||||
|
Cash and cash equivalents |
$ | 400,951 | ― | ― | $ | 400,951 | ||||||||||
|
Investments available for sale: |
||||||||||||||||
|
U.S. Treasury securities and obligations of U.S. government corporations and agencies |
$ | 16,635 | $ | 2,764 | $ | ― | $ | 19,399 | ||||||||
|
Corporate securities |
― | 152,919 | ― | 152,919 | ||||||||||||
|
State and municipal securities |
― | 345,552 | ― | 345,552 | ||||||||||||
|
Equity securities |
3,585 | ― | ― | 3,585 | ||||||||||||
|
Asset backed securities |
― | 19,995 | ― | 19,995 | ||||||||||||
|
Total investments |
$ | 20,220 | $ | 521,230 | $ | ― | $ | 541,450 | ||||||||
|
Restricted deposits available for sale: |
||||||||||||||||
|
Cash and cash equivalents |
$ | 7,285 | $ | ― | $ | ― | $ | 7,285 | ||||||||
|
Certificates of deposit |
4,958 | ― | ― | 4,958 | ||||||||||||
|
U.S. Treasury securities and obligations of U.S. government corporations and agencies |
7,889 | ― | ― | 7,889 | ||||||||||||
|
Total restricted deposits |
$ | 20,132 | $ | ― | $ | ― | $ | 20,132 | ||||||||
|
Total assets at fair value |
$ | 441,303 | $ | 521,230 | $ | ― | $ | 962,533 | ||||||||
|
Total debt |
$ | ― | $ | 305,544 | $ | ― | $ | 305,544 | ||||||||
The following table summarizes fair value measurements by level at December 31, 2008 for assets and liabilities measured at fair value on a recurring basis:
|
Level I |
Level II |
Level III |
Total |
|||||||||||||
|
Cash and cash equivalents |
$ | 370,999 | ― | ― | $ | 370,999 | ||||||||||
|
Investments available for sale: |
||||||||||||||||
|
Corporate securities |
$ | ― | $ | 41,382 | $ | ― | $ | 41,382 | ||||||||
|
State and municipal securities |
― | 366,591 | ― | 366,591 | ||||||||||||
|
Equity securities |
3,328 | ― | ― | 3,328 | ||||||||||||
|
Total investments |
$ | 3,328 | $ | 407,973 | $ | ― | $ | 411,301 | ||||||||
|
Restricted deposits available for sale: |
||||||||||||||||
|
Cash and cash equivalents |
$ | 3,401 | $ | ― | $ | ― | $ | 3,401 | ||||||||
|
Certificates of deposit |
1,669 | ― | ― | 1,669 | ||||||||||||
|
U.S. Treasury securities and obligations of U.S. government corporations and agencies |
4,184 | ― | ― | 4,184 | ||||||||||||
|
Total restricted deposits |
$ | 9,254 | $ | ― | $ | ― | $ | 9,254 | ||||||||
|
Total assets at fair value |
$ | 383,581 | $ | 407,973 | $ | ― | $ | 791,554 | ||||||||
|
Total debt |
$ | ― | $ | 226,829 | $ | ― | $ | 226,829 | ||||||||
The aggregate carrying amount of the Company’s life insurance contracts and cost-method investments, which approximates fair value, was $23,601 and $30,503 as of December 31, 2009 and December 31, 2008, respectively. During 2008, the fair value estimates of corporate securities and state and municipal securities were categorized
as Level I. The prior period disclosure has been reclassified to reflect these securities as Level II measurements.
9. Property, Software and Equipment
Property, software and equipment consist of the following as of December 31:
|
|
2009 |
2008 |
||||||
|
Computer software |
|
$ |
113,416 |
$ |
97,829 |
|||
|
Building |
|
104,786 |
|
38,503 |
||||
|
Land |
|
40,639 |
40,525 |
|||||
|
Computer hardware |
31,651 |
31,897 |
||||||
|
Furniture and office equipment |
|
24,012 |
22,756 |
|||||
|
Leasehold improvements |
|
19,800 |
18,542 |
|||||
|
|
334,304 |
250,052 |
||||||
|
Less accumulated depreciation |
|
(103,883 |
) |
(74,194 |
) | |||
|
Property, software and equipment, net |
|
$ |
230,421 |
$ |
175,858 |
|||
As of December 31, 2009 and 2008, the Company had assets acquired under capital leases with a net book value of $6,411 and $6,605, respectively. Depreciation expense for the years ended December 31, 2009, 2008 and 2007 was $33,103, $28,453 and $22,647, respectively.
10. Goodwill and Intangible Assets
The following table summarizes the changes in goodwill by operating segment:
|
Medicaid Managed Care |
Specialty Services |
Total |
||||||||||
|
Balance as of December 31, 2007 |
$ | 51,468 | $ | 87,394 | $ | 138,862 | ||||||
|
Acquisitions |
80 | 24,438 | 24,518 | |||||||||
|
Balance as of December 31, 2008 |
51,548 | 111,832 | 163,380 | |||||||||
|
Acquisitions |
59,515 | 1,692 | 61,207 | |||||||||
|
Balance as of December 31, 2009 |
$ | 111,063 | $ | 113,524 | $ | 224,587 | ||||||
Goodwill additions in 2009 and 2008 were related to the acquisitions discussed in Note 5, Acquisitions.
Intangible assets at December 31, consist of the following:
|
|
Weighted Average Life in Years | ||||||||||
|
|
2009 |
2008 |
2009 |
2008 | |||||||
|
Purchased contract rights |
|
$ |
12,997 |
$ |
6,116 |
7.7 |
6.9 | ||||
|
Provider contracts |
|
1,078 |
1,078 |
9.9 |
9.9 | ||||||
|
Customer relationships |
15,845 |
14,130 |
7.3 |
7.6 | |||||||
|
Trade names |
|
5,545 |
5,545 |
19.0 |
19.0 | ||||||
|
Intangible assets |
|
35,465 |
26,869 |
9.4 |
9.9 | ||||||
|
Less accumulated amortization: |
|
||||||||||
|
Purchased contract rights |
|
(5,752 |
) |
(4,642 |
) |
||||||
|
Provider contracts |
|
(515 |
) |
(405 |
) |
||||||
|
Customer relationships |
(5,741 |
) |
(3,566 |
) |
|||||||
|
Trade names |
|
(978 |
) |
(681 |
) |
||||||
|
Total accumulated amortization |
|
(12,986 |
) |
(9,294 |
) |
||||||
|
Intangible assets, net |
|
$ |
22,479 |
$ |
17,575 |
||||||
|
|
|||||||||||
Amortization expense was $3,692, $2,480 and $1,970 for the years ended December 31, 2009, 2008 and 2007, respectively.
Estimated total amortization expense related to intangible assets for each of the five succeeding fiscal years is as follows:
|
Year |
Expense |
|||
|
2010 |
$ | 3,700 | ||
|
2011 |
3,500 | |||
|
2012 |
3,400 | |||
|
2013 |
2,900 | |||
|
2014 |
2,500 | |||
11. Income Taxes
The consolidated income tax expense consists of the following for the years ended December 31:
|
|
2009 |
2008 |
2007 | |||||||
|
Current provision: |
|
|||||||||
|
Federal |
|
$ |
41,310 |
$ |
53,543 |
$ |
31,170 | |||
|
State and local |
|
5,578 |
6,726 |
2,741 | ||||||
|
Total current provision |
|
46,888 |
60,269 |
33,911 | ||||||
|
Deferred provision |
|
1,953 |
(7,834 |
) |
(10,880) | |||||
|
Total provision for income taxes |
$ |
48,841 |
$ |
52,435 |
$ |
23,031 | ||||
The reconciliation of the tax provision at the U.S. Federal Statutory Rate to the provision for income taxes is as follows:
|
|
2009 |
2008 |
2007 | |||||||
|
Tax provision at the U.S. federal statutory rate |
|
$ |
48,128 |
$ |
47,816 |
$ |
22,425 | |||
|
State income taxes, net of federal income tax benefit |
|
2,419 |
4,938 |
821 | ||||||
|
Partnership income attributable to noncontrolling interest |
(901 |
) |
— |
— | ||||||
|
Tax exempt investment income |
(3,132 |
) |
(3,727 |
) |
(2,636) | |||||
|
Nondeductible incentive stock option compensation |
1,093 |
1,316 |
1,542 | |||||||
|
Other, net |
|
1,234 |
2,092 |
879 | ||||||
|
Income tax expense |
|
$ |
48,841 |
$ |
52,435 |
$ |
23,031 | |||
The tax effects of temporary differences which give rise to deferred tax assets and liabilities are presented below for the years ended December 31:
|
2009 |
2008 |
|||||||
|
Deferred tax assets: |
||||||||
|
Current: |
||||||||
|
Medical claims liability and other accruals |
$ | 29,487 | $ | 34,222 | ||||
|
Unearned premium and other deferred revenue |
6,734 | 959 | ||||||
|
State net operating loss carry forward |
578 | 1,033 | ||||||
|
Capital loss carryovers and impairment losses |
1,738 | 2,111 | ||||||
|
Other |
317 | 221 | ||||||
|
Net current deferred tax assets |
$ | 38,854 | $ | 38,546 | ||||
|
Non-current deferred tax assets: |
||||||||
|
Medical claims liability and other accruals |
$ | 493 | $ | 3,092 | ||||
|
Federal net operating loss carry forward |
2,048 | 2,444 | ||||||
|
State net operating loss carry forward |
4,408 | 3,029 | ||||||
|
Investment in partnerships |
6,071 | — | ||||||
|
Stock compensation |
13,915 | 11,796 | ||||||
|
State tax credits |
786 | — | ||||||
|
Other |
2,226 | 1,155 | ||||||
| 29,947 | 21,516 | |||||||
|
Valuation allowance |
(2,140 | ) | (1,541 | ) | ||||
|
Net non-current deferred tax assets |
$ | 27,807 | $ | 19,975 | ||||
|
Deferred tax liabilities: |
||||||||
|
Current: |
||||||||
|
Prepaid assets |
$ | 3,575 | $ | 2,026 | ||||
|
Unrealized short term gains |
117 | 524 | ||||||
|
Other |
13 | — | ||||||
|
Net current deferred tax liabilities |
$ | 3,705 | $ | 2,550 | ||||
|
Non-current deferred tax liabilities: |
||||||||
|
Intangible assets |
$ | 9,837 | $ | 7,969 | ||||
|
Depreciation and amortization |
38,302 | 26,557 | ||||||
|
Unrealized gain on investments |
4,114 | 1,364 | ||||||
|
Prepaid assets |
— | 1,154 | ||||||
|
Other |
85 | 25 | ||||||
|
Net non-current deferred tax liabilities |
$ | 52,338 | $ | 37,069 | ||||
|
Net deferred tax assets |
$ | 10,618 | $ | 18,902 | ||||
The Company's deferred tax assets include federal and state net operating losses, or NOLs, of which $2,543 were acquired in business combinations. Accordingly, the total and annual deduction for those NOLs is limited by tax law. The Company 's federal NOLs expire between the years 2011 and 2027 and the state NOLs expire
between the years 2010 and 2027. Valuation allowances are recorded for those NOLs the Company believes are more likely than not to expire unused. During 2009 and 2008, the Company recorded valuation allowance additions in the tax provision of $1,381 and $1,829, respectively. In 2009 and 2008 the Company recorded valuation allowance reductions of $80 and $126.
The Company maintains a reserve for uncertain tax positions that may be challenged by a tax authority. A roll-forward of the reserve is as follows:
|
Balance as of December 31, 2008 |
|
$ |
4,054 |
|
|
Reductions based on tax positions during the current year |
|
(11 |
) | |
|
Settlements |
(52 |
) | ||
|
Balance as of December 31, 2009 |
|
$ |
3,991 |
The December 31, 2009 balance includes $933 (net of federal tax benefit) that would decrease income tax expense, if recognized, and the remainder would reduce deferred tax assets.
The Company recognizes interest accrued related to unrecognized tax benefits in the provision for income taxes. Interest accrued, net of federal benefit, was $1,072 and $560 as of December 31, 2009 and December 31, 2008, respectively. No penalties have been accrued.
The federal income tax returns for 2006 through 2009 are open tax years. In May 2008, the Internal Revenue Service began an audit of the Company's 2006 and 2007 tax returns. As a result of this audit, the IRS has initially denied the $34,856 tax benefit the Company recognized for the abandonment of the FirstGuard stock
in 2007. The Company is proceeding with the appeals process and believes that it is more likely than not that the Company's tax position will be upheld. Accordingly, the Company has not made any adjustments to the reserve for this position.
The Company files in numerous state jurisdictions with varying statutes of limitation. The unrecognized state tax benefits are related to returns open from 2004 to 2009.
12. Medical Claims Liability
The change in medical claims liability is summarized as follows:
|
Year Ended December 31, |
|||||||||||
|
2009 |
2008 |
2007 |
|||||||||
|
Balance, January 1, |
$ |
384,360 |
$ |
323,741 |
$ |
241,073 |
|||||
|
Acquisitions |
— |
15,398 |
— |
||||||||
|
Incurred related to: |
|||||||||||
|
Current year |
3,216,533 |
2,659,036 |
2,212,901 |
||||||||
|
Prior years |
(53,010 |
) |
(18,701 |
) |
(22,003 |
) | |||||
|
Total incurred |
3,163,523 |
2,640,335 |
2,190,898 |
||||||||
|
Paid related to: |
|||||||||||
|
Current year |
2,752,983 |
2,292,150 |
1,892,233 |
||||||||
|
Prior years |
323,968 |
302,964 |
215,997 |
||||||||
|
Total paid |
3,076,951 |
2,595,114 |
2,108,230 |
||||||||
|
Balance, December 31, |
$ |
470,932 |
$ |
384,360 |
$ |
323,741 |
|||||
Changes in estimates of incurred claims for prior years are primarily attributable to reserving under moderately adverse conditions. In addition, claims processing initiatives yielded increased claim payment recoveries and coordination of benefits related to prior year dates of service. Changes in medical utilization
and cost trends and the effect of medical management initiatives may also contribute to changes in medical claim liability estimates. While the Company has evidence that medical management initiatives are effective on a case by case basis, medical management initiatives primarily focus on events and behaviors prior to the incurrence of the medical event and generation of a claim. Accordingly, any change in behavior, leveling of care, or coordination of treatment occurs prior to claim generation
and as a result, the costs prior to the medical management initiative are not known by the Company. Additionally, certain medical management initiatives are focused on member and provider education with the intent of influencing behavior to appropriately align the medical services provided with the member’s acuity. In these cases, determining whether the medical management initiative changed the behavior cannot be determined. Because of the complexity of its business, the
number of states in which it operates, and the volume of claims that it processes, the Company is unable to practically quantify the impact of these initiatives on its changes in estimates of IBNR.
As discussed in Note 2, Summary of Significant Accounting Policies, certain amounts in the consolidated financial statements have been reclassified to conform to the 2009 presentation. These reclassifications include the reclassification of certain pharmacy liabilities from
accounts payable and accrued expenses to medical claims liability. This reclassification totaled $18,303, $11,323, and $10,377 as of the year ended December 31, 2009, 2008 and 2007, respectively.
The Company had reinsurance recoverables related to medical claims liability of $4,700 and $4,972 at December 31, 2009 and 2008, respectively, included in premium and related receivables.
13. Debt
Debt consists of the following at December 31:
|
2009 |
2008 |
|||||||
|
$175,000 senior notes |
$ | 175,000 | $ | 175,000 | ||||
|
$300,000 revolving credit agreement |
84,000 | 63,000 | ||||||
|
Mortgage note payable |
9,900 | ― | ||||||
|
$20,500 revolving loan agreement |
― | 20,364 | ||||||
|
Capital leases |
6,272 | 6,528 | ||||||
|
Joint venture construction loan |
32,559 | ― | ||||||
|
Total debt |
307,731 | 264,892 | ||||||
|
Less current maturities |
(646 | ) | (255 | ) | ||||
|
Long-term debt |
$ | 307,085 | $ | 264,637 | ||||
$20,500 Revolving Loan Agreement and Mortgage Note Payable
During the third quarter of 2009, the Company paid the balance of the revolving loan agreement and refinanced a portion of the balance with another bank as a mortgage note payable. The mortgage note is collateralized by the Company’s existing headquarters building and parking garage. The collateralized properties
had a net book value of $17,958 at December 31, 2009. The mortgage is due August 31, 2014 and bears interest at the LIBOR rate plus 3% or the bank’s certificate of deposit rate plus 2%. The mortgage includes financial covenants requiring a minimum fixed charge coverage ratio. The weighted average interest rate of outstanding borrowings was 3.12% at December 31, 2009.
Joint Venture Construction Loan
In June 2009, the Company and its development partner executed a $95,000 construction loan associated with the construction of a real estate development to include the Company’s corporate headquarters. The construction loan is due June 1, 2011 which may be extended for two additional one year terms. The loan bears
interest at the LIBOR rate plus 4% with a minimum rate of 5%. The Company and its development partner have each guaranteed up to $65,000 associated with the construction loan. The agreement contains non-financial and financial covenants, including requirements for the Company to maintain a specified net worth. As of December 31, 2009, there was $32,559 outstanding under the construction loan, bearing interest at 5.0%.
$175,000 Senior Notes
In March 2007, the Company issued $175,000 aggregate principal amount of 7 ¼% Senior Notes due April 1, 2014, or the Notes. The Notes have been registered under the Securities Act of 1933, as amended, pursuant to a registration rights agreement with the initial purchasers. The indenture governing the Notes contains
non-financial and financial covenants, including requirements of a minimum fixed charge coverage ratio. Interest is paid semi-annually in April and October.
$300,000 Revolving Credit Agreement
The Company has a $300,000 five-year Revolving Credit Agreement dated September 14, 2004 with various financial institutions. Borrowings under the agreement bear interest based upon LIBOR rates, the Federal Funds Rate or the Prime Rate. There is a commitment fee on the unused portion of the agreement that ranges from
0.15% to 0.275% depending on the total debt-to-EBITDA ratio. The agreement contains non-financial and financial covenants, including requirements of minimum fixed charge coverage ratios, maximum debt-to-EBITDA ratios and minimum tangible net worth. The agreement will expire in September 2011. As of December 31, 2009, the Company had $84,000 in borrowings outstanding under the agreement and $40,495 in letters of credit outstanding, leaving availability of $175,505. The
outstanding borrowings at December 31, 2009 bore interest at LIBOR plus 1.0%, or the prime rate. The weighted average interest rate of outstanding borrowings was 1.69% at December 31, 2009.
Aggregate maturities for the Company’s debt are as follows:
|
2010 |
$ | 646 | ||
|
2011 |
117,209 | |||
|
2012 |
661 | |||
|
2013 |
673 | |||
|
2014 |
183,585 | |||
|
Thereafter |
4,957 | |||
|
Total |
$ | 307,731 |
The fair value of outstanding debt was approximately $305,544 and $226,829 at December 31, 2009 and 2008, respectively.
14. Stockholders’ Equity
The Company has 10,000,000 authorized shares of preferred stock at $.001 par value. At December 31, 2009, there were no preferred shares outstanding.
On October 26, 2009, the Company’s Board of Directors extended the Company’s stock repurchase program. The program authorizes the repurchase of up to 4,000,000 shares of the Company’s common stock from time to time on the open market or through privately negotiated transactions. No duration has been
placed on the repurchase program and the Company reserves the right to discontinue the repurchase program at any time. During the year ended December 31, 2009, the Company repurchased 332,595 shares at an aggregate cost of $6,304. During the year ended December 31, 2008, the Company repurchased 1,218,858 shares at an aggregate cost of $23,510.
15. Statutory Capital Requirements and Dividend Restrictions
Various state laws require Centene’s regulated subsidiaries to maintain minimum capital levels specified by each state and restrict the amount of dividends that may be paid without prior regulatory approval. At December 31, 2009 and 2008, Centene’s subsidiaries, including UHP, had aggregate statutory capital and surplus
of $453,200 and $391,400, respectively, compared with the required minimum aggregate statutory capital and surplus of $286,500 and $241,500, respectively.
16. Stock Incentive Plans
The Company’s stock incentive plans allow for the granting of restricted stock or restricted stock unit awards and options to purchase common stock. Both incentive stock options and nonqualified stock options can be awarded under the plans. No option will be exercisable for longer than ten years after the date
of grant. The plans have 672,164 shares available for future awards. Compensation expense for stock options and restricted stock unit awards is recognized on a straight-line basis over the vesting period, generally three to five years for stock options and one to ten years for restricted stock or restricted stock unit awards. Certain restricted stock unit awards contain performance-based as well as service-based provisions. Certain awards provide for accelerated vesting
if there is a change in control as defined in the plans. The total compensation cost that has been charged against income for the stock incentive plans was $14,634, $15,328 and $15,781 for the years ended December 31, 2009, 2008 and 2007, respectively. The total income tax benefit recognized in the income statement for stock-based compensation arrangements was $3,945, $4,771 and $4,536 for the years ended December 31, 2009, 2008 and 2007, respectively.
Option activity for the year ended December 31, 2009 is summarized below:
|
Shares |
Weighted Average
Exercise Price |
Aggregate Intrinsic Value |
Weighted Average Remaining
Contractual Term |
||||||||||||
|
Outstanding as of December 31, 2008 |
3,718,372 |
$ |
19.81 |
||||||||||||
|
Granted |
68,000 |
17.75 |
|||||||||||||
|
Exercised |
(193,017) |
8.21 |
|||||||||||||
|
Forfeited |
(132,600) |
22.56 |
|||||||||||||
|
Outstanding as of December 31, 2009 |
3,460,755 |
$ |
20.31 |
$ |
10,376 |
5.6 |
|||||||||
|
Exercisable as of December 31, 2009 |
2,763,489 |
$ |
19.83 |
$ |
9,556 |
5.1 |
|||||||||
The fair value of each option grant is estimated on the date of the grant using the Black-Scholes option-pricing model with the following weighted-average assumptions:
|
Year Ended December 31, | |||||
|
2009 |
2008 |
2007 | |||
|
Expected life (in years) |
5.8 |
5.8 |
6.1 | ||
|
Risk-free interest rate |
2.2% |
3.0% |
4.1% | ||
|
Expected volatility |
50.9% |
50.3% |
47.5% | ||
|
Expected dividend yield |
0% |
0% |
0% | ||
For the years ended December 31, 2009, 2008 and 2007, the Company used a projected expected life for each award granted based on historical experience of employees’ exercise behavior. The expected volatility is primarily based on historical volatility levels along with the implied volatility of exchange traded options to
purchase Centene common stock. The risk-free interest rates are based on the implied yield currently available on U.S. Treasury instruments with a remaining term equal to the expected life.
Other information pertaining to option activity during the years ended December 31, 2009, 2008 and 2007 is as follows:
|
Year Ended December 31, | |||||
|
2009 |
2008 |
2007 | |||
|
Weighted-average fair value of options granted |
$ 8.76 |
$ 9.27 |
$ 12.02 | ||
|
Total intrinsic value of stock options exercised |
$ 2,192 |
$ 3,529 |
$ 9,847 | ||
A summary of the status of the Company's non-vested restricted stock and restricted stock unit shares as of December 31, 2009, and changes during the year ended December 31, 2009, is presented below:
|
Shares |
Weighted Average Grant Date Fair
Value |
|||||||
|
Non-vested balance as of December 31, 2008 |
1,914,130 |
$ |
22.73 |
|||||
|
Granted |
701,412 |
19.04 |
||||||
|
Vested |
(887,314 |
) |
23.68 |
|||||
|
Forfeited |
(37,167 |
) |
21.90 |
|||||
|
Non-vested balance as of December 31, 2009 |
1,691,061 |
$ |
20.73 |
|||||
The total fair value of restricted stock and restricted stock units vested during the years ended December 31, 2009, 2008 and 2007, was $17,213, $1,822 and $2,168, respectively.
As of December 31, 2009, there was $32,660 of total unrecognized compensation cost related to non-vested share-based compensation arrangements granted under the plans; that cost is expected to be recognized over a weighted-average period of 2.0 years. The actual tax benefit realized for the tax deductions from stock option exercises
totaled $395, $1,127 and $512 for the years ended December 31, 2009, 2008 and 2007, respectively.
The Company maintains an employee stock purchase plan and has issued 34,306 shares, 36,682 shares, and 32,563 shares in 2009, 2008 and 2007, respectively.
17. Retirement Plan
Centene has a defined contribution plan which covers substantially all employees who are at least twenty-one years of age. Under the plan, eligible employees may contribute a percentage of their base salary, subject to certain limitations. Centene may elect to match a portion of the employee’s contribution. Company
expense related to matching contributions to the plan was $3,499, $3,681 and $2,312 during the years ended December 31, 2009, 2008 and 2007, respectively.
18. Commitments
Centene and its subsidiaries lease office facilities and various equipment under non-cancelable operating leases which may contain escalation provisions. The rental expense related to these leases is recorded on a straight-line basis over the lease term, including rent holidays. Tenant improvement allowances are recorded
as a liability and amortized against rent expense over the term of the lease. Rent expense was $20,211, $19,561 and $15,108 for the years ended December 31, 2009, 2008 and 2007, respectively. Annual non-cancelable minimum lease payments over the next five years and thereafter are as follows:
|
2010 |
|
$ |
20,527 |
|
2011 |
|
17,812 | |
|
2012 |
|
13,502 | |
|
2013 |
|
9,645 | |
|
2014 |
|
7,425 | |
|
Thereafter |
|
14,439 | |
|
|
$ |
83,350 |
19. Contingencies
In May 2008, the Internal Revenue Services began an audit of the Company’s 2006 and 2007 tax returns. As a result of this audit, the IRS has initially denied the $34,856 tax benefit the Company recognized for the abandonment of the FirstGuard stock in 2007. The Company is proceeding with the appeals process and
believes that it is more likely than not that the Company’s tax position will be upheld. Accordingly, the Company has not made any adjustments to the reserve for this position.
The Company is routinely subjected to legal proceedings in the normal course of business. While the ultimate resolution of such matters is uncertain, the Company does not expect the results of any of these matters discussed above individually, or in the aggregate, to have a material effect on its financial position or results of
operations.
20. Earnings Per Share
The following table sets forth the calculation of basic and diluted net earnings per share for the years ended December 31:
|
2009 |
2008 |
2007 |
||||||||||
|
Earnings (loss) attributable to Centene Corporation common shareholders: |
||||||||||||
|
Earnings from continuing operations, net of tax |
$ | 86,093 | $ | 84,181 | $ | 41,040 | ||||||
|
Discontinued operations, net of tax |
(2,422 | ) | (684 | ) | 32,362 | |||||||
|
Net earnings |
$ | 83,671 | $ | 83,497 | $ | 73,402 | ||||||
|
Shares used in computing per share amounts: |
||||||||||||
|
Weighted average number of common shares outstanding |
43,034,791 | 43,275,187 | 43,539,950 | |||||||||
|
Common stock equivalents (as determined by applying the treasury stock method) |
1,281,676 | 1,123,768 | 1,283,132 | |||||||||
|
Weighted average number of common shares and potential dilutive common shares outstanding |
44,316,467 | 44,398,955 | 44,823,082 | |||||||||
|
Net earnings (loss) per share attributable to Centene Corporation: |
||||||||||||
|
Basic: |
||||||||||||
|
Continuing operations |
$ | 2.00 | $ | 1.95 | $ | 0.95 | ||||||
|
Discontinued operations |
(0.06 | ) | (0.02 | ) | 0.74 | |||||||
|
Earnings per common share |
$ | 1.94 | $ | 1.93 | $ | 1.69 | ||||||
|
Diluted: |
||||||||||||
|
Continuing operations |
$ | 1.94 | $ | 1.90 | $ | 0.92 | ||||||
|
Discontinued operations |
(0.05 | ) | (0.02 | ) | 0.72 | |||||||
|
Earnings per common share |
$ | 1.89 | $ | 1.88 | $ | 1.64 | ||||||
The calculation of diluted earnings per common share for 2009, 2008 and 2007 excludes the impact of 2,351,679 shares, 2,004,778 shares and 3,002,030 shares, respectively, related to anti-dilutive stock options, restricted stock and restricted stock units.
21. Segment Information
Centene operates in two segments: Medicaid Managed Care and Specialty Services. The Medicaid Managed Care segment consists of Centene’s health plans including all of the functions needed to operate them. The Specialty Services segment consists of Centene’s specialty companies including behavioral health,
individual health, life and health management, long-term care, managed vision, telehealth services, pharmacy benefits management and treatment compliance functions.
Factors used in determining the reportable business segments include the nature of operating activities, existence of separate senior management teams, and the type of information presented to the Company’s chief operating decision maker to evaluate all results of operations.
Segment information as of and for the year ended December 31, 2009, follows:
|
Medicaid
Managed Care |
Specialty
Services |
Eliminations |
Consolidated
Total |
|||||||||||||
|
Revenue from external customers |
$ | 3,617,675 | $ | 485,189 | $ | — | $ | 4,102,864 | ||||||||
|
Revenue from internal customers |
66,763 | 569,191 | (635,954 | ) | — | |||||||||||
|
Total revenue |
3,684,438 | 1,054,380 | (635,954 | ) | 4,102,864 | |||||||||||
|
Earnings from operations |
99,307 | 38,828 | — | 138,135 | ||||||||||||
|
Total assets |
1,330,987 | 371,377 | — | 1,702,364 | ||||||||||||
|
Stock compensation expense |
13,285 | 1,349 | — | 14,634 | ||||||||||||
|
Depreciation expense |
29,007 | 4,096 | — | 33,103 | ||||||||||||
|
Capital expenditures |
80,867 | 2,246 | — | 83,113 | ||||||||||||
Segment information as of and for the year ended December 31, 2008, follows:
|
Medicaid
Managed Care |
Specialty
Services |
Eliminations |
Consolidated
Total |
|||||||||||||
|
Revenue from external customers |
$ | 3,020,248 | $ | 344,267 | $ | — | $ | 3,364,515 | ||||||||
|
Revenue from internal customers |
60,451 | 474,061 | (534,512 | ) | — | |||||||||||
|
Total revenue |
3,080,699 | 818,328 | (534,512 | ) | 3,364,515 | |||||||||||
|
Earnings from operations |
108,363 | 23,198 | — | 131,561 | ||||||||||||
|
Total assets |
1,105,610 | 345,542 | — | 1,451,152 | ||||||||||||
|
Stock compensation expense |
13,840 | 1,346 | — | 15,186 | ||||||||||||
|
Depreciation expense |
25,271 | 3,182 | — | 28,453 | ||||||||||||
|
Capital expenditures |
58,856 | 4,635 | — | 63,491 | ||||||||||||
Segment information as of and for the year ended December 31, 2007, follows:
|
Medicaid
Managed Care |
Specialty
Services |
Eliminations |
Consolidated
Total |
|||||||||||||
|
Revenue from external customers |
$ | 2,523,667 | $ | 245,361 | $ | — | $ | 2,769,028 | ||||||||
|
Revenue from internal customers |
76,637 | 407,563 | (484,200 | ) | — | |||||||||||
|
Total revenue |
2,600,304 | 652,924 | (484,200 | ) | 2,769,028 | |||||||||||
|
Earnings from operations |
35,545 | 19,700 | — | 55,245 | ||||||||||||
|
Total assets |
939,012 | 182,812 | — | 1,121,824 | ||||||||||||
|
Stock compensation expense |
13,820 | 1,505 | — | 15,325 | ||||||||||||
|
Depreciation expense |
19,970 | 2,677 | — | 22,647 | ||||||||||||
|
Capital expenditures |
49,846 | 3,941 | — | 53,787 | ||||||||||||
The Company evaluates performance and allocates resources based on earnings from operations. The accounting policies are the same as those described in Note 2, Summary of Significant Accounting Policies.
22. Comprehensive Earnings
Differences between net earnings and total comprehensive earnings resulted from changes in unrealized gains on investments available for sale, as follows:
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Net earnings |
$ | 83,671 | $ | 83,497 | $ | 73,402 | ||||||
|
Reclassification adjustment, net of tax |
252 | 252 | (242 | ) | ||||||||
|
Change in unrealized gains on investments available for sale, net of tax |
3,944 | 1,329 | 3,064 | |||||||||
|
Total change |
4,196 | 1,581 | 2,822 | |||||||||
|
Comprehensive earnings |
87,867 | 85,078 | 76,224 | |||||||||
|
Comprehensive earnings attributable to the noncontrolling interest |
2,574 | — | — | |||||||||
|
Comprehensive earnings attributable to Centene Corporation |
$ | 85,293 | $ | 85,078 | $ | 76,224 | ||||||
23. Quarterly Selected Financial Information
(In thousands, except share data and membership data)
(Unaudited)
|
For the Quarter Ended |
||||||||||||||||
|
March 31,
2009 |
June 30,
2009 |
September 30,
2009 |
December 31,
2009 |
|||||||||||||
|
Total revenues |
$ | 932,435 | $ | 1,039,469 | $ | 1,038,234 | $ | 1,092,726 | ||||||||
|
Amounts attributable to Centene Corporation common shareholders: |
||||||||||||||||
|
Earnings from continuing operations, net of income tax expense |
18,907 | 20,715 | 22,728 | 23,743 | ||||||||||||
|
Discontinued operations, net of income tax (benefit) expense |
(449 | ) | (485 | ) | (1,460 | ) | (28 | ) | ||||||||
|
Net earnings |
$ | 18,458 | $ | 20,230 | $ | 21,268 | $ | 23,715 | ||||||||
|
Net earnings (loss) per share attributable to Centene Corporation: |
||||||||||||||||
|
Basic: |
||||||||||||||||
|
Continued operations |
$ | 0.44 | $ | 0.48 | $ | 0.53 | $ | 0.55 | ||||||||
|
Discontinued operations |
(0.01 | ) | (0.01 | ) | (0.04 | ) | — | |||||||||
|
Basic earnings per common share |
$ | 0.43 | $ | 0.47 | $ | 0.49 | $ | 0.55 | ||||||||
|
Diluted: |
||||||||||||||||
|
Continued operations |
$ | 0.43 | $ | 0.47 | $ | 0.51 | $ | 0.53 | ||||||||
|
Discontinued operations |
(0.01 | ) | (0.01 | ) | (0.03 | ) | — | |||||||||
|
Diluted earnings per common share |
$ | 0.42 | $ | 0.46 | $ | 0.48 | $ | 0.53 | ||||||||
|
Period end at-risk membership |
1,247,300 | 1,289,000 | 1,386,400 | 1,455,600 | ||||||||||||
|
For the Quarter Ended |
||||||||||||||||
|
March 31,
2008 (1) |
June 30,
2008 |
September 30,
2008 |
December 31,
2008 (2) |
|||||||||||||
|
Total revenues |
$ | 779,228 | $ | 823,930 | $ | 858,599 | $ | 902,758 | ||||||||
|
Amounts attributable to Centene Corporation common shareholders: |
||||||||||||||||
|
Earnings from continuing operations, net of income tax expense |
24,933 | 17,883 | 18,099 | 23,266 | ||||||||||||
|
Discontinued operations, net of income tax (benefit) expense |
690 | 320 | 149 | (1,843 | ) | |||||||||||
|
Net earnings |
$ | 25,623 | $ | 18,203 | $ | 18,248 | $ | 21,423 | ||||||||
|
Net earnings (loss) per share attributable to Centene Corporation: |
||||||||||||||||
|
Basic: |
||||||||||||||||
|
Continued operations |
$ | 0.57 | $ | 0.41 | $ | 0.42 | $ | 0.54 | ||||||||
|
Discontinued operations |
0.02 | 0.01 | - | (0.04 | ) | |||||||||||
|
Basic earnings per common share |
$ | 0.59 | $ | 0.42 | $ | 0.42 | $ | 0.50 | ||||||||
|
Diluted: |
||||||||||||||||
|
Continued operations |
$ | 0.56 | $ | 0.40 | $ | 0.41 | $ | 0.53 | ||||||||
|
Discontinued operations |
0.01 | 0.01 | - | (0.04 | ) | |||||||||||
|
Diluted earnings per common share |
$ | 0.57 | $ | 0.41 | $ | 0.41 | $ | 0.49 | ||||||||
|
Period end at-risk membership |
1,069,700 | 1,148,800 | 1,171,100 | 1,196,000 | ||||||||||||
______________________________________
(1) Includes $20.8 million pre-tax premium revenue for the Georgia premium rate increase for July 1, 2007 – December 31, 2007.
(2) Includes a $3.7 million pre-tax charge primarily for asset impairments and employee severance related to the sale of the New Jersey health plan, included in discontinued operations.
24. Condensed Financial Information of Registrant
Centene Corporation (Parent Company Only)
Condensed Balance Sheets
(In thousands, except share data)
|
December 31, |
||||||||
|
2009 |
2008 |
|||||||
|
ASSETS |
||||||||
|
Current assets: |
||||||||
|
Cash and cash equivalents |
$ | 8,664 | $ | 5,041 | ||||
|
Short-term investments, at fair value (amortized cost $1,305 and $1,516, respectively) |
1,307 | 1,524 | ||||||
|
Other current assets |
84,588 | 72,270 | ||||||
|
Total current assets |
94,559 | 78,835 | ||||||
|
Long-term investments, at fair value (amortized cost $16,646 and 14,379, respectively) |
17,160 | 13,725 | ||||||
|
Investment in subsidiaries |
756,892 | 637,384 | ||||||
|
Other long-term assets |
14,673 | 17,217 | ||||||
|
Total assets |
$ | 883,284 | $ | 747,161 | ||||
|
LIABILITIES AND STOCKHOLDERS’ EQUITY |
||||||||
|
Current liabilities |
$ | 3,785 | $ | 7,342 | ||||
|
Long-term debt |
259,000 | 238,000 | ||||||
|
Other long-term liabilities |
1,072 | 547 | ||||||
|
Total liabilities |
263,857 | 245,889 | ||||||
|
Stockholders’ equity: |
||||||||
|
Common stock, $.001 par value; authorized 100,000,000 shares; issued and outstanding 45,593,383 and 45,071,179 shares, respectively |
46 | 45 | ||||||
|
Additional paid-in capital |
281,806 | 263,835 | ||||||
|
Accumulated other comprehensive income: |
||||||||
|
Unrealized gain on investments, net of tax |
7,348 | 3,152 | ||||||
|
Retained earnings |
358,907 | 275,236 | ||||||
|
Treasury stock, at cost (2,414,010 and 2,083,415 shares, respectively) |
(47,262 | ) | (40,996 | ) | ||||
|
Total Centene stockholders’ equity |
600,845 | 501,272 | ||||||
|
Noncontrolling interest |
18,582 | — | ||||||
|
Total stockholders’ equity |
619,427 | 501,272 | ||||||
|
Total liabilities and stockholders’ equity |
$ | 883,284 | $ | 747,161 | ||||
See notes to condensed financial information of registrant.
Centene Corporation (Parent Company Only)
Condensed Statements of Operations
(In thousands, except share data)
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Expenses: |
||||||||||||
|
General and administrative expenses |
$ |
(2,906 |
) |
$ |
(6,153 |
) |
$ |
(5,513 |
) | |||
|
Other income (expense): |
||||||||||||
|
Investment and other income |
6 |
(324 |
) |
913 |
||||||||
|
Interest expense |
(15,692 |
) |
(15,395 |
) |
(13,627 |
) | ||||||
|
Loss before income taxes |
(18,592 |
) |
(21,872 |
) |
(18,227 |
) | ||||||
|
Income tax benefit |
(6,004 |
) |
(7,988 |
) |
(51,178 |
) | ||||||
|
Net earnings (loss) before equity in subsidiaries |
(12,588 |
) |
(13,884 |
) |
32,951 |
|||||||
|
Equity in earnings from subsidiaries |
96,259 |
97,381 |
40,451 |
|||||||||
|
Net earnings |
$ |
83,671 |
$ |
83,497 |
$ |
73,402 |
||||||
|
Net earnings per share: |
||||||||||||
|
Basic earnings per common share |
$ |
1.94 |
$ |
1.93 |
$ |
1.69 |
||||||
|
Diluted earnings per common share |
$ |
1.89 |
$ |
1.88 |
$ |
1.64 |
||||||
|
Weighted average number of shares outstanding: |
||||||||||||
|
Basic |
43,034,791 |
43,275,187 |
43,539,950 |
|||||||||
|
Diluted |
44,316,467 |
44,398,955 |
44,823,082 |
|||||||||
See notes to condensed financial information of registrant.
Centene Corporation (Parent Company Only)
Condensed Statements of Cash Flows
(In thousands)
|
Year Ended December 31, |
||||||||||||
|
2009 |
2008 |
2007 |
||||||||||
|
Cash flows from operating activities: |
||||||||||||
|
Cash provided by operating activities |
$ |
92,711 |
$ |
37,487 |
$ |
94,145 |
||||||
|
Cash flows from investing activities: |
||||||||||||
|
Net dividends from and capital contributions to subsidiaries |
(67,328 |
) |
10,146 |
(71,813 |
) | |||||||
|
Purchase of investments |
(17,181 |
) |
(39,261 |
) |
(84,088 |
) | ||||||
|
Sales and maturities of investments |
9,189 |
30,779 |
77,086 |
|||||||||
|
Acquisitions, net of cash acquired |
(38,563 |
) |
(91,345 |
) |
(38,532 |
) | ||||||
|
Proceeds from asset sales |
— |
— |
14,102 |
|||||||||
|
Net cash used in investing activities |
(113,883 |
) |
(89,681 |
) |
(103,245 |
) | ||||||
|
Cash flows from financing activities: |
||||||||||||
|
Proceeds from borrowings |
616,500 |
224,000 |
212,000 |
|||||||||
|
Payment of long-term debt and notes payable |
(595,500 |
) |
(166,000 |
) |
(181,000 |
) | ||||||
|
Proceeds from exercise of stock options |
2,365 |
5,354 |
5,464 |
|||||||||
|
Common stock repurchases |
(6,304 |
) |
(23,510 |
) |
(9,541 |
) | ||||||
|
Debt issue costs |
(368 |
) |
— |
(5,181 |
) | |||||||
|
Distribution to noncontrolling interest |
(3,170 |
) |
— |
— |
||||||||
|
Contributions from noncontrolling interest |
11,219 |
— |
— |
|||||||||
|
Excess tax benefits from stock compensation |
53 |
3,100 |
— |
|||||||||
|
Net cash provided by financing activities |
24,795 |
42,944 |
21,742 |
|||||||||
|
Net increase (decrease) in cash and cash equivalents |
3,623 |
(9,250 |
) |
12,642 |
||||||||
|
Cash and cash equivalents, beginning of period |
5,041 |
14,291 |
1,649 |
|||||||||
|
Cash and cash equivalents, end of period |
$ |
8,664 |
$ |
5,041 |
$ |
14,291 |
||||||
See notes to condensed financial information of registrant.
Notes to Condensed Financial Information of Registrant
Note A – Basis of Presentation and Significant Accounting Policies
In Centene Corporation’s parent company only financial statements, Centene Corporation’s investment in subsidiaries is stated at cost plus equity in undistributed earnings of the subsidiaries. Centene Corporation’s share of net income of its unconsolidated subsidiaries is included in income using the equity method
of accounting.
Certain amounts presented in the parent company only financial statements are eliminated in the consolidated financial statements of Centene Corporation. The 2007 income tax benefit reflects a $34,856 tax benefit associated with the stock abandonment discussed in Note 3, Discontinued
Operations: University Health Plans and FirstGuard Health Plans.
Centene Corporation’s parent company only financial statements should be read in conjunction with Centene Corporation’s audited consolidated financial statements and the notes to consolidated financial statements included in this Form 10-K.
Note B – Dividends
During 2009, 2008 and 2007, the Registrant received dividends from its subsidiaries totaling $19,122, $48,411 and $53,937, respectively.
25. Subsequent Events
On January 21, 2010, the Company completed the sale of an additional 5.75 million shares of common stock for $19.25 per share. Net proceeds from the sale of the additional shares were approximately $104,500. A portion of the proceeds was used to repay the outstanding
indebtedness under our $300,000 revolving credit loan facility ($84,000 as of December 31, 2009). The Company intends to use the remaining net proceeds for general corporate purposes, which may include the repayment of indebtedness, funding for acquisitions, capital expenditures, additions to working capital and to meet statutory capital requirements in new or existing states.
Item 9. Changes in and Disagreements With Accountants on Accounting and Financial Disclosure
None.
Item 9A. Controls and Procedures
Evaluation of Disclosure Controls and Procedures - Our management, with the participation of our Chief Executive Officer and Chief Financial Officer, evaluated the effectiveness of our disclosure controls and procedures as of December 31, 2009. The term “disclosure controls
and procedures,” as defined in Rules 13a-15(e) and 15d-15(e) under the Exchange Act, means controls and other procedures of a company that are designed to ensure that information required to be disclosed by a company in the reports that it files or submits under the Exchange Act is recorded, processed, summarized and reported, within the time periods specified in the SEC's rules and forms. Disclosure controls and procedures include, without limitation, controls and procedures designed to ensure
that information required to be disclosed by a company in the reports that it files or submits under the Exchange Act is accumulated and communicated to the company’s management, including its principal executive and principal financial officers, as appropriate to allow timely decisions regarding required disclosure. Management recognizes that any controls and procedures, no matter how well designed and operated, can provide only reasonable assurance of achieving their objectives and management
necessarily applies its judgment in evaluating the cost-benefit relationship of possible controls and procedures. Based on the evaluation of our disclosure controls and procedures as of December 31, 2009, our Chief Executive Officer and Chief Financial Officer concluded that, as of such date, our disclosure controls and procedures were effective at the reasonable assurance level.
Management’s Report on Internal Control Over Financial Reporting - Our management is responsible for establishing and maintaining adequate internal control over financial reporting, as such term is defined in Exchange Act Rules 13a-15(f) and 15d-15(f). Under
the supervision and with the participation of our management, including our principal executive officer and principal financial officer, we conducted an evaluation of the effectiveness of our internal control over financial reporting based on the framework in Internal Control – Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway Commission. Based
on our evaluation under the framework in Internal Control - Integrated Framework, our management concluded that our internal control over financial reporting was effective at the reasonable assurance level as of December 31, 2009. Our management’s assessment of the effectiveness of our internal control over financial reporting as of December 31, 2009 has been audited by KPMG LLP, an independent registered public accounting firm, as stated
in their report which is included herein.
Changes in Internal Control Over Financial Reporting - No change in our internal control over financial reporting (as defined in Rules 13a-15(f) and 15d-15(f) under the Exchange Act) occurred during the quarter ended December 31, 2009 that has materially affected,
or is reasonably likely to materially affect, our internal control over financial reporting.
Report of Independent Registered Public Accounting Firm
The Board of Directors and Stockholders
Centene Corporation:
We have audited Centene Corporation’s internal control over financial reporting as of December 31, 2009, based on criteria established in Internal Control - Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway Commission (COSO). Centene
Corporation’s management is responsible for maintaining effective internal control over financial reporting and for its assessment of the effectiveness of internal control over financial reporting, included in the accompanying Management’s Report on Internal Control Over Financial Reporting. Our responsibility is to express an opinion on the Company’s internal control over financial reporting based on our audit.
We conducted our audit in accordance with the standards of the Public Company Accounting Oversight Board (United States). Those standards require that we plan and perform the audit to obtain reasonable assurance about whether effective internal control over financial reporting was maintained in all material respects. Our audit included obtaining
an understanding of internal control over financial reporting, assessing the risk that a material weakness exists, and testing and evaluating the design and operating effectiveness of internal control based on the assessed risk. Our audit also included performing such other procedures as we considered necessary in the circumstances. We believe that our audit provides a reasonable basis for our opinion.
A company's internal control over financial reporting is a process designed to provide reasonable assurance regarding the reliability of financial reporting and the preparation of financial statements for external purposes in accordance with generally accepted accounting principles. A company's internal control over financial reporting
includes those policies and procedures that (1) pertain to the maintenance of records that, in reasonable detail, accurately and fairly reflect the transactions and dispositions of the assets of the company; (2) provide reasonable assurance that transactions are recorded as necessary to permit preparation of financial statements in accordance with generally accepted accounting principles, and that receipts and expenditures of the company are being made only in accordance with authorizations of management and
directors of the company; and (3) provide reasonable assurance regarding prevention or timely detection of unauthorized acquisition, use, or disposition of the company’s assets that could have a material effect on the financial statements.
Because of its inherent limitations, internal control over financial reporting may not prevent or detect misstatements. Also, projections of any evaluation of effectiveness to future periods are subject to the risk that controls may become inadequate because of changes in conditions, or that the degree of compliance with the policies
or procedures may deteriorate.
In our opinion, Centene Corporation maintained, in all material respects, effective internal control over financial reporting as of December 31, 2009, based on criteria established in Internal Control - Integrated Framework issued by the Committee of Sponsoring Organizations of the Treadway
Commission.
We also have audited, in accordance with the standards of the Public Company Accounting Oversight Board (United States), the consolidated balance sheets of Centene Corporation as of December 31, 2009 and 2008, and the related consolidated statements of operations, stockholders’ equity, and cash flows for each of the years in the three-year
period ended December 31, 2009, and our report dated February 21, 2010 expressed an unqualified opinion on those consolidated financial statements.
KPMG LLP
St. Louis, Missouri
February 21, 2010
Item 9B. Other Information
None.
PART III
Item 10. Directors, Executive Officers and Corporate Governance
(a) Directors of the Registrant
Information concerning our directors will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Election of Directors.” This portion of the Proxy Statement is incorporated herein by reference.
(b) Executive Officers of the Registrant
Pursuant to General Instruction G(3) to Form 10-K and Instruction 3 to Item 401(b) of Regulation S-K, information regarding our executive officers is provided in Item 1 of Part I of this Annual Report on Form 10-K under the caption “Executive Officers of the Registrant.”
Information concerning our executive officers’ compliance with Section 16(a) of the Securities Exchange Act will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Section 16(a) Beneficial Ownership Reporting Compliance.” These portions of our Proxy Statement are incorporated herein by reference. Information
concerning our audit committee financial expert and identification of our audit committee will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Information about Corporate Governance.” Information concerning our code of ethics will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Code of Business Conduct and Ethics.”
(c) Corporate Governance
Information concerning certain corporate governance matters will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Information About Corporate Governance -- Director Candidates”, “Information About Corporate Governance -- Board and Committee Meetings” and “Information
About Corporate Governance -- Audit Committee.” These portions of our Proxy Statement are incorporated herein by reference.
Item 11. Executive Compensation
Information concerning executive compensation will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Information About Executive Compensation.” This portion of the Proxy Statement is incorporated herein by reference. The sections entitled “Compensation Committee Report”
in our 2010 Proxy Statement are not incorporated herein by reference.
Item 12. Security Ownership of Certain Beneficial Owners and Management and Related Stockholder Matters
Information concerning the security ownership of certain beneficial owners and management and our equity compensation plans will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Information About Stock Ownership” and “Equity Compensation Plan Information.” These portions of the Proxy
Statement are incorporated herein by reference.
Item 13. Certain Relationships and Related Transactions, and Director Independence
Information concerning certain relationships and related transactions will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Related Party Transactions.” This portion of our Proxy Statement is incorporated herein by reference.
Item 14. Principal Accountant Fees and Services
Information concerning principal accountant fees and services will appear in our Proxy Statement for our 2010 annual meeting of stockholders under “Independent Auditor Fees.” This portion of our Proxy Statement is incorporated herein by reference.
PART IV
Item 15. Exhibits and Financial Statement Schedules
|
(a) |
Financial Statements and Schedules |
The following documents are filed under Item 8 of this report:
1. Financial Statements:
|
Report of Independent Registered Public Accounting Firm |
|
Consolidated Balance Sheets as of December 31, 2009 and 2008 |
|
Consolidated Statements of Operations for the Years Ended December 31, 2009, 2008 and 2007 |
|
Consolidated Statements of Stockholders’ Equity for the Years Ended December 31, 2009, 2008 and 2007 |
|
Consolidated Statements of Cash Flows for the Years Ended December 31, 2009, 2008 and 2007 |
|
Notes to Consolidated Financial Statements |
2. Financial Statement Schedules:
None.
|
(b) |
Exhibits |
The exhibits listed in the accompanying Exhibit Index are filed or incorporated by reference as part of this filing.
EXHIBIT INDEX
|
|
|
|
INCORPORATED BY REFERENCE 1 | |||||||
|
EXHIBIT
NUMBER |
|
DESCRIPTION |
|
FILED WITH
THIS
FORM 10-K |
|
FORM |
|
FILING DATE
WITH SEC |
|
EXHIBIT
NUMBER |
|
3.1 |
|
Certificate of Incorporation of Centene Corporation |
|
|
S-1 |
|
October 9, 2001 |
|
3.2 | |
|
3.1a |
|
Certificate of Amendment to Certificate of Incorporation of Centene Corporation, dated November 8, 2001 |
|
|
S-1/A |
|
November 13, 2001 |
|
3.2a | |
|
3.1b |
|
Certificate of Amendment to Certificate of Incorporation of Centene Corporation as filed with the Secretary of State of the State of Delaware |
|
|
10-Q |
|
July 26, 2004 |
|
3.1b | |
|
3.2 |
|
By-laws of Centene Corporation |
|
|
S-1 |
|
October 9, 2001 |
|
3.4 | |
|
4.1 |
|
Rights Agreement between Centene Corporation and Mellon Investor Services LLC, as Rights Agent, dated August 30, 2002 |
|
|
8-K |
|
August 30, 2002 |
|
4.1 | |
|
4.1a |
|
Amendment No. 1 to Rights Agreement by and between Centene Corporation and Mellon Investor Services LLC, as right agent, dated April 23, 2007 |
|
|
8-K |
|
April 26, 2007 |
|
4.1 | |
|
4.2 |
|
Indenture for the 7 ¼% Senior Notes due 2014 dated March 22, 2007 among Centene Corporation and The Bank of New York Trust Company, N.A., as trustee |
|
|
S-4 |
|
May 11, 2007 |
|
4.3 | |
|
10.1 |
Contract Between the Georgia Department of Community Health and Peach State Contract for provision of Services to Georgia Health Families |
8-K |
July 22, 2005 |
10.1 | ||||||
|
10.1a |
Amendment #1 to the Contract No. 0653 Between Georgia Department of Community Health and Peach State |
10-Q |
October 25, 2005 |
10.9 | ||||||
|
10.1b |
Amendment #2 to the Contract No. 0653 Between Georgia Department of Community Health and Peach State |
10-K |
February 23, 2008 |
10.1b | ||||||
|
10.1c |
Amendment #3 to the Contract No. 0653 Between Georgia Department of Community Health and Peach State |
10-K |
February 23, 2009 |
10.1c | ||||||
|
10.1d |
Amendment #4 to the Contract No. 0653 Between Georgia Department of Community Health and Peach State |
10-K |
February 23, 2009 |
10.1d | ||||||
|
10.1e |
** |
Amendment #6 to the Contract No. 0653 Between Georgia Department of Community Health and Peach State |
X |
|||||||
|
10.1f |
Notice of Renewal for fiscal year 2008 between Peach State Health Plan, Inc. and Georgia Department of Community Health |
10-Q |
July 24, 2007 |
10.4 | ||||||
|
10.1g |
Notice of Renewal for fiscal year 2009 between Peach State Health Plan, Inc. and Georgia Department of Community Health |
10-Q |
July 22, 2008 |
10.1 | ||||||
|
10.1h |
Notice of Renewal for fiscal year 2010 between Peach State Health Plan, Inc. and Georgia Department of Community Health |
10-Q |
July 28, 2009 |
10.2 | ||||||
|
10.2 |
Contract between the Texas Health and Human Services Commission and Superior HealthPlan, Inc. |
|
10-K |
February 24, 2006 |
10.5 | |||||
|
10.2a |
** |
Amendment M (Version 1.13) to Contract between the Texas Health and Human Services Commission and Superior HealthPlan, Inc. |
10-Q |
October 27, 2009 |
10.1 | |||||
|
10.3 |
* |
1996 Stock Plan of Centene Corporation, shares which are registered on Form S-8 – File Number 333-83190 |
S-1 |
October 9, 2001 |
10.9 | |||||
|
10.4 |
* |
1998 Stock Plan of Centene Corporation, shares which are registered on Form S-8 – File number 333-83190 |
S-1 |
October 9, 2001 |
10.10 | |||||
|
10.5 |
* |
1999 Stock Plan of Centene Corporation, shares which are registered on Form S-8 – File Number 333-83190 |
S-1 |
October 9, 2001 |
10.11 | |||||
|
10.6 |
* |
2000 Stock Plan of Centene Corporation, shares which are registered on Form S-8 – File Number 333-83190 |
S-1 |
October 9, 2001 |
10.12 | |||||
|
10.7 |
* |
2002 Employee Stock Purchase Plan of Centene Corporation, shares which are registered on Form S-8 – File Number 333-90976 |
10-Q |
April 29, 2002 |
10.5 | |||||
|
10.7a |
* |
First Amendment to the 2002 Employee Stock Purchase Plan |
10-K |
February 24, 2005 |
10.9a | |||||
|
10.7b |
* |
Second Amendment to the 2002 Employee Stock Purchase Plan |
|
10-K |
February 24, 2006 |
10.10b | ||||
|
10.8 |
* |
Centene Corporation Amended and Restated 2003 Stock Incentive Plan, shares which are registered on Form S-8 – File Number 333-108467 |
8-K |
April 25, 2008 |
10.1 | |||||
|
10.9 |
* |
Centene Corporation Non-Employee Directors Deferred Stock Compensation Plan |
10-Q |
October 25, 2004 |
10.1 | |||||
|
10.9a |
* |
First Amendment to the Non-Employee Directors Deferred Stock Compensation Plan |
|
10-K |
February 24, 2006 |
10.12a | ||||
|
10.10 |
* |
Centene Corporation Employee Deferred Compensation Plan |
X |
|||||||
|
10.11 |
* |
Centene Corporation 2007 Long-Term Incentive Plan |
8-K |
April 26, 2007 |
10.2 | |||||
|
10.12 |
* |
Executive Employment Agreement between Centene Corporation and Michael F. Neidorff, dated November 8, 2004 |
8-K |
November 9, 2004 |
10.1 | |||||
|
10.12a |
* |
Amendment No. 1 to Executive Employment Agreement between Centene Corporation and Michael F. Neidorff |
10-Q |
October 28, 2008 |
10.2 | |||||
|
10.12b |
* |
Amendment No. 2 to Executive Employment Agreement between Centene Corporation and Michael F. Neidorff |
10-Q |
April 28, 2009 |
10.2 | |||||
|
10.13 |
* |
Form of Executive Severance and Change in Control Agreement |
10-Q |
October 28, 2008 |
10.3 | |||||
|
10.14 |
* |
Form of Restricted Stock Unit Agreement |
10-Q |
October 28, 2008 |
10.4 | |||||
|
10.15 |
* |
Form of Non-statutory Stock Option Agreement (Non-Employees) |
8-K |
July 28, 2005 |
10.3 | |||||
|
10.16 |
* |
Form of Non-statutory Stock Option Agreement (Employees) |
10-Q |
October 28, 2008 |
10.5 | |||||
|
10.17 |
* |
Form of Non-statutory Stock Option Agreement (Directors) |
10-K |
February 23, 2009 |
10.18 | |||||
|
10.18 |
* |
Form of Incentive Stock Option Agreement |
10-Q |
October 28, 2008 |
10.6 | |||||
|
10.19 |
* |
Form of Stock Appreciation Right Agreement |
8-K |
July 28, 2005 |
10.6 | |||||
|
10.20 |
* |
Form of Restricted Stock Agreement |
10-Q |
October 25, 2005 |
10.8 | |||||
|
10.21 |
* |
Form of Performance Based Restricted Stock Unit Agreement #1 |
10-Q |
October 28, 2008 |
10.7 | |||||
|
10.22 |
* |
Form of Performance Based Restricted Stock Unit Agreement #2 |
10-K |
February 23, 2009 |
10.23 | |||||
|
10.23 |
* |
Form of Long Term Incentive Plan Agreement |
8-K |
February 7, 2008 |
10.1 | |||||
|
10.24 |
Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
10-Q |
October 25, 2004 |
10.2 | ||||||
|
10.24a |
Amendment No. 2 to Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
10-Q |
October 25, 2005 |
10.11 | ||||||
|
10.24b |
Amendment No. 3 to Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
|
10-K |
February 24, 2006 |
10.22b | |||||
|
10.24c |
Amendment No. 4 to Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
10-Q |
July 25, 2006 |
10.2 | ||||||
|
10.24d |
Amendment No. 5 to Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
10-Q |
October 24, 2006 |
10.1 | ||||||
|
10.24e |
Amendment No. 6 to Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
10-K |
February 23, 2008 |
10.23e | ||||||
|
10.24f |
Amendment No. 7 to Credit Agreement dated as of September 14, 2004 among Centene Corporation, the various financial institutions party hereto and LaSalle Bank National Association |
10-Q |
July 28, 2009 |
10.1 | ||||||
|
12.1 |
Computation of ratio of earnings to fixed charges |
X |
|
|||||||
|
21 |
List of subsidiaries |
X |
||||||||
|
23 |
Consent of Independent Registered Public Accounting Firm incorporated by reference in each prospectus constituting part of the Registration Statements on Form S-3 (File Number 333-164390) and on Form S-8 (File Numbers 333-108467, 333-90976 and 333-83190) |
X |
||||||||
|
31.1 |
Certification Pursuant to Rule 13a-14(a) and 15d-14(a) of the Exchange Act, as Adopted Pursuant to Section 302 of the Sarbanes-Oxley Act of 2002 (Chief Executive Officer) |
X |
||||||||
|
31.2 |
Certification Pursuant to Rule 13a-14(a) and 15d-14(a) of the Exchange Act, as Adopted Pursuant to Section 302 of the Sarbanes-Oxley Act of 2002 (Chief Financial Officer) |
X |
||||||||
|
32.1 |
Certification Pursuant to 18 U.S.C. Section 1350 (Chief Executive Officer) |
X |
||||||||
|
32.2 |
Certification Pursuant to 18 U.S.C. Section 1350 (Chief Financial Officer) |
X |
||||||||
|
1 SEC File No. 001-31826 (for filings prior to October 14, 2003, the Registrant’s SEC File No. was 000-33395).
* Indicates a management contract or compensatory plan or arrangement.
** The Company has requested confidential treatment of the redacted portions of this exhibit pursuant to Rule 24b-2 under the Securities Exchange Act of 1934, as amended, and has separately filed a complete copy of this exhibit with the Securities and Exchange Commission. | ||||||||||
SIGNATURES
Pursuant to the requirements of Section 13 or 15(d) of the Securities Exchange Act of 1934, the registrant has duly caused this report to be signed on its behalf by the undersigned, thereunto duly authorized, as of February 22, 2010.
|
CENTENE CORPORATION | ||
|
By: |
/s/ MICHAEL F. NEIDORFF | |
|
Michael F. Neidorff
Chairman and Chief Executive Officer | ||
Pursuant to the requirements of the Securities Exchange Act of 1934, this report has been signed below by the following persons on behalf of the registrant and in the capacities as indicated, as of February 22, 2010.
|
Signature |
|
Title |
|
/s/ MICHAEL F. NEIDORFF
Michael F. Neidorff
|
|
Chairman and Chief Executive Officer
(principal executive officer) |
|
/s/ WILLIAM N. SCHEFFEL
William N. Scheffel
|
|
Executive Vice President and Chief Financial Officer (principal financial officer) |
|
/s/ JEFFREY A. SCHWANEKE
Jeffrey A. Schwaneke
|
Vice President, Corporate Controller and Chief Accounting Officer (principal accounting officer) | |
|
/s/ STEVE BARTLETT
Steve Bartlett
|
|
Director |
|
/s/ ROBERT K. DITMORE
Robert K. Ditmore
|
|
Director |
|
/s/ FRED H. EPPINGER
Fred H. Eppinger
|
|
Director |
|
/s/ RICHARD A. GEPHARDT
Richard A. Gephardt
|
|
Director |
|
/s/ PAMELA A. JOSEPH
Pamela A. Joseph
|
|
Director |
|
/s/ JOHN R. ROBERTS
John R. Roberts
|
|
Director |
|
/s/ DAVID L. STEWARD
David L. Steward
|
|
Director |
|
/s/ TOMMY G. THOMPSON
Tommy G. Thompson |
|
Director |
